Clear Sky Science · en
Cranberry extract-supplemented microbiota effluents enhance intestinal barrier integrity via mucin production and antimicrobial activity in murine organoids
Why Cranberries Matter for Your Gut
Most of us know cranberries as a tart holiday side dish or a juice touted for urinary health. This study asks a different question: what happens when cranberry compounds meet the trillions of microbes in your gut, and how does that encounter affect the thin cellular wall that separates your intestines from the rest of your body? Using sophisticated lab models that mimic both the human colon and miniature mouse intestines, the researchers show that cranberry extract can nudge gut microbes to make helpful substances that, in turn, strengthen the gut’s protective lining and its built‑in antimicrobial defenses.
From Berry to Bacteria
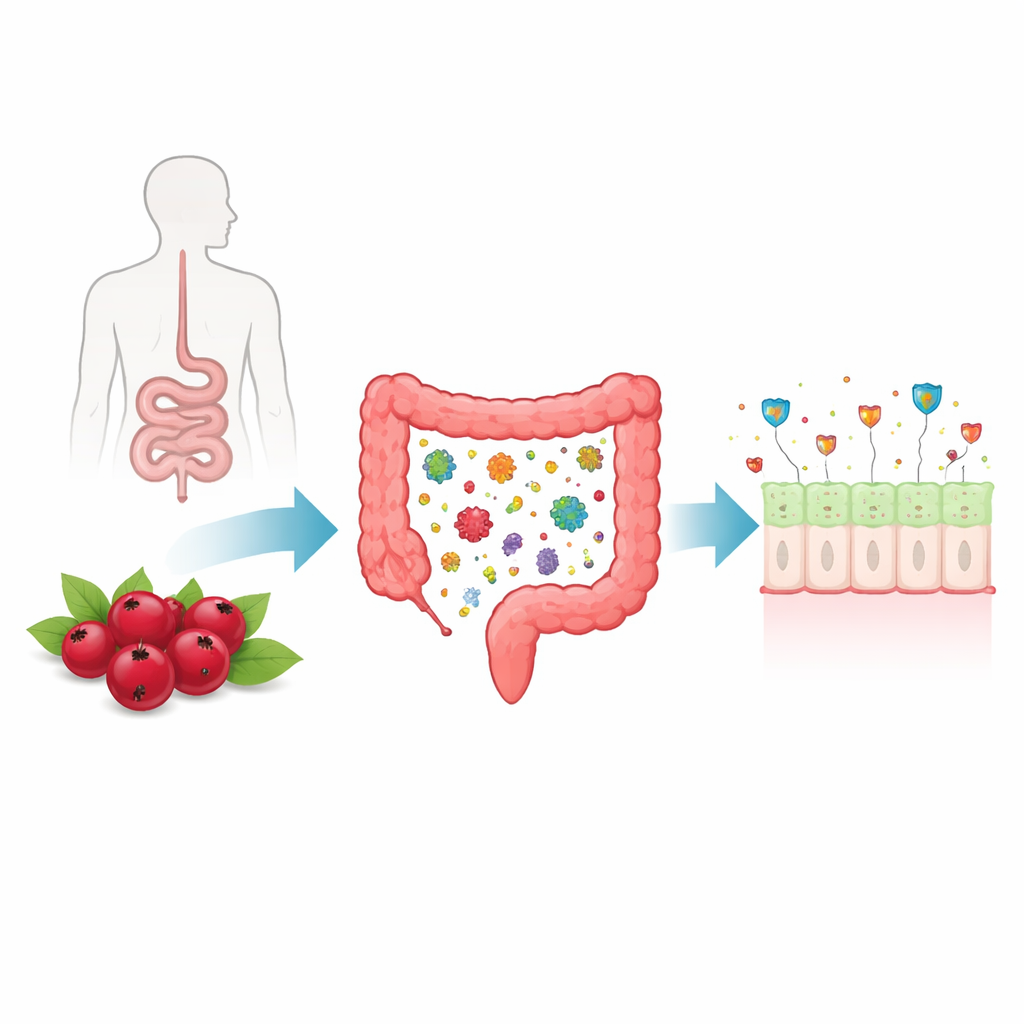
Cranberries are rich in two kinds of hard‑to‑digest ingredients: complex plant chemicals called proanthocyanidins and fiber‑like oligosaccharides. Because these compounds are poorly absorbed in the upper gut, they travel largely intact to the colon, where they become food for resident microbes. Earlier work by the same group showed that a standardized cranberry extract shifts the gut community toward beneficial species and boosts production of short‑chain fatty acids, especially butyrate, a small molecule known to support gut health. Building on that, the current study set out to connect these microbial changes to direct effects on the gut lining itself.
Simulating the Human Colon and Tiny Intestines
To capture this chain of events, the team combined two advanced systems. First, they used a device called TWIN‑M‑SHIME, which recreates key features of the human large intestine and is seeded with fecal microbes from healthy donors. Over several weeks, this artificial gut was run first without and then with daily doses of cranberry extract equivalent to eating a generous serving of fresh berries. Liquid from the model colon, containing microbial breakdown products of the extract, was then collected. Second, the researchers grew three‑dimensional “organoids” from mouse intestinal tissue—mini‑gut structures that include the main cell types found in the intestinal lining. By exposing these organoids to the colon liquids, they could watch how the gut epithelium responds to cranberry‑conditioned microbial activity.
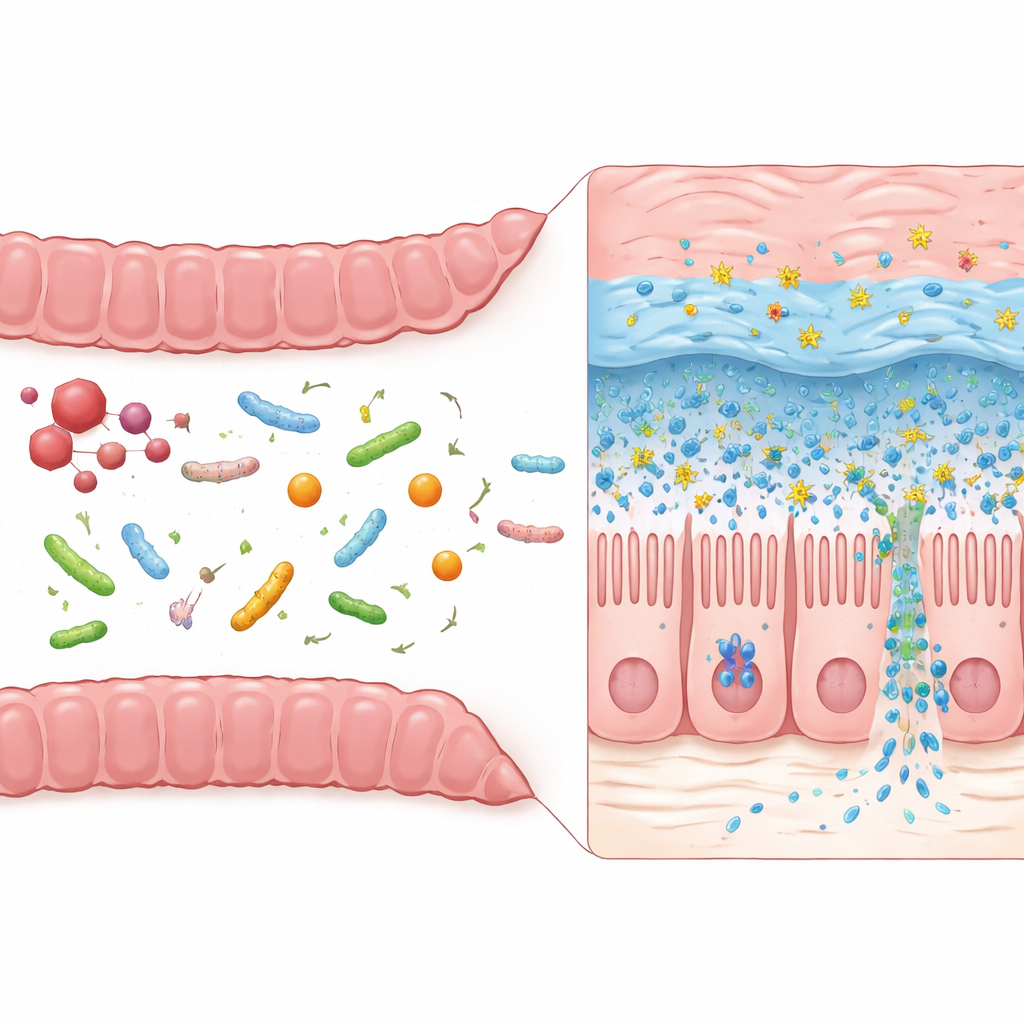
Thicker Mucus and Stronger Chemical Defenses
When organoids were bathed in liquids from cranberry‑supplemented microbiota, they switched on genes linked to mucus production and specialized mucus‑producing goblet cells. In particular, activity of the gene for Muc2, a key building block of the intestinal mucus layer, rose notably a few days after supplementation, along with genes (Atoh1 and Klf4) that drive goblet cell formation and maturation. At the same time, the organoids ramped up Defa20, a gene encoding antimicrobial peptides released by Paneth cells—tiny protein weapons that help keep harmful microbes at bay. These changes appeared rapidly, within hours of first exposure, and some, like the antimicrobial response, remained elevated over the full two‑week period, suggesting both an immediate and a sustained strengthening of the gut’s frontline defenses.
Microbial Metabolites as Messengers
The study also probed how microbe‑made metabolites might signal these changes. Cranberry supplementation in the colon model was known to increase butyrate and, to a lesser extent, propionate—two short‑chain fatty acids produced when microbes ferment complex carbohydrates. In the organoids, the researchers observed higher activity of receptors (such as GPR109a and GPR43) that sit on intestinal cells and sense these fatty acids. Statistical analyses linked butyrate and propionate levels to stronger expression of Defa20 and, in some cases, Muc2 and other barrier‑related genes, whereas acetate often showed the opposite pattern. This points to a scenario in which cranberry compounds reshape the microbiota, the altered microbiota produce more butyrate and related molecules, and those molecules then activate receptors on intestinal cells to boost mucus and antimicrobial defenses.
What This Could Mean for Everyday Health
Taken together, the findings outline a multi‑step story: cranberry extract feeds select gut microbes, those microbes generate protective metabolites, and the intestinal lining responds by thickening its mucus shield and sharpening its chemical weapons against unwanted invaders. While the work was done in lab models rather than in people, it supports the idea that cranberry‑based supplements or foods, especially when combined with certain fibers, could help maintain a resilient gut barrier. A sturdier barrier may, in turn, lower the risk of problems linked to a “leaky” gut, such as chronic inflammation or metabolic disturbances. In plain terms, cranberries appear to help your gut microbes help you, reinforcing the invisible wall that keeps the contents of your intestines where they belong.
Citation: Cattero, V., Mayer, T., Veilleux, A. et al. Cranberry extract-supplemented microbiota effluents enhance intestinal barrier integrity via mucin production and antimicrobial activity in murine organoids. Sci Rep 16, 8539 (2026). https://doi.org/10.1038/s41598-026-39008-2
Keywords: cranberry extract, gut microbiota, intestinal barrier, short-chain fatty acids, mucus layer