Clear Sky Science · en
Airway mucus plugs in COPD clinical phenotypes and prognosis across stable and exacerbation states
Why thick mucus in the lungs matters
For millions of people living with chronic obstructive pulmonary disease (COPD), flare‑ups that lead to emergency visits and hospital stays can feel unpredictable and frightening. This study asks a simple but important question: can we see warning signs inside the lungs that flag which patients are at higher risk? By using routine chest CT scans to look for mucus plugs—thick clumps of mucus that completely block small airways—the researchers show that these hidden blockages are closely tied to worse breathing, more flare‑ups, higher costs, and a greater chance of death.
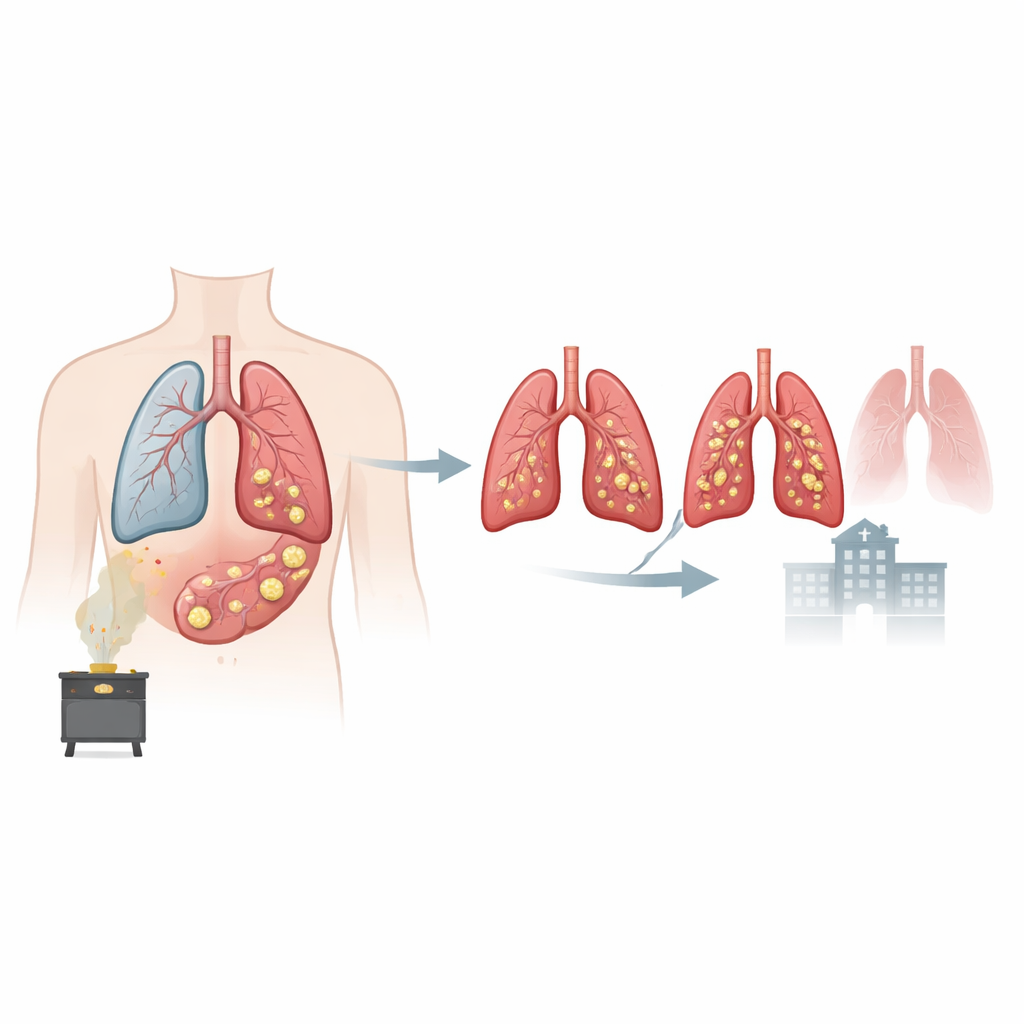
Hidden blockages in common lung disease
COPD is a long‑term lung condition that makes it hard to breathe and is now a leading cause of death worldwide. Many patients produce extra phlegm and have a chronic cough, but mucus deep inside the lungs cannot be seen or felt directly. In this large study from China, more than 2700 people with COPD underwent detailed CT scans. Radiologists looked for mucus plugs, defined as solid‑looking material that completely filled an airway branch. About one in three patients had these plugs. They were more common in people who were older, had worse symptoms, had been exposed to smoke from biofuels such as wood or crop waste, and already had poorer lung function.
Worse during flare‑ups, not just on quiet days
The researchers compared people seen during a stable phase of COPD with those hospitalized for an acute worsening, known as an exacerbation. Mucus plugs showed up far more often during these flare‑ups: nearly half of hospitalized patients had them, compared with less than a third of stable patients. When plugs were present, they tended to appear in more lung segments and in both lungs. CT measurements also revealed that these patients had thicker airway walls but, somewhat surprisingly, less emphysema (the air‑sac damage classically linked with COPD). This pattern suggests a form of COPD in which narrowed, inflamed airways clogged with mucus—rather than destroyed air sacs—play the starring role in limiting airflow.
Slower recovery and faster decline
To see what these blockages meant for everyday life, the team followed patients for months to years. Among those in a stable phase of COPD, people with mucus plugs improved less after treatment: their symptom scores dropped only slightly compared with those without plugs, and their lung function declined faster over time. Measures of how much air could be blown out in one second worsened more steeply in the plugged group, even after accounting for age, smoking, baseline lung strength, and other factors. The more lung segments contained plugs, the greater the deterioration, hinting at a dose–response relationship between the burden of blockage and loss of breathing capacity.
More hospital days, higher bills, and greater risk
For patients hospitalized with COPD flare‑ups, mucus plugs were linked to clearly worse outcomes. Those with plugs stayed in the hospital longer and generated higher total medical costs, even though intensive care use was similar. After discharge, they were more likely to return to the hospital, to experience further moderate or severe exacerbations over the next one to two years, and to die during follow‑up. Across both stable and exacerbation groups, having plugs more than doubled the risk of future serious flare‑ups, and patients with plugs in more than two lung segments had a notably higher risk of death than those without plugs.
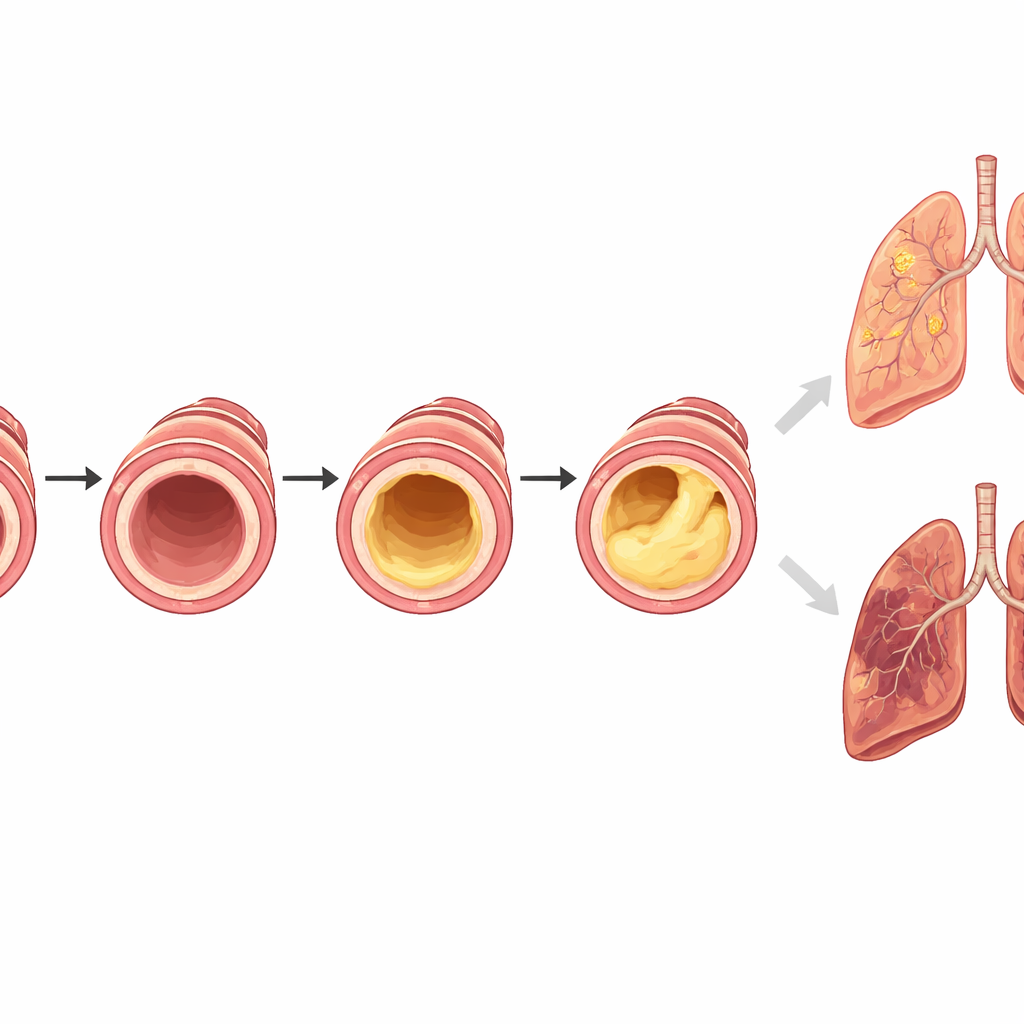
What this means for patients and doctors
Taken together, the findings paint mucus plugs as more than a side effect of COPD—they appear to be a powerful marker, and likely a driver, of worse disease. Because these plugs can be seen on standard CT scans already used in many clinics, they could serve as a simple visual flag to identify high‑risk patients who need closer monitoring and more aggressive care. The results also suggest that treatments aimed at thinning, loosening, or clearing mucus might not just ease coughing, but potentially slow lung decline, shorten hospital stays, and reduce deaths in people whose scans show these hidden blockages.
Citation: Lin, L., Li, T., Zhang, P. et al. Airway mucus plugs in COPD clinical phenotypes and prognosis across stable and exacerbation states. Sci Rep 16, 8178 (2026). https://doi.org/10.1038/s41598-026-38985-8
Keywords: COPD, airway mucus plugs, lung function decline, exacerbations, chest CT