Clear Sky Science · en
Protective effect of Baicalin against doxorubicin-induced cytotoxic and electrophysiological damage in human iPSC-cardiomyocytes
Why this matters for cancer patients’ hearts
Chemotherapy drugs like doxorubicin save lives, but they can also quietly injure the heart, with problems that sometimes appear years after treatment. This study explores whether baicalin, a plant-derived compound already known for its antioxidant and anti-inflammatory actions, can shield human heart cells from doxorubicin’s harmful side effects. Using heart cells grown from human stem cells, the researchers ask a simple but crucial question: can we protect the heart without weakening cancer treatment?
A powerful cancer drug with a hidden cost
Doxorubicin is widely used to treat many cancers, yet it can damage the heart muscle, leading to rhythm problems, weakened pumping, and in severe cases, heart failure. Some patients experience short-term electrical disturbances right after treatment, while others develop long-term, often irreversible, heart disease long after their cancer therapy ends. This damage is linked to a burst of reactive molecules, activation of cell death pathways, and structural breakdown inside heart muscle cells, which have limited ability to regenerate. Despite intense research, doctors still lack widely usable drugs that reliably prevent this heart injury in people receiving doxorubicin.
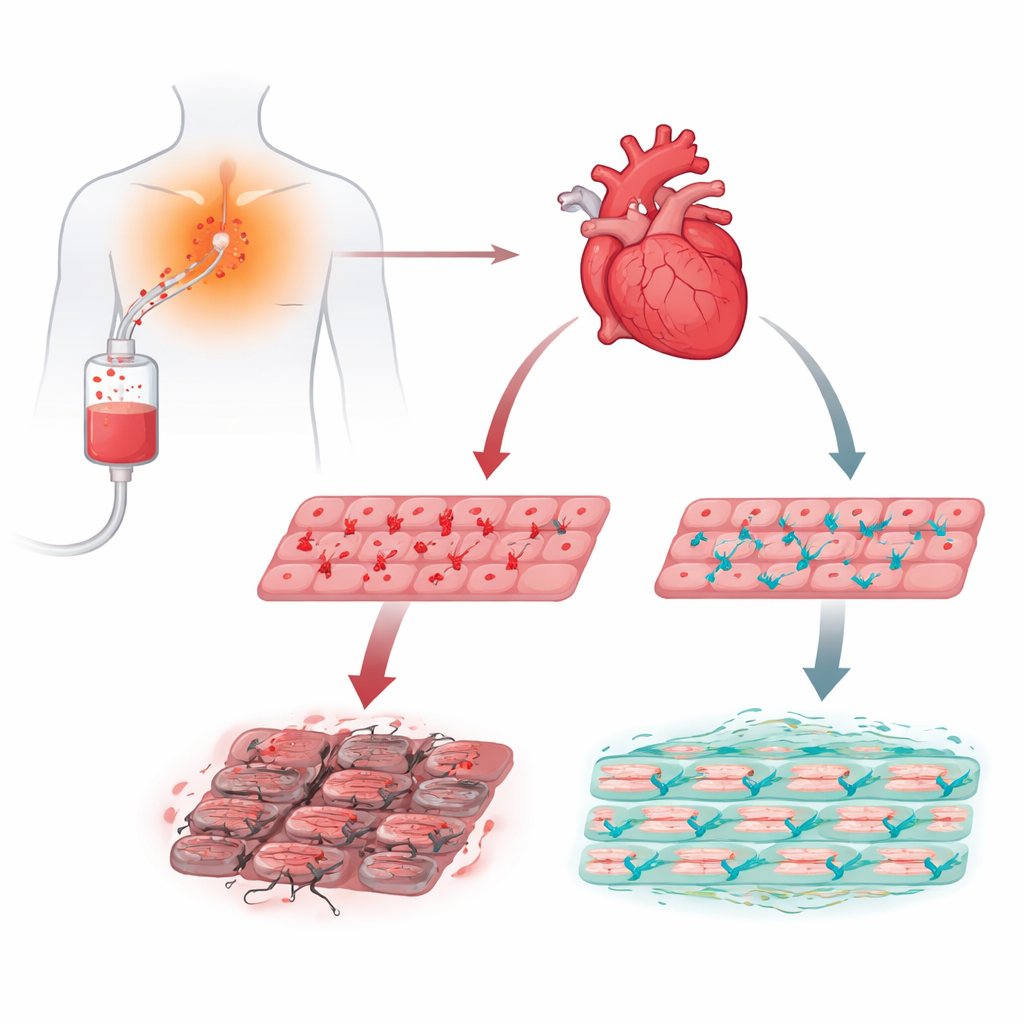
A natural compound put to the test
Baicalin is extracted from the roots of the plant Scutellaria baicalensis and has shown heart-protective effects in animal models. To test its effects in a more human-like setting, the researchers used cardiomyocytes—beating heart cells—derived from human induced pluripotent stem cells. These laboratory-grown cells mimic many key aspects of human heart tissue and can be monitored for both survival and electrical activity over time. The team first pretreated the cells with different amounts of baicalin, then exposed them to either a high, short burst of doxorubicin (to mimic acute injury) or a lower, longer exposure (to mimic chronic treatment), closely tracking how the cells fared.
Keeping heart cells alive and structurally sound
When exposed to doxorubicin alone, the heart cells showed clear signs of distress: fewer living cells, more dead and dying cells, and strong signals of DNA damage and oxidative stress. Under the microscope, their internal contractile machinery—organized stripes formed by proteins like α-actinin and troponin—became patchy and disordered, a hallmark of weakened muscle function. Adding baicalin, especially at medium and higher doses, dramatically reduced cell death in both short- and long-term treatments. The compound cut back the build-up of reactive oxygen species, lessened DNA damage, and preserved the regular striped pattern of the contractile fibers. Importantly, baicalin alone did not trigger extra cell death, suggesting it was safe in this human cell model.
Protecting the heart’s electrical rhythm
The heart’s job is not only to beat strongly but also to beat in a coordinated rhythm. Using multielectrode array technology, the authors recorded the electrical signals traveling across the cell layer. Long-term exposure to doxorubicin slowed conduction between cells, reduced signal strength, and altered timing measures related to how long each beat takes to repolarize, changes that are linked to arrhythmias and poor pumping in patients. Baicalin co-treatment largely stabilized these electrical measures: signal duration, beat-to-beat intervals, conduction speed, and action potential shape moved back toward normal, even though doxorubicin was still present. This suggests that baicalin helps maintain both the wiring and the working strength of the heart cells.
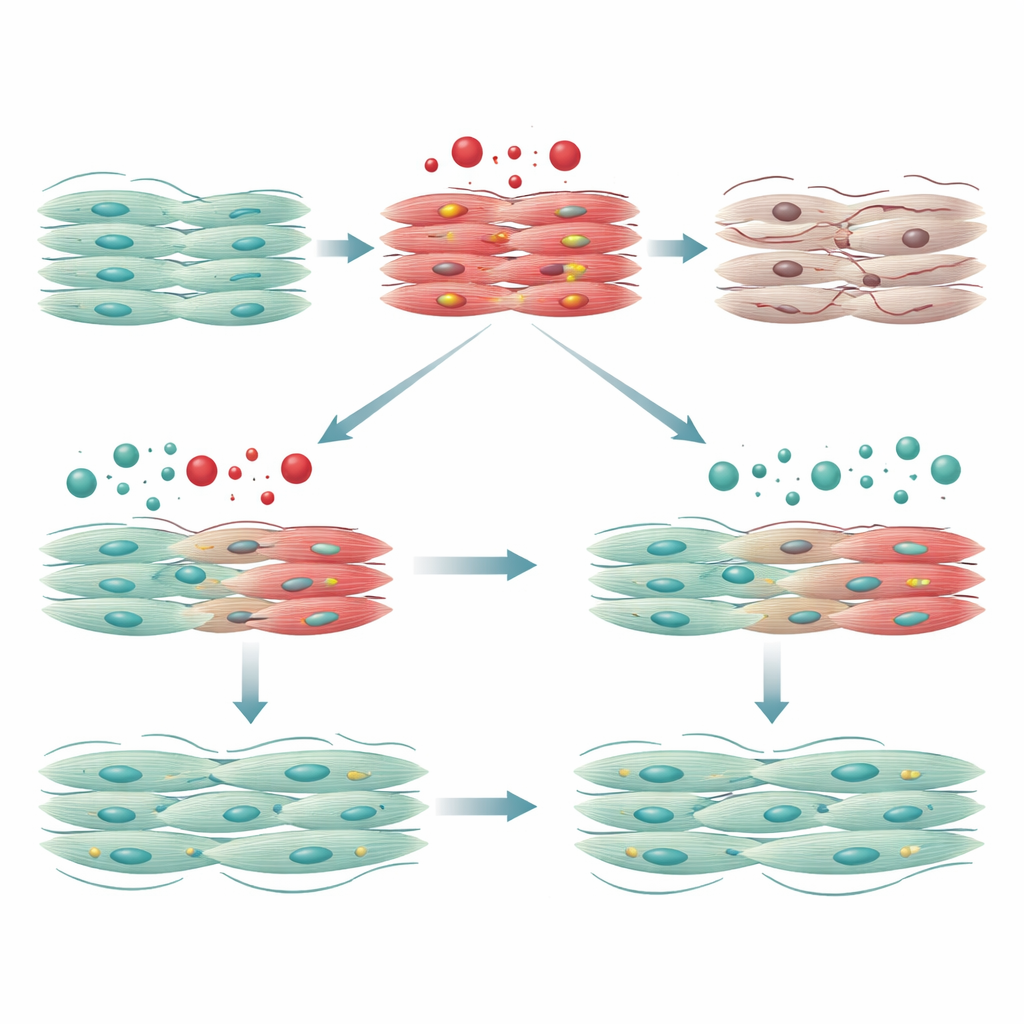
What this could mean for future therapies
Taken together, the results show that baicalin can shield human heart-like cells from many of doxorubicin’s worst effects, from oxidative stress and DNA damage to structural breakdown and electrical instability. While these experiments were done in a dish and not in patients, they provide a strong scientific rationale to explore baicalin, or better-delivered versions of it, as an add-on therapy during chemotherapy. If future animal and clinical studies confirm these findings, cancer patients might one day receive a companion treatment that helps preserve their hearts while their chemotherapy fights their tumors.
Citation: Ulivieri, A., Lavra, L., Magi, F. et al. Protective effect of Baicalin against doxorubicin-induced cytotoxic and electrophysiological damage in human iPSC-cardiomyocytes. Sci Rep 16, 8059 (2026). https://doi.org/10.1038/s41598-026-38838-4
Keywords: doxorubicin cardiotoxicity, baicalin, cardioprotection, stem cell–derived cardiomyocytes, chemotherapy side effects