Clear Sky Science · en
Impact of venetoclax trough levels on safety and efficacy in the treatment of acute myeloid leukemia
Why drug levels matter for leukemia patients
For many older adults with acute myeloid leukemia, an aggressive blood cancer, powerful chemotherapy is simply too hard on the body. A newer pill called venetoclax, given together with another drug called azacitidine, has become a lifeline for these patients. But like many modern cancer medicines, venetoclax can interact with other drugs and build up in the bloodstream, raising questions that matter deeply to patients and doctors: how much of the drug is enough to fight the cancer, and how much is too much for the body to safely handle?
Balancing hope and harm
This study followed 152 adults in Japan with acute myeloid leukemia who were treated with the venetoclax–azacitidine combination. Most were around 70 years old and either newly diagnosed or facing leukemia that had come back or resisted earlier treatment. The researchers focused on a simple blood measurement called the “trough level” of venetoclax—the lowest concentration of the drug in the blood just before the next dose. Because venetoclax is broken down by a common liver enzyme that also handles many antifungal medicines, the team paid close attention to which antifungal drugs patients were taking and how the venetoclax dose was adjusted. Their goal was to see how these trough levels related to both side effects and cancer control in everyday clinical practice, not just in tightly controlled trials.
Hidden differences in how the body handles the drug
Even when doctors followed national dosing rules and adjusted venetoclax for the type of antifungal medicine used, patients’ blood levels of the drug varied widely—more than a hundredfold from the lowest to the highest. People taking the moderate-strength antifungal fluconazole tended to have slightly higher venetoclax levels than those taking stronger antifungals at a lower venetoclax dose, but there was still a great deal of overlap. Patients whose liver or kidney blood tests were worse—higher bilirubin or creatinine—were more likely to have higher venetoclax levels. This suggests that standard dose charts cannot fully predict how much drug will actually circulate in a given patient, especially when organ function is strained.
When too much medicine hurts the blood
The main safety concern was “hematologic toxicity,” a catch-all term for very low red cells, white cells, or platelets that can cause fatigue, infection, or bleeding. These problems were common, especially during the first treatment cycle: nearly all patients had some degree of blood-cell damage. By comparing venetoclax levels with toxicity, the team found that patients whose trough level stayed below about 1,800 units in the first cycle and below about 1,300 units in the second cycle were less likely to experience the worst blood-cell problems. Everyone whose level climbed into the highest ranges had serious hematologic toxicity. Interestingly, in later cycles the drug levels often crept higher while side effects became less frequent, likely because bone marrow recovered as the leukemia responded, making patients more resilient to the same amount of medicine.
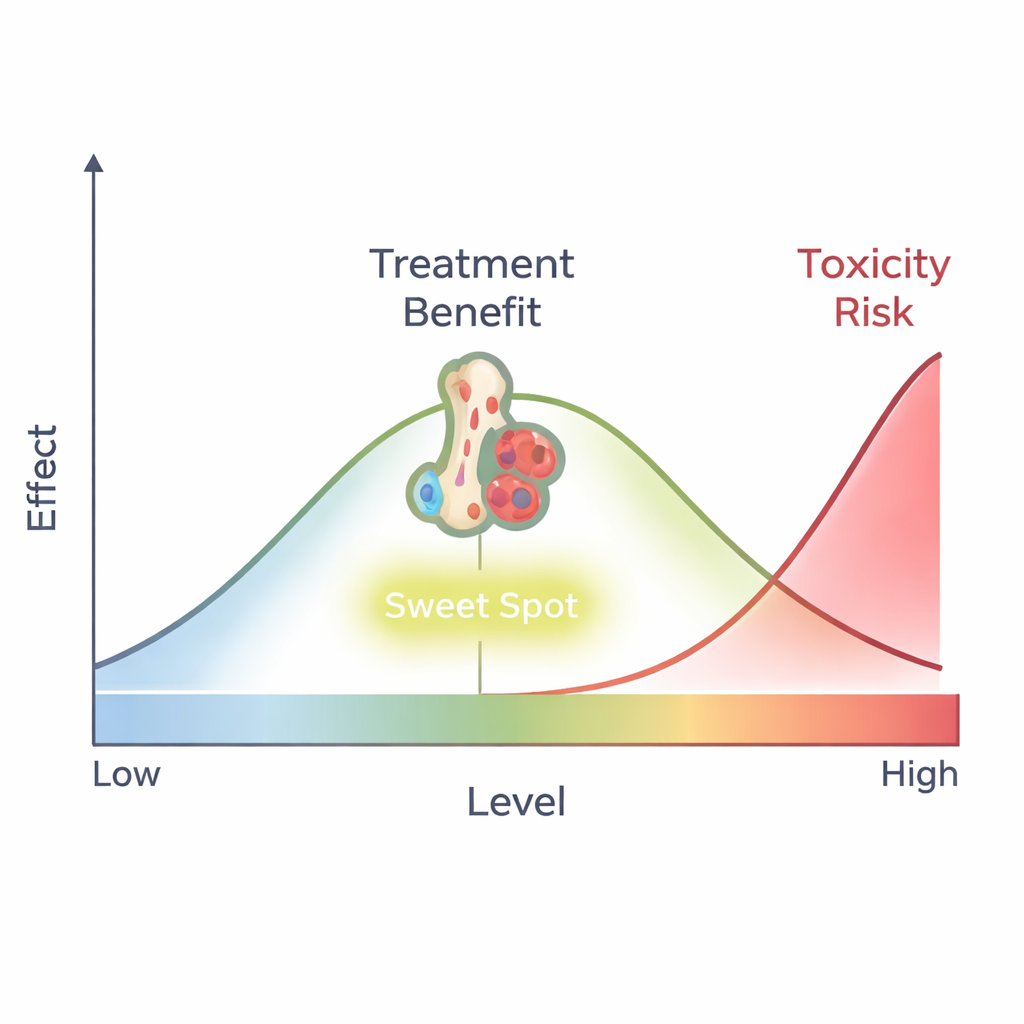
Linking drug levels to treatment success
The researchers also asked whether higher venetoclax levels led to better cancer control. Among all patients who were not in remission at the start, there was no clear threshold where more drug reliably meant better results. But in those receiving venetoclax as their very first leukemia treatment, a pattern appeared: patients whose trough levels rose above about 1,400 units were significantly more likely to reach a deep remission, where leukemia cells were no longer detectable and blood counts began to recover. This suggests that, at least early in treatment and especially for newly diagnosed patients, there may be a “sweet spot” where venetoclax is high enough to strongly attack leukemia cells but not so high that it devastates healthy blood-forming cells.
What this means for patients and doctors
To a layperson, the key message is that the same pill can behave very differently from one person to another, and those differences matter. In this study, measuring venetoclax levels in the blood helped reveal who was at higher risk of severe drops in blood counts and, in some cases, who was more likely to benefit. The authors argue that routinely checking venetoclax trough levels—at least in the first few treatment cycles—could help doctors fine-tune doses for each patient, protecting the bone marrow while still giving the leukemia a strong hit. Larger, prospective studies will be needed before such monitoring becomes standard care, but the work points toward a future in which cancer dosing is guided not just by age and weight, but by real-time measurements of how each body handles the drug.
Citation: Hayashi, H., Yamagiwa, T., Kanda, J. et al. Impact of venetoclax trough levels on safety and efficacy in the treatment of acute myeloid leukemia. Sci Rep 16, 7667 (2026). https://doi.org/10.1038/s41598-026-38587-4
Keywords: acute myeloid leukemia, venetoclax, drug monitoring, chemotherapy side effects, antifungal interactions