Clear Sky Science · en
Seroprevalence and determinants of hepatitis E virus infection among people living with HIV in Chiang Mai, Thailand: a cross-sectional analysis
Why this study matters
Hepatitis E is a lesser-known liver infection that can be especially dangerous for people whose immune systems are already weakened, such as those living with HIV. In northern Thailand, both HIV and hepatitis E are present, yet doctors have had little information on how often these infections overlap or which patients are most at risk. This study from Chiang Mai helps fill that gap, offering new insight that can guide better screening and protection for vulnerable patients.
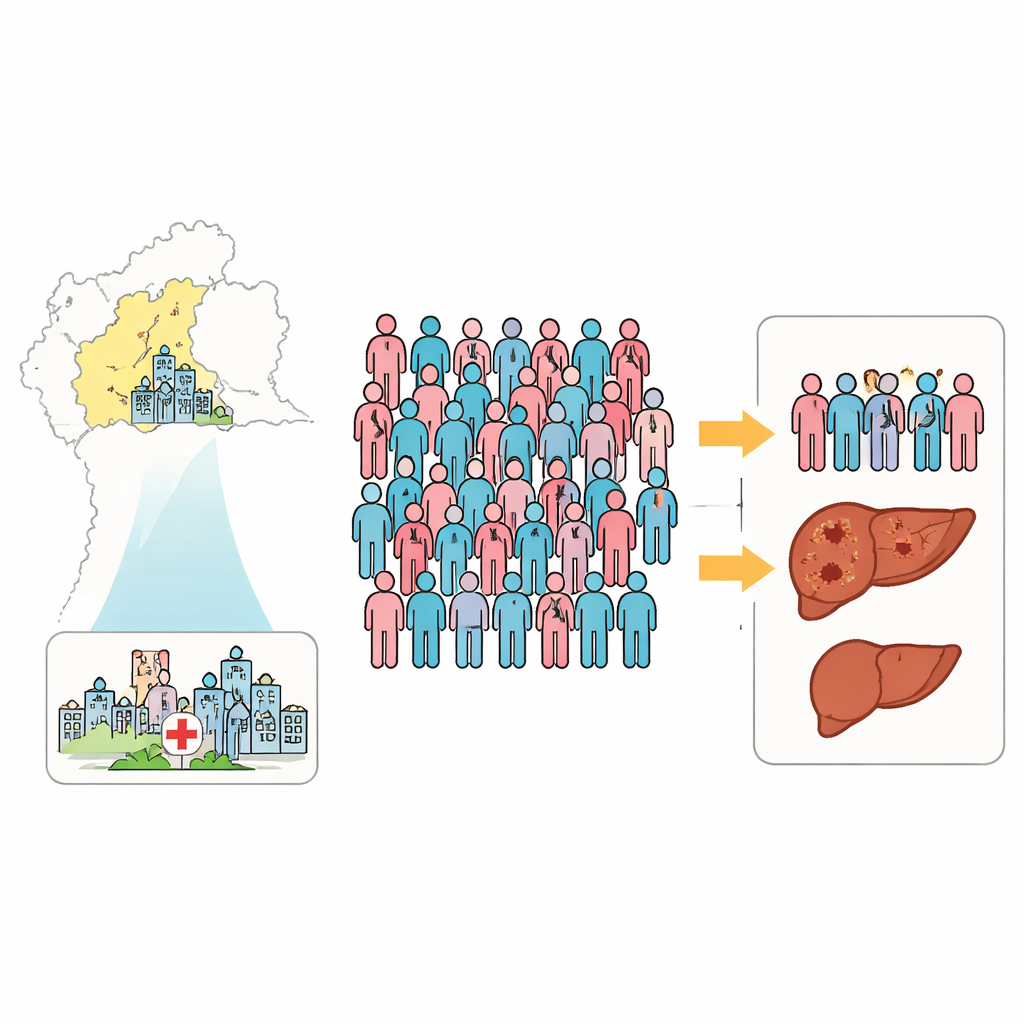
Taking a snapshot of a hidden infection
The researchers focused on 200 adults living with HIV who were receiving routine care at four referral hospitals in Chiang Mai province between 2023 and 2024. All participants were at least 18 years old and well enough to complete an interview. The team used stored blood samples to test for antibodies against the hepatitis E virus, which signal that a person has been exposed to the virus at some point in the past. They also tested for signs of hepatitis B and C, two other viruses that can damage the liver, and collected detailed information about each person’s age, income, work, health history, and everyday behaviors.
How common was hepatitis E exposure?
Overall, 13 percent of the people in the study showed clear evidence of past hepatitis E infection. Men and women were affected at similar rates. A small additional group had borderline test results, suggesting possible prior exposure. By comparison, 8 percent had been exposed to hepatitis C and 6.5 percent were carrying hepatitis B surface antigen, a marker of active or chronic hepatitis B. Some participants had evidence of more than one liver virus, but triple infection with all three viruses was not observed. These numbers indicate that hepatitis E is by no means rare among people living with HIV in this setting, even though it is not currently part of routine screening.
Clues from age and medical history
To understand who was most at risk, the team used statistical models to look for patterns linking hepatitis E exposure with personal and medical factors. One clear signal was age: people aged 50 and older were more than three times as likely to show hepatitis E antibodies as younger adults, consistent with gradual build-up of exposure over a lifetime. Two medical clues also stood out. Participants who reported ever having a needle stick injury, such as an accidental puncture during medical or caregiving work, were more than three times as likely to have markers of past infection. Those with a history of kidney failure had a much higher likelihood of prior hepatitis E exposure, suggesting that repeated medical procedures or underlying frailty might increase vulnerability.
What did not seem to drive risk
Interestingly, many behaviors that might be assumed to matter did not show a strong link to hepatitis E in this group. Smoking, alcohol use, tattoos, piercings, sexual activity, and past surgery or blood transfusions were not clearly tied to higher exposure once other factors were taken into account. Nor did infection with hepatitis B or C appear to change the odds of having had hepatitis E. This pattern points toward broader environmental exposures and healthcare-related contacts, rather than individual lifestyle choices, as more important drivers of risk for people living with HIV in Chiang Mai.
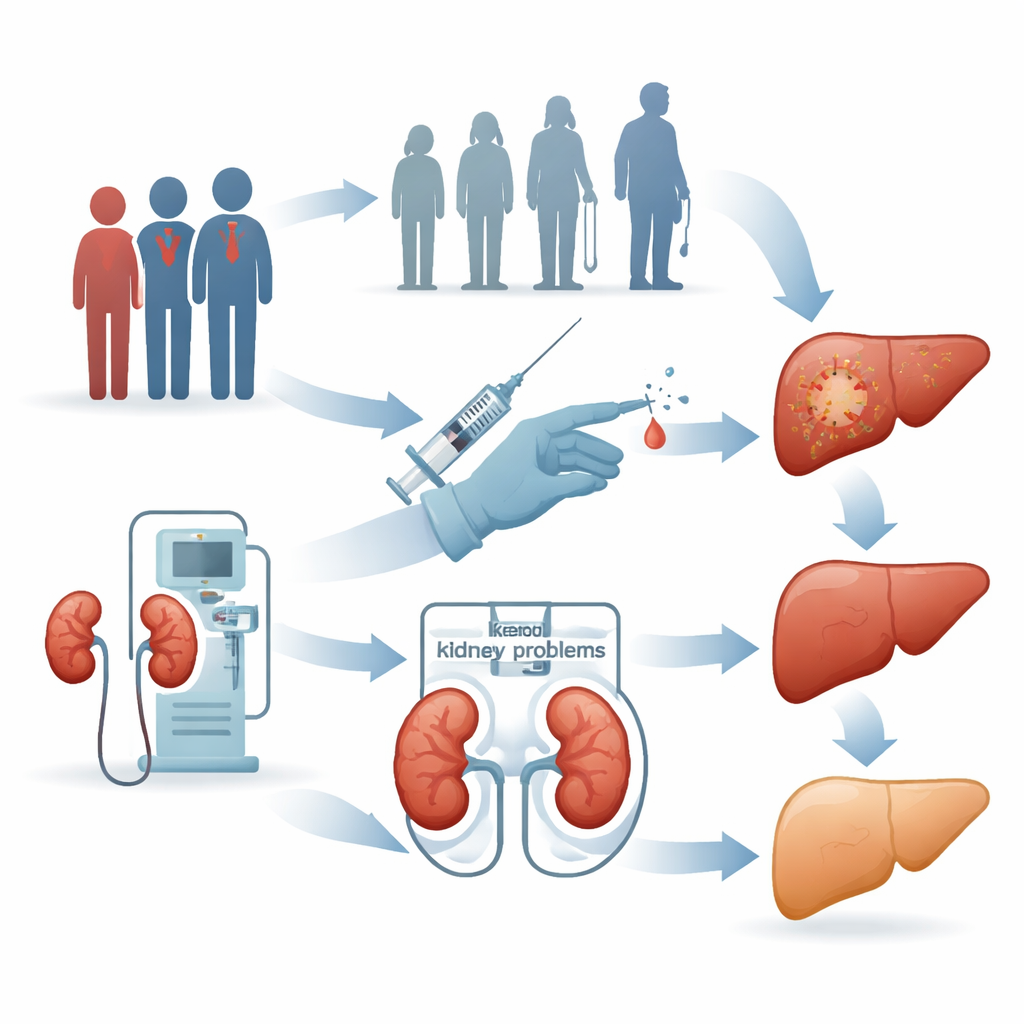
What this means for patients and care
The study shows that roughly one in eight people living with HIV in Chiang Mai has already encountered hepatitis E, and that older age, kidney problems, and past needle injuries mark those at greatest risk. For patients, this means that a largely silent infection may be adding extra strain to an already vulnerable liver. For clinics and policy makers, the findings argue for including hepatitis E tests alongside existing checks for hepatitis B and C, especially for older patients and those with kidney disease or frequent medical procedures. Strengthening surveillance and prevention in this way could catch problems earlier, guide safer care, and ultimately reduce avoidable illness among people living with HIV in Thailand and across Southeast Asia.
Citation: Chakma, R., Jindaphun, K., Umer, M. et al. Seroprevalence and determinants of hepatitis E virus infection among people living with HIV in Chiang Mai, Thailand: a cross-sectional analysis. Sci Rep 16, 7853 (2026). https://doi.org/10.1038/s41598-026-39147-6
Keywords: hepatitis E, HIV coinfection, Chiang Mai Thailand, liver infection, seroprevalence