Clear Sky Science · en
Resting-state fMRI reveals immediate hemodialysis-related changes in cognitive function and brain network connectivity in end-stage renal disease
Why brain changes during dialysis matter
For people whose kidneys have failed, hemodialysis is a lifeline that cleans the blood several times a week. Yet many of these patients struggle with memory, concentration, and mood. This study asks a pressing question for patients and families: what happens inside the brain during a single dialysis session, and can those changes help explain the day‑to‑day swings in thinking and attention that many experience?
Kidney failure, thinking problems, and the brain at rest
End-stage renal disease means the kidneys can no longer filter wastes and maintain the body’s internal balance. Hemodialysis replaces part of this work by circulating blood through a machine. While this treatment extends life, up to seven in ten patients develop problems with attention, processing speed, and planning. To explore why, the researchers used resting-state functional MRI, a technique that tracks natural, ongoing activity in the brain when a person is lying quietly in the scanner. This activity reveals large communication systems, or networks, that support hearing, movement, vision, and higher mental functions such as attention and daydreaming.
Tracking patients before and after one dialysis session
The team studied 20 dialysis patients and 22 healthy volunteers of similar age and sex. Patients completed thinking tests and then underwent brain scans both before and after a regular dialysis session. At the same time, the researchers measured blood chemicals related to kidney function, salts, and hormones. Using a method called independent component analysis, they separated the brain data into eight major networks, including attention, sensory, and default mode networks. They then compared how strongly these networks were connected with each other across the three situations: patients before dialysis, patients after dialysis, and healthy people.
What changed in the blood and what stayed the same
As expected, one dialysis session sharply improved standard kidney measures. Levels of urea and creatinine, two waste products that build up when kidneys fail, dropped to a fraction of their starting values, and overall filtering capacity rose more than threefold. A key hormone involved in bone and mineral balance also fell. Some salts in the blood shifted in specific ways: potassium and phosphorus decreased, while calcium rose modestly. Other salts, such as sodium, magnesium, bicarbonate, and chloride, hardly changed at all, and iron-related measures remained stable. In short, dialysis quickly cleared wastes and adjusted certain minerals, without drastically disturbing the overall salt balance.
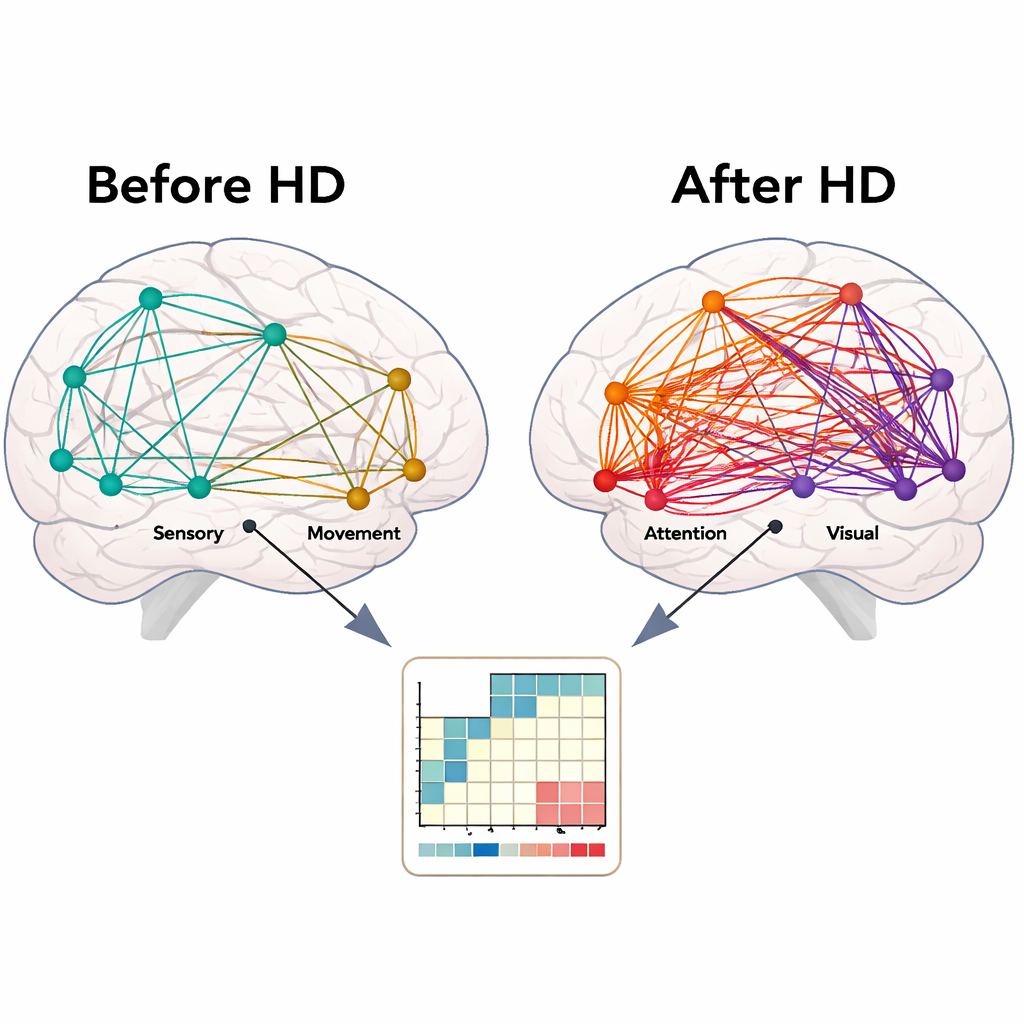
Brain networks that weaken and rebound with dialysis
Compared with healthy volunteers, patients showed weaker links between brain networks that handle sound, movement, and attention, both before and after dialysis. This suggests long-lasting problems with how sensory information is integrated and used to guide actions. At the same time, some connections shifted acutely with dialysis. After treatment, communication between attention-related networks and between visual and attention networks increased. Patients whose attention networks were initially less connected tended to show bigger gains on a test of processing speed after dialysis, and those whose network connections strengthened the most also showed the greatest mental improvement. Surprisingly, higher pre-dialysis levels of chloride, a common blood salt, were linked to weaker attention-network connections after dialysis, hinting that even subtle, chronic changes in chemistry may shape brain function.
What this means for patients and care
For a layperson, the message is that dialysis affects far more than the kidneys. Within a single treatment, the brain’s communication networks can reorganize, and these shifts track with short-term changes in thinking skills. Some networks remain chronically impaired, but others appear flexible and partly recover as blood chemistry improves. These early findings suggest that monitoring mind and mood around dialysis sessions—possibly with brain scans in research settings—could help doctors spot patients at risk of cognitive decline and guide more personalized care. While larger, longer-term studies are needed, the work offers a window into the hidden brain changes that accompany each life-sustaining trip to the dialysis machine.
Citation: Du, T., Zeng, Z., Guo, D. et al. Resting-state fMRI reveals immediate hemodialysis-related changes in cognitive function and brain network connectivity in end-stage renal disease. Sci Rep 16, 7398 (2026). https://doi.org/10.1038/s41598-026-38807-x
Keywords: hemodialysis, cognitive function, brain networks, functional MRI, end-stage renal disease