Clear Sky Science · en
Proteomic profiling of equine airway mucus reveals compositional changes in asthmatic phenotypes
Why Horse Airway Mucus Matters
Anyone who has watched a horse cough through a dusty ride has seen how breathing problems can limit an animal’s health and performance. In many horses, a chronic form of “asthma” leads to thick, sticky mucus that clogs the airways. This study set out to look closely at what that mucus is actually made of, using modern protein analysis tools. By comparing mucus from healthy horses and from those with mild to moderate or severe asthma, the researchers hoped to uncover molecular clues that explain why the mucus becomes so abnormal—and how those clues could guide better diagnosis and treatment.
Two Kinds of Asthma in Horses
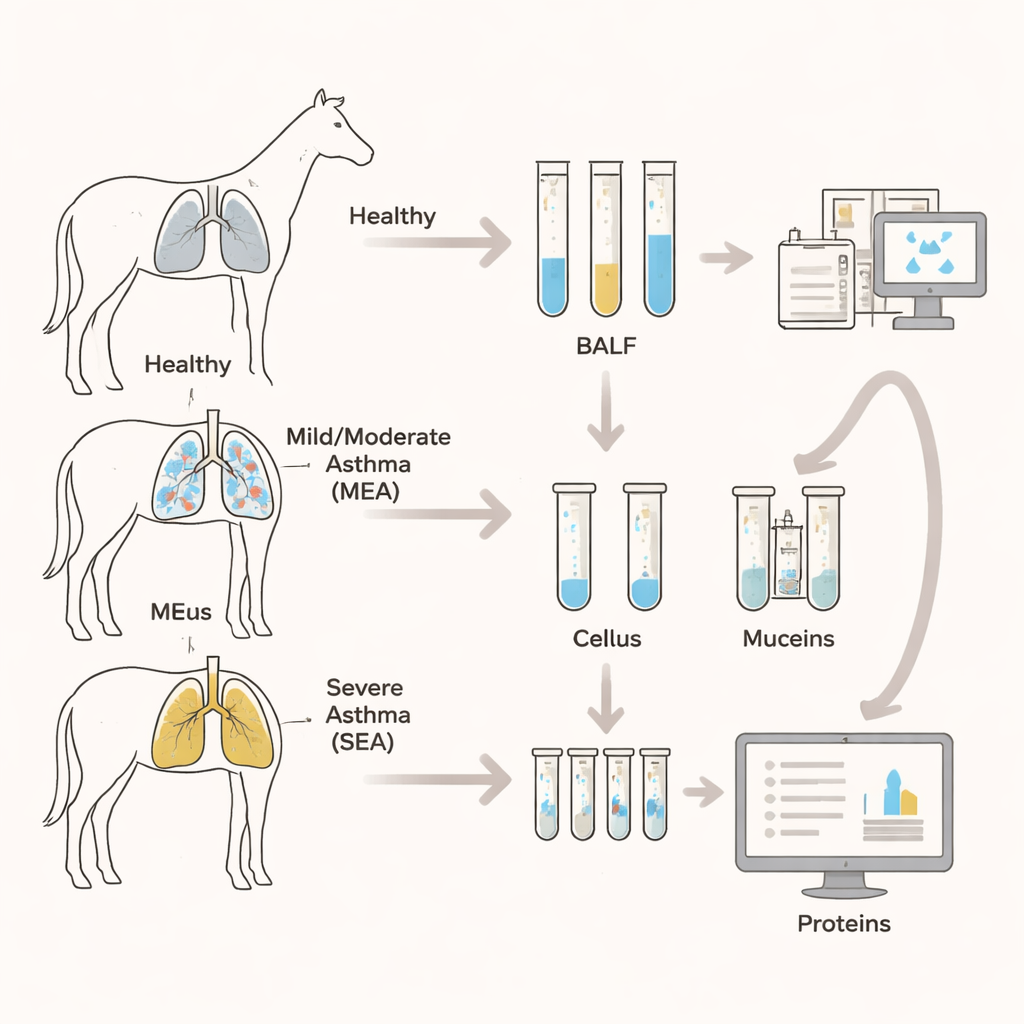
Equine asthma is one of the most common non-infectious lung diseases in horses. It comes in two main forms: mild to moderate equine asthma (MEA), which often affects younger or middle-aged horses and shows up as occasional coughing and reduced performance; and severe equine asthma (SEA), which usually strikes older horses and causes frequent coughing, clear breathing difficulty at rest, and heavy mucus plugging of the small airways. In both forms, the airways fill with excess mucus and inflammatory cells, especially a type of white blood cell called a neutrophil. Because horses share many features of human asthma, understanding what happens in their airway mucus can also provide insight into human disease.
Peering Into the Mucus with Protein Mapping
The team collected fluid washed from the horses’ lower airways, then isolated just the mucus portion and broke its proteins into smaller fragments for detailed measurement by mass spectrometry. This technique allowed them to identify and quantify 2,275 different proteins in the mucus samples from eight healthy horses, six with MEA, and ten with SEA. Overall, healthy and asthmatic horses shared most of the same proteins, but some proteins were found only in diseased or only in healthy animals, and their relative amounts often differed. When the researchers used statistical methods to group samples based on protein patterns, healthy horses clearly clustered apart from asthmatic horses, highlighting a distinct “asthma fingerprint” in the mucus, even though the two asthma severities overlapped.
Key Mucus Proteins That Shift in Disease
Among the many proteins, special attention focused on mucins—the large, sugar-rich molecules that give mucus its gel-like character. Two gel-forming mucins, MUC5AC and MUC5B, and two membrane-tethered mucins, MUC1 and MUC4, were all detected. MUC5AC was higher in both asthma types than in healthy controls, while MUC5B rose mainly in the severe form, matching the stickier mucus and airway plugs seen in those horses. MUC1 did not show clear differences. In contrast, MUC4 stood out: it was strongly increased in both MEA and SEA, closely tracked the number of neutrophils in the airway, and almost perfectly separated healthy from asthmatic horses in diagnostic performance tests. Other mucus-associated proteins, including enzymes that shape the sugar side chains on mucins and water-channel proteins called aquaporins, also shifted, suggesting that the mucus in asthma is not just more abundant, but chemically and physically different.
Inflammation, Remodeling, and Immune Defense
By feeding the protein lists into pathway and function databases, the researchers saw a strong signature of inflammation and stress responses in both asthma types. Many of the increased proteins were linked to innate immunity, neutrophil activity, and blood clotting processes. Structural proteins of the airway lining and components of the surrounding support matrix were also enriched, indicating ongoing tissue remodeling. Interestingly, mild to moderate asthma showed a relatively stronger signal for changes in the extracellular matrix and clot-related pathways, hinting that remodeling of the airway wall begins early, even before disease becomes clinically severe. Several immune proteins that help transport and assemble antibodies in mucus, such as the polymeric immunoglobulin receptor (PIGR) and the joining chain JCHAIN, were also higher in asthmatic mucus, consistent with an activated local immune defense that could be driven by inhaled molds or other environmental triggers.
What This Means for Horses and Beyond
To a non-specialist, the central message is that in equine asthma the problem is not just “too much” mucus—it is mucus with a different recipe. The balance of gel-forming mucins, surface mucins like MUC4, water-handling channels, and immune factors all shifts in ways that likely make the mucus thicker, stickier, and harder to clear. These compositional changes align with the observed buildup of mucus plugs and the presence of large numbers of neutrophils in the airways. Because some of these proteins, especially MUC4 and several antibody-related components, can distinguish healthy from asthmatic horses very well, they may serve as future biomarkers to diagnose asthma or track how well treatments are working. The work also reinforces the value of horses as a model for human asthma, showing how close study of a single, slimy material—airway mucus—can reveal much about the health of the lungs.
Citation: Bartenschlager, F., Kuropka, B., Schmitz, P. et al. Proteomic profiling of equine airway mucus reveals compositional changes in asthmatic phenotypes. Sci Rep 16, 5880 (2026). https://doi.org/10.1038/s41598-026-38766-3
Keywords: equine asthma, airway mucus, mucins, proteomics, horse respiratory disease