Clear Sky Science · en
PTGDS is a potential marker for lung adenocarcinoma identified in a pancancer analysis
Why a little-known enzyme could matter to cancer patients
Most people have never heard of PTGDS, an enzyme that helps our bodies make hormone-like molecules called prostaglandins. Yet this quiet worker may hold important clues for how cancers grow, how they interact with the immune system, and why some lung tumors behave more aggressively than others. In this study, researchers combed through massive cancer databases and ran lab experiments to see how PTGDS behaves across many tumor types, and whether it could serve as a warning light—or even a brake—on cancer, especially lung adenocarcinoma, the most common form of lung cancer in non-smokers.
Looking across many cancers at once
To understand PTGDS in a broad context, the team performed a so‑called “pan‑cancer” analysis, examining its activity in 33 different cancer types using large public resources such as The Cancer Genome Atlas and other multi‑omics datasets that track RNA, protein, DNA changes, and more. They found that PTGDS levels were abnormally low in most cancers when compared with healthy tissues, both at the gene and protein level. Only a few tumor types, like ovarian and pancreatic cancers, showed higher levels. These patterns suggested that, in many settings, PTGDS might act more like a defender than a driver of cancer. 
Clues from patient survival and tumor DNA
The researchers then asked whether PTGDS levels were linked to how long patients lived or how quickly their disease progressed. In several cancers, including lung adenocarcinoma and some brain tumors, higher PTGDS was associated with better survival, while in certain kidney cancers it tracked with worse outcomes, hinting that its role depends heavily on the tissue and disease context. They also studied how often the PTGDS gene is altered in tumor DNA and how it relates to measures of how genetically unstable a tumor is, such as tumor mutational burden and microsatellite instability. In many cancers, higher PTGDS went hand in hand with fewer mutations and lower “stem‑like” qualities, features that often mark less aggressive disease.
The tumor neighborhood and the immune system
Cancer does not grow in isolation—it interacts constantly with surrounding support cells and immune cells. Using computational tools that infer immune cell presence from gene activity, the team found that PTGDS levels were strongly tied to how many immune and connective tissue cells are found inside tumors. In lung adenocarcinoma and several other cancers, higher PTGDS was linked with more infiltration by key immune players such as T cells, B cells, macrophages, and natural killer cells. Single‑cell datasets, which profile individual cells one by one, showed that PTGDS is particularly active in fibroblasts (structural cells), blood vessel cells, and several immune cell types in normal lung tissue. This supports the idea that PTGDS helps shape the “neighborhood” around the tumor, potentially influencing whether the immune system can recognize and control cancer cells.
Zooming in on lung cancer: mechanics inside the cell
Because the patterns in lung adenocarcinoma were especially striking, the researchers took a closer look at this cancer in the lab. They altered PTGDS levels in two human lung cancer cell lines, A549 and H1975. When they forced cells to make more PTGDS, the cells grew more slowly and formed fewer colonies, indicating reduced tumor‑like behavior. When they reduced PTGDS, the opposite happened: cells multiplied faster. Further tests showed that extra PTGDS shifted how the cells handled fat‑based fuels, ramping up fatty acid breakdown while dampening pathways that support rapid growth. It also disturbed the normal cell‑division cycle, causing cells to pause longer before dividing again. Interestingly, although some death‑related proteins increased, overall cell death did not rise much, suggesting that PTGDS mainly slows growth rather than simply killing cells. 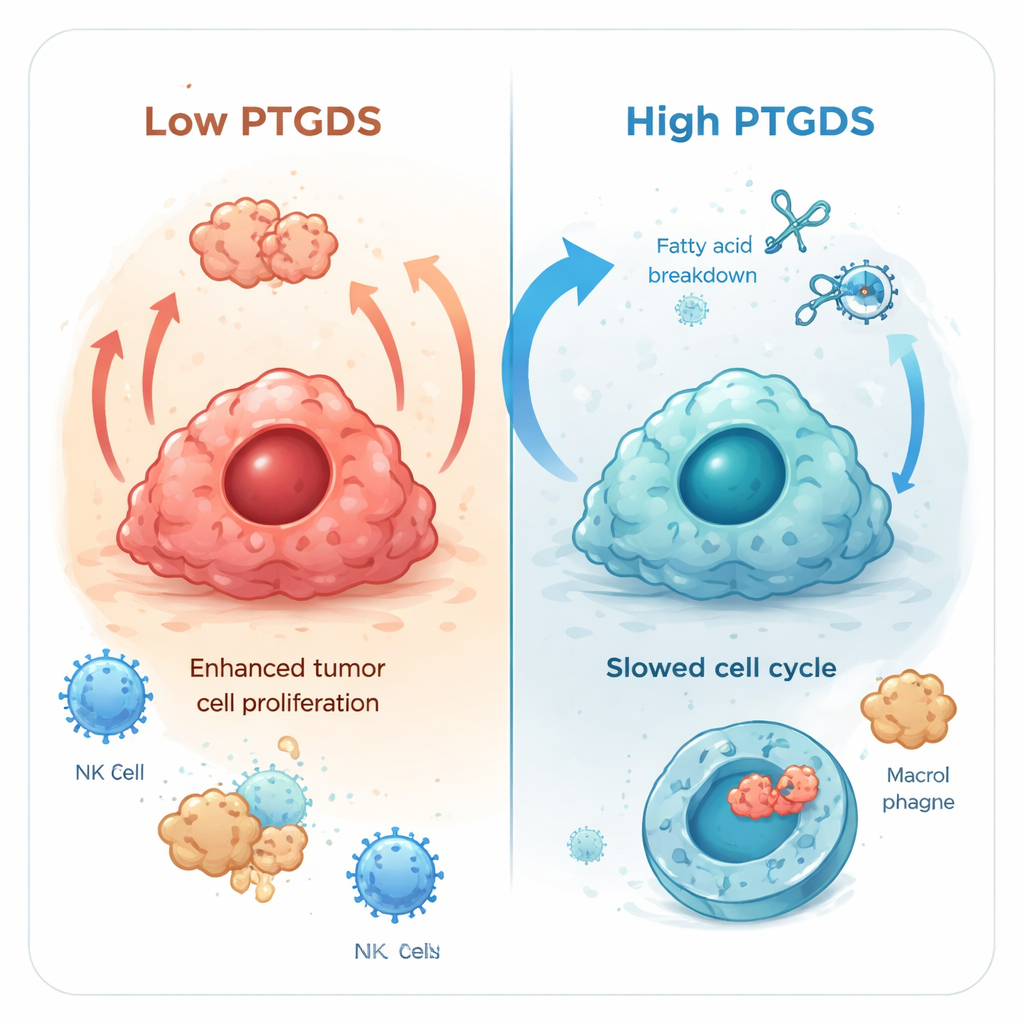
Epigenetic switches and microRNA controls
The study also explored how PTGDS itself is controlled. The team found that certain chemical marks on DNA, known as methylation, were more common in the PTGDS gene region in lung tumors than in normal lung tissue, and several of these marks tracked with how much PTGDS was produced. This suggests that tumors may silence PTGDS through epigenetic switches. In addition, by scanning patterns of small regulatory RNAs called microRNAs, they highlighted one candidate, miR‑3944, that is more abundant in lung tumors and negatively linked to PTGDS levels. Together, these findings point to multiple layers of regulation that tumors might use to dial PTGDS up or down.
What this could mean for future patients
For non‑specialists, the key message is that PTGDS shows a consistent pattern of being turned down in many cancers and, in lung adenocarcinoma in particular, seems to act as a natural brake on tumor growth. Its levels relate not only to how tumors grow and divide, but also to how they interact with the body’s immune defenses and how they use fuel. While more research is needed—including animal studies and clinical tests—PTGDS could eventually help doctors better predict outcomes, refine who might benefit from certain immunotherapies, and perhaps inspire new treatments that restore or mimic its tumor‑restraining effects.
Citation: Wang, R., Shao, F., Liu, D. et al. PTGDS is a potential marker for lung adenocarcinoma identified in a pancancer analysis. Sci Rep 16, 7611 (2026). https://doi.org/10.1038/s41598-026-38688-0
Keywords: lung adenocarcinoma, cancer biomarker, tumor microenvironment, fatty acid metabolism, prostaglandin D2 synthase