Clear Sky Science · en
Analysis of the mechanism and prognostic value of PRKCQ-AS1 in inhibiting the progression of lung adenocarcinoma via regulating the PD-1/PD-L1 pathway
Why this hidden molecule matters
Lung adenocarcinoma is the most common form of lung cancer, and even with modern immunotherapy, too many patients see their disease return or resist treatment. This study focuses on a little-known RNA molecule, PRKCQ-AS1, that does not make proteins but may quietly influence whether lung tumors grow unchecked or are kept under control by the immune system. Understanding this invisible player could open new doors for earlier prognosis and better use of immunotherapy.
A quiet signal in lung tumors
The researchers began by mining a large public cancer database to see how much PRKCQ-AS1 is present in tumor samples from hundreds of people with lung adenocarcinoma. They found that this RNA is consistently lower in tumor tissue than in normal lung, and its levels drop even further as tumors advance to later stages. Patients whose tumors had less of this RNA tended to fare worse over time, suggesting that PRKCQ-AS1 behaves more like a natural brake on cancer than a fuel. The team then confirmed this pattern in real patient tissue samples collected in the clinic, reinforcing the idea that PRKCQ-AS1 could serve as a useful warning sign for aggressive disease.
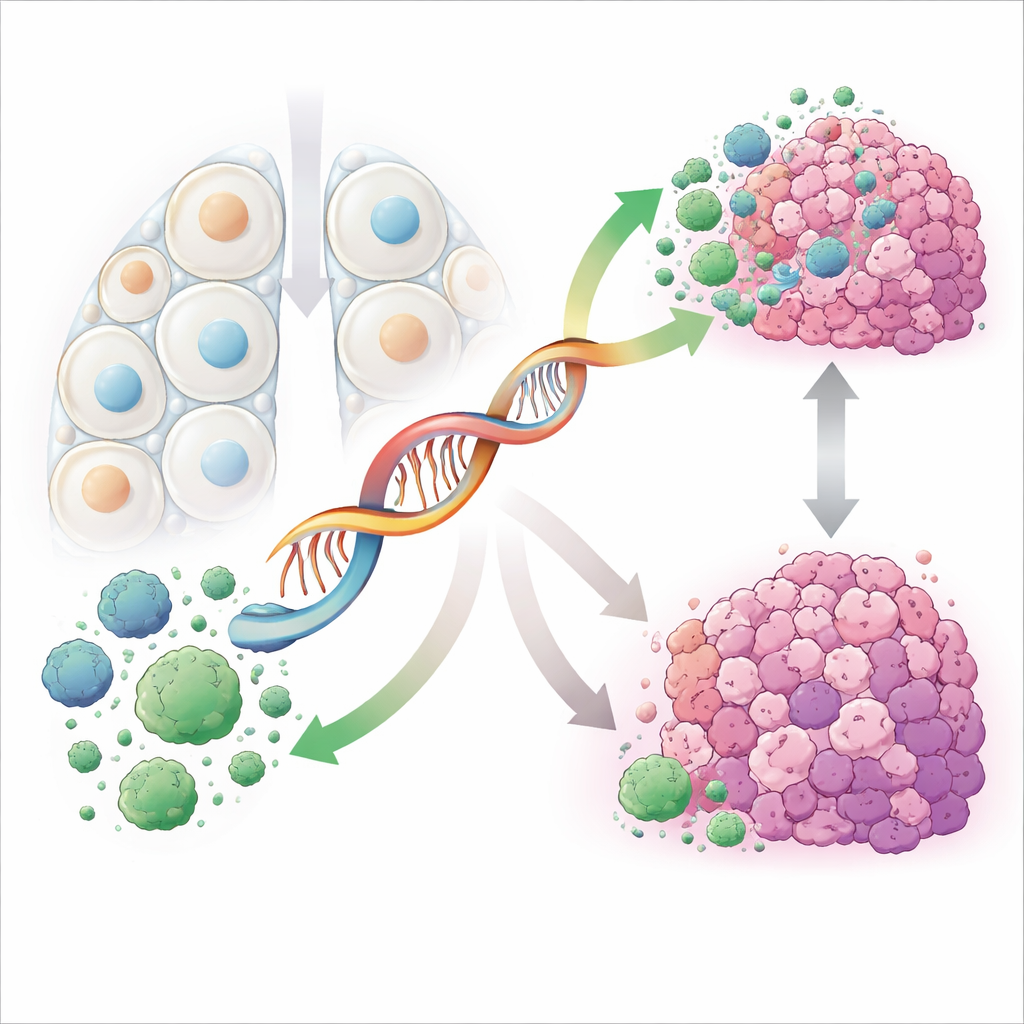
Probing how the molecule shapes cancer cell behavior
To move from database patterns to biology, the scientists turned to lung adenocarcinoma cells grown in the lab. They artificially dialed PRKCQ-AS1 levels up or down and watched how the cells responded. When they reduced this RNA, cancer cells multiplied faster, moved more readily across artificial barriers, and invaded through membranes more aggressively. At the same time, fewer cells underwent programmed cell death, the self-destruct process that normally helps keep damaged cells in check. Raising PRKCQ-AS1 had the opposite effect: growth slowed, movement and invasion dropped, and more cells died. Together, these experiments show that PRKCQ-AS1 directly reins in several hallmark behaviors that make lung tumors dangerous.
Links to the body’s defenses
The study also asked how this RNA might influence the broader environment around the tumor, especially immune cells that patrol for abnormal growths. Using computational tools, the authors built a regulatory map connecting PRKCQ-AS1 to other RNA molecules and genes involved in cancer and immunity. They found that genes tied to this RNA cluster in pathways related to immune responses and cell signaling. In patient data, tumors with more PRKCQ-AS1 tended to harbor higher levels of certain beneficial immune cells, including killer T cells that can directly destroy cancer cells. Tumors with less PRKCQ-AS1 showed a different mix of immune cells that may be less effective or even exhausted, hinting that this RNA helps shape how welcoming—or hostile—the tumor environment is to the body’s defenses.
Controlling a key immune checkpoint
One of the most powerful defenses tumors use to survive is the PD-1/PD-L1 checkpoint system, which acts like a molecular disguise that tells immune cells to stand down. Modern immunotherapy drugs work by blocking this signal. The authors discovered a strong connection between PRKCQ-AS1 and this checkpoint. In patient tissues and in cultured cells, low PRKCQ-AS1 went hand in hand with higher levels of PD-1 and PD-L1, while boosting the RNA pushed those checkpoint signals down. This suggests that when PRKCQ-AS1 is abundant, tumor cells display fewer “do not attack” signals on their surface, making them more visible to immune cells. When PRKCQ-AS1 is scarce, the checkpoint is more active, making it easier for tumors to hide from immune attack and continue growing.
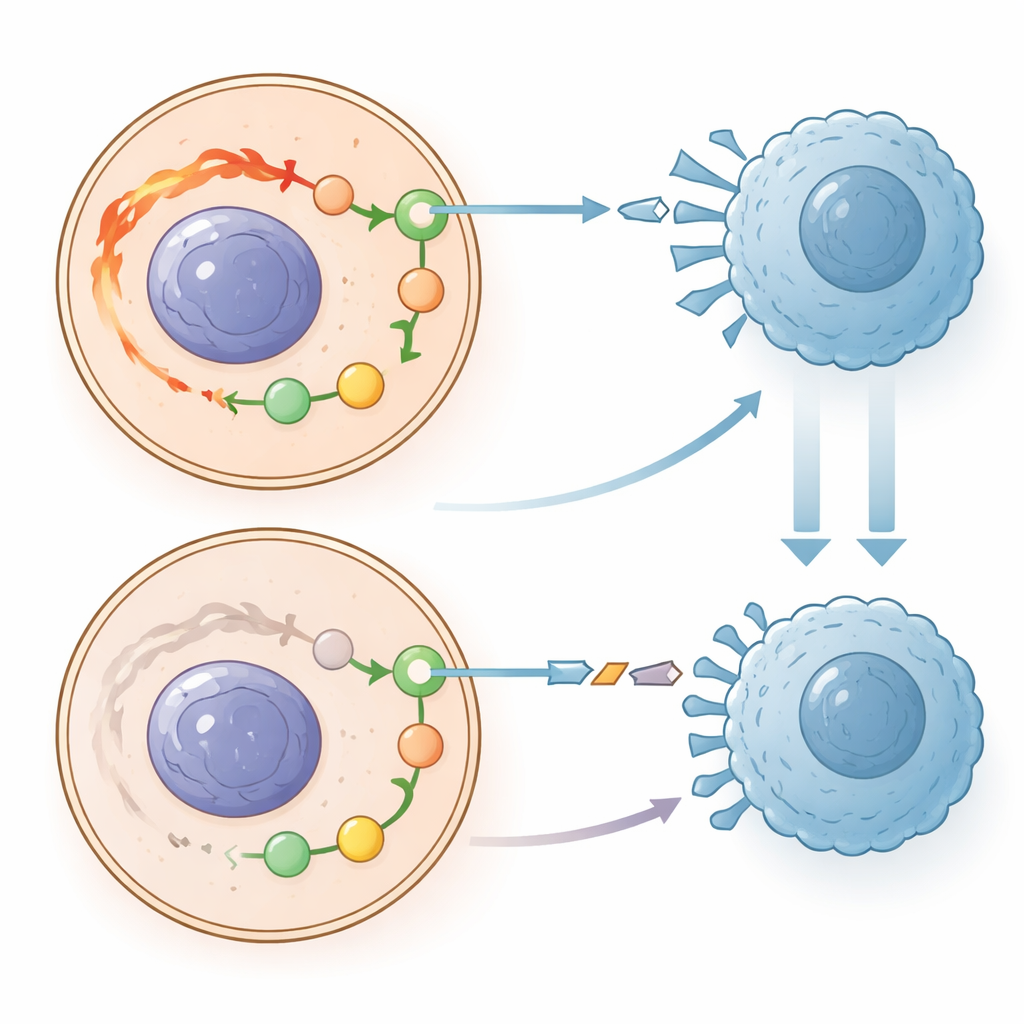
What this could mean for future care
Although this work still relies on cell models and a relatively small clinical group, it points to PRKCQ-AS1 as a natural tumor suppressor in lung adenocarcinoma. By restraining cancer cell growth and tamping down a key immune escape route, this non-coding RNA may influence both how quickly tumors progress and how well they respond to immunotherapy. In the future, measuring PRKCQ-AS1 could help doctors estimate a patient’s prognosis, and treatments that restore or mimic its activity might make immune-based drugs more effective. For now, this study adds an important piece to the puzzle of why some lung cancers resist the body’s defenses—and offers a new molecular handle for tackling them.
Citation: Wu, M., Wang, Y., He, G. et al. Analysis of the mechanism and prognostic value of PRKCQ-AS1 in inhibiting the progression of lung adenocarcinoma via regulating the PD-1/PD-L1 pathway. Sci Rep 16, 9782 (2026). https://doi.org/10.1038/s41598-026-39024-2
Keywords: lung adenocarcinoma, immune checkpoint, long non-coding RNA, tumor microenvironment, PD-1 PD-L1