Clear Sky Science · en
Analysis of interception problems in donning and doffing personal protective equipment in a large cabin hospital during the COVID-19 pandemic: a real world study
Why the Way We Wear Protective Gear Matters
When COVID-19 swept through cities, many people with mild infections were treated in huge temporary “cabin” hospitals. Inside these facilities, doctors, nurses, cleaners, and security guards relied on layers of masks, gowns, gloves, and face shields to stay safe. This study looked closely at how often people made mistakes when putting on and taking off this protective gear—and where those mistakes happened. Understanding these weak spots can help keep frontline workers safer in future outbreaks, and indirectly protect patients and the wider community.
Life and Work Inside a Giant Temporary Hospital
In spring 2022, Shanghai faced a massive wave of infections from the Omicron variant. To handle the surge, authorities set up large mobile cabin hospitals, each with thousands of beds for people with mild or no symptoms. In one such hospital with 1,240 beds, every person entering or leaving the areas where patients stayed had to put on (don) and remove (doff) personal protective equipment, or PPE. This included protective clothing, respirators, gloves, caps, shoe covers, and face shields. A team of infection control supervisors watched these steps around the clock and recorded every time they had to step in and correct a problem—what the researchers called “interception problems.” 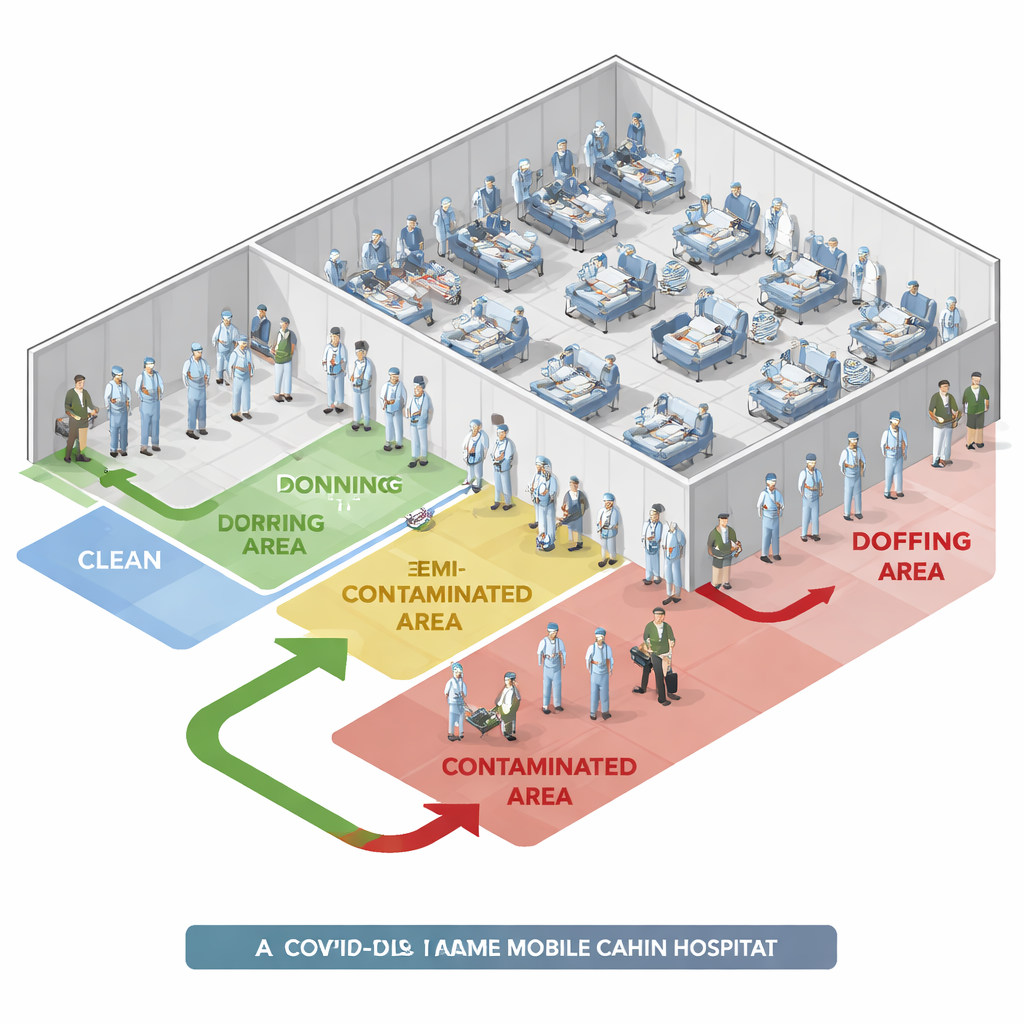
Where Mistakes Happen Most Often
Over about one month, staff carried out 9,177 PPE procedures: 4,652 times putting gear on and 4,525 times taking it off. Overall, mistakes were more common when taking PPE off than when putting it on. About 5 out of every 100 donning procedures had a problem, compared with more than 8 out of every 100 doffing procedures. The riskiest group was not doctors or nurses, but the non-medical workers who keep the hospital running—cleaners, security guards, and maintenance staff. For them, roughly one in five doffing attempts involved some kind of error. Even though everyone had been trained, the stress of working in a high-risk environment, unfamiliar routines, and different educational backgrounds all likely contributed to these figures.
The Trouble Spots in Protective Gear
Most problems involved protective clothing and respirators. When putting gear on, the most frequent issue was loose fabric around the head and neck, leaving bits of skin exposed that viruses could reach. There were also cases of ill-fitting suits, damaged zippers or seams, and clothing that bunched up and covered the face or mask. With respirators, many workers either failed the seal test—a simple check to see if air leaks around the edges—or ended up with masks that shifted or became deformed. Gloves and face shields caused fewer problems, but there were still instances of torn gloves, tape wrapped too tightly, and face shields placed incorrectly or used with their protective film still attached. 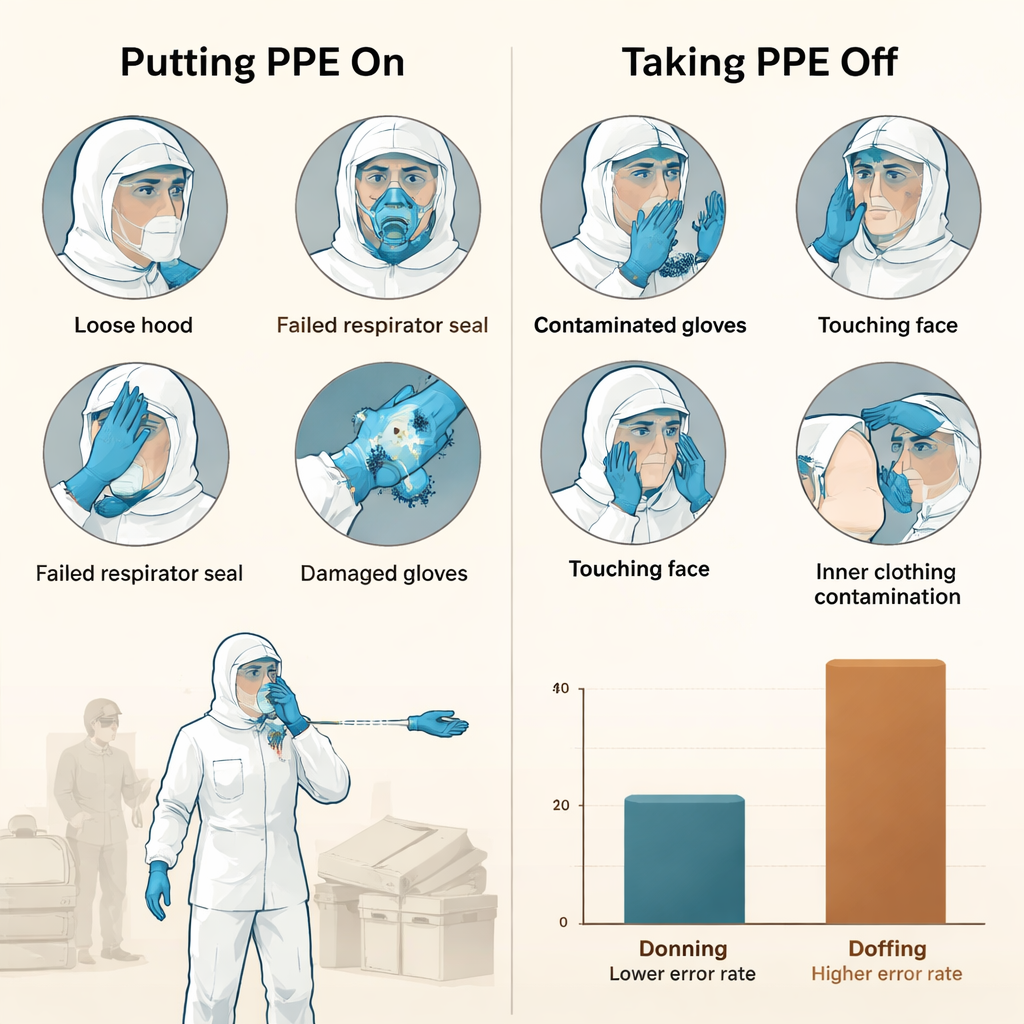
Taking Gear Off: The Most Delicate Moment
The biggest vulnerabilities appeared when staff removed their PPE, the moment when the outer layers are likely contaminated. A common error was contaminating the inside of the protective suit while peeling it off, or soiling the inner clothing or socks. For respirators, masks sometimes slipped or touched clean clothing during removal. Many workers also performed hand hygiene steps poorly or inconsistently, increasing the chance that germs on the outside of gloves or clothing could reach their skin. Items like inner caps, shoe covers, and personal belongings sometimes fell to the floor mid-process, adding to the confusion. These findings make clear that doffing is a complex, high-stress sequence where even small missteps can defeat the purpose of the gear.
Turning Data Into Better Protection
By mapping out exactly where and how PPE errors occurred, this study gives hospital leaders a practical guide for improving safety. Instead of offering the same generic training to everyone, they can focus on the highest-risk steps—especially taking PPE off—and on groups that need the most support, such as cleaners and security staff. The authors suggest targeted drills, mirror-based self-checks, repeated practice of mask seal tests, and supervised “buddy” systems during doffing. For a layperson, the key message is simple: protective gear is only as good as the way it is used. Careful design of training and supervision can greatly reduce the chances that the people we rely on most during outbreaks will themselves become infected.
Citation: Li, Z., Tang, C., Zang, F. et al. Analysis of interception problems in donning and doffing personal protective equipment in a large cabin hospital during the COVID-19 pandemic: a real world study. Sci Rep 16, 7764 (2026). https://doi.org/10.1038/s41598-026-39259-z
Keywords: personal protective equipment, COVID-19, mobile cabin hospitals, healthcare worker safety, infection control training