Clear Sky Science · en
Single cell RNA transcriptome response to fentanyl use in persons with HIV infection
Why this matters for people and public health
Fentanyl, a powerful synthetic painkiller driving today’s overdose crisis, is also widely used by people living with HIV. This study asks a question that matters to patients, clinicians, and policymakers alike: beyond overdoses, how does fentanyl use affect the immune system of people with HIV at the level of individual blood cells? By zooming in on hundreds of thousands of single cells, the researchers show that fentanyl use is linked to subtle but important shifts in how immune cells behave, which may help explain why some people with HIV who use opioids face worse health outcomes.
A closer look at HIV, fentanyl, and the immune system
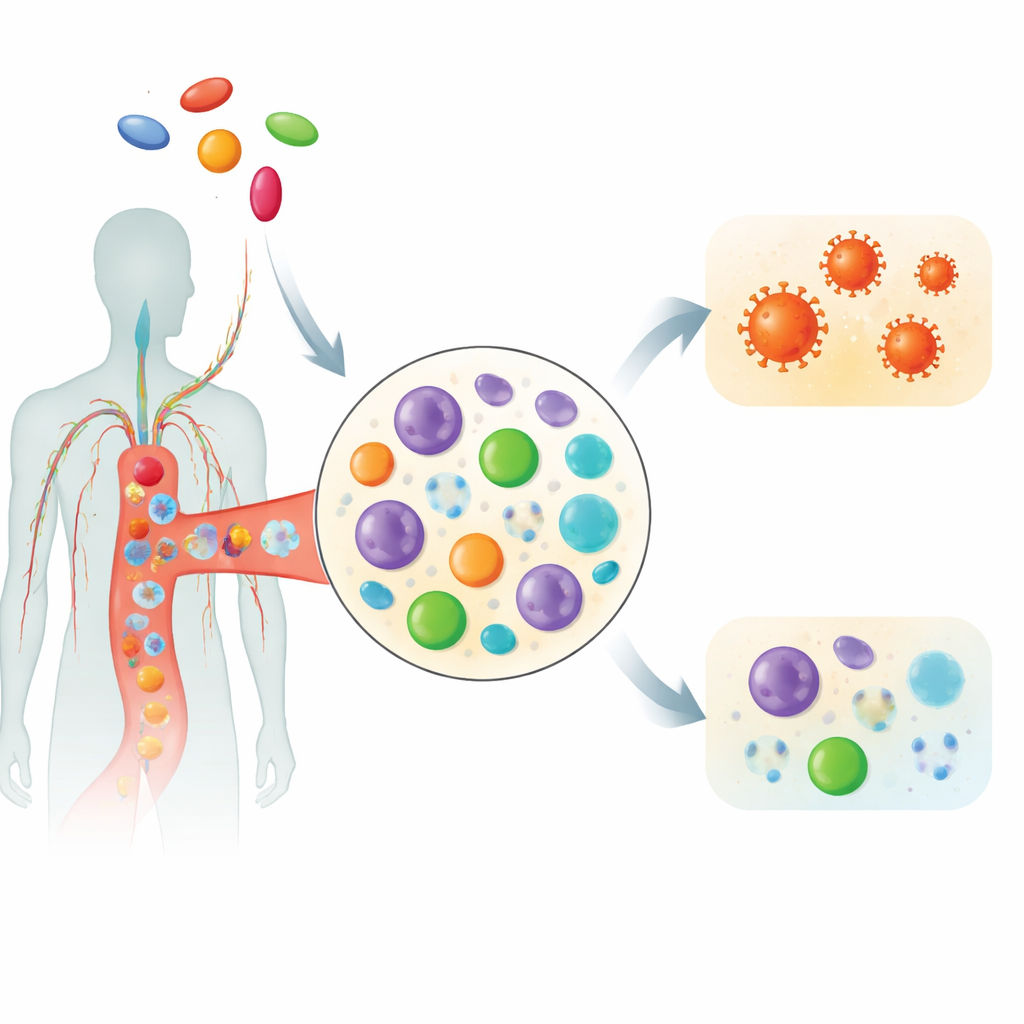
Opioids like fentanyl are best known for relieving pain and causing addiction, but they also act on the immune system. Earlier work had shown that various opioids can boost HIV’s ability to copy itself in lab-grown cells. Fentanyl, in particular, was found to increase HIV replication and the levels of cell-surface gateways the virus uses to enter cells. What had been missing was evidence from real people showing how ongoing fentanyl use might rewire the immune cells that circulate in the blood of those already living with HIV.
How the study was done in real patients
The researchers enrolled 17 adults living with HIV who were treated at emergency departments in the Cincinnati area, most of whom also had hepatitis C. Ten had a documented opioid use disorder and seven did not. Blood samples were collected and carefully processed to isolate peripheral blood mononuclear cells, a mixed population that includes T cells, B cells, monocytes, natural killer (NK) cells, and dendritic cells. Using single-cell RNA sequencing, a technology that reads out which genes are switched on in individual cells, the team profiled more than 216,000 cells and then compared patterns of gene activity between opioid-using and non-using participants, while accounting for sex and hepatitis C status.
What changed in the blood’s defender cells
At first glance, the overall mix of major immune-cell types looked similar in people with and without opioid use, with one notable exception: NK cells were significantly less frequent in those using opioids. NK cells help kill virus-infected cells and are an important early line of defense in HIV infection, so a drop in their numbers could weaken immune control. When the team examined gene activity cell by cell, they found dozens of genes turned up or down across key cell types. CD4 and CD8 T cells, monocytes, B cells, dendritic cells, and NK cells all showed distinct sets of genes that differed between opioid-positive and opioid-negative participants, suggesting that fentanyl use leaves a broad molecular fingerprint on the immune system.
Signals of antiviral alarm and viral opportunity
Many of the altered genes clustered in pathways involved in antiviral defense, particularly those driven by type I interferons, the body’s early alarm signal against viruses. In T cells, B cells, monocytes, and dendritic cells, genes tied to interferon responses, viral genome replication, and innate immunity were enriched. Some antiviral factors, such as interferon-induced transmembrane proteins (IFITMs) and ISG15, were more active in opioid-using individuals; these molecules can block HIV entry or release from cells but are also linked to higher viral loads and immune activation in people with HIV. Other genes, including those that influence cell death, inflammation, and viral reactivation, were also shifted. Together, these patterns point to a state in which immune cells are simultaneously more alarmed and, in some ways, more permissive to ongoing HIV activity.
What this could mean for people living with HIV
This work does not prove that fentanyl directly worsens HIV disease in every user, and it has limitations, including a small sample size and uncertainty about how long and how often participants used opioids or other drugs. Still, by showing that opioid use is linked to fewer NK cells and widespread changes in antiviral genes across multiple blood cell types, the study highlights concrete biological pathways through which fentanyl might shape HIV’s course. Understanding these cell-level changes can help clinicians better manage care for people with both HIV and opioid use disorder and may guide the development of new treatments that target these pathways, ultimately improving health outcomes in a population facing overlapping epidemics.
Citation: Roskin, K.M., Meeds, H.L., Krishnan, J.M. et al. Single cell RNA transcriptome response to fentanyl use in persons with HIV infection. Sci Rep 16, 7988 (2026). https://doi.org/10.1038/s41598-026-38854-4
Keywords: fentanyl, HIV, opioid use disorder, immune cells, single-cell RNA sequencing