Clear Sky Science · en
Comparison of artificial intelligence and multidisciplinary team recommendations in the management of colorectal cancer liver metastases
Why this matters for patients and families
For many people with colorectal cancer, the disease can spread to the liver, turning treatment decisions into a race against time. Today, these choices are usually made by multidisciplinary teams—groups of specialists who meet to agree on the best plan. At the same time, chat-based artificial intelligence tools, such as ChatGPT, are beginning to appear in doctors’ offices as potential helpers. This study asks a simple but important question: when given the same patient summaries, how closely do AI suggestions match what an expert team decides?
How care decisions are usually made
When colorectal cancer reaches the liver, treatment options can range from surgery to chemotherapy to more limited, symptom-focused care. Deciding among these paths is rarely straightforward. Hospitals rely on multidisciplinary team (MDT) meetings that bring together surgeons, medical oncologists, radiologists, and other experts. These discussions weigh tumor size and number, scan findings, overall health, and the chances that surgery can safely remove all visible disease. This team-based model improves survival and helps ensure patients get consistent, evidence-based treatment, but it is also time-consuming and depends on having the right experts available.
What the researchers set out to test
The authors examined whether a chat-based AI system could act as a decision-support partner for these expert teams, not a replacement. They focused on 30 patients with colorectal cancer that had spread to the liver, all previously discussed by an MDT at a single hospital. For each patient, they created a standardized, anonymized text summary including key clinical and scan details, but the AI system had no direct access to images or full medical records. They then asked ChatGPT what the most appropriate treatment would be, repeating the question three times per case to see if the answers were stable. In a second round, they added one crucial piece of information: they explicitly stated that the liver tumors were potentially removable by surgery and asked whether that should change the plan.
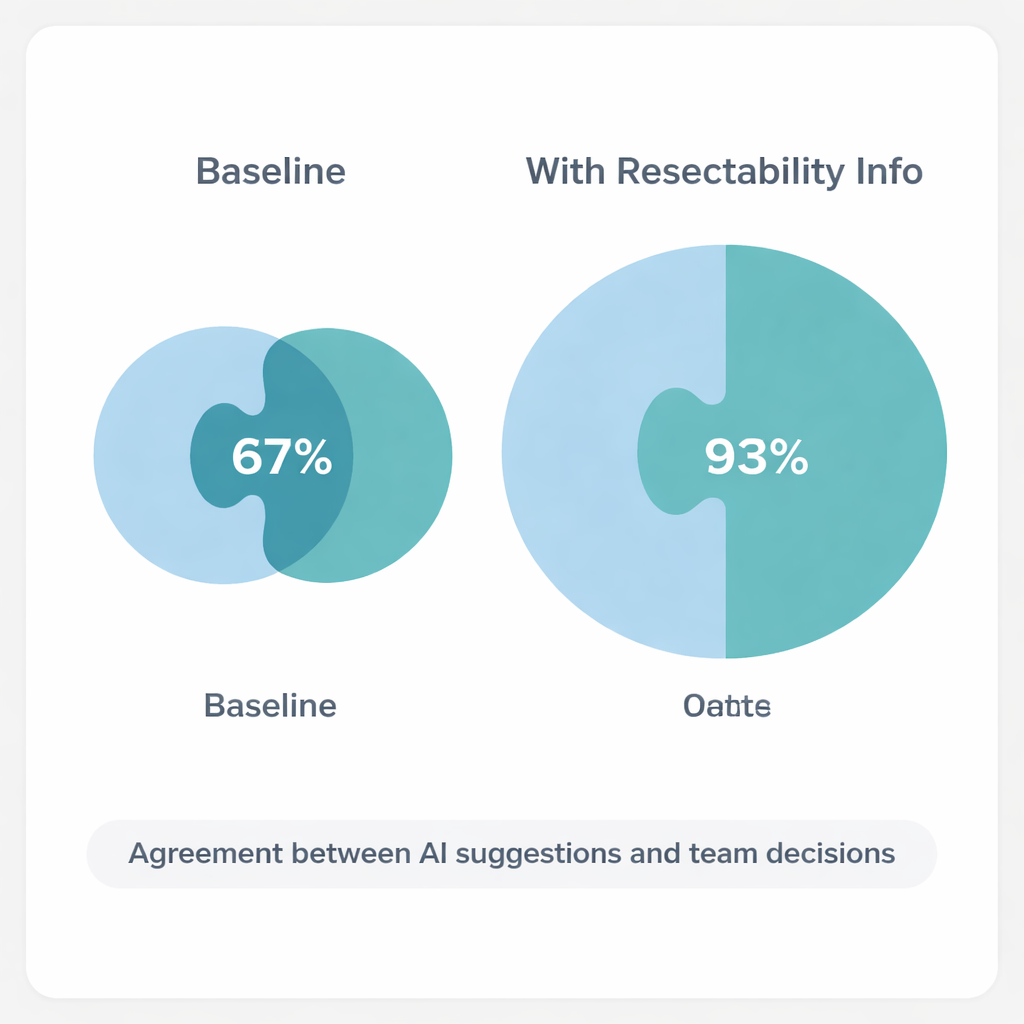
How well the AI agreed with the expert team
The AI gave the same type of recommendation every time it was asked about a given case, showing very high internal consistency. When working only from the basic summaries, its final recommendation matched the MDT’s unanimous decision in about two-thirds of patients (20 out of 30). Most disagreements came from the AI favoring more cautious steps—such as suggesting chemotherapy first, more imaging, or biopsies—while the expert team chose to proceed directly to surgery in carefully selected cases. When the researchers repeated the exercise but clearly stated that the liver metastases appeared operable, agreement rose sharply. In this “resectability-specified” setting, the AI and the MDT matched in 28 of 30 cases, or 93%, a level the authors describe as very good agreement.
What the patterns of disagreement reveal
Even after the extra information was provided, there were still two patients for whom the AI recommended continued systemic treatment instead of surgery, while the MDT opted for an operation aimed at long-term control. Across the study, the AI tended to lean toward conservative choices when there was any hint of uncertainty, likely reflecting both safety-focused training and the limits of working from short text summaries alone. The authors and prior research note that such systems can behave differently across hospitals, cancer types, and software versions, which means performance numbers from one setting cannot be assumed to hold everywhere. They also stress that important human factors—like a patient’s preferences, values, and day-to-day quality of life—are not easily captured in text or guidelines and remain the domain of face-to-face clinical judgment.
What this could mean for future cancer care
This small pilot study suggests that, when given clear and complete written information, a chat-based AI can often reach similar treatment suggestions to those of an experienced cancer team for colorectal cancer that has spread to the liver. However, matching expert decisions on paper is not the same as proving that AI-guided care is safe or improves outcomes. The authors emphasize that these systems should be viewed, at best, as supervised assistants—useful for structuring case summaries or highlighting missing details—rather than autonomous decision-makers. Larger, prospective studies that track real patient outcomes, not just agreement rates, will be essential before such tools can be trusted as part of routine care.
Citation: Yılmaz, M., Abbaslı, N., Tuna, S. et al. Comparison of artificial intelligence and multidisciplinary team recommendations in the management of colorectal cancer liver metastases. Sci Rep 16, 7278 (2026). https://doi.org/10.1038/s41598-026-38449-z
Keywords: colorectal cancer, liver metastases, multidisciplinary teams, clinical decision support, artificial intelligence in oncology