Clear Sky Science · en
Types and frequency of preanalytical errors occurring in the hematology laboratory at Debre Tabor comprehensive specialized hospital, North Central, Ethiopia, 2025
Why Small Lab Mistakes Matter for Your Health
When you have a blood test, you probably assume the result is either right or wrong because of the machine in the lab. But many problems actually start long before the blood ever reaches the analyzer. This study from Debre Tabor Comprehensive Specialized Hospital in North Central Ethiopia looked closely at the “before the test” steps for routine blood work and found that small human mistakes on forms and during blood collection are common enough to threaten safe, accurate care.
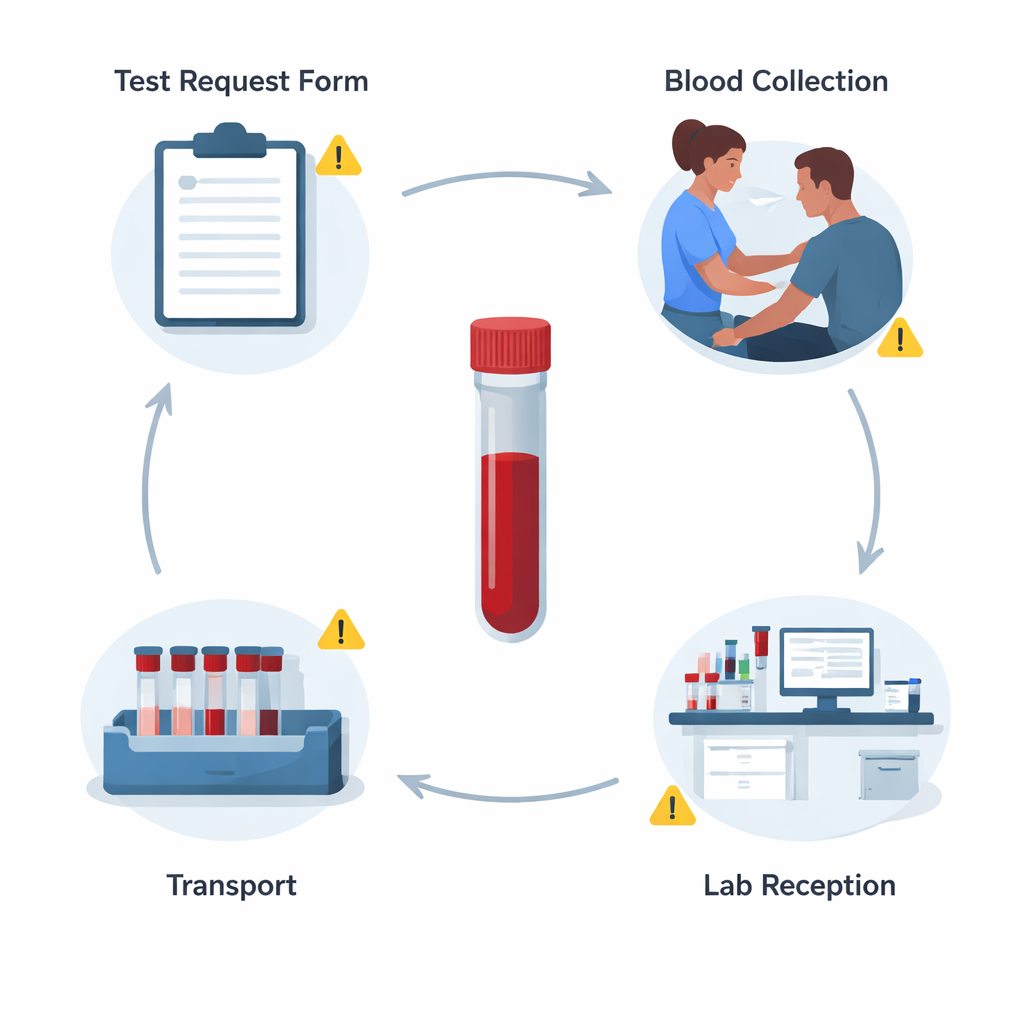
From Doctor’s Pen to Test Tube
Every blood test begins with a doctor filling out a request form and a health worker drawing a sample. The researchers reviewed 2,221 hematology (blood) test requests and their matching samples over two months. About half came from inpatients and half from outpatients. Instead of focusing on rare machine failures, the team examined how often basic details were missing on the forms and how often the samples themselves had obvious problems, such as too little blood or poor labeling. These basic quality checks are the backbone of trustworthy lab medicine but are easy to overlook on a busy ward.
Missing Pieces on the Paperwork
The most striking finding was how often test request forms were incomplete. Only about one in five forms had all the required information. While every form included the patient’s name and the test requested, many left out other crucial details. The patient’s diagnosis was missing in roughly one out of five cases, the date of the request in about one out of twelve, and age in about one out of fourteen. Nearly one in ten forms lacked the clinician’s name, and more than one in ten were missing a signature. Basic timing information was often ignored: the date the sample was taken was absent on more than half of the forms, and the time of collection was missing on nearly half. Altogether, more than 80 percent of forms contained at least one pre-test error.
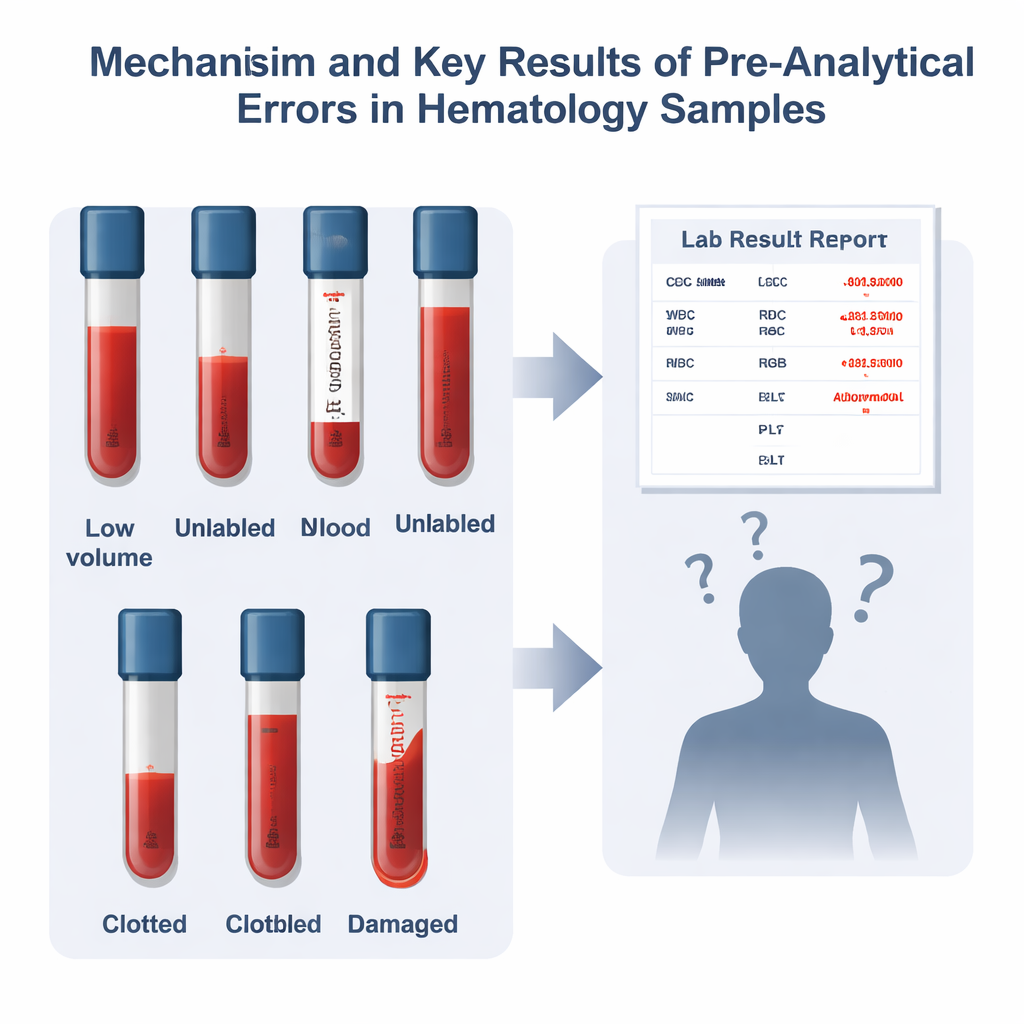
Problems Inside the Blood Tubes
The team also inspected the physical samples. About 5 percent of all blood tubes were judged too poor in quality to be reliable. The most frequent problem was simply not drawing enough blood: around 1.35 percent of samples had an insufficient volume for proper testing. Next came unlabeled tubes, at about 1.22 percent, followed by mislabeled tubes and clotted samples, each around 0.9 percent. A smaller share showed other issues like dilution, damage to red blood cells (hemolysis), or being placed in the wrong type of container. Even though these percentages may seem small, in a hospital that runs thousands of tests, they translate into many patients whose results may be delayed, repeated, or misleading.
Why These Errors Happen
The study points mainly to human factors rather than technology failures. Forms are filled out in busy clinics and wards, sometimes by overworked staff or by people who have not been fully trained in lab requirements. Blood may be drawn by nurses, midwives, physicians, or laboratory workers, each with different levels of familiarity with best practices. High patient loads, limited staff, and the absence of computerized order systems make it easy for details to be skipped or labels to be applied incorrectly. Similar problems have been reported in other hospitals in Ethiopia and abroad, suggesting this is a widespread challenge rather than a single-hospital issue.
Improving the Journey from Vein to Result
The authors argue that preventing these early-stage errors is one of the simplest and most cost-effective ways to improve patient care. They recommend better communication between wards and the laboratory, introducing electronic laboratory information systems to reduce handwriting and manual copying, and giving regular, hands-on training to everyone involved in ordering tests and drawing blood. They also highlight structured quality tools, such as systematic risk analysis and regular staff competency checks, to spot weak points before they harm patients.
What This Means for Patients
For a layperson, the takeaway is clear: the accuracy of your blood test does not depend only on a modern machine; it also depends on ordinary people filling out forms carefully, labeling tubes correctly, and following simple, consistent steps. At Debre Tabor Hospital, most errors happened before the sample ever touched an analyzer, echoing patterns seen worldwide. Tightening up these basic tasks—through better training, clearer systems, and smarter technology—can reduce repeated blood draws, speed up correct diagnoses, and make care safer and more reliable for millions of patients.
Citation: Berhan, A., Sharew, B., Almaw, A. et al. Types and frequency of preanalytical errors occurring in the hematology laboratory at Debre Tabor comprehensive specialized hospital, North Central, Ethiopia, 2025. Sci Rep 16, 7300 (2026). https://doi.org/10.1038/s41598-026-38458-y
Keywords: laboratory errors, blood tests, hematology, patient safety, Ethiopia