Clear Sky Science · en
24-hour ambulatory blood pressure and associated factors in women with polycystic ovary syndrome compared with ovulatory controls
Why this study matters for women’s health
Many women with polycystic ovary syndrome (PCOS) worry about more than irregular periods and unwanted hair growth. Doctors increasingly suspect that PCOS may quietly strain the heart and blood vessels years before any symptoms appear. This study asks a simple but important question: do women with PCOS go through the day with slightly higher blood pressure than women without PCOS, even if they are the same age and have similar body size? By tracking blood pressure around the clock, the researchers shed light on a hidden layer of cardiovascular risk and what might be driving it.
Looking at blood pressure over a full day
Most clinic visits capture blood pressure at a single moment, in a calm room, with the patient sitting still. That snapshot can miss important swings that occur during work, chores, and sleep. To get a fuller picture, the researchers used 24-hour ambulatory blood pressure monitoring: women wore a portable cuff that took automatic readings throughout the day and night. The team studied 100 non-smoking women, ages 18 to 44. Half had PCOS, diagnosed using standard criteria that consider menstrual patterns, hormone levels, and ovary appearance on ultrasound. The other half had regular cycles and no signs of excess male hormones. None had been diagnosed with high blood pressure or were taking hormonal contraceptives.
PCOS and an unfavorable health profile
Although the women with and without PCOS were similar in age, their overall health profiles differed. Women with PCOS tended to have a higher body mass index (BMI) and larger waistlines, pointing to more body fat and abdominal fat. Their blood tests also painted a more worrisome picture: higher fasting insulin and long-term blood sugar (HbA1c), higher triglycerides, and slightly higher creatinine, a marker related to kidney function. Inflammatory signals such as TNF-alpha were also elevated. At the same time, key female hormones like estradiol and progesterone were lower. Taken together, these findings confirm that PCOS is strongly linked to a cluster of metabolic and hormonal changes that can stress the heart and circulation over time.
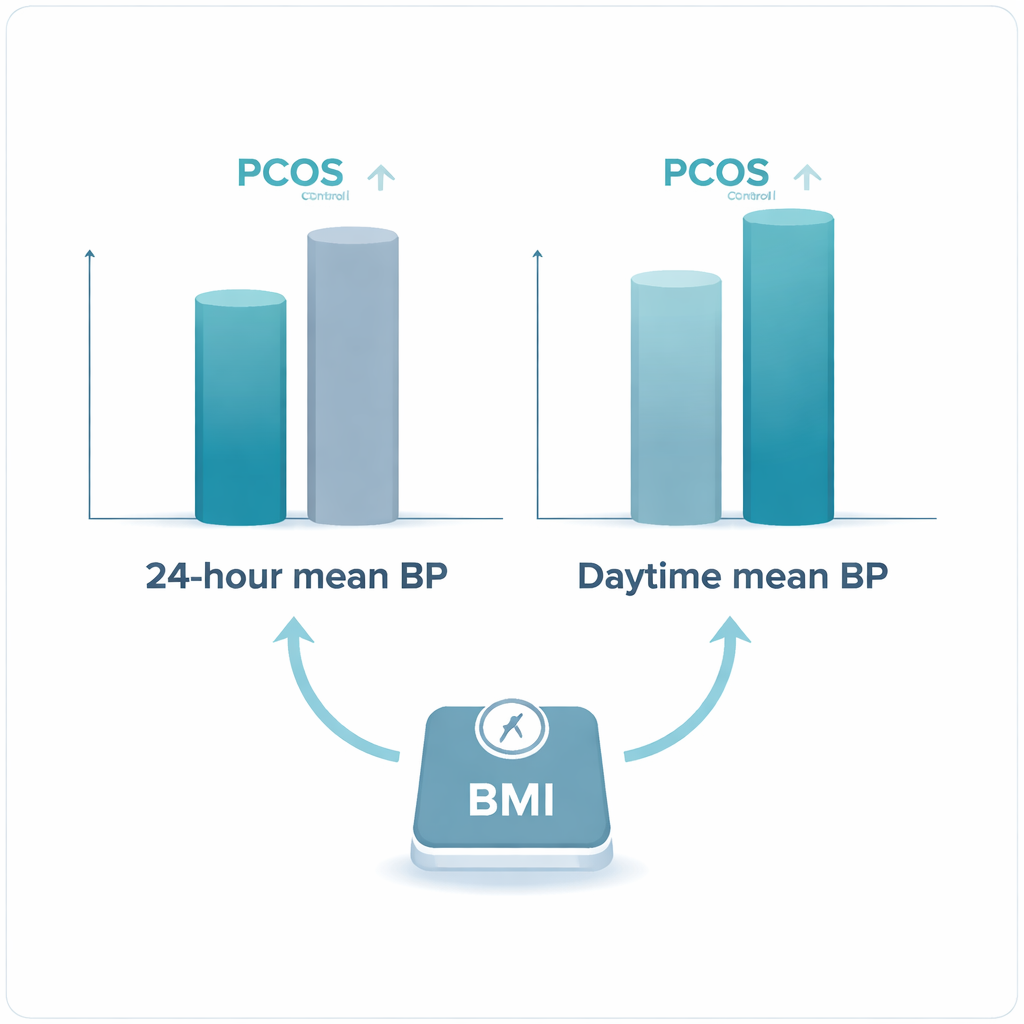
Daytime blood pressure runs higher in PCOS
When the researchers compared blood pressure data, they found that women with PCOS had higher average readings across the 24-hour period than the control group. The differences were modest—on the order of three millimeters of mercury for overall and daytime mean pressure—but they persisted even after adjusting for BMI. In other words, the higher blood pressure could not be explained simply by the fact that many women with PCOS were heavier. The gap was most pronounced during daytime hours, when participants were awake and active. At night, blood pressure levels in the two groups were more similar, suggesting that the natural nighttime “dip” in pressure is mostly preserved in PCOS. Heart rate followed a similar pattern: women with PCOS showed slightly faster pulses over 24 hours and during the day, hinting at a more activated nervous system.
Weight as a central piece of the puzzle
To understand which health factors best predicted blood pressure within the PCOS group, the scientists ran a statistical analysis that weighs many variables at once and keeps only those that truly add information. Across 24-hour, daytime, and nighttime readings, BMI emerged as the single most consistent factor linked to higher blood pressure. In specific cases, waist size, long-term blood sugar, and creatinine also played a role, but most hormones and inflammatory markers dropped out of the models. This pattern suggests that overall body fat—and the many changes that travel with it—may act as a powerful summary of cardiovascular strain in women with PCOS. However, the authors caution that their models had only moderate accuracy and that unmeasured lifestyle habits such as diet, sleep, and physical activity likely matter as well.
What this means for women living with PCOS
For women with PCOS, the study sends a clear message: even small, hidden increases in blood pressure during everyday life may nudge long-term heart risk upward, especially when combined with extra weight and other metabolic problems. Standard in-office readings may look normal and still miss these subtle rises. The findings support asking doctors about 24-hour blood pressure monitoring, particularly for women with PCOS who are overweight or have borderline blood tests. Just as important, the strong link between BMI and blood pressure highlights the value of lifestyle changes—such as healthier eating patterns and regular physical activity—that promote weight control. While more and larger studies are needed, this work reinforces that PCOS is not only a reproductive condition but also a whole-body syndrome that deserves careful cardiovascular follow-up.
Citation: de Fátima Azevedo, M., Rocha, A.K.C., de Melo, L.M.B. et al. 24-hour ambulatory blood pressure and associated factors in women with polycystic ovary syndrome compared with ovulatory controls. Sci Rep 16, 7215 (2026). https://doi.org/10.1038/s41598-026-38731-0
Keywords: polycystic ovary syndrome, ambulatory blood pressure, cardiometabolic risk, body mass index, women’s cardiovascular health