Clear Sky Science · en
Wnt/β -catenin signalling shapes macrophage behaviour during injury and repair in the mouse submandibular gland
Why Dry Mouth Matters
Xerostomia, or chronic dry mouth, is more than a minor annoyance. It can make eating painful, speaking difficult, and greatly increase the risk of infection and tooth decay. Many people develop severe dry mouth after head and neck radiotherapy or in autoimmune diseases such as Sjögren’s syndrome. Once the salivary glands are damaged, they often heal poorly, and current treatments mainly ease symptoms rather than restore function. This study explores how a specific group of immune cells, called macrophages, and a key cell‑communication route known as Wnt/β‑catenin signaling, work together to shape whether injured salivary glands scar or regenerate.
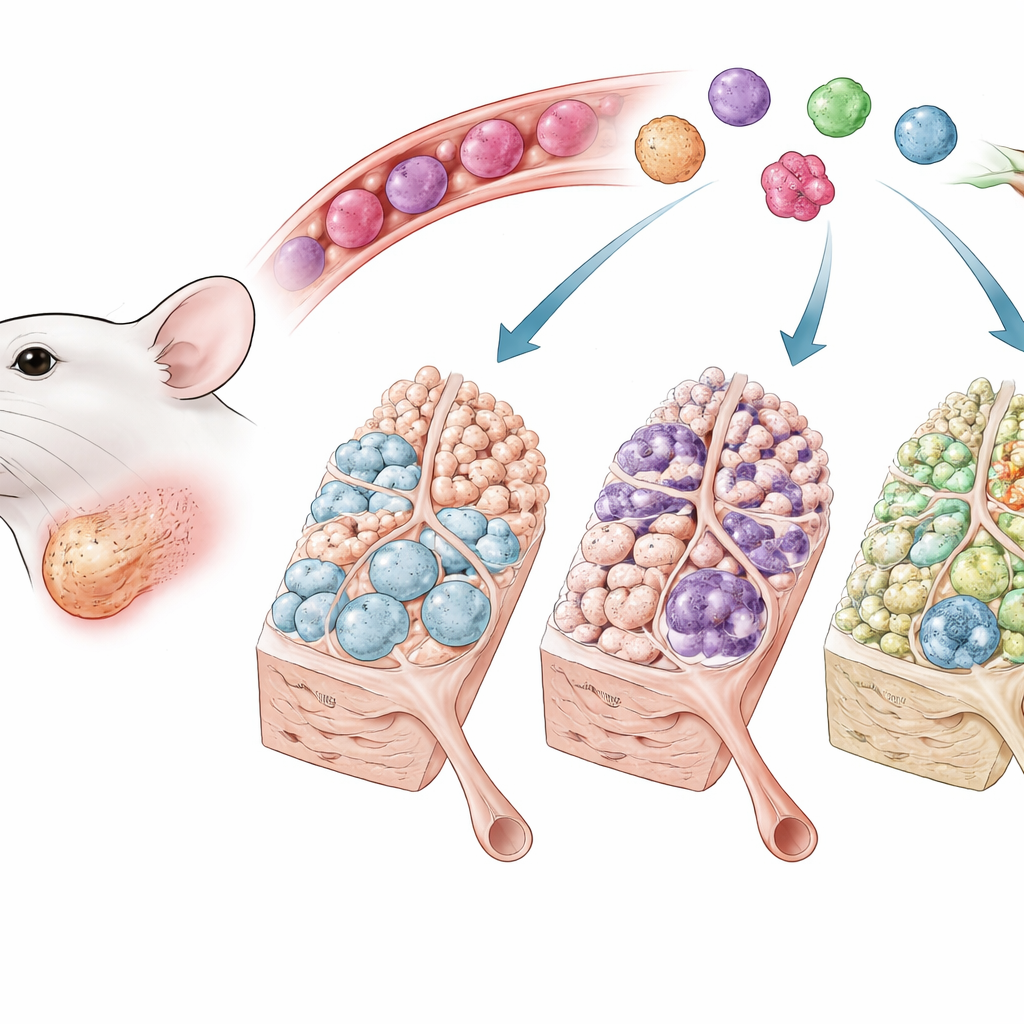
Guard Cells at the Gate
Salivary glands are packed with acinar cells that secrete saliva and ducts that carry it into the mouth. When the main duct is blocked, these delicate structures collapse, tissue becomes inflamed, and fibrous scar tissue accumulates. Macrophages are frontline immune cells that rush into injured tissue and can either fuel inflammation and scarring or help with calm, orderly repair. The authors used a well‑established mouse model in which the main duct of the submandibular gland is temporarily clamped to mimic obstructive injury, then reopened to allow recovery. They combined this model with genetic reporter mice that light up when Wnt/β‑catenin signaling is active, allowing them to see which cells are listening to this signal after injury.
Signals in the Supporting Tissues
After duct blockage, the researchers saw dramatic tissue damage: loss of acinar units, swollen ducts, and a thickened capsule rich in collagen. At the same time, they observed a surge of Wnt‑responsive cells, not inside the saliva‑producing units, but mainly in the supporting stroma—the capsule, internal partitions, and spaces between ducts and acini. Most of these Wnt‑responsive cells carried immune and macrophage markers, showing that macrophages are a major Wnt‑active population during injury. Gene‑expression measurements over time revealed that both a Wnt readout gene (Axin2) and a macrophage marker (F4/80) peaked around three and six days after injury, indicating that macrophage arrival and Wnt signaling are tightly linked during the early and mid‑stages of repair.
Macrophages as Both Senders and Receivers
To find out where the Wnt signals come from, the team measured all known Wnt genes in the damaged glands. Several were elevated, with Wnt2 and Wnt2b standing out as especially increased at both three and six days. Microscopy showed that these particular Wnt proteins were present inside macrophages, suggesting that the same cells releasing Wnt signals were also responding to them. Further experiments indicated that many of the Wnt‑active macrophages were recently recruited from the bloodstream rather than long‑term residents of the gland. In essence, injury draws in new macrophages that then switch on a Wnt‑driven feedback loop, potentially influencing how they behave and how surrounding support cells remodel the tissue.
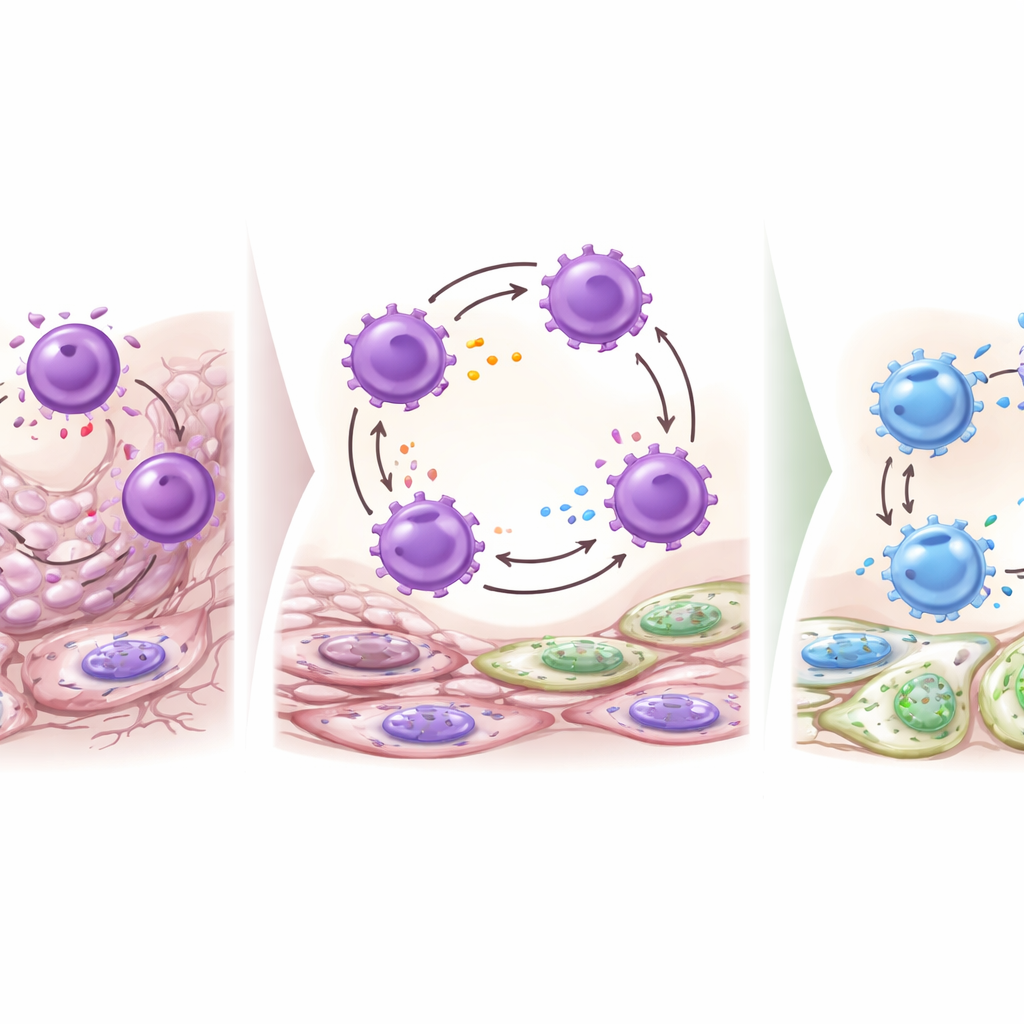
Scarring Versus Gentle Healing
The authors also asked whether Wnt‑responsive cells directly rebuild the acinar cells that produce saliva. Despite strong Wnt activity in both stromal and ductal cells after injury, lineage‑tracing experiments showed that these Axin2‑marked cells did not turn into new acinar cells once the duct was reopened and the gland recovered. Instead, they mainly contributed to duct maintenance. To test how Wnt signaling alters repair quality, the team partially disabled Wnt ligand secretion by removing a gene called Wntless (Wls) either broadly or specifically in Wnt‑responsive cells. In these mice, injured glands showed thinner fibrotic capsules, fewer dilated ducts, and a noticeable increase in CD206‑positive macrophages, a population generally associated with a more reparative, pro‑healing profile. This suggests that dialing down Wnt output nudges macrophages toward a gentler, less scarring response.
What This Means for People With Dry Mouth
Together, the findings position Wnt/β‑catenin signaling as a key switch that helps determine whether macrophages in an injured salivary gland support harmful fibrosis or more constructive repair. Macrophages in this system do not seem to rebuild saliva‑producing cells directly, but their signaling strongly influences the balance between scarring and regeneration in the gland’s supporting framework. For patients with radiation‑induced dry mouth or autoimmune salivary diseases, carefully targeting Wnt signaling in macrophages—rather than wiping these cells out—could one day help reduce scarring, restore healthier tissue architecture, and improve gland function. This work lays mechanistic groundwork for therapies that aim to reshape the healing environment of the salivary gland instead of simply replacing what has been lost.
Citation: Ahmed, A., Sachdeva, S., Whawell, S. et al. Wnt/β -catenin signalling shapes macrophage behaviour during injury and repair in the mouse submandibular gland. Sci Rep 16, 8972 (2026). https://doi.org/10.1038/s41598-026-38873-1
Keywords: salivary gland repair, macrophages, Wnt signaling, fibrosis, xerostomia