Clear Sky Science · en
Pharmacological evaluation of a Brucine-loaded nanoemulgel for enhanced wound healing through in-silico and in-vivo investigations
Why slow-healing wounds matter
For many people with diabetes, even a small cut on the foot or leg can turn into a stubborn wound that refuses to heal. These chronic wounds are painful, prone to infection, and can, in severe cases, lead to amputation. The study behind this article explores a new gel-based treatment that packages a plant-derived compound into tiny droplets, aiming to help damaged skin close faster and more completely.
A plant ingredient with hidden promise
The researchers focused on brucine, a natural substance found in the seeds of the tree Nux vomica. In the laboratory, brucine is known to calm inflammation, neutralize harmful oxygen by-products, and encourage the growth of fibroblasts—cells that lay down the scaffolding of new tissue. Unfortunately, brucine does not dissolve well in water and can be toxic if it spreads widely through the body, which has limited its medical use. The team set out to see whether enclosing brucine inside a modern skin-friendly formulation could keep its benefits, reduce its risks, and turn it into a useful treatment for hard-to-heal wounds.
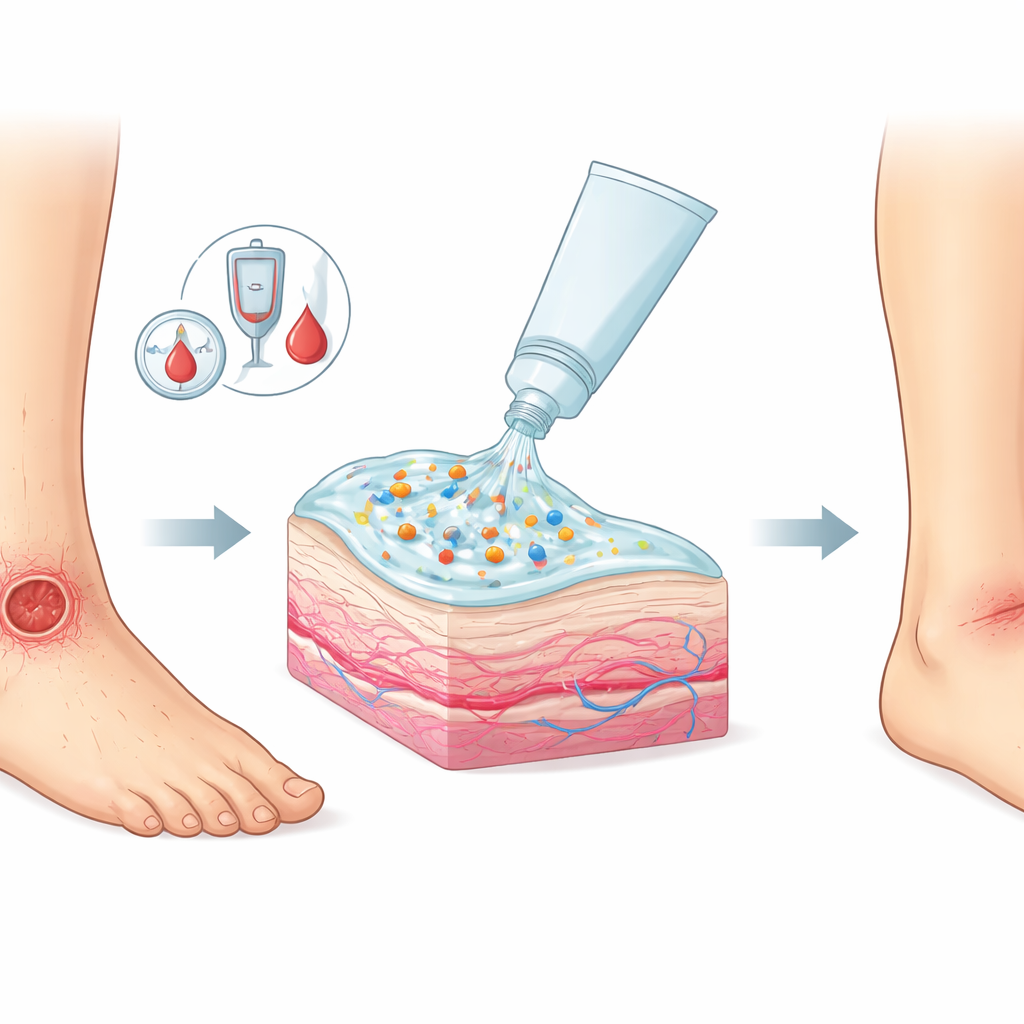
Designing a smarter skin gel
To do this, the scientists built a “nanoemulgel,” a hybrid that combines a traditional gel with a very fine oil-in-water mixture. In this system, brucine sits inside tiny oil droplets—less than a thousandth of a millimeter across—dispersed within a soft, spreadable gel. The droplets help dissolve the oily drug and nudge it through the outer layers of the skin, while the gel keeps the medicine in close contact with the wound for hours. The team carefully measured the size and uniformity of these droplets, their electrical charge, and how easily the gel spreads. They found that the nanoemulgel formed smooth, stable, nanosized spheres with good spreadability and skin-compatible acidity, all signs that it should apply easily and stay where it is needed.
Checking how brucine talks to healing signals
Before testing on animals, the researchers used computer models to predict how brucine might interact with key proteins that orchestrate wound repair. These virtual “docking” experiments suggested that brucine snugly fits into receptors that drive cell growth and tissue rebuilding, particularly those that guide fibroblast activity and skin cell renewal. It also showed interactions with proteins involved in reshaping the tissue scaffold and tuning inflammation. Together, these findings supported the idea that brucine could push wounds through the stalled inflammatory stage and into active rebuilding, especially in the difficult environment created by diabetes.
Putting the new gel to the test
The real-world challenge came from diabetic rats, whose wounds heal slowly in ways similar to human diabetic ulcers. The animals were divided into several groups: some were left untreated, some received a standard antiseptic ointment, some got a simple brucine gel, and others were treated with either a brucine emulgel or the new brucine nanoemulgel. Over two weeks, the researchers tracked how quickly the wounds shrank and examined tissue samples under the microscope. Wounds treated with the brucine nanoemulgel closed the fastest, with about four-fifths of the original area gone by day 14—better than both the standard treatment and the plain brucine gel. Microscopic views showed thicker, better-organized collagen fibers, more fibroblasts, new blood vessels, and fewer inflammatory cells in the nanoemulgel group, indicating more complete and orderly repair.
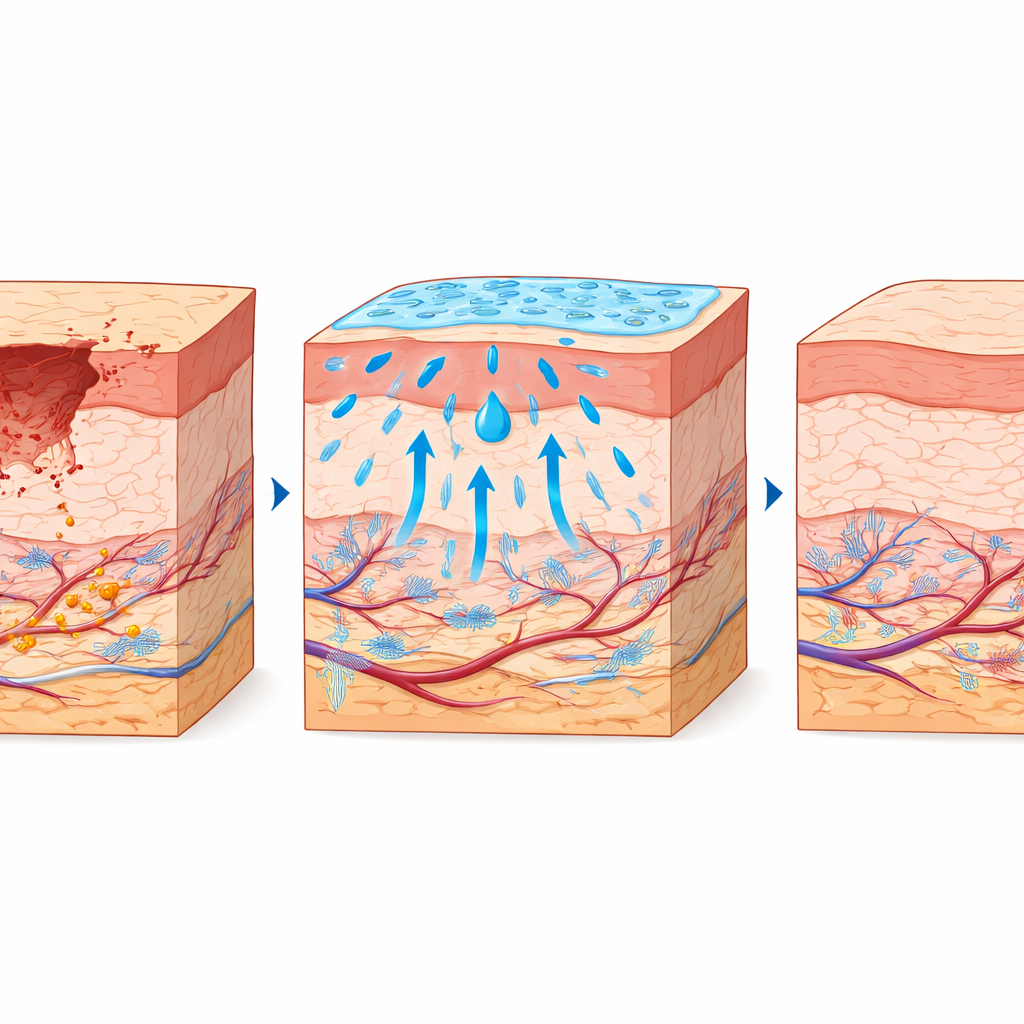
What this could mean for future care
The work suggests that wrapping brucine inside a nanoemulgel can overcome its poor solubility, keep it at the wound surface, and harness its healing-friendly actions while reducing concerns about whole-body exposure. For people living with diabetes, such a topical treatment could one day offer a more effective way to close chronic wounds, limit infections, and preserve limb function. The authors stress that more studies are needed—especially long-term safety tests and clinical trials in humans—but their results highlight how nanotechnology and natural compounds can be combined to tackle one of the most persistent problems in modern medicine: getting stubborn wounds to finally heal.
Citation: Vasudevan, R., Narayanan, J., Aldahish, A. et al. Pharmacological evaluation of a Brucine-loaded nanoemulgel for enhanced wound healing through in-silico and in-vivo investigations. Sci Rep 16, 9304 (2026). https://doi.org/10.1038/s41598-026-39194-z
Keywords: diabetic wound healing, topical nanoemulgel, brucine, skin regeneration, nanotechnology in medicine