Clear Sky Science · en
8-OHdG and NT-proBNP as complementary biomarkers in the postmortem diagnosis of acute ischemic heart disease
Why sudden heart deaths are hard to explain
When someone dies suddenly, especially from a suspected heart problem, families and doctors alike want clear answers. Yet in many cases of acute ischemic heart disease—when blood flow to the heart is abruptly cut off—the heart tissue can look surprisingly normal under the microscope, particularly if death occurs early. This study explores whether two tiny molecular clues left behind after death can help forensic doctors more reliably tell when the heart was truly the culprit, even when standard tests fall short.
Two hidden warning signals inside the heart
The researchers focused on two substances that reflect different types of stress on the heart. The first, called 8-OHdG, appears when DNA inside heart cells is damaged by oxidative stress, a kind of chemical “rusting” that happens during a heart attack. The second, NT-proBNP, is a hormone fragment released into the blood when the heart wall is under strain, such as during heart failure or a serious shortage of blood supply. Together, these two markers were tested as a pair of complementary clues: one from inside the heart cells, the other circulating in the bloodstream.
Studying hearts after sudden and unexpected deaths
The team analyzed 67 forensic autopsy cases. Thirty-three people had died suddenly from acute ischemic heart disease, and 34 had died from other causes such as drowning, fire, trauma, or poisoning, with no clear heart damage. Importantly, even in the heart-disease group, classic signs of a full-blown heart attack—large areas of dead tissue—were often missing or very subtle. This makes such cases particularly challenging, because routine tissue stains can show only mild changes that are hard to interpret. By looking at both heart tissue and postmortem blood, the researchers aimed to see whether 8-OHdG and NT-proBNP could distinguish heart-related deaths from others.
What the molecular fingerprints revealed
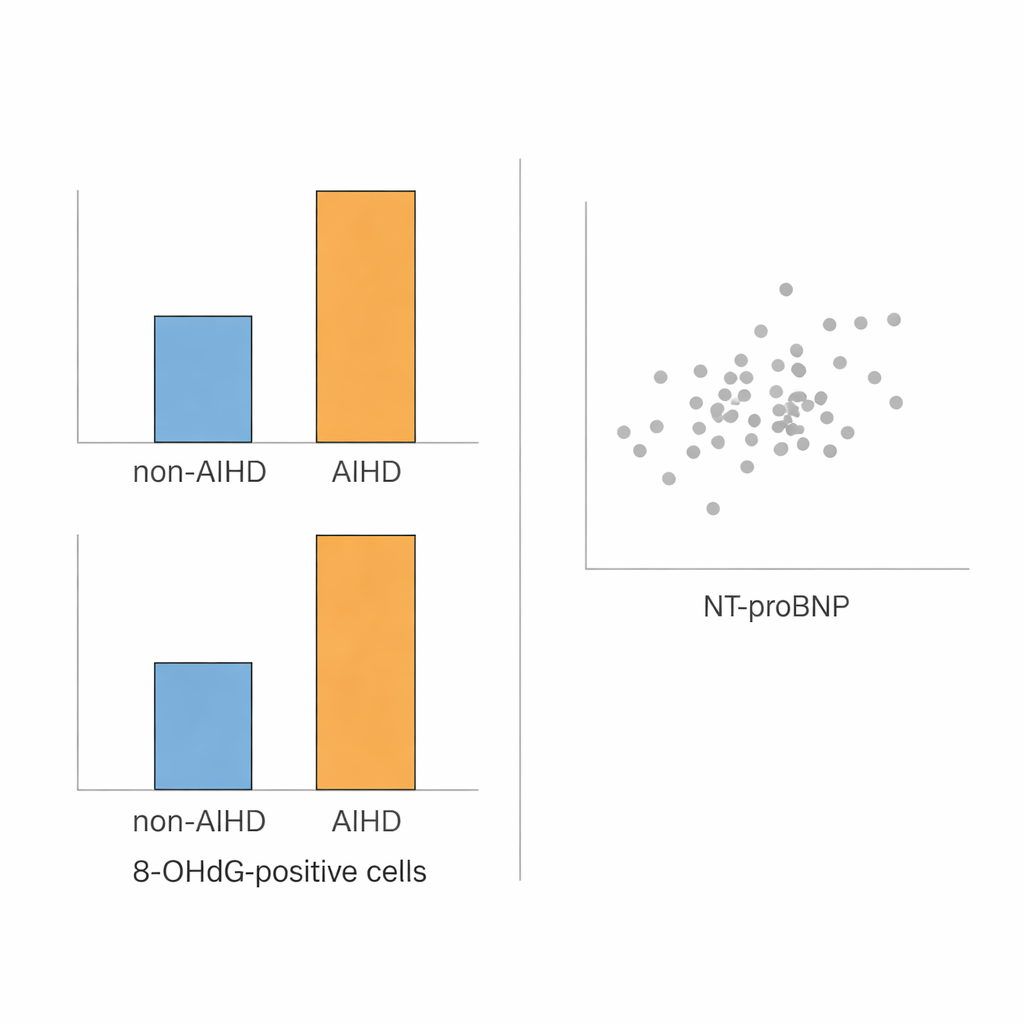
Under the microscope, the scientists stained heart samples to highlight 8-OHdG inside the cell nuclei. They found that hearts from the ischemic heart disease group showed many more nuclei rich in 8-OHdG, and the staining was more widespread, than in hearts from people who died of non-cardiac causes. Blood tests told a similar story from a different angle: NT-proBNP levels were more than twice as high, on average, in the heart-disease group as in the others. These differences held up across a range of ages, times since death, and in both men and women, suggesting that the markers remained relatively stable and were not simply artifacts of decomposition or demographics.
Different stories, stronger together
An intriguing finding was that the two markers did not move in lockstep. Higher 8-OHdG in heart cells did not reliably line up with higher NT-proBNP in the blood, and 8-OHdG levels did not track with other microscopic features like contraction bands, or with the time between death and autopsy. This lack of correlation suggests that each marker is telling a different part of the story: 8-OHdG reflects direct oxidative injury to the heart’s DNA, while NT-proBNP reflects how hard the heart was working under stress. Because they capture distinct processes, using them together can give forensic pathologists a more complete picture in cases where traditional signs of a heart attack are faint or absent.
What this means for understanding sudden heart death
For families and investigators seeking clarity after a sudden, unexplained death, these findings offer a promising step forward. The study suggests that measuring oxidative DNA damage in heart tissue alongside a stress hormone in postmortem blood can sharpen the diagnosis of acute ischemic heart disease, especially in “borderline” cases where the heart looks almost normal. While the authors acknowledge limitations—such as not including every possible comparison group and the complex effects of other illnesses—they conclude that this two-marker approach could become a valuable addition to forensic practice, helping to reveal when a seemingly quiet heart was in fact at the center of a fatal event.
Citation: Kuninaka, Y., Ishida, Y., Grimaldi, F. et al. 8-OHdG and NT-proBNP as complementary biomarkers in the postmortem diagnosis of acute ischemic heart disease. Sci Rep 16, 6154 (2026). https://doi.org/10.1038/s41598-026-38797-w
Keywords: sudden cardiac death, ischemic heart disease, forensic biomarkers, oxidative DNA damage, NT-proBNP