Clear Sky Science · en
Candida albicans infection suppresses lipopolysaccharide or Pseudomonas aeruginosa stimulated murine bone marrow derived macrophage (BMDM) responses
When Friendly Fungi Turn Complicated
Most of the time, the yeast Candida albicans lives quietly on our skin and mucosal surfaces. But under the right (or rather, wrong) conditions it can cause serious, even deadly infections, especially in people with weakened immune systems. This study explores a less obvious danger: how Candida can subtly interfere with our immune defenses when it appears together with bacteria, potentially changing the course of mixed infections in ways that standard lab tests and treatments may overlook.
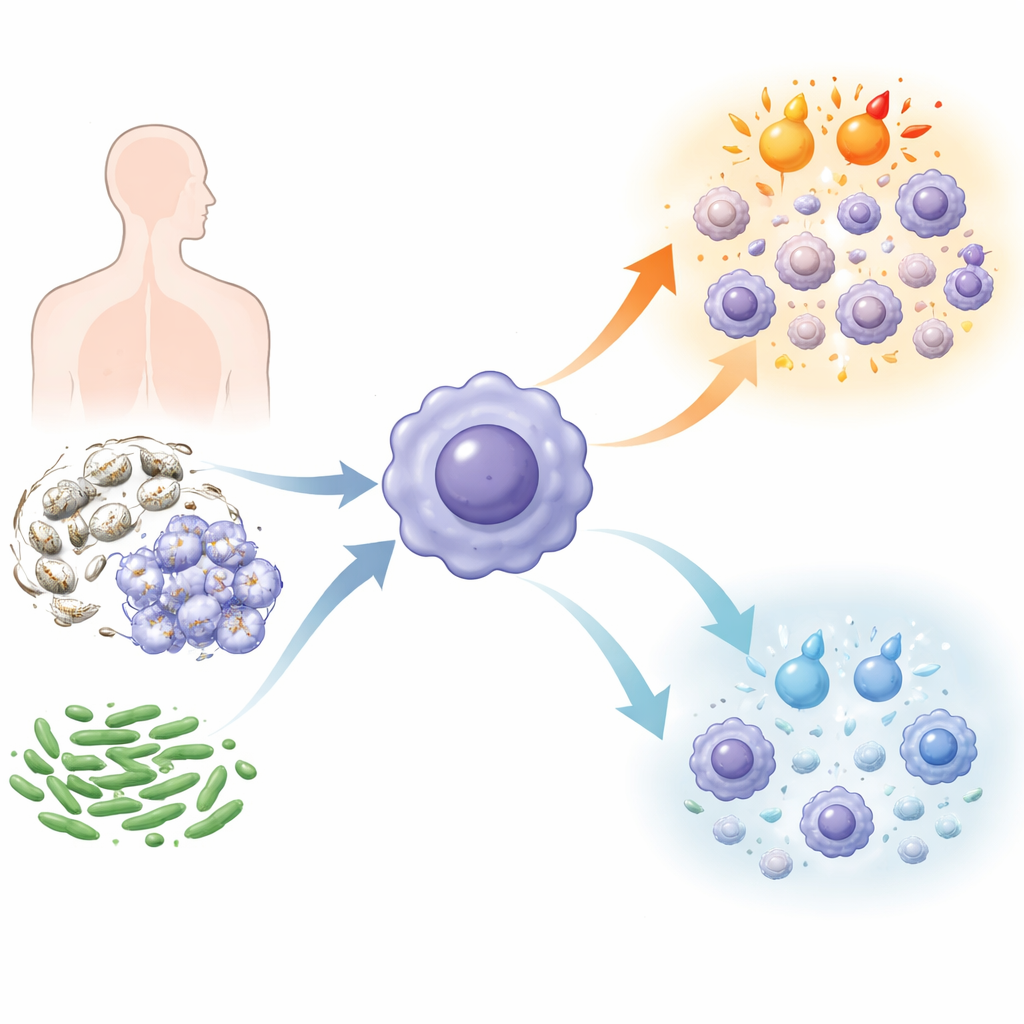
Why This Common Yeast Matters
Candida albicans is best known for causing local infections like thrush, but it can also enter the bloodstream and spread throughout the body, where it is very hard to treat and often fatal. At the same time, resistance to the limited set of antifungal drugs is rising. Our bodies rely heavily on immune cells called macrophages to recognize and engulf Candida, then call in reinforcements by releasing signaling proteins known as cytokines. In real life, however, Candida rarely acts alone: it often shares space with bacteria, such as the lung pathogen Pseudomonas aeruginosa in people with cystic fibrosis. Mixed infections like these are linked to worse outcomes, yet we know surprisingly little about how single immune cells behave when they face fungi and bacteria at the same time.
Taking a Proteome-Wide Look Inside Immune Cells
The researchers used mouse bone marrow–derived macrophages as a model and infected them with live Candida, with bacterial molecules such as lipopolysaccharide (LPS), or with the bacterium Pseudomonas itself. They then applied a high-resolution method called data‑independent acquisition proteomics, which essentially takes an inventory of thousands of proteins inside each cell. By comparing infected and uninfected cells, they could see how strongly the macrophages rearranged their internal machinery and which immune pathways turned on or off under each condition.
A Surprisingly Quiet Response to Candida Alone
When macrophages encountered live Candida by itself, they did respond, but not nearly as strongly as they did to LPS or Pseudomonas. Candida triggered some classic alarm pathways and modest production of inflammatory proteins like TNF, but the overall reshaping of the cell’s protein landscape was relatively muted. The data suggest that Candida can hide many of the features on its surface that immune receptors are built to recognize, blunting the macrophage’s alarm. Still, a small but consistent set of immune‑related proteins and regulators was altered, hinting that Candida was quietly priming the cells in more subtle ways.
How Candida Blunts Bacterial Alarms
The most striking finding appeared when Candida and bacterial stimuli were present together. In mixed exposures, Candida consistently dampened the macrophage’s response to LPS and to live Pseudomonas, sharply reducing production of certain key cytokines, particularly IL‑6 and IL‑12p40, while leaving others such as TNF and IL‑10 largely intact or even increased. Proteomic analysis showed that Candida broadly suppressed the large group of proteins that LPS or Pseudomonas normally turn up, but had little effect on proteins those agents turned down. This suppressive effect required live Candida in direct contact with the macrophage, and strains that could switch into long filamentous hyphae were better at dampening the response than mutants locked in the round yeast form, pointing to a role for fungal shape‑driven stress inside the cell.
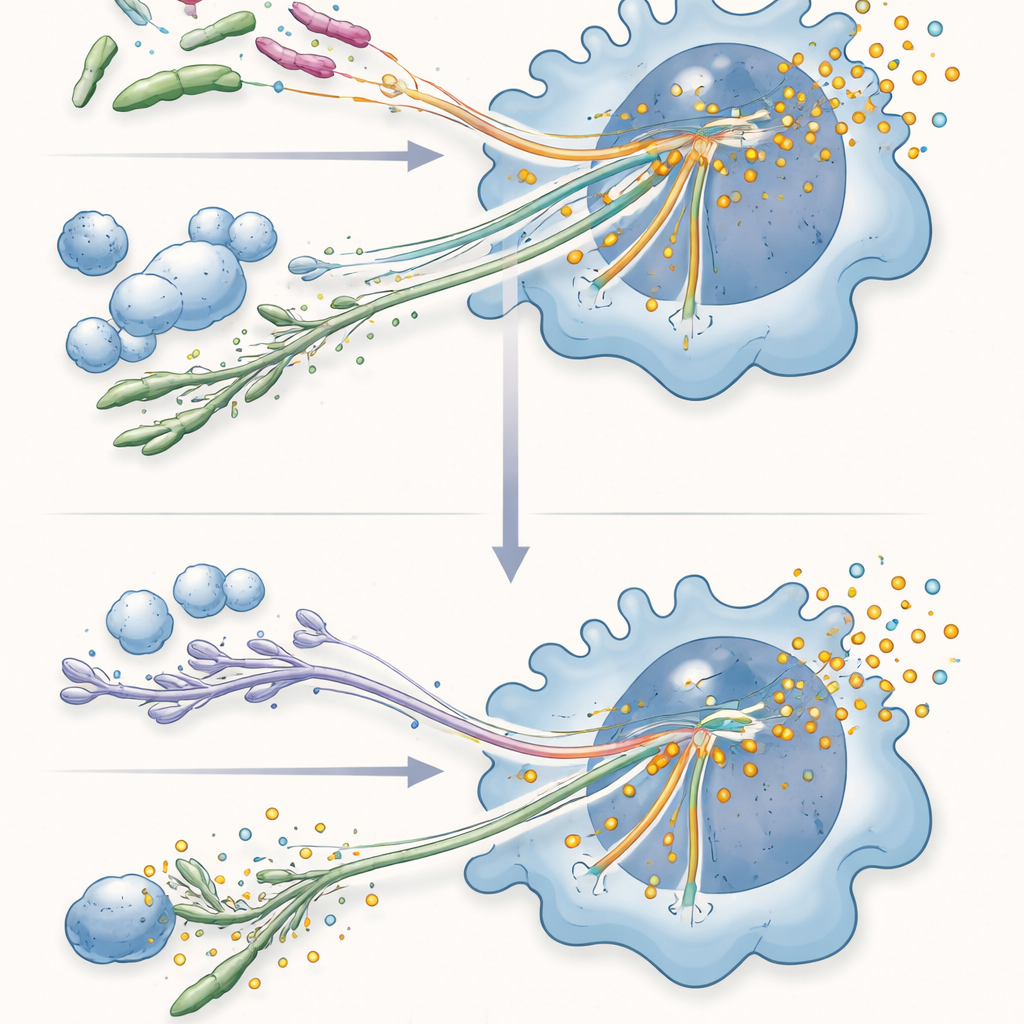
What This Means for Infections in Real Life
For a non‑specialist, the key message is that Candida does more than just cause its own infections; it can also act as a quiet saboteur of the immune system’s reaction to bacteria. By selectively turning down certain inflammatory signals inside macrophages during mixed infections, Candida may alter how effectively the body controls both fungi and bacteria. This work suggests that doctors and researchers should consider the combined behavior of microbes, not just one pathogen at a time, when thinking about severe infections and potential treatments. Understanding exactly how Candida applies this molecular “brake” on immune cells could eventually open new strategies to restore a balanced response without worsening inflammation.
Citation: Baker, C.P., Laba, S., Warner, J. et al. Candida albicans infection suppresses lipopolysaccharide or Pseudomonas aeruginosa stimulated murine bone marrow derived macrophage (BMDM) responses. Sci Rep 16, 8751 (2026). https://doi.org/10.1038/s41598-026-39429-z
Keywords: Candida albicans, macrophages, coinfection, innate immunity, Pseudomonas aeruginosa