Clear Sky Science · en
Changes in macular structure after removal of epiretinal membrane in combined hamartomas of the retina and retinal pigment epithelium
Why this eye study matters
Vision problems are often blamed on glasses prescriptions or cataracts, but sometimes the issue lies in tiny structural changes deep inside the back of the eye. This study looks at a rare eye tumor that can warp the central retina—the spot responsible for sharp vision—and asks a practical question: if surgeons remove a thin film of scar-like tissue tugging on the retina, can they protect or even improve sight? The answer helps eye doctors decide when surgery is worth the risk for patients facing slow but serious visual distortion.
A rare growth that bends the center of sight
The researchers focused on a rare condition called a combined hamartoma of the retina and retinal pigment epithelium. In simple terms, this is a benign overgrowth of tissue near the light-sensitive layer at the back of the eye. Almost all patients with this growth also develop a fine “shrink wrap” on the surface of the retina, known as an epiretinal membrane. This film can contract over time, pulling on the central retina (the macula) and subtly dragging the point of sharpest vision away from its normal position toward the optic nerve. Patients may notice gradual blurring, distortion, or worsening of one eye, sometimes starting in childhood but also seen in adults.
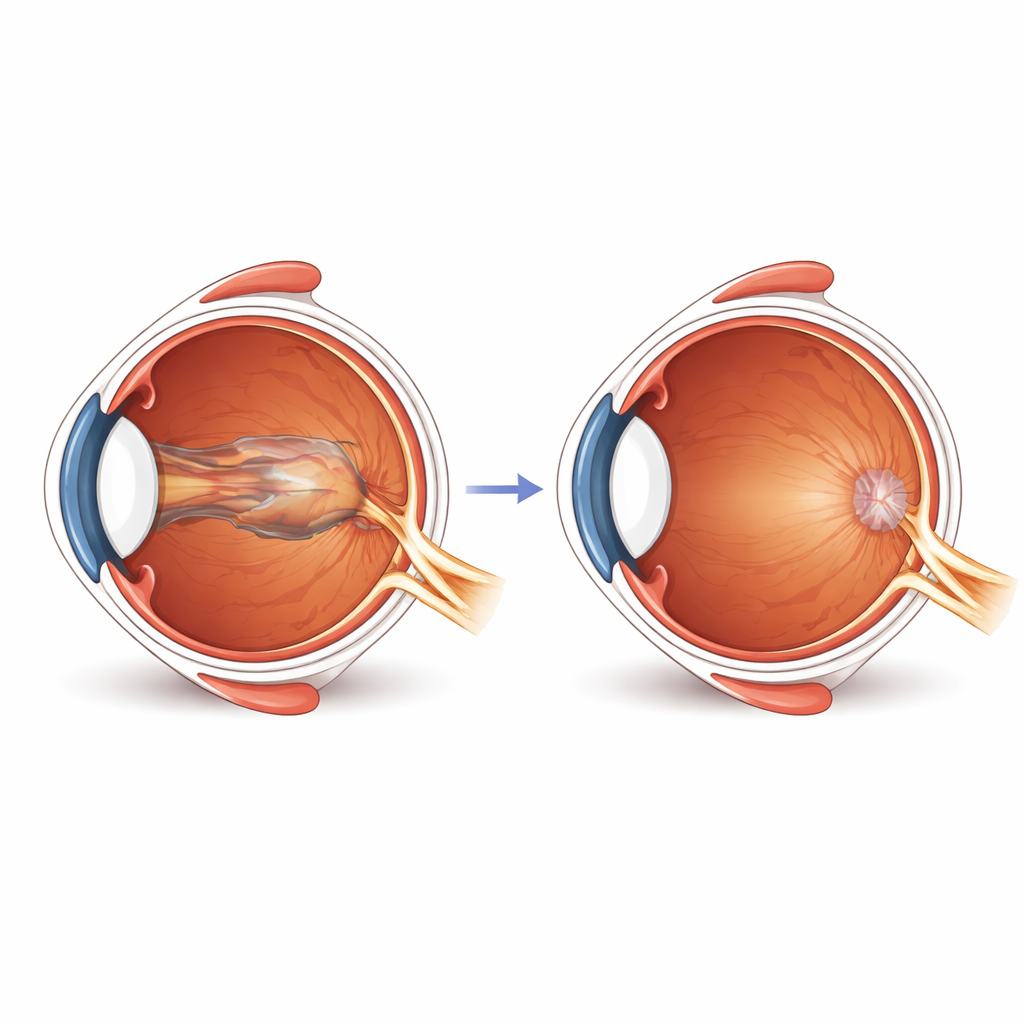
How the study was set up
Because the condition is rare, the team looked back through 16 years of records at their hospital and identified 15 people with this type of hamartoma. All had the surface membrane, but only some underwent surgery to remove it; the rest were monitored without an operation. Six eyes formed the “operation group,” treated with modern small-incision vitrectomy, during which surgeons removed the gel inside the eye and gently peeled off the membrane on the retinal surface. Nine eyes formed the “observation group,” which received regular checkups and imaging but no surgery. The groups were similar in age and membrane severity when first seen, allowing a fair comparison of how their eyes changed over time.
Measuring changes in retinal shape and position
To track what happened inside the eye, the team used detailed scanning technology called optical coherence tomography. From these images, they measured central macular thickness—how swollen or thick the central retina was—and a distance called the foveo-papillary distance, which indicates how far the very center of sight sits from the optic nerve. A shorter distance means the center has been dragged nasally, toward the nerve. They also recorded best corrected visual acuity, essentially how small a line of letters patients could read with proper lenses. These measurements were taken at the first visit and again after years of follow-up, both in operated and non-operated eyes.
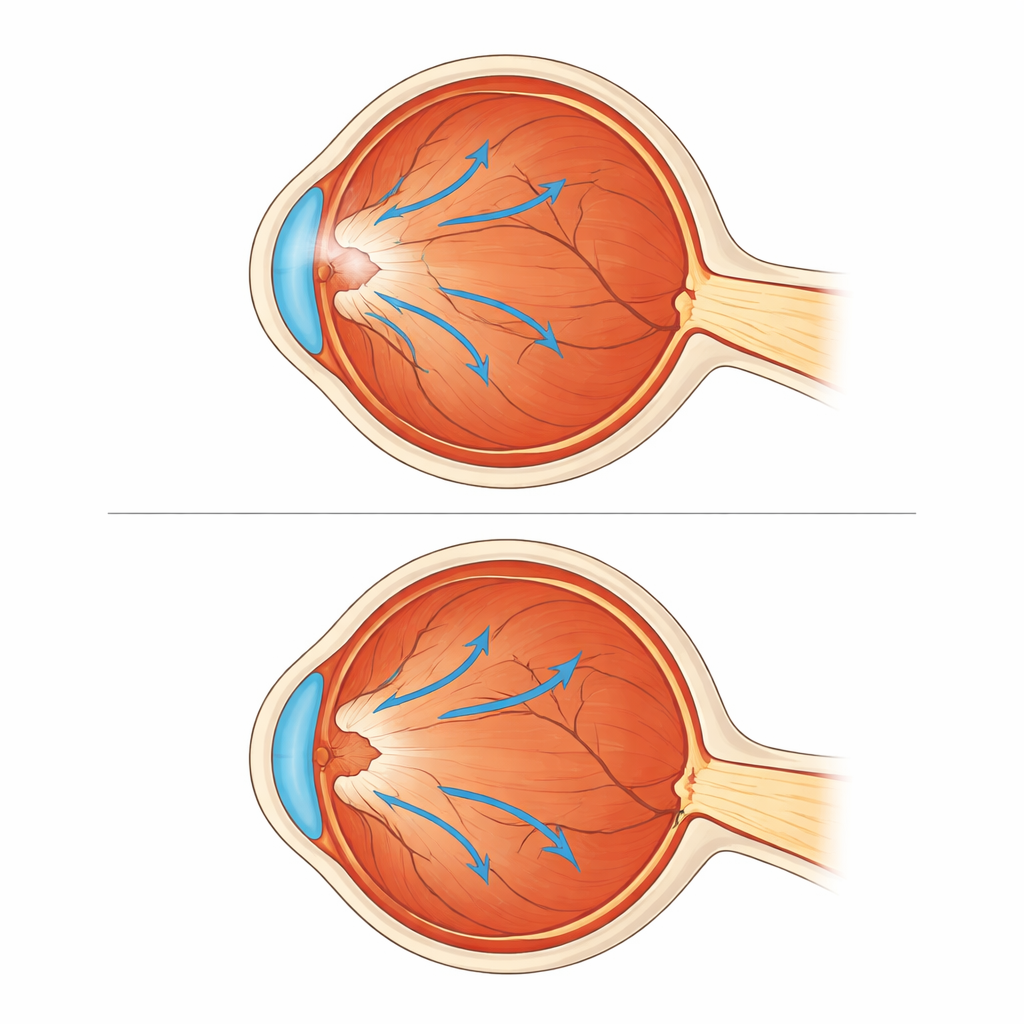
What surgery changed inside the eye
Eyes that underwent membrane removal showed clear structural improvements. Their central retina became thinner and closer to normal, shrinking from an average of about 480 micrometers to 365 micrometers. At the same time, the center of sight moved slightly back toward its natural location, as shown by an increase in foveo-papillary distance in every operated eye. In contrast, the eyes that were simply observed tended to drift the wrong way: their foveo-papillary distance shortened in all cases, showing continued dragging toward the optic nerve, and their retinal thickness did not improve. Vision followed the same pattern. Patients in the surgery group gained meaningful clarity, while those in the observation group, on average, did not improve and some experienced noticeable worsening over time.
What this means for patients and doctors
For people with this rare retinal growth and its accompanying surface film, the study suggests that carefully performed membrane removal does more than tidy up scan images—it can help restore a more natural shape and position of the macula and support better vision, even in adults. While surgery always carries risks and not every eye will respond the same way, leaving the membrane in place appears to allow ongoing traction and slow distortion. The authors conclude that, particularly for patients whose vision is declining or at risk of amblyopia (lazy eye), early surgical peeling of the membrane may help preserve central sight by relieving the mechanical pull that bends the retina out of place.
Citation: Lee, C.H., Kim, K.H., Choi, Y.J. et al. Changes in macular structure after removal of epiretinal membrane in combined hamartomas of the retina and retinal pigment epithelium. Sci Rep 16, 9462 (2026). https://doi.org/10.1038/s41598-026-39124-z
Keywords: retinal tumor, epiretinal membrane, macular surgery, vitrectomy, visual acuity