Clear Sky Science · en
Feasibility of multisource CBCT for improving the predictability of dental implant primary stability compared to conventional CBCT
Stronger Foundations for Dental Implants
When someone receives a dental implant, the hidden key to long-term success is how firmly that implant grips the surrounding bone on the day it is placed. Dentists try to predict this “first-day stability” using 3D x-ray scans, but today’s scanners often give fuzzy, unreliable numbers. This study explores a new kind of dental scanner that may allow dentists to measure bone quality more accurately, choose implant sites with greater confidence, and reduce the risk of early implant problems.
Why Bone Quality Matters
Dental implants have become an everyday solution for missing teeth, and their use is expected to keep rising. For an implant to last, it must lock tightly into the jawbone so that bone can grow onto its surface over time. That initial grip—called primary stability—depends largely on how dense and strong the nearby bone is. In medical imaging, bone density is often estimated using a CT-based value called the Hounsfield Unit, or HU, which scales with how much mineral is packed into the bone. In hospitals, specialized CT scans can measure this reliably, but those machines are expensive, expose patients to higher radiation doses, and are rarely found in dental offices.
The Limits of Today’s Dental 3D Scans
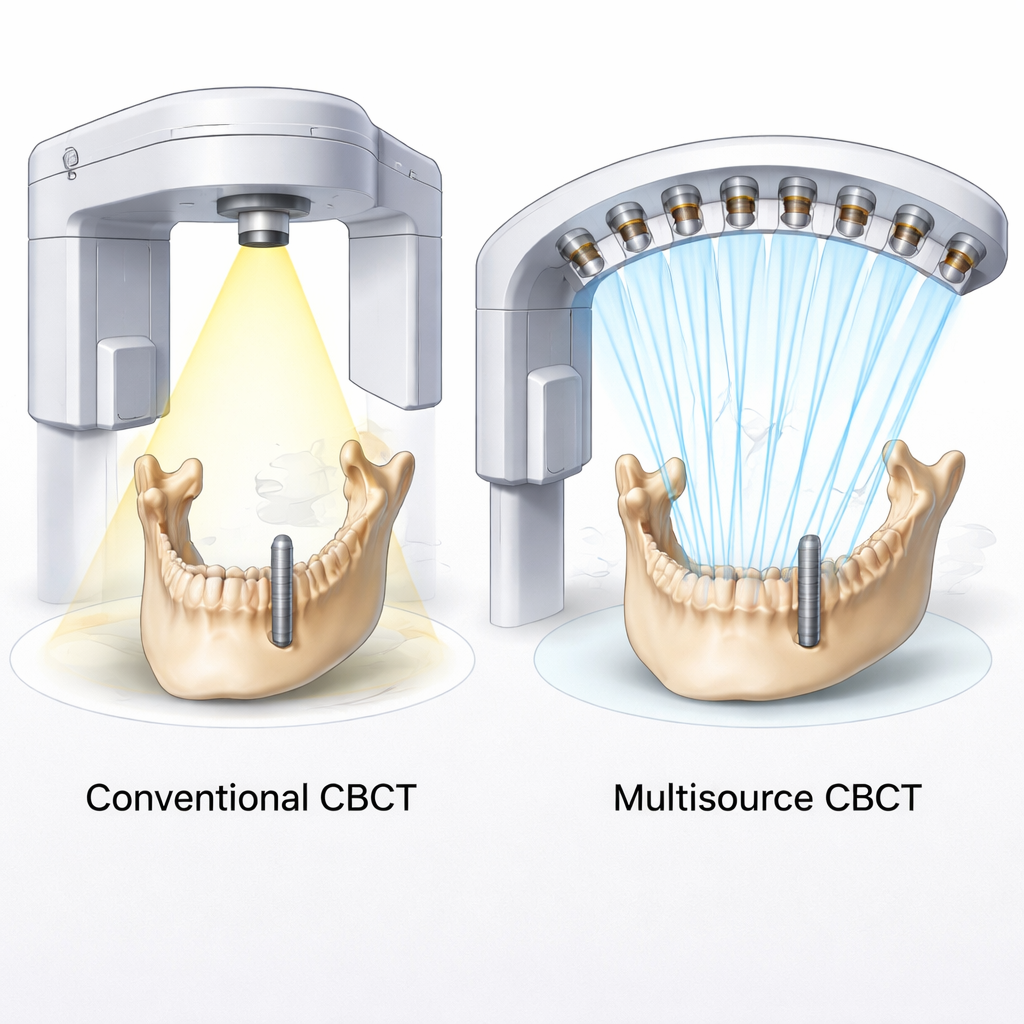
Most dentists instead use cone beam CT (CBCT), a more compact 3D x-ray system designed for the mouth and jaw. In theory, CBCT images could provide HU-like values to judge bone quality before placing an implant. In practice, however, current CBCT machines struggle to measure HU accurately. Their wide x-ray beams scatter heavily inside the head, and the geometry of the scan creates image distortions and missing information. As a result, the same piece of bone can show very different HU-like numbers depending on its position or the scan settings. Previous studies trying to link CBCT-based bone values to how stable implants actually were have found everything from no correlation to only weak or inconsistent relationships.
A New Way to Shine X-rays
The research team tested a new approach called multisource CBCT (ms-CBCT). Instead of a single x-ray tube that floods the whole jaw with a broad cone of radiation, this system uses an arc of eight tiny x-ray sources based on carbon nanotube technology. Each source fires a narrow beam that covers only a thin “slice” of the object, and the beams are switched on one after another as the device rotates. Together, they build up a full 3D picture while greatly reducing scattered radiation and common cone-beam distortions. Earlier phantom studies showed that this design could match or approach the accuracy of hospital CT scanners for measuring bone density, without increasing radiation dose.
Testing the New Scanner in a Lab Model
To see whether ms-CBCT could better predict real implant stability, the researchers worked with four porcine (pig) thigh bones, which have dense outer bone similar to human jawbone. They placed twelve identical titanium implants following standard clinical drilling steps and recorded the maximum insertion torque—the peak twisting force needed to seat each implant—using a digital torque wrench. Higher torque reflects better primary stability. Each bone was scanned twice on the same benchtop device: once in the new multisource mode and once in a conventional single-source mode that mimicked a standard dental CBCT. In the resulting 3D images, software identified the implant and measured the average HU in a thin shell of dense outer bone surrounding each implant, for both scan types.
Clearer Numbers, Clearer Predictions
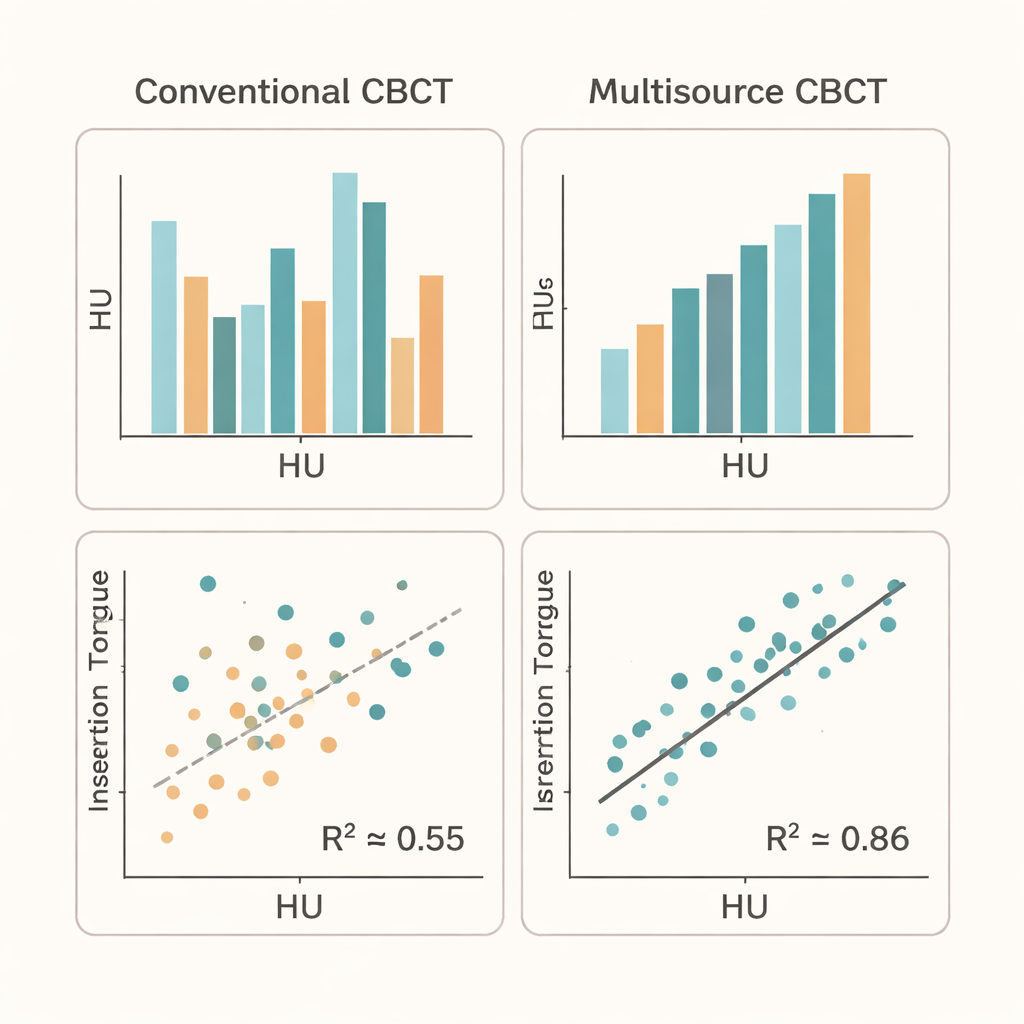
When the team compared bone HU values with insertion torque, they found a striking difference between the two scan modes. For the multisource CBCT, the relationship was strong and statistically significant: implants in denser bone consistently showed higher torque, with a coefficient of determination (R²) of about 0.86. For the conventional CBCT configuration, the correlation was only moderate (R² about 0.55), in line with the mixed results reported in earlier studies. The conventional scans also tended to underestimate bone density compared with the multisource scans, likely reflecting the impact of scattered x-rays and image artifacts. Notably, simple measurements of bone thickness did not predict stability in this experiment, underscoring that accurate density measurement is crucial.
What This Could Mean for Patients
This early laboratory study, though small and carried out in animal bone, suggests that multisource CBCT can provide cleaner, more trustworthy bone density numbers that mirror how stable implants actually are. If confirmed in human jaws and larger patient groups, such scanners could help dentists better judge where and how to place implants, personalize treatment to each patient’s bone quality, and potentially reduce failures—all without extra radiation compared to current devices. In short, by sharpening the imaging tool dentists already rely on, multisource CBCT may offer a more solid foundation for the next generation of dental implants.
Citation: Luo, W., Hu, Y., Stadler, A.F. et al. Feasibility of multisource CBCT for improving the predictability of dental implant primary stability compared to conventional CBCT. Sci Rep 16, 7700 (2026). https://doi.org/10.1038/s41598-026-39266-0
Keywords: dental implants, bone density, cone beam CT, multisource CBCT, implant stability