Clear Sky Science · en
The effect of macromolecular crowders as a supplement to serum free media on human corneal stromal cells proliferation and marker expression
Keeping the Window of the Eye Clear
The front of the eye, the cornea, must stay perfectly clear for us to see well. When it is scarred or clouded, people often need a corneal transplant—but donor tissue is in short supply worldwide. This study explores how to grow the cornea’s supporting cells in the lab under cleaner, safer conditions that avoid animal serum, while still keeping the cells in a healthy, native‑like state. The work could help pave the way for lab‑grown corneal tissue to repair or even replace damaged human corneas.
Why Lab-Grown Corneal Cells Matter
The cornea’s strength and transparency depend on a layer of cells called stromal keratocytes and on the orderly collagen matrix they build around themselves. In the body, these cells are usually quiet, with a branched shape and a low level of activity that preserves clarity. Standard lab methods rely on animal serum to make cells multiply, but serum tends to push keratocytes into a wound‑healing, scar‑forming state that is very different from their natural role. To make reliable cell therapies, researchers need culture conditions that both expand cell numbers and keep their native, non‑scarring behavior.
Using Crowded Spaces Instead of Serum
Inside the body, cells live in a tightly packed environment full of large molecules. This natural crowding helps proteins fold, signals move, and the surrounding matrix assemble properly. The authors mimicked this by adding macromolecular crowders—large, inert molecules optimized for corneal cells—to serum‑free culture media. They grew human corneal stromal cells from donor tissue in two types of sugar conditions: a standard, high‑glucose medium commonly used in labs, and a lower‑glucose medium closer to the levels found in the human cornea. Each was tested with 0%, 4%, or 8% crowder and compared with traditional serum‑containing controls. 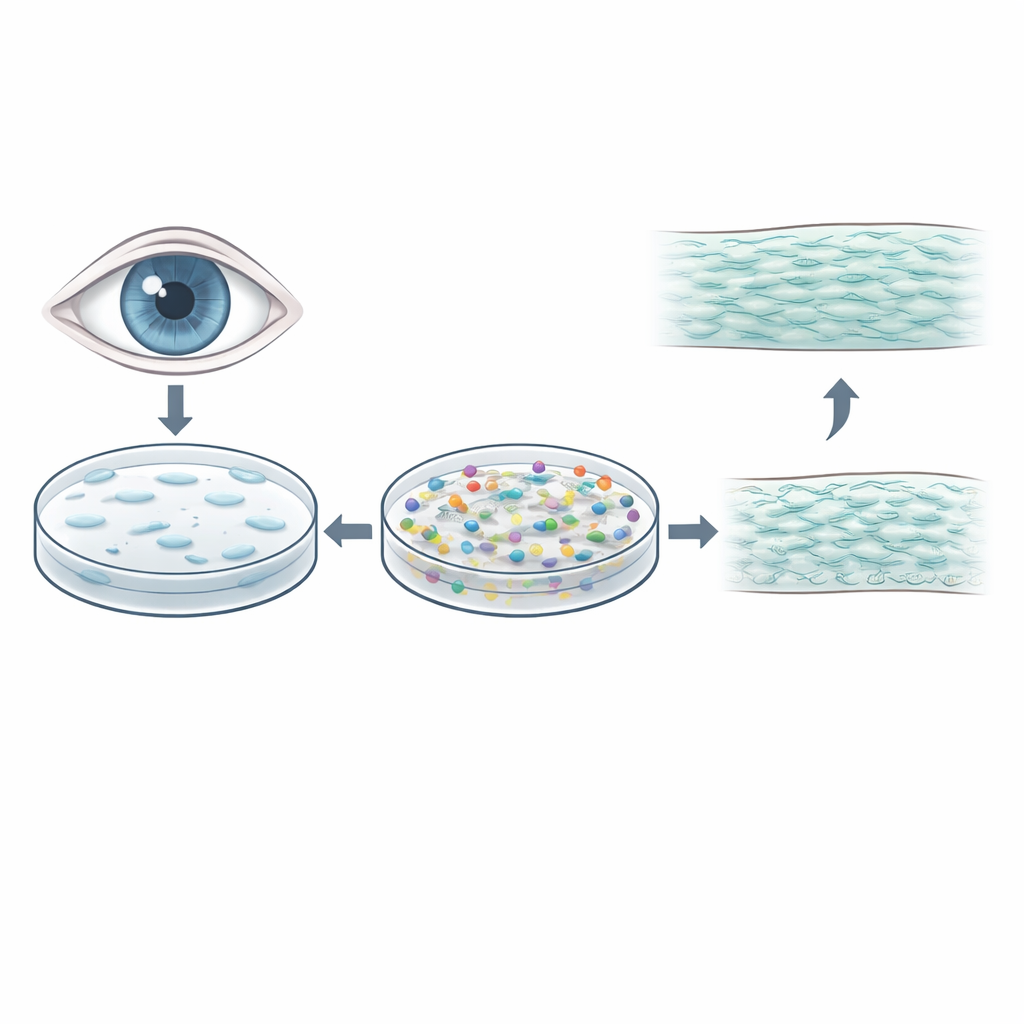
How the Cells Responded
Across both glucose conditions, adding crowders improved cell metabolic activity over three weeks compared with serum‑free media alone. In standard high‑glucose medium, 4% and 8% crowder supported sustained growth, and higher crowder levels boosted production of collagen V, a key ingredient of the corneal scaffold. However, this energetic environment also increased the risk that cells would drift toward a more activated, fibroblast‑like state. By contrast, in low‑glucose medium the cells stayed more subdued overall, and crowders mainly helped prevent their activity from collapsing over time rather than driving strong expansion.
Signs of Healthy Versus Scar-Forming Cells
The team tracked molecules that distinguish quiet, native‑like keratocytes from scar‑forming cells. A protective enzyme called ALDH3A1 and collagen V signaled a desirable, quiescent state, while α‑smooth muscle actin and the enzyme MMP2 are associated with wound‑healing and tissue remodeling. In both glucose settings, crowder‑supplemented, serum‑free cultures showed higher levels of the “good” markers and much lower levels of the “scar” markers than serum‑grown controls. Serum‑treated cells adopted a bulky, fibroblastic shape and strongly expressed α‑smooth muscle actin and MMP2. In contrast, crowder‑treated cells kept a branched, dendritic look, and α‑smooth muscle actin was essentially undetectable, suggesting a safer, more native‑like behavior for regenerative use. 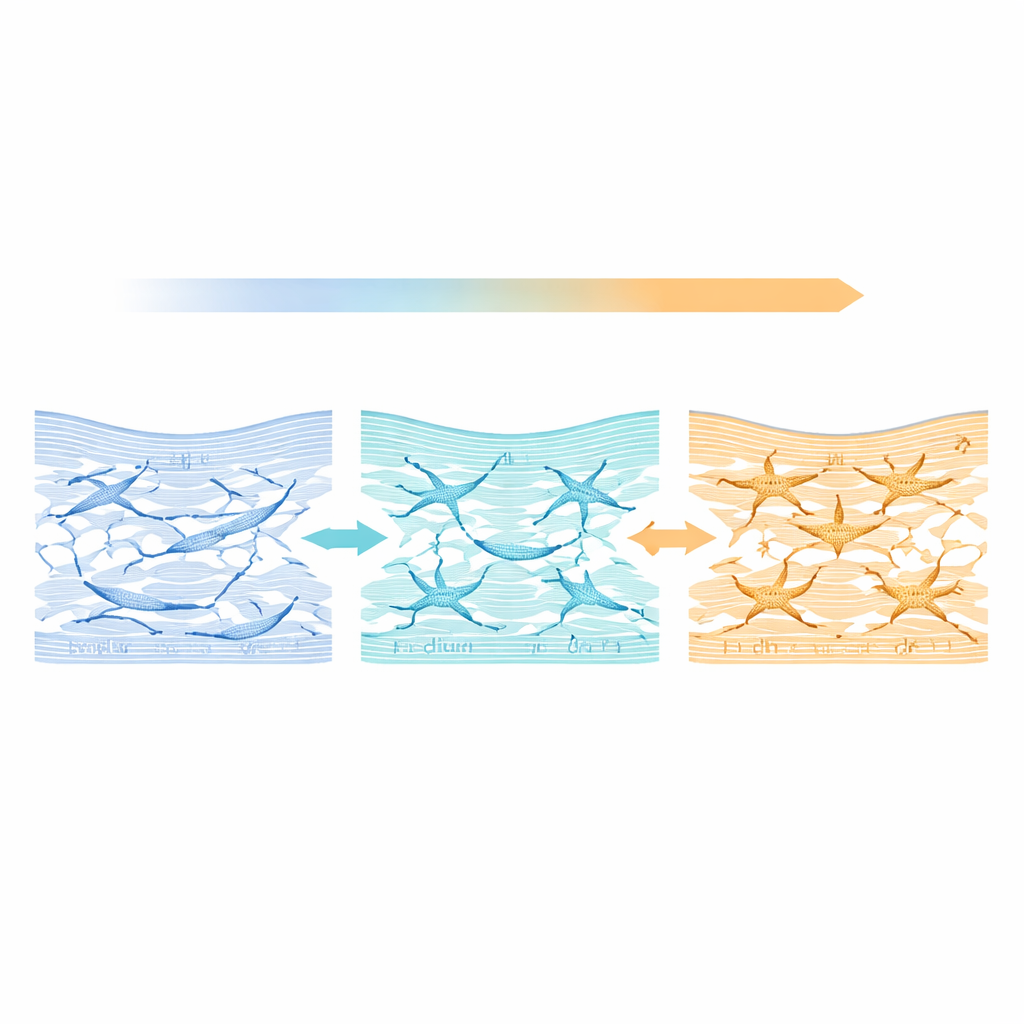
Finding the Right Balance for Therapy
The results show that macromolecular crowders can replace many of the benefits of serum—especially supporting cell survival and collagen production—while better preserving the cornea’s natural cell identity. Yet the surrounding sugar level matters: high glucose favors faster growth and stronger matrix deposition but can edge cells toward activation, while lower glucose better matches the natural corneal environment and supports a stable, quiet phenotype. For future corneal repair strategies, this work suggests that tuning both crowding and glucose can help strike the desired balance between expanding enough cells and keeping them in a form that maintains clarity rather than causing scarring.
What This Means for Future Eye Treatments
For a non‑specialist, the key message is that researchers are learning how to grow corneal cells in a lab in ways that more closely mimic the body, without relying on animal‑derived serum. By crowding the culture medium with large molecules and adjusting sugar levels, they can both nurture these delicate cells and keep them in a clear‑preserving, non‑scar‑forming state. This approach brings us a step closer to producing lab‑grown corneal tissue that could safely restore sight for people who currently have to wait for scarce donor corneas.
Citation: Sultan, W.A., Connon, C.J. The effect of macromolecular crowders as a supplement to serum free media on human corneal stromal cells proliferation and marker expression. Sci Rep 16, 9415 (2026). https://doi.org/10.1038/s41598-026-39340-7
Keywords: corneal regeneration, cell culture, serum-free media, macromolecular crowding, tissue engineering