Clear Sky Science · en
STYK1 expression in breast cancer and its association with vascular invasion and clinicopathological features
Why a blood vessel story matters in breast cancer
When breast cancer becomes life‑threatening, it is usually because cancer cells escape the original tumor and travel through blood or lymph vessels to other parts of the body. This study asks whether a little‑known protein, called STYK1, helps breast cancer cells invade these vessels. Understanding such a helper molecule could open doors to new tests that flag risk earlier and, eventually, to drugs that shut down one of cancer’s escape routes.
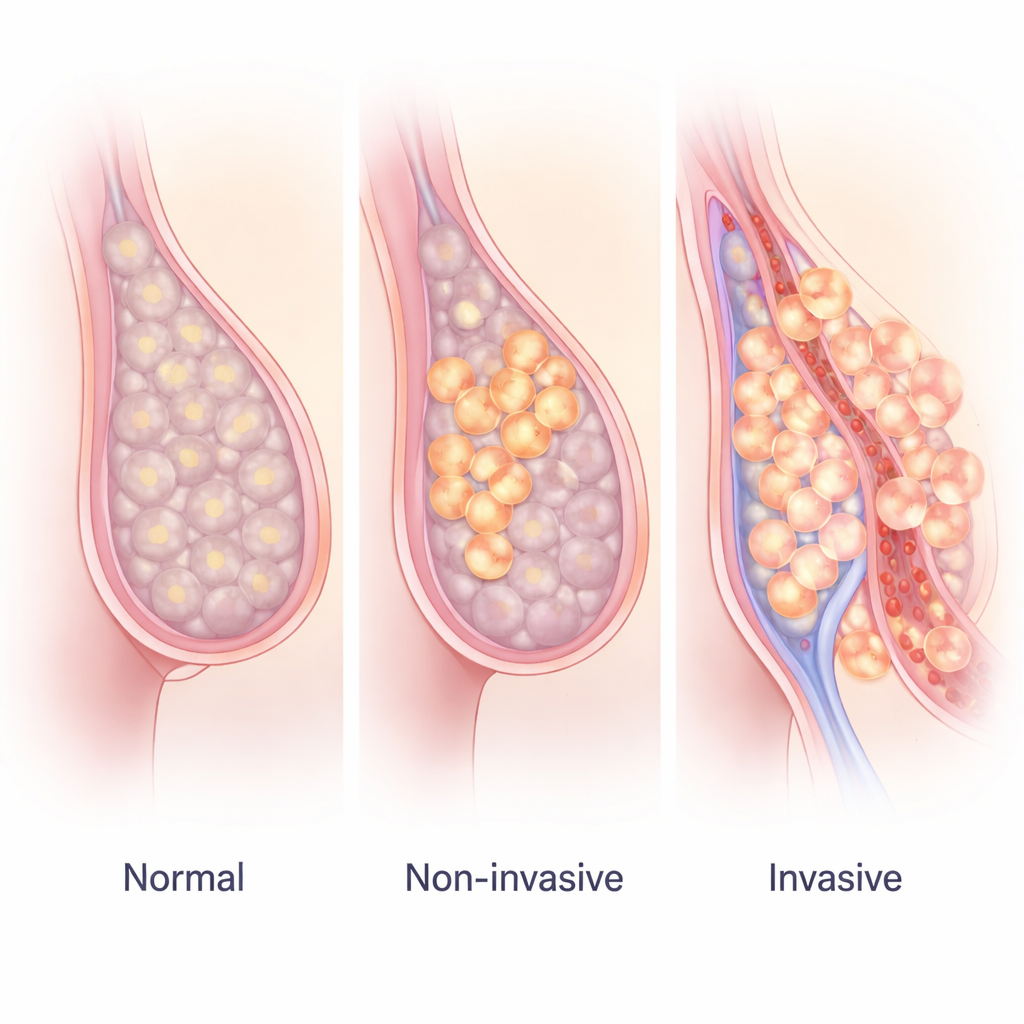
A closer look at an under‑the‑radar protein
STYK1 is part of a large family of “on” switches that sit on the surface of cells and react to growth signals. In several other cancers, high levels of STYK1 have been linked to faster growth, greater ability to spread, and poorer outcomes. However, very little was known about how often STYK1 appears in human breast tumors, whether it is tied to invasion of blood vessels, or how it relates to familiar markers such as hormone receptors or HER2.
Examining real patient tumors
The researchers studied tissue samples from 220 women with invasive breast cancer treated at a single medical center. Using a staining method that colors cells containing STYK1, they measured how strongly the protein was present in each tumor and in any nearby normal or non‑invasive (in situ) tissue. They then compared these scores with detailed information on tumor type, size, grade, stage, hormone receptor status, lymph node involvement, and 10‑year follow‑up, including whether the cancer came back or spread.
Where STYK1 shows up, invasion is more likely
STYK1 levels were clearly higher in invasive cancers than in normal breast tissue or non‑invasive lesions, suggesting a role in the step where tumors break through their natural boundaries. Tumors with high STYK1 were much more likely to have cancer cells inside blood or lymph vessels and to have already reached the lymph nodes. High STYK1 was also more common in tumors that carried estrogen receptors and in cancers that were not of the “triple‑negative” type. In contrast, STYK1 levels did not track with tumor size, grade, or HER2 status, hinting that its main role may be helping cells move and invade rather than simply grow faster.
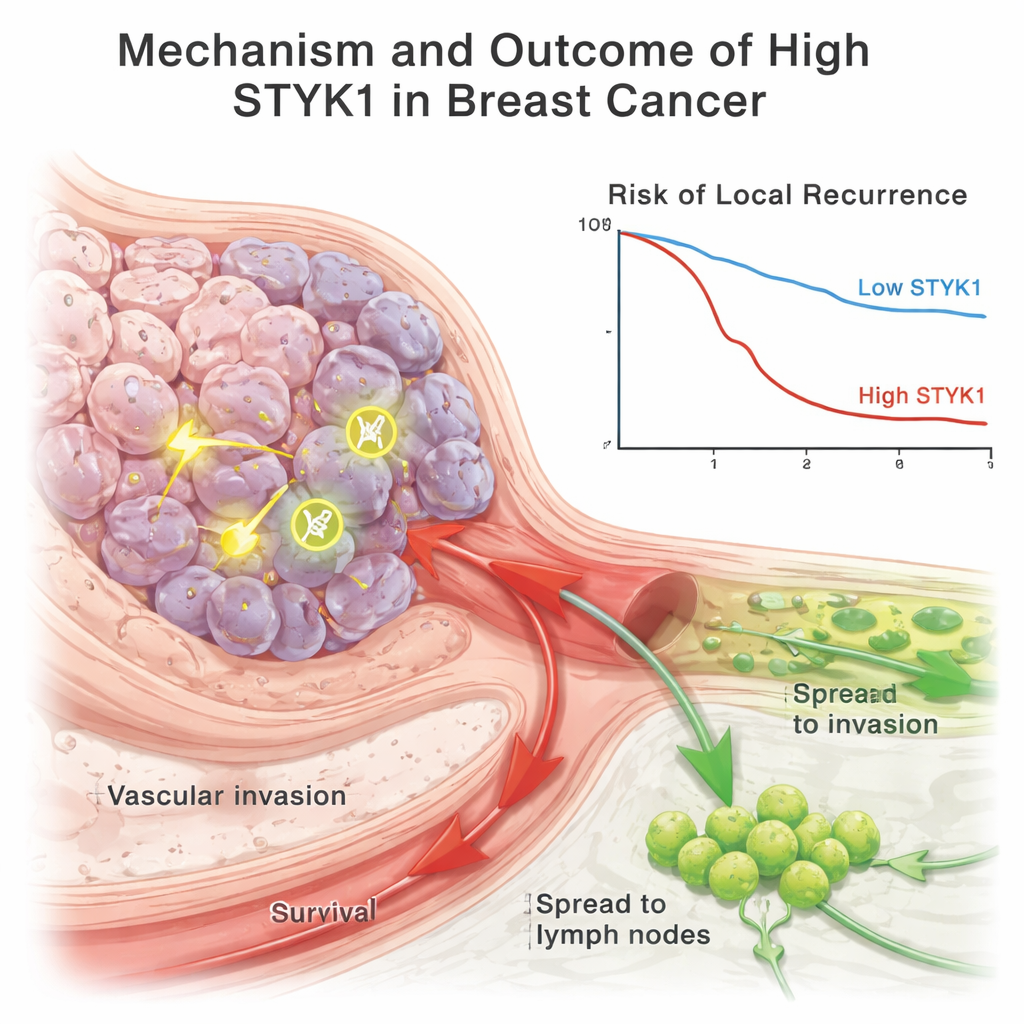
Links to cancer coming back, but not a perfect crystal ball
When the team looked at patient outcomes over time, women whose tumors had high STYK1 were more likely to develop a local or regional recurrence of their cancer. However, high STYK1 did not predict the development of distant metastases or overall survival on its own. A more detailed statistical test showed that STYK1, by itself, was only a weak predictor of remaining free of disease, meaning it cannot yet be used as a stand‑alone marker to guide treatment decisions.
What this could mean for future treatments
To a non‑specialist, the take‑home message is that STYK1 appears to be one of the tools breast cancer cells use to break into nearby vessels and to return after treatment. This makes it a promising target for future drugs designed to block invasion and reduce the chance of recurrence. The current work is an early but important step: it shows that STYK1 is often switched on in invasive breast cancers and that its presence goes hand in hand with vessel invasion and lymph node spread. Larger, multi‑center and experimental studies will be needed to confirm whether turning off STYK1 can truly help keep breast cancer from spreading.
Citation: Mohammed, R., Ismaeel, A., Alshaikh, S. et al. STYK1 expression in breast cancer and its association with vascular invasion and clinicopathological features. Sci Rep 16, 7775 (2026). https://doi.org/10.1038/s41598-026-39385-8
Keywords: breast cancer, STYK1, vascular invasion, biomarkers, targeted therapy