Clear Sky Science · en
Integrative framework for cancer detection via integro-differential equations using deep learning techniques
Why Smarter Scans Matter
Finding cancer early can save lives, but reading medical scans like mammograms is difficult, time‑consuming, and prone to human error. Doctors must distinguish faint patterns of disease from normal tissue and image noise, often under tight time pressure. This paper presents a new way to help: it turns complex breast images into simpler one‑dimensional signals, then uses both mathematics and artificial intelligence to decide whether cancer is likely present. The goal is not to replace doctors, but to give them clearer, more reliable clues hidden inside each scan.
Turning Pictures into Signals
The authors start by rethinking how a medical image is represented. Instead of treating a mammogram as a giant grid of pixels, they convert it into a single line‑like signal that summarizes how brightness changes across the breast. First, the image is cleaned: converted to shades of gray, denoised, and intensity‑balanced so that dark and bright regions are comparable. Edges and textures are emphasized using standard filters, and the overall pattern of light and dark is analyzed in terms of its frequencies (similar to how audio is split into bass and treble). Then, pixel values are averaged row by row or column by column to produce a smooth one‑dimensional curve. Peaks in this curve reflect dense tissue or suspicious regions; valleys reflect emptier areas. Although some fine detail is lost, the result is a compact signal that still preserves the broad structures most relevant for diagnosis. 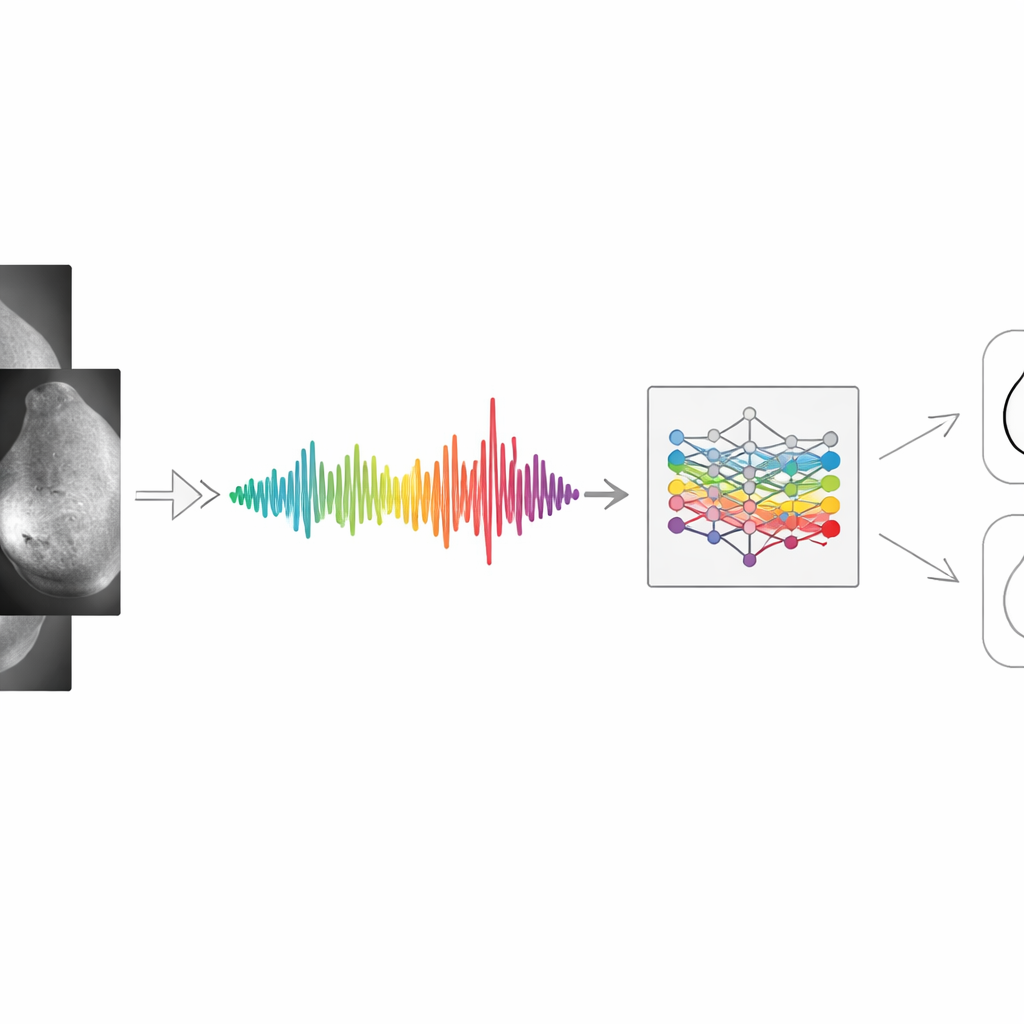
Adding a Layer of Biology with Equations
Many current deep learning systems work directly on images and are often criticized as "black boxes" that offer little insight into how tumors actually behave. To address this, the authors embed mathematical models of tumor growth into their signal pipeline. They use integro‑differential equations—equations that describe how something changes over time while also remembering its past—to mimic how cancer cells multiply, spread, and draw blood supply. These equations include terms for growth rate, crowding limits, cell movement, and the formation of new blood vessels. By simulating how a tumor might evolve and influence the brightness pattern in a mammogram, the framework produces extra features grounded in known biology, not just in pattern recognition. These enriched signals aim to make the final predictions more interpretable to clinicians.
Teaching a Compact Neural Network to Decide
Once the image has been turned into a mathematically enriched signal, a streamlined one‑dimensional convolutional neural network (CNN) performs the actual classification. This network slides small filters along the signal to detect telling shapes—sharp jumps, smooth ramps, or repeated ripples—that could indicate abnormal tissue. The model is trained on publicly available mammography datasets (INbreast and MIAS), with the data split into training, validation, and testing portions to prevent overfitting. The authors augment the signals and carefully tune model settings to improve robustness. To open the black box further, they apply explainability tools that highlight which parts of the signal most influenced the decision, linking them back to regions in the original breast image where tissue density or boundaries changed in a suspicious way. 
How Well It Works in Practice
In tests on these real‑world mammogram collections, the integrative framework correctly distinguished cancerous from non‑cancerous cases about 96.4% of the time, outperforming standard CNNs, support vector machines, decision trees, and several modern deep learning baselines. It also showed high sensitivity, meaning most cancers were successfully detected, and strong specificity, meaning healthy patients were less likely to be flagged by mistake. Because the system works on 1D signals rather than full images, it requires less memory and can deliver predictions faster than many heavy image‑based networks, which is important for use in busy clinics or on modest hardware. The added mathematical modeling appears to sharpen the features that matter, improving accuracy without an extreme computational cost.
Where This Could Lead Next
The authors conclude that combining image‑to‑signal conversion, mathematical models of tumor growth, and deep learning offers a promising path toward more accurate and understandable cancer screening tools. Their approach is still in an early stage: it has been validated mainly on breast images, and some fine‑grained visual details may be lost during signal conversion. Future work will test the method on other cancers, add richer forms of explanation for doctors, and blend in additional data such as tissue slides, clinical markers, and genetic information. With broader validation, this kind of mathematically informed AI could eventually support real‑time decision systems that help radiologists catch cancers earlier and with greater confidence.
Citation: Gopisairam, T., Thota, S. & Bikku, T. Integrative framework for cancer detection via integro-differential equations using deep learning techniques. Sci Rep 16, 9714 (2026). https://doi.org/10.1038/s41598-026-39283-z
Keywords: cancer detection, medical imaging, deep learning, mathematical modeling, breast mammography