Clear Sky Science · en
Altered expression of the CD26/ADA axis in immune-mediated inflammation of infectious mononucleosis
Why this childhood virus matters
Many parents know infectious mononucleosis, often called “mono,” as a bad but usually temporary illness marked by fever, sore throat, and swollen glands. Yet in a small number of children, the infection can become severe and damage organs like the liver. This study looks under the microscope at how children’s immune systems react to Epstein–Barr virus, the main cause of mono, and focuses on a pair of tiny cell-surface partners—CD26 and an enzyme called ADA—that may help explain why some immune responses become dangerously intense.
The body’s defenders in overdrive
When Epstein–Barr virus enters the body, it mainly infects certain white blood cells and triggers a strong immune reaction. In this study, doctors compared blood from 30 children with acute mono to 30 healthy children. They found that the sick children had many more white blood cells overall, especially a subset called CD8 T cells that specialize in killing infected cells. At the same time, another important helper group, CD4 T cells, was relatively reduced, so the usual balance between “attack” and “support” cells was flipped. Levels of infection-fighting proteins in the blood, including several signaling molecules that turn inflammation up or down, were also higher, showing the immune system was fully activated.
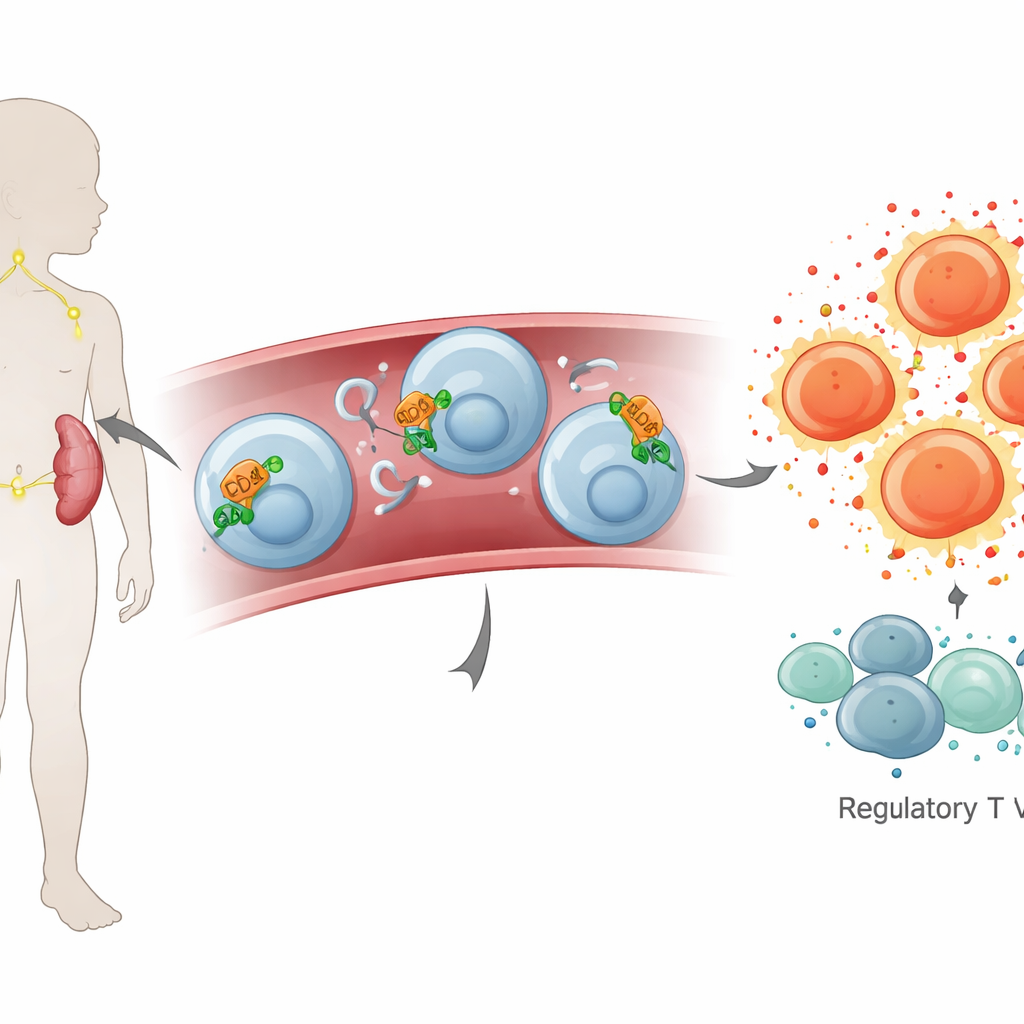
A close look at a tiny control switch
The researchers then homed in on CD26 and ADA, two molecules that sit at the crossroads between cell activation and chemical signaling outside the cells. Using genetic tests on blood cells, they found that children with mono had higher levels of CD26 and ADA instructions (mRNA), suggesting that immune cells were gearing up to make more of these proteins. Blood tests confirmed that ADA activity itself was higher. Interestingly, the circulating amount of CD26 protein in plasma did not differ much between sick and healthy children, hinting that in mono this molecule may stay mainly attached to cell surfaces rather than floating freely.
Shifting balance between attack and restraint
To understand how this control switch behaved on different immune cells, the team used flow cytometry, a method that counts and characterizes cells one by one. On CD8 T cells, the ones that expand dramatically during mono, CD26 was more common, whether or not the cells carried another marker called CD39 that is linked to a powerful chemical brake system. This pattern suggests that in these “killer” cells, CD26 may help overcome local chemical signals that would normally dampen their activity, supporting a strong attack on virus-infected cells. At the same time, among CD4 T cells that usually help coordinate immune responses, the picture was more mixed. Cells bearing both CD4 and CD39—often associated with regulatory, calming roles—were relatively more frequent, which may help explain high levels of soothing signals like the cytokine IL-10.
When regulation weakens
However, within the CD4 population that lacks CD39 and is typically made up of active helper cells, the fraction of cells displaying CD26 was actually lower in children with mono than in healthy peers. This loss of CD26 on helper cells may blunt their ability to proliferate and coordinate balanced responses, even as CD8 cells are pushed toward stronger activity. The study also showed that the amount of CD26 in plasma tracked with ADA levels and with interferon-gamma, a potent inflammatory signal, and was inversely linked to the share of CD4 T cells and to the CD4-to-CD8 ratio. Together, these patterns point to the CD26/ADA “axis” as tightly connected to how forcefully the immune system responds during infection.
What it means for sick children
For families and clinicians, these findings offer a clearer picture of why a common virus can sometimes lead to worrisome illness. In acute mono, children’s immune systems appear to lean heavily on CD8 T cells armed with extra CD26–ADA activity, driving a strong antiviral push that risks overshooting and harming tissues. At the same time, certain helper and regulatory cells lose or reshape their CD26 patterns, potentially weakening the brakes that normally keep inflammation under control. While more work is needed—especially in very severe cases—this study suggests that measuring and eventually modulating the CD26/ADA axis could one day help doctors gauge disease severity or design treatments that calm harmful immune fires without fully turning off the body’s defenses.
Citation: Shi, T., Shi, W., Tian, J. et al. Altered expression of the CD26/ADA axis in immune-mediated inflammation of infectious mononucleosis. Sci Rep 16, 9316 (2026). https://doi.org/10.1038/s41598-026-38891-z
Keywords: infectious mononucleosis, Epstein-Barr virus, T cells, immune regulation, adenosine pathway