Clear Sky Science · en
Validity of spasticity related parameters obtained from manual clinical instrumented assessment in stroke patients
Why this matters for life after stroke
Many people who survive a stroke are left with a stubborn tightness in their muscles that makes walking and standing difficult. Doctors call this spasticity, and today they mostly rely on how a limb “feels” in their hands to judge its severity. This study explores a portable testing setup that adds precise sensors to that familiar bedside exam, with the goal of separating what comes from the nerves from what comes from stiff muscles and joints. If successful, it could help clinicians choose treatments that are better matched to each person’s underlying problem.
Muscle tightness is more than just stiffness
After a stroke, the lower leg often becomes both overactive and stiff. Part of the problem comes from the nervous system: stretch a muscle quickly, and it may fire off an exaggerated reflex, snapping the foot downward. Another part is mechanical: tendons and soft tissues can shorten and harden over time, limiting how far the ankle can bend even when the muscle is quiet. Standard bedside rating scales capture the overall resistance a clinician feels but cannot tell how much is due to reflex overactivity and how much is due to structural tightness. This distinction matters, because nerve-targeting treatments such as botulinum toxin injections are unlikely to fix a joint that is already locked by contracture.
Turning a hands-on exam into a measured test
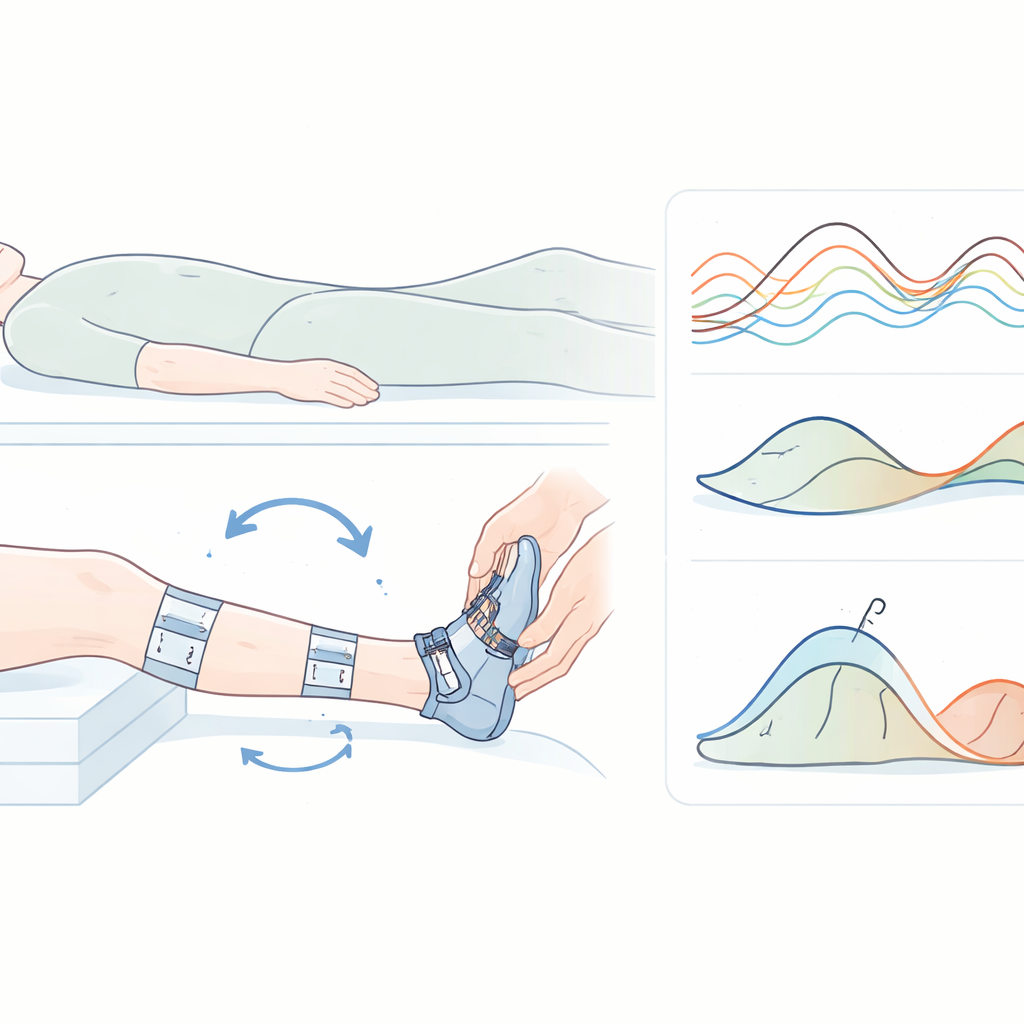
The research team adapted an existing instrumented spasticity assessment, originally developed for children with cerebral palsy, to adults who had experienced a stroke. The setup looks much like a routine ankle exam. The person lies on their back with the knee slightly bent, while lightweight motion sensors are strapped to the thigh, shin, and foot. A slim brace under the foot is connected to a force sensor that records how much twisting force, or torque, builds up at the ankle as it is moved. Small sticky electrodes on the calf muscle record electrical activity, showing when muscle fibers switch on. A trained examiner then repeatedly moves the ankle through its range of motion, first very quickly and then slowly, while the sensors capture both movement and muscle signals.
Comparing affected legs, healthy legs, and speed
The study enrolled 18 adults with a first stroke and ankle spasticity and 27 similar adults without stroke. For each person, the researchers analyzed several carefully selected stretches from both legs, focusing on the calf muscle that points the toes downward. They compared what happened during fast and slow stretches, paying special attention to three things: how much extra muscle activity appeared at higher speed, how strongly that activity changed relative to each person’s best voluntary effort, and how much the measured ankle torque shifted between slow and fast movements. In stroke survivors, the affected leg often had a smaller range of motion and weaker voluntary contractions than the non-affected leg and than healthy volunteers, reflecting both weakness and contracture.
What the sensors revealed about tight muscles
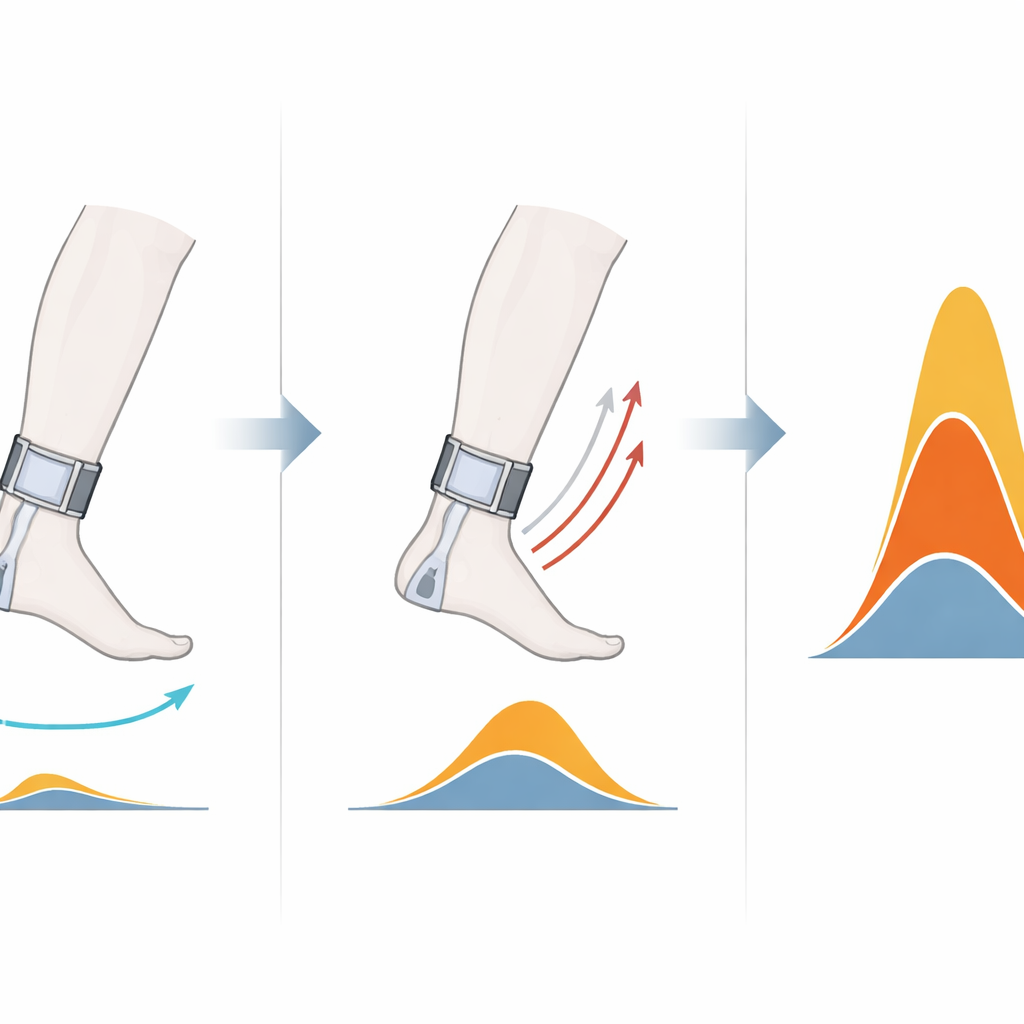
When the ankle was moved quickly, the affected legs showed a clearer spike in muscle activity than healthy legs, consistent with an exaggerated stretch reflex. Expressed as a percentage of each person’s maximum voluntary effort, this reflex-related activity was markedly higher in the affected legs than in their own non-affected legs and than in the legs of healthy volunteers. At the same time, the change in ankle torque between fast and slow stretches was actually smaller in the affected legs. This pattern suggests that, for many participants, mechanical stiffness and contracture were already adding a large, speed-independent resistance, so the reflex contribution made up a smaller share of the total torque. By combining both electrical and mechanical signals, the instrument could tease apart these overlapping contributors to the feeling of “tightness.”
How this could shape future stroke care
The authors conclude that their instrumented ankle test can reliably distinguish the affected leg of stroke patients from their non-affected leg and from healthy legs, based on parameters closely linked to spasticity. For patients, this means that in the future clinicians may be able to quantify how much of their movement limitation is driven by nerve-driven overactivity versus hardened tissues. Such insight could guide decisions about when to use nerve-blocking injections, when to emphasize stretching and splinting, and when to consider surgery or other options. While larger studies are still needed, this work shows that adding smart sensors to a familiar hands-on exam can bring new clarity to one of stroke rehabilitation’s most persistent challenges.
Citation: Schillebeeckx, F., Hanssen, B., De Beukelaer, N. et al. Validity of spasticity related parameters obtained from manual clinical instrumented assessment in stroke patients. Sci Rep 16, 8368 (2026). https://doi.org/10.1038/s41598-026-38551-2
Keywords: stroke rehabilitation, muscle spasticity, ankle movement, electromyography, clinical assessment tools