Clear Sky Science · en
Ultrasound wrist mapping to develop a noninvasive radiation detector for dynamic positron emission tomography
Why Wrist Scans Matter for Better Cancer Imaging
Modern PET scans can track how tracers move through the body over time, helping doctors judge how well a tumor treatment is working or how a new drug behaves. But to do this accurately, they need to know exactly how much radioactivity is in the blood at every moment—a quantity usually measured by repeatedly drawing blood from an artery. This study explores a less painful alternative: using ultrasound to map the blood vessels in the wrist so engineers can design a comfortable, wrist-worn radiation detector that could replace many needle sticks.
From Needles to Wearable Sensors
Dynamic PET scans follow a radioactive tracer as it travels through the bloodstream and into organs and tumors. To interpret these scans properly, researchers must know the tracer level in arterial blood over time, a curve called the arterial input function. Today, the gold-standard way to get this curve is by placing a catheter in an artery and drawing blood repeatedly—an invasive, time-consuming, and uncomfortable process that also exposes staff to radiation. Several groups are developing small external detectors that could sit over a superficial artery, such as the radial artery in the wrist, and capture the same information noninvasively. However, to work reliably on many different people, these devices must be carefully tuned to real human anatomy.
Mapping the Hidden Plumbing of the Wrist
To provide that anatomical roadmap, the researchers used ultrasound imaging on 154 healthy volunteers. Each person’s wrists were scanned at three fixed positions: 2, 4, and 6 centimeters up the forearm from the main wrist crease. For each scan, the team measured two key features: how deep the radial artery and its neighboring veins lay beneath the skin, and how large each vessel’s cross-sectional area was. Measurements were taken on both the left and right arms, and the data were analyzed with statistical models that could account for repeated measurements per person and explore the influence of factors like sex, age, and body mass index.
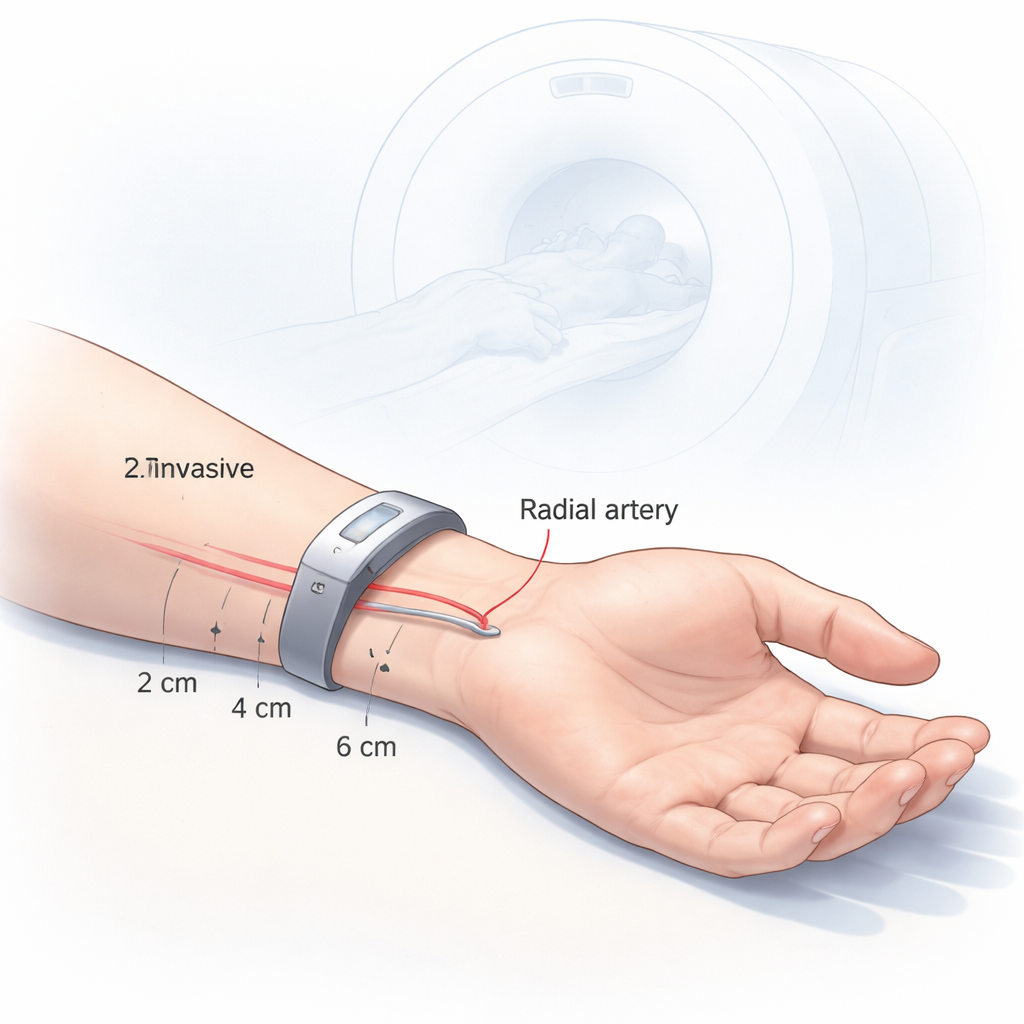
What the Ultrasound Pictures Revealed
The study found a clear pattern: as the artery travels toward the wrist, it becomes both shallower and slightly wider. On average, at 2 centimeters from the wrist crease, the radial artery lay about 3.36 millimeters under the skin and had a cross-sectional area of 4.23 square millimeters. Farther up the arm, at 6 centimeters, it was deeper—around 4.66 millimeters—and slightly smaller in area. The accompanying veins showed a similar trend in depth but tended to become a bit smaller closer to the wrist. The left and right arms were not identical: across participants, the radial artery tended to lie closer to the skin on the left side, suggesting that a wrist detector might perform best when worn on the left arm. Men generally had larger vessels but, somewhat surprisingly, their vessels tended to sit slightly closer to the skin than women’s when body size was taken into account.
Design Clues for a Future Wrist Detector
These measurements are more than anatomical trivia; they give engineers the numbers they need to simulate how a wrist-worn detector will respond in real people. A shallower artery means less tissue for radiation to pass through, so more signal reaches the detector. A larger artery carries more tracer-filled blood, which also boosts the signal. Combining both effects, the data point to a sweet spot: about 2 centimeters up from the wrist crease on the left forearm. The authors plan to incorporate the full range of observed depths and vessel sizes into computer models that will test different detector designs, placement tolerances, and even the effects of different radioactive tracers, some of which emit higher-energy particles that can travel farther through tissue.
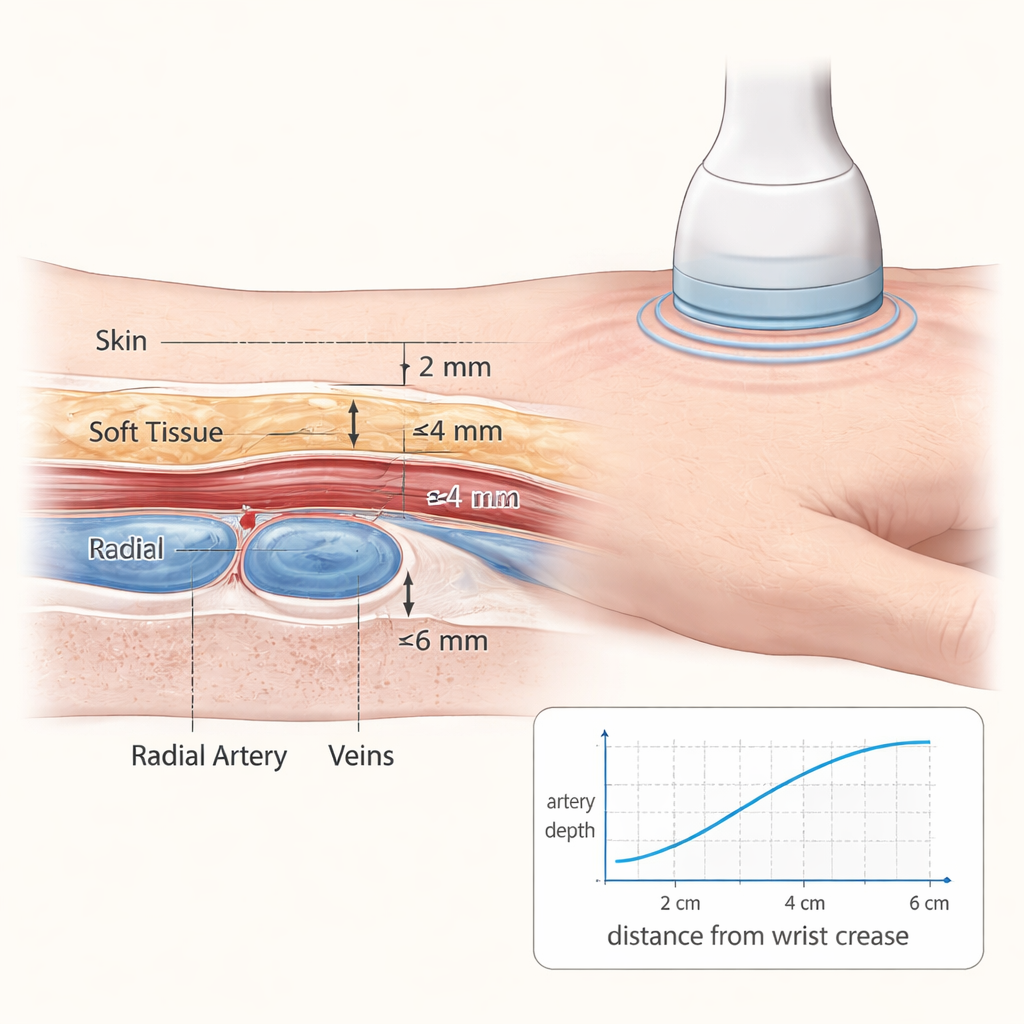
A Step Toward Needle-Free PET Measurements
For patients, the key takeaway is simple: the study shows that the radial artery near the wrist is typically both close to the skin and relatively large, especially about 2 centimeters from the main wrist crease on the left arm. That spot offers a promising target for a wearable radiation detector that could one day replace repeated arterial blood draws during advanced PET scans. By turning detailed wrist ultrasound measurements into practical design rules, this work moves the field closer to a future in which gathering the information needed for high-precision PET imaging can be done with a comfortable band on the wrist instead of a catheter in the artery.
Citation: Leclerc, MA., Mesko, M., Daoud, Y. et al. Ultrasound wrist mapping to develop a noninvasive radiation detector for dynamic positron emission tomography. Sci Rep 16, 7772 (2026). https://doi.org/10.1038/s41598-026-39073-7
Keywords: dynamic PET, wrist-worn detector, radial artery ultrasound, arterial input function, noninvasive imaging