Clear Sky Science · en
Early chest x-ray severity assessed by the MBrixia score is associated with mortality in hospitalized patients with COVID-19 pneumonia
Why chest X-rays still matter in COVID-19 care
Even as vaccines and antiviral drugs have changed the course of the COVID-19 pandemic, doctors still need simple tools to tell which hospitalized patients are most at risk. Chest X-rays are cheap, fast and available almost everywhere, but turning a grey, streaky image into a reliable measure of danger is not straightforward. This study asks whether a detailed scoring system applied to early chest X-rays can help predict how severely a person will fare and whether they are more likely to die within three months of being admitted to the hospital.
Turning X-ray pictures into a risk scale
The researchers focused on a system called the MBrixia score, which breaks each lung X-ray into 12 small zones and grades how badly each zone is affected, from clear to heavily clouded. The scores from all zones are added up to a total between 0 and 36, with higher numbers reflecting more widespread lung damage. Unlike many earlier studies done before modern COVID-19 treatments became routine, this work looked at patients treated after steroids and antiviral drugs such as remdesivir had become standard care. Adults hospitalized with COVID-19 at a large Danish hospital from mid-2020 to early 2021 were included if they had at least one chest X-ray during their stay, and a subgroup had an X-ray within the first two days of admission for focused analysis of early risk.
Linking X-ray scores to breathing support and blood tests
Across 279 patients and over 600 scored X-rays, the team examined how MBrixia scores matched up with the help patients needed to breathe. They found a clear stepwise pattern: people who breathed room air had the lowest average scores; those needing small amounts of oxygen had higher scores; those needing larger flows higher still; and patients in intensive care had the highest scores. The researchers also compared the X-ray scores with 15 common blood markers used to track inflammation and organ stress. Nine of these, including measures such as C-reactive protein, ferritin, D-dimer and lactate dehydrogenase, rose in tandem with MBrixia scores, while albumin and hemoglobin tended to fall as the score climbed, reinforcing that the X-ray measure reflected overall illness severity.
How well do doctors agree on the score?
Because any scoring system is only as good as its consistency, three radiologists with different levels of experience independently scored a set of admission X-rays. Agreement between them was moderate: they usually placed patients in similar ranges but did not match perfectly, especially when lungs were badly affected. Senior radiologists tended to give slightly higher scores than the trainee, and differences grew at the high end of the scale. These findings highlight both the usefulness and the human limits of manual scoring, and they suggest that computer-based tools might eventually help standardize scores, provided they are trained on high-quality human ratings.
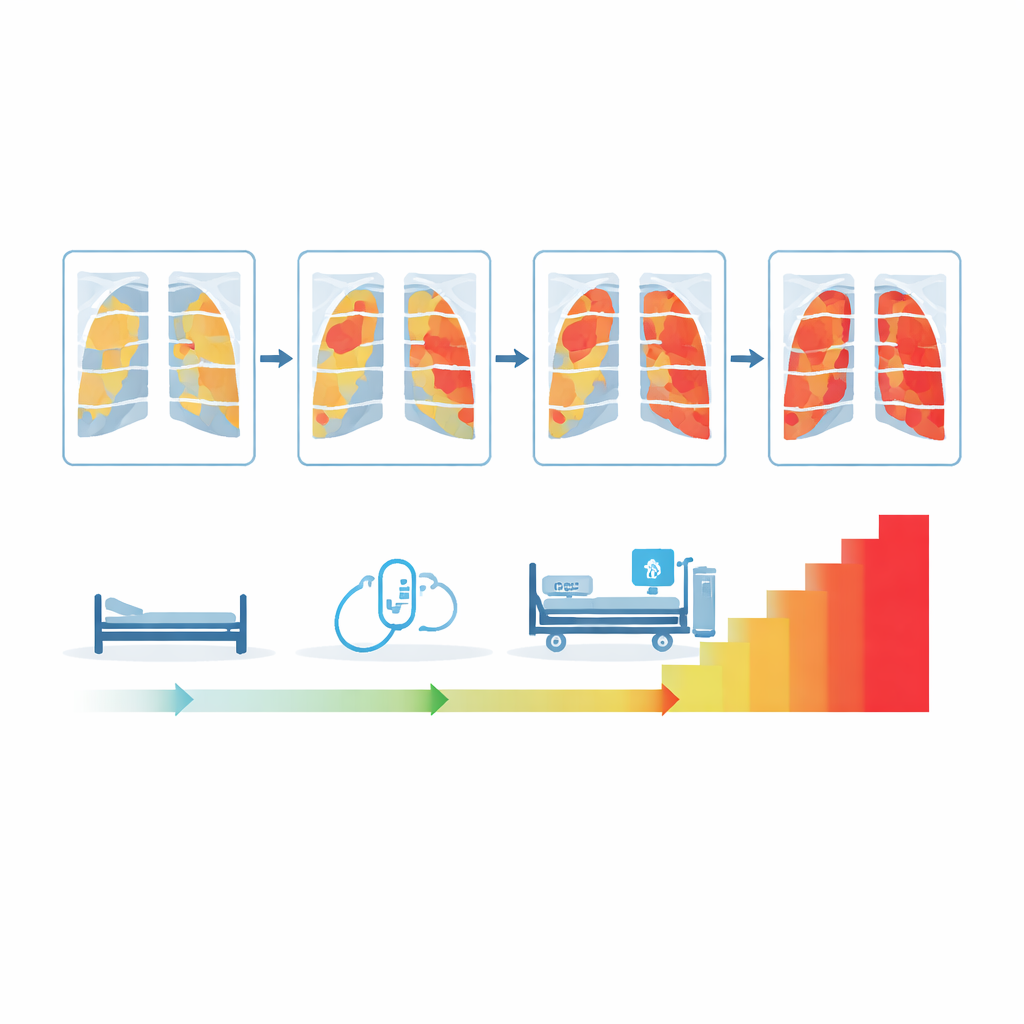
Early X-ray damage and the risk of death
The heart of the study was whether the first X-ray taken around the time of hospitalization could forecast who would die within 90 days. Among 251 patients with such early X-rays, no one had the very highest score range, but many fell into low (0–9), medium (10–18) or high (19–27) bands. After accounting for age, existing health problems and immune status, patients whose initial score landed in the highest observed band had about three times the risk of dying within 90 days compared with those in the lowest band. Similar patterns appeared when the researchers looked at the worst X-ray score reached at any point during the hospital stay: patients whose scores climbed into the top ranges faced a sharply higher death risk.
What this means for patients and future care
To a layperson, the message is that how cloudy the lungs look on a carefully scored chest X-ray still carries powerful information about the likely course of COVID-19, even in an era of better treatments. The MBrixia score offers a way to turn a fuzzy image into a number that reflects how sick the lungs are and how much danger the patient may face. While the method is not perfect and depends on who reads the image, it can help doctors identify high-risk patients early, guide decisions about monitoring and treatment, and support research. The authors note that newer virus variants, widespread vaccination and changing therapies may alter the landscape, so the score will need fresh testing in modern patient groups. Still, as a simple, widely accessible tool, an early X-ray severity score remains a promising guidepost in managing severe lung infections like COVID-19.
Citation: Jensen, C.M., Marandi, R.Z., Costa, J.C. et al. Early chest x-ray severity assessed by the MBrixia score is associated with mortality in hospitalized patients with COVID-19 pneumonia. Sci Rep 16, 8309 (2026). https://doi.org/10.1038/s41598-026-39285-x
Keywords: COVID-19 pneumonia, chest X-ray, risk prediction, lung severity score, hospital outcomes