Clear Sky Science · en
Pathways to lung cancer diagnosis and treatment among patients in Ethiopia: A qualitative study
Why this story matters
Lung cancer is often seen as a disease of older smokers in wealthy countries. This study shows a very different picture from Ethiopia, where most people with lung cancer are younger, have never smoked, and still reach hospitals only when the disease is far advanced. By listening closely to 33 patients across three major hospitals, the researchers trace the real-life journey from first cough to first treatment—and reveal where lives are being quietly lost along the way.
First signs that don’t ring alarm bells
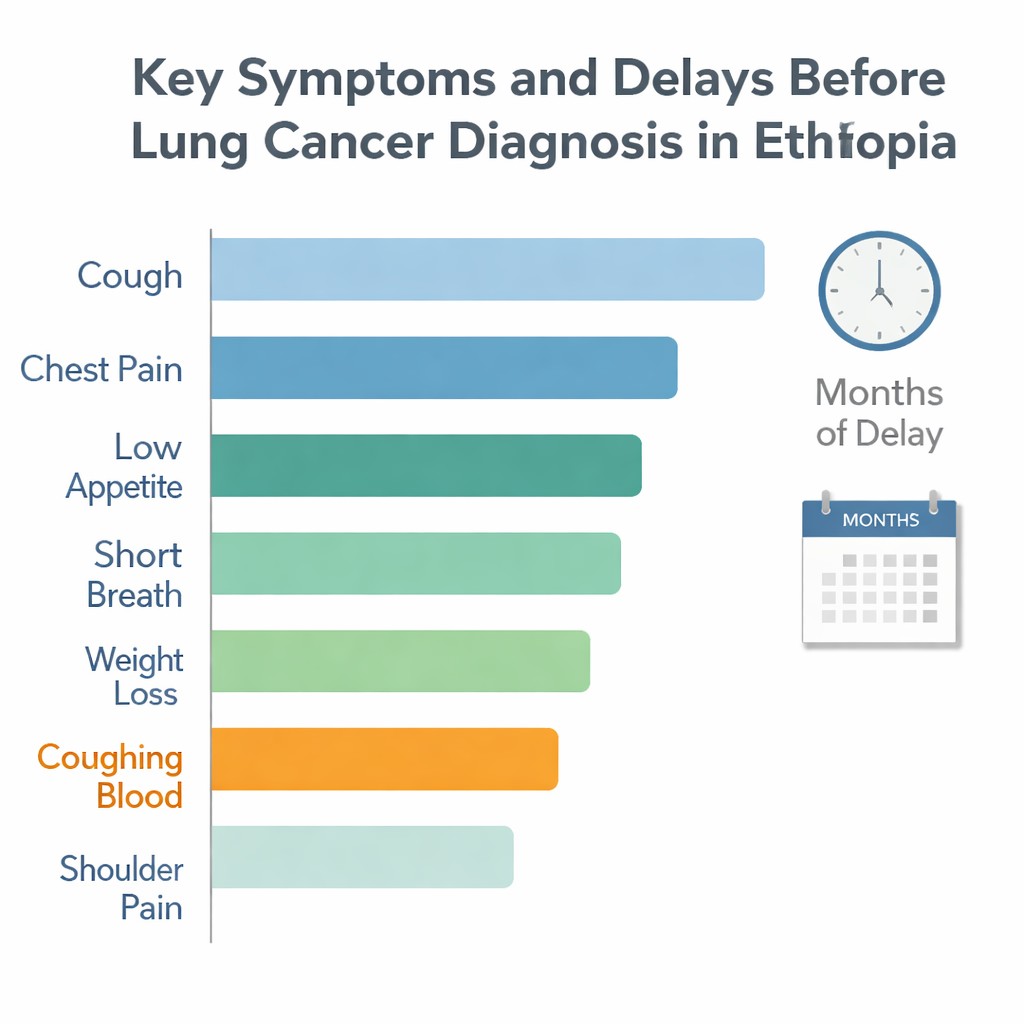
The journey usually begins with everyday problems: a stubborn cough, chest or shoulder pain, shortness of breath, weight loss, tiredness, or coughing up blood. None of the patients in this study thought these early signals might mean cancer. Many blamed a simple cold, flu, or dust; smokers assumed it was just their habit catching up with them. If symptoms came and went, or did not stop them from working, people tended to ignore them. Past good health, rural lifestyles that felt “protective,” and the belief that non-smokers are safe from lung cancer all made it easier to dismiss warning signs.
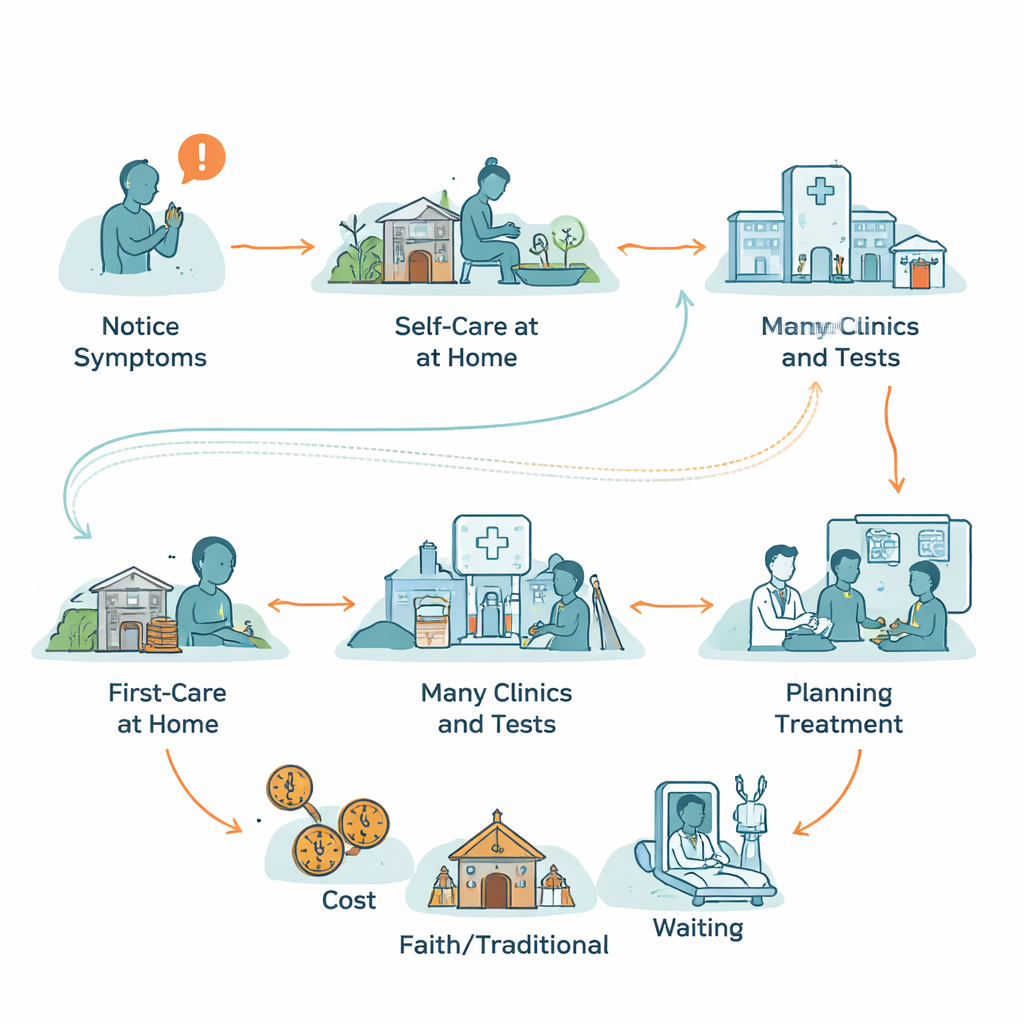
Trying home remedies and holy water first
Before seeing a doctor, most patients tried to handle symptoms on their own. They waited to “see if it goes away,” used herbal mixtures, toasted garlic and spices, bought cough syrups and pain pills, or turned to holy water and other faith-based healing. These choices were not only cultural but practical: clinics can be far away, health care is costly, and people are unsure which symptoms truly demand a formal visit. Family and friends played a decisive role—many patients finally went to a clinic only after relatives insisted, or when symptoms became frightening, such as coughing up blood or being too weak to work.
Lost in a maze of clinics and wrong diagnoses
Once patients entered the health system, their path was rarely straightforward. People bounced between 2 and 12 different health facilities—health posts, local clinics, general hospitals, private centers, and finally big referral hospitals. Along the way, many were told they had pneumonia, a simple flu, asthma, malaria, typhoid, kidney infections, or, very often, tuberculosis. Some took months of TB drugs without improvement. Because Ethiopia has a heavy TB burden and limited scanning equipment, it is easy for lung cancer to hide behind more common diseases. Essential tests such as CT scans or biopsies were often only available in private centers or large city hospitals, adding more trips, more costs, and more delay. Repeated misdiagnoses left patients confused, exhausted, and sometimes ready to give up on the formal system.
Receiving the news and facing new hurdles
Most patients finally learned they had lung cancer in large teaching hospitals. Yet even at this stage, communication was often unclear. Some doctors hinted at the diagnosis instead of naming it; others told family members but not the patient directly. Many people felt they did not receive enough explanation or emotional support. Hearing the word “cancer” brought shock, fear, and thoughts of death—especially for those who had already lost a relative to the disease. A few patients responded by leaving the hospital to seek comfort through holy water or other spiritual care before returning, often sicker, to start medical treatment.
Long waits, high costs, and tough choices
After diagnosis, treatment did not start quickly. Median waits were five months from first symptoms to first clinic visit, nine more months to an accurate diagnosis, and about seven additional weeks to treatment. In a country of over 105 million people, there are only three centers that can provide radiation therapy, all in big cities. Patients may travel hundreds of kilometers, rent temporary rooms, and pay for food and transport for themselves and caregivers. Some sell livestock or other assets and borrow heavily to afford private "fast-track" care or drugs that are out of stock in public hospitals. Those who cannot pay face long queues—sometimes more than a year for radiation—or simply return home, placing their fate in God’s hands. Most eventually receive chemotherapy, with fewer getting surgery or radiation; by then, 85% are already in advanced stages where cure is unlikely.
What this means for people and policy
For lung cancer patients in Ethiopia, the road from first symptom to first treatment is long, winding, and littered with obstacles. Everyday coughs and chest pains are brushed aside, home and religious remedies are tried first, clinics struggle to spot cancer early, and specialized services are scarce and expensive. The study shows that saving lives will require more than one solution: people need better awareness that non-smokers can get lung cancer; frontline clinics need better tools and training to suspect cancer sooner; referral routes must be simpler; and treatment centers must be more numerous, affordable, and humane. Working with trusted traditional and religious leaders could also bring people into care earlier and support them emotionally along the way.
Citation: Estifanos, N., Egata, G., Addissie, A. et al. Pathways to lung cancer diagnosis and treatment among patients in Ethiopia: A qualitative study. Sci Rep 16, 7704 (2026). https://doi.org/10.1038/s41598-026-38876-y
Keywords: lung cancer, Ethiopia, diagnosis delay, patient journey, cancer care access