Clear Sky Science · en
Changes in ovarian hardness and elasticity affect the development and function of secondary follicles
Why the firmness of the ovary matters
As women age, it becomes harder to conceive, but the reasons go beyond changing hormone levels or dwindling egg numbers. This study asks a deceptively simple question: does the physical feel of the ovary—how soft or stiff it is—change with age, and do those changes alter how eggs and their surrounding cells develop? By treating the ovary like a tiny mechanical organ whose texture can be measured and mimicked in the lab, the researchers uncover how subtle shifts in hardness and elasticity can push egg-supporting cells toward either healthy growth, premature aging, or inflammation.
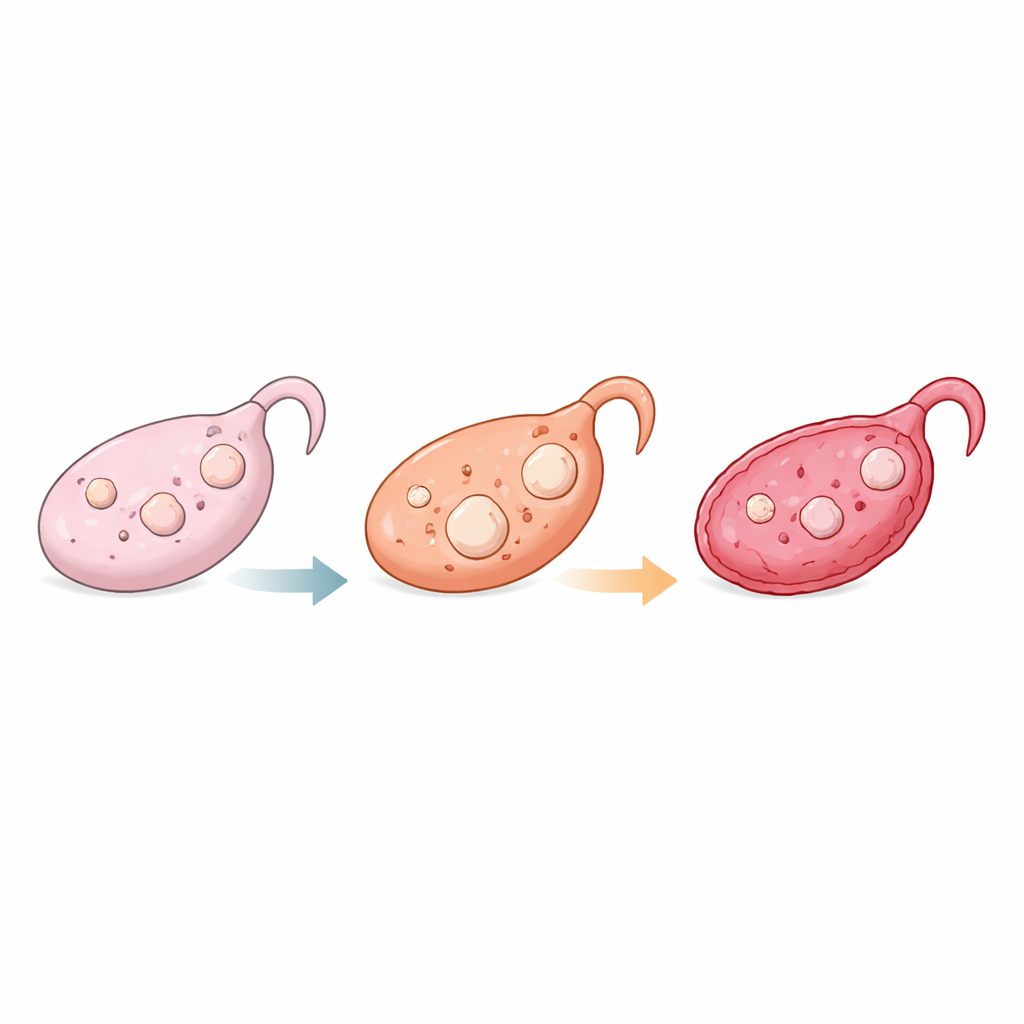
From soft youth to stiff old age
The ovary is not a uniform bag of cells. It is packed with follicles—small spheres in which an egg is surrounded by supportive granulosa cells and a capsule of connective tissue rich in collagen. The authors used a texture analyzer, a device more commonly seen in food science or materials testing, to quantify how hard and springy mouse ovaries are at different ages. Ovaries from young mice were both soft and easily deformed, those from mature adults were firmer and more elastic, and those from aged mice were unusually hard yet less elastic. This pattern matches earlier microscopic observations that collagen fibers around follicles are underdeveloped in young ovaries, optimally organized in mature ones, and overly abundant and rigid in older ovaries.
Recreating ovarian feel in a bead
To test cause and effect, the team recreated these age-specific textures using tiny spheres of alginate gel, a seaweed-derived material often used for three-dimensional cell culture. By changing alginate concentration and viscosity, they produced beads that matched the hardness and elasticity of young, mature, and aged mouse ovaries. They then embedded secondary follicles—an early growing stage with multiple layers of granulosa cells—inside these beads and cultured them for a week in hormone-containing medium. Follicles in the “young-like” soft, low-elasticity beads grew larger than those in “mature-like” beads, while follicles in “aged-like” hard, low-elasticity beads showed stunted growth. This showed that the surrounding mechanical environment alone, even with the same hormones, can steer how well follicles expand.
Signals of early aging and inflammation
Size was only part of the story. The researchers measured gene activity in granulosa cells to see how texture reshaped cell behavior. In the very soft condition, cells ramped up genes linked to luteinization—the process by which granulosa cells transform into hormone-producing cells normally seen after ovulation—as well as genes driving cell division. At the same time, they produced less of an egg-derived signaling factor and markers of ongoing follicle maturation. In other words, a too-soft environment made follicles look big but biochemically older than they should be. In contrast, in the very stiff condition mimicking aged ovaries, granulosa cells strongly increased genes associated with inflammation. This suggests that an overly rigid collagen-rich stroma can provoke a low-grade inflammatory state that interferes with normal follicle development, a scenario that resembles features of conditions such as polycystic ovary syndrome and age-related ovarian fibrosis.
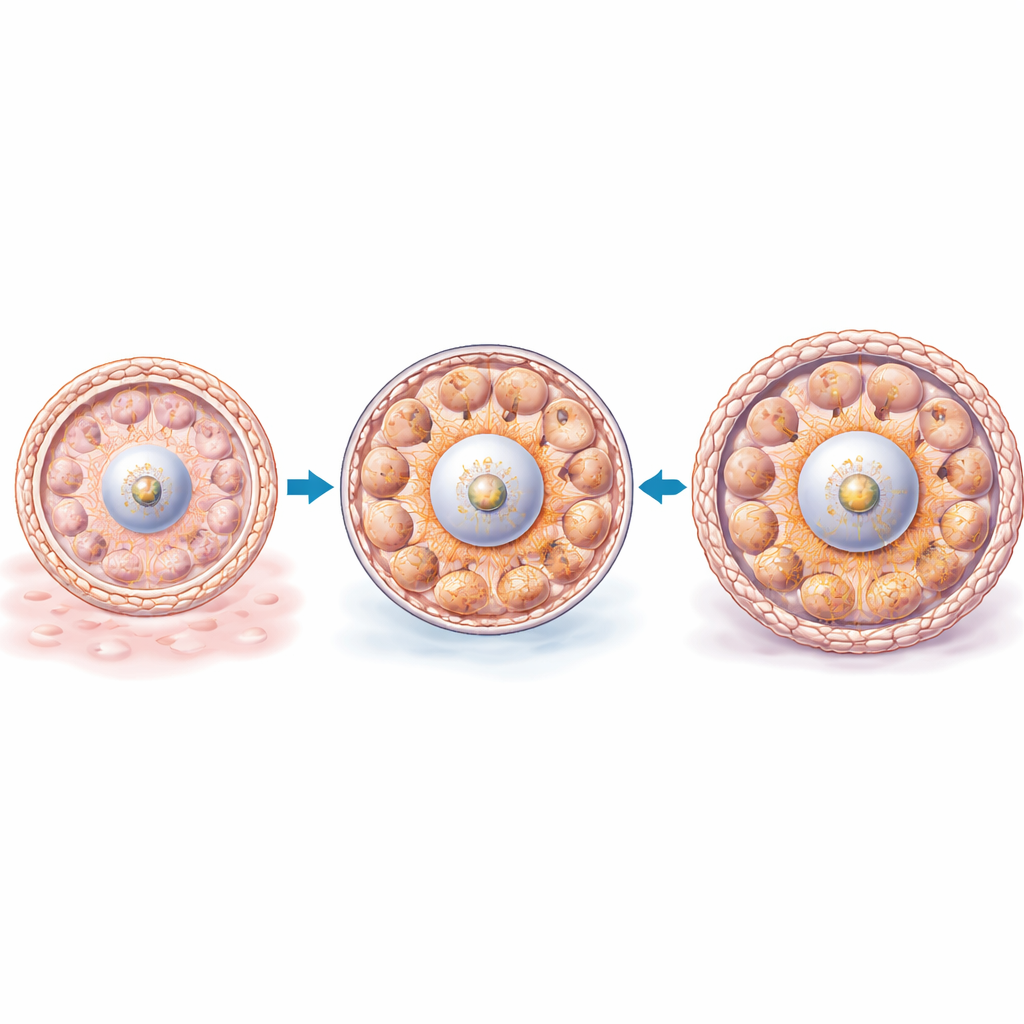
How cells feel and translate force
Granulosa cells need a way to “sense” how hard their surroundings are and convert that information into altered gene activity. The study focuses on YAP, a protein known as a mechanosensor: its location and modification state change when the cell’s internal scaffolding of actin fibers is tugged or compressed. In follicles cultured in both overly soft and overly stiff beads, YAP levels rose and its active form in the nucleus increased, along with several well-known YAP target genes. Disrupting actin fibers with cytochalasin pushed YAP into its active state and boosted the same targets, tying mechanical changes to this signaling route. These findings indicate that mismatched ovarian stiffness—too low or too high—feeds through the actin–YAP system to reprogram granulosa cells toward either premature luteinization or inflammatory behavior.
What this means for fertility and disease
To a lay reader, the takeaway is that the ovary’s physical setting is as important as its hormones. There appears to be a “just right” level of firmness and elasticity that lets follicles grow to the correct size, maintain healthy communication between the egg and its surrounding cells, and avoid chronic inflammation. When the ovary is too soft, cells may rush into a later, hormone-producing state before the egg is ready; when it is too stiff, inflammatory signals rise and follicle growth stalls. By mapping how these mechanical cues are sensed through YAP and the actin network, this work suggests that future fertility treatments or therapies for conditions like age-related infertility and ovarian fibrosis might one day target not only molecules, but also the tissue’s mechanical environment.
Citation: Kawai, T., Shimada, M. Changes in ovarian hardness and elasticity affect the development and function of secondary follicles. Sci Rep 16, 8837 (2026). https://doi.org/10.1038/s41598-026-39396-5
Keywords: ovarian stiffness, follicle development, mechanotransduction, YAP signaling, female fertility