Clear Sky Science · en
Combination of artesunate and ruxolitinib suppresses T cell leukemia/lymphoma proliferation via the JAK STAT pathway
New Ways to Slow a Fast-Moving Blood Cancer
T‑cell acute lymphoblastic leukemia and lymphoma are aggressive blood cancers that often strike children and adults in the prime of life. Despite modern chemotherapy, many patients relapse, and their outlook is poor. This study explores whether pairing two existing medicines, one originally used for malaria and another for bone marrow disease, could team up to better restrain these cancers by dialing down an overactive growth signal inside the cells.
A Deadly Disease That Still Needs Better Options
T‑cell acute lymphoblastic leukemia and lymphoma arise when immature infection‑fighting T cells in the bone marrow or lymph nodes begin to grow out of control. Intensive chemotherapy has steadily improved survival, especially in children, but about a third of patients still see their cancer return. When that happens, treatment becomes much harder and long‑term survival drops sharply. Because many of these tumors depend on particular internal signaling routes to keep dividing, researchers are looking for drugs that quietly sabotage those routes instead of relying only on broadly toxic chemotherapy.
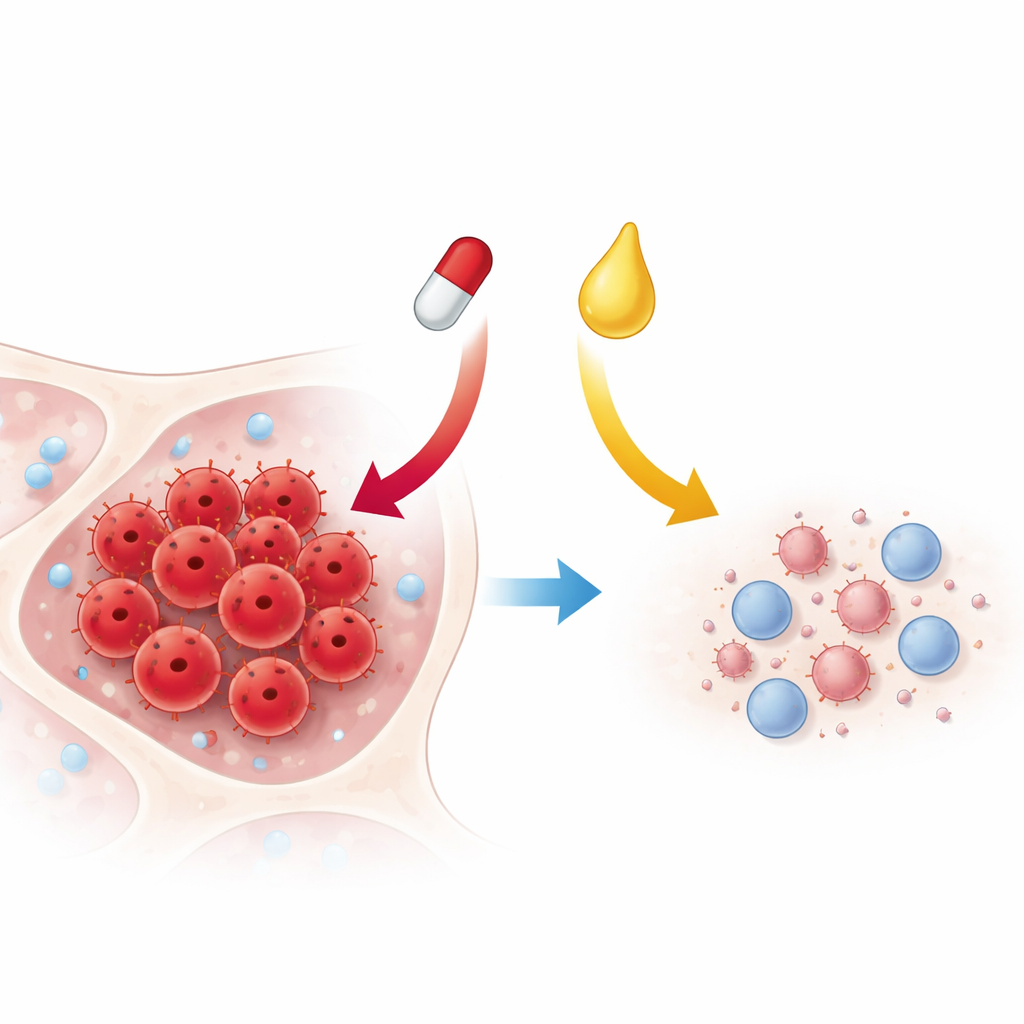
A Faulty Growth Signal as a Target
One of the key routes that T cells use to respond to hormones and immune messengers is known as the JAK–STAT pathway. In healthy cells, it helps control growth, survival, and immune responses. In many T‑cell leukemias and lymphomas, this pathway is stuck in the “on” position, telling cells to keep multiplying. The authors examined tissue from patients and found signs that this pathway is abnormally active in a portion of cases, supporting the idea that it could be a useful target. If scientists can safely turn this signal down, they may be able to slow the cancer without shutting down the entire immune system.
Repurposing Two Familiar Drugs
The team focused on two medicines already in clinical use. Artesunate is a derivative of the anti‑malarial compound artemisinin and has shown anticancer activity in several tumor types. Ruxolitinib is a targeted inhibitor that blocks JAK enzymes and is approved for certain bone marrow disorders. Using a human T‑cell leukemia cell line called Jurkat, the researchers exposed cells to different doses of each drug alone and in combination. They measured how many cells remained alive, how many underwent programmed cell death, and how strongly the JAK–STAT pathway was firing at both the genetic and protein levels.
Stronger Together Than Alone
Both artesunate and ruxolitinib caused the leukemia cells to die and reduced their ability to proliferate, with artesunate showing the stronger single‑drug effect. Importantly, when the two drugs were combined at several moderate to higher dose pairs, they worked synergistically: together they killed more cells and suppressed growth more than would be expected from simply adding their individual effects. The combination also increased the share of cells undergoing apoptosis compared with either drug alone. At lower doses, however, the drugs sometimes interfered with one another, highlighting that careful dose selection would be crucial if this strategy moves toward the clinic.
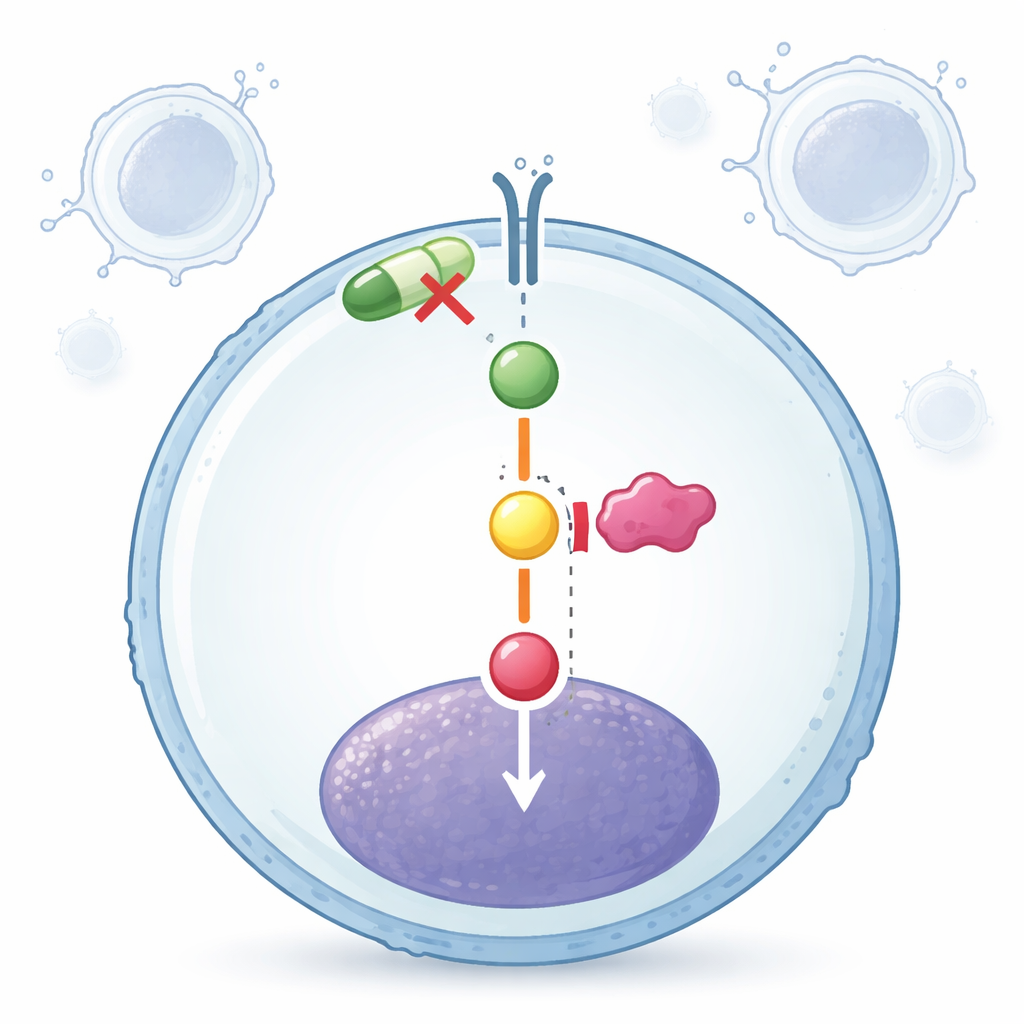
Quieting the Cancer’s Inner Conversation
Looking inside the cells, the scientists found that the total amount of key pathway proteins JAK2 and STAT5 stayed roughly the same after treatment. What changed was their activation state. Both drugs, alone and especially together, reduced the phosphorylated (switched‑on) forms of these proteins, effectively lowering the volume on the growth signal without altering how much of the proteins the cell produced. Artesunate and ruxolitinib also dampened certain inflammatory messengers linked to this pathway. The authors suggest that artesunate mainly acts on the proteins after they are made, while ruxolitinib directly blocks the JAK enzyme activity, and that hitting these different points in the same pathway explains their enhanced joint effect.
What This Could Mean for Patients
For now, these findings come entirely from dishes of leukemia cells and a small set of patient tissue samples, not from human trials. Even so, the work offers a clear message for non‑specialists: combining a repurposed anti‑malarial drug with a targeted signal blocker can more powerfully shut down a key growth pathway in T‑cell leukemia cells than either drug can alone. By selectively turning off the cancer’s internal instructions to grow and survive, this strategy hints at a future in which treatments are both more effective and potentially less harsh than current chemotherapy. To reach patients’ bedsides, however, the approach must still be tested in animal models, expanded to different leukemia cell types, and carefully evaluated in clinical studies to confirm its safety and real‑world benefit.
Citation: Yuan, Y., Li, Y., Li, J. et al. Combination of artesunate and ruxolitinib suppresses T cell leukemia/lymphoma proliferation via the JAK STAT pathway. Sci Rep 16, 8354 (2026). https://doi.org/10.1038/s41598-026-39393-8
Keywords: T-cell acute lymphoblastic leukemia, JAK-STAT signaling, artesunate, ruxolitinib, targeted combination therapy