Clear Sky Science · en
Risk of irritable bowel syndrome in patients with hidradenitis suppurativa: a global-federated, multicenter cohort study
When Skin Trouble Connects to Gut Trouble
Many people think of rashes and stomach pain as completely separate problems. This study suggests they may sometimes be linked. It looks at a painful, long-lasting skin condition called hidradenitis suppurativa (HS) and asks whether people who have it are more likely to later develop irritable bowel syndrome (IBS), a common cause of ongoing belly pain and bowel changes. Understanding this link could help patients and doctors catch gut problems earlier and treat the whole person, not just one organ at a time.
A Painful Skin Disease with Hidden Reach
HS causes recurring lumps, abscesses, and draining tunnels in areas such as the armpits and groin. These flare-ups are not only physically painful; they also affect mood, work, and relationships. Over the past decade, researchers have realized that HS is more than a localized skin problem. The same overactive immune system that inflames hair follicles and sweat glands in the skin may also disturb other organs, contributing to conditions like joint disease, metabolic problems, and now possibly gut disorders.
What Is Irritable Bowel Syndrome?
IBS is one of the most common digestive complaints worldwide. People with IBS live with repeated bouts of abdominal pain, bloating, and diarrhea, constipation, or both, even though standard tests often show no obvious damage to the intestines. Scientists think IBS arises from a mix of factors: low-level inflammation, changes in the community of microbes living in the gut, a leakier gut lining that lets irritants cross into the body, and a sensitive “brain–gut” communication system that amplifies pain signals.
Tracking Millions of Medical Records
To explore whether HS raises the chance of developing IBS, the researchers used a huge electronic health record network in the United States that includes about 100 million patients. They identified over 119,000 adults with HS seen between 2005 and 2023 and matched each of them to a similar person without HS. The matching accounted for age, sex, race, body weight, mental health diagnoses, and other medical conditions, making the two groups as alike as possible except for the presence of HS. Anyone who already had IBS or cancer was excluded, and the team then followed people for up to 15 years to see who was later diagnosed with IBS.
Higher Gut Risk in People with HS
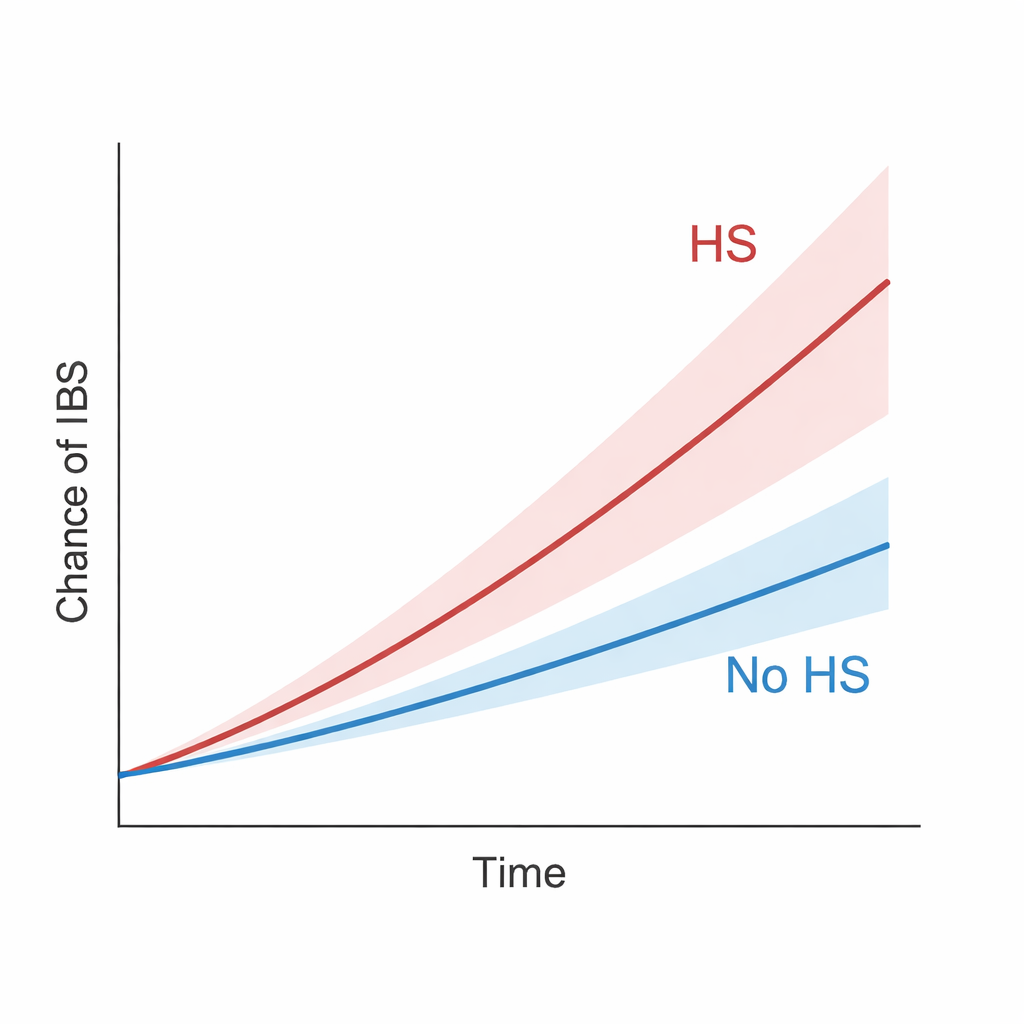
Across this long follow-up, people with HS were more likely to develop IBS than their matched counterparts without HS. Overall, HS was linked to about a 42 percent higher risk of IBS. The difference between groups grew steadily over time, suggesting this was not just a short-term blip. The pattern held up even when the researchers applied stricter rules, such as ignoring IBS cases that appeared in the first one to three years after HS diagnosis, or redefining HS to capture only the most clearly documented or severe cases. In fact, people with HS severe enough to require hospital stays or surgical procedures had especially high IBS risk. When HS patients were compared to people with psoriasis—another long-lasting inflammatory skin disease already tied to IBS—the HS group still had a higher chance of IBS, implying a unique added risk.
Who Seems Most Affected?
The increased risk of IBS showed up in both men and women with HS, and in both younger and older adults. However, it appeared particularly strong in people aged 65 and older, who had more than double the risk of IBS compared with older adults without HS. The authors argue that shared biological pathways may help explain this connection: disturbed skin and gut microbes, a chronically “on” immune system, and a weakened barrier in both skin and intestine that lets irritants slip through. Emotional stress, pain, and repeated antibiotic use—common in HS care—may also contribute by influencing gut bacteria and the brain–gut–skin axis.
What This Means for Patients
For someone living with HS, the study’s message is not that IBS is inevitable, but that it is more likely and worth watching for. Doctors caring for HS patients might consider asking about long-lasting abdominal pain, bloating, or sudden changes in bowel habits and referring patients for evaluation sooner rather than later. Earlier recognition of IBS can lead to better symptom control through diet, medications, and stress management. More broadly, these results add to a growing view of HS as a whole-body condition, encouraging future research into how the skin, gut, immune system, and mind interact—and how treating one part of that network might improve the others.
Citation: Chang, HC., Hsu, YH., Chen, SJ. et al. Risk of irritable bowel syndrome in patients with hidradenitis suppurativa: a global-federated, multicenter cohort study. Sci Rep 16, 7157 (2026). https://doi.org/10.1038/s41598-026-38442-6
Keywords: hidradenitis suppurativa, irritable bowel syndrome, gut-skin axis, chronic inflammation, comorbidities