Clear Sky Science · en
Impact of vitamin D deficiency on clinical outcomes in non-traumatic subarachnoid hemorrhage: A single-center prospective cohort study
Why Sunshine Vitamins Matter After a Brain Bleed
Subarachnoid hemorrhage—a sudden, often devastating bleed around the brain—can strike without warning and leave survivors with lasting disability. This study asks a surprisingly everyday question with serious consequences: could something as simple as low vitamin D levels help determine who recovers and who does not? By tracking patients with brain bleeds and measuring their vitamin D soon after arrival in the hospital, the researchers explored links between this “sunshine vitamin,” inflammation, infections, and long-term recovery.
Following Patients From Crisis to Recovery
The research team followed 115 adults admitted to a Hungarian intensive care unit with non-traumatic subarachnoid hemorrhage. Within 24 hours, each patient had a blood test to measure 25-hydroxyvitamin D, the standard marker of vitamin D status. Patients were then divided into two groups: those with low vitamin D and those with levels considered sufficient. Over the next three weeks, doctors closely monitored them for brain complications, infections, and changes in blood markers of inflammation. Recovery was assessed at 14, 30, and 90 days using widely used scales that capture how independently a person can live after a brain injury.
Low Vitamin D Tied to More Brain Damage
Although patients with and without vitamin D deficiency looked similar in age, disease severity, and treatment, their brains did not fare equally over time. Follow-up brain scans showed that patients with low vitamin D were much more likely to develop new areas of ischemia—patches of brain tissue damaged by a lack of blood flow—than those with adequate levels. Importantly, this higher rate of new brain injury was not explained by more frequent vessel narrowing (vasospasm), suggesting that vitamin D might influence how the brain responds to injury rather than how often blood vessels constrict. Statistical modeling indicated that vitamin D deficiency was independently associated with delayed cerebral ischemia, a major driver of poor outcomes after these hemorrhages.
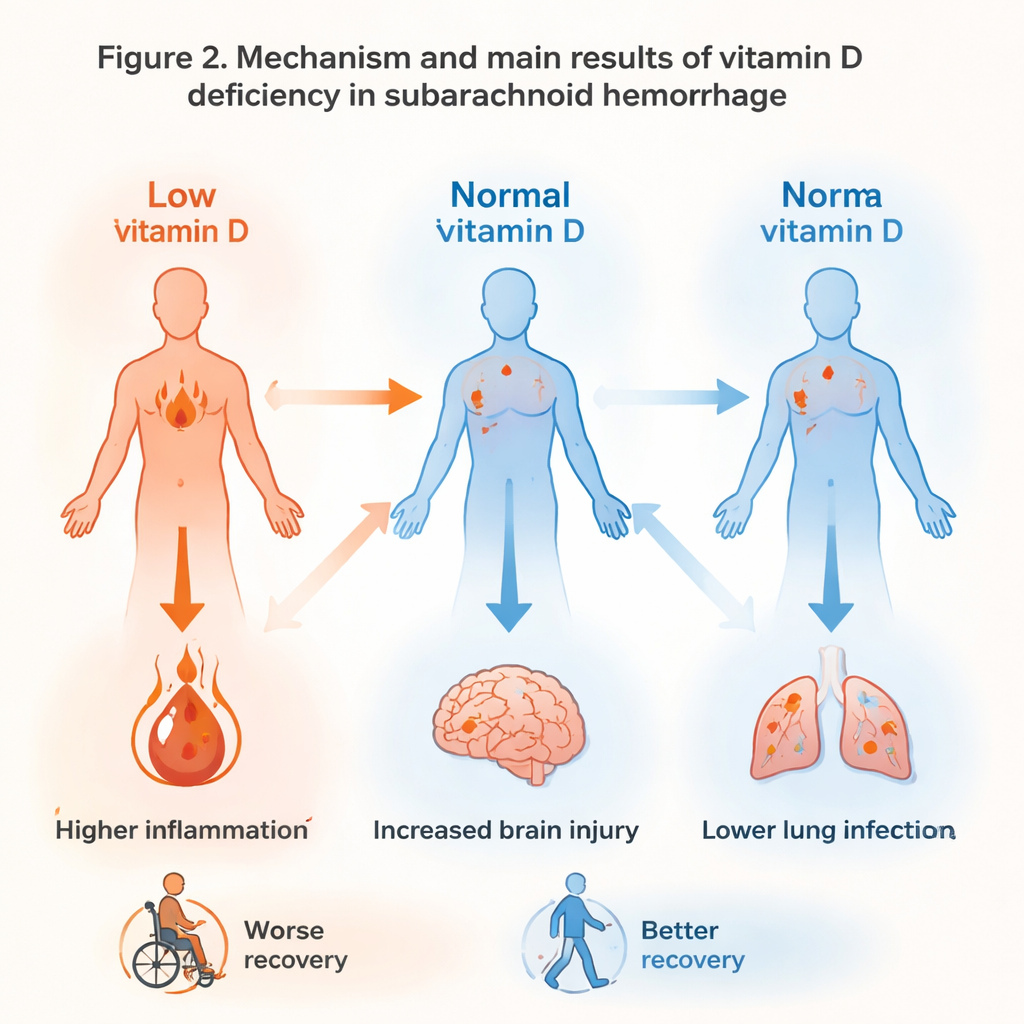
Inflammation, Infections, and the Immune Response
Vitamin D is known to help regulate the immune system, and that pattern appeared here as well. Patients with low vitamin D showed higher peaks of inflammatory markers in their blood, including C-reactive protein and the ratio of neutrophils to lymphocytes, both of which signal a strong and potentially harmful inflammatory response. When the team separated patients into those who developed infections and those who did not, some differences in inflammation narrowed. Yet even among patients without infections, vitamin D–deficient individuals still had higher signs of systemic inflammation. Clinically, infections were common overall, but pneumonia stood out: it occurred far more often in patients with low vitamin D, pointing to a possible weakening of the body’s defenses in the lungs.
How Vitamin D Levels Related to Everyday Function
The impact of vitamin D status ultimately showed up in how well people recovered their daily lives. By three months after the hemorrhage, patients with low vitamin D were substantially more likely to have moderate to severe disability or death, and among survivors they were more likely to remain heavily dependent on others for basic activities. When the researchers accounted for other factors—such as smoking, aneurysm type, new brain lesions, and pneumonia—the direct effect of vitamin D levels on outcome became less clear. This suggests that low vitamin D may worsen prognosis indirectly, by increasing the chances of secondary brain injury and serious lung infections, rather than acting as a simple on–off switch for recovery.
What This Means for Patients and the Public
To a non-specialist, the message is straightforward but important: in this study, patients who arrived at the hospital after a major brain bleed with low vitamin D were more likely to develop further brain damage, suffer pneumonia, mount stronger inflammatory responses, and end up more disabled months later. The research cannot yet prove that low vitamin D causes these problems—levels may drop as part of the body’s reaction to severe illness—but it raises the possibility that maintaining adequate vitamin D, or correcting low levels early, might improve outcomes. Larger, carefully designed trials will be needed to test whether vitamin D supplementation can genuinely protect the brain and lungs after subarachnoid hemorrhage. Until then, the study underscores how a seemingly simple nutrient could play a role in one of neurology’s most serious emergencies.
Citation: Szántó, D., Fülesdi, B., Simon, L. et al. Impact of vitamin D deficiency on clinical outcomes in non-traumatic subarachnoid hemorrhage: A single-center prospective cohort study. Sci Rep 16, 7320 (2026). https://doi.org/10.1038/s41598-026-38728-9
Keywords: vitamin D, brain hemorrhage, subarachnoid hemorrhage, inflammation, stroke recovery