Clear Sky Science · en
An ensemble machine learning classifier for Parkinson’s disease diagnosis using optical coherence tomography angiography
Why the Eyes May Reveal Hidden Brain Disease
Parkinson’s disease is usually diagnosed only after tremors, stiffness, or slowed movement appear—signs that the brain has already been changing for years. This study explores an unexpected shortcut: looking at tiny blood vessels in the back of the eye with a painless imaging scan and then using artificial intelligence to flag people who may have Parkinson’s earlier and more objectively than today’s checkups allow.
Looking at the Brain Through the Eye
The light-sensitive tissue at the back of the eye, the retina, is essentially an accessible part of the brain. It shares similar nerves and blood vessels but can be examined non-invasively in a clinic. The researchers used a technology called optical coherence tomography angiography, or OCTA, which produces detailed, dye-free maps of the retinal circulation. Because Parkinson’s has been linked to problems in small blood vessels elsewhere in the body, the team asked whether subtle changes in these retinal networks could act as a “window” into early disease.
Turning Eye Scans Into Numbers
In a retrospective study, the team collected OCTA scans from 53 people with Parkinson’s and 39 healthy, age-matched volunteers. They focused on two layers of retinal vessels: a superficial layer near the surface and a deeper layer underneath. From each layer they automatically segmented the central foveal avascular zone—the tiny blood-vessel–free pit needed for sharp vision—as well as the surrounding capillaries. They then converted each image into 22 numerical measurements. Some described the shape of the foveal zone, such as how round, smooth, or irregular its edge was. Others captured how dense the blood vessels were overall and in a ring around the fovea. Together, these measurements quantified microvascular health with far more nuance than a human eye could judge. 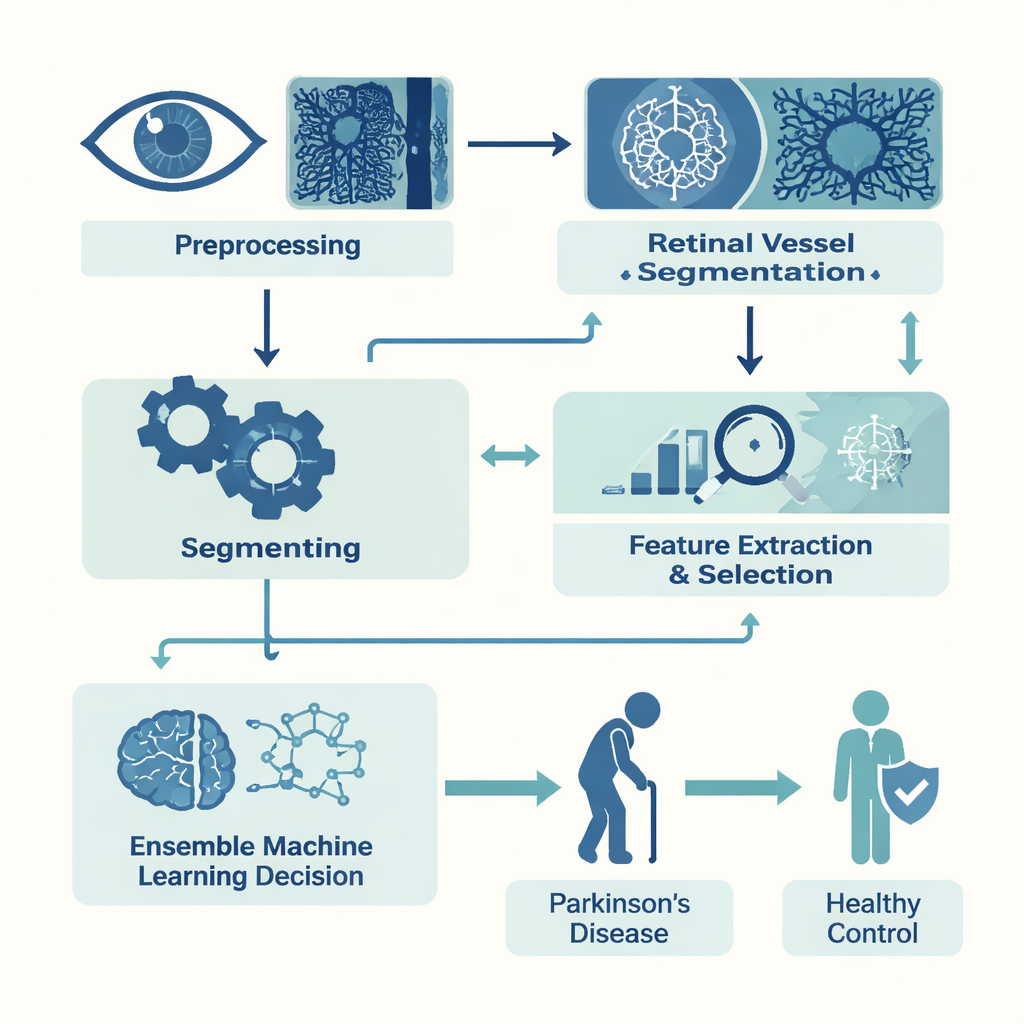
Training an AI to Spot Parkinson’s Patterns
With these measurements in hand, the researchers built computer models to tell Parkinson’s scans from healthy ones. Because their dataset was modest, they first used feature-selection techniques to pare down the 22 measurements to the most informative subset, reducing noise and overfitting. They then trained several common machine-learning algorithms, including decision-tree–based methods and a k-nearest neighbors classifier. Finally, they combined the three strongest performers—XGBoost, Random Forest, and K-Nearest Neighbors—into a weighted “ensemble,” so that each model’s vote counted in proportion to how well it tended to perform.
What the Models Found in the Retina
Compared with healthy volunteers, people with Parkinson’s showed clear signs of altered retinal microcirculation. Measures of vessel density were lower, and the central foveal zone tended to be less regular in shape—less round, less smooth, and less solid—across both superficial and deep vessel layers. When tested on previously unseen data, the ensemble model correctly classified about three out of four eyes overall. Most notably, it reached 90% sensitivity: it correctly identified nine in ten Parkinson’s cases. Specificity was more modest, just over half, meaning some healthy individuals were incorrectly flagged as having disease. The area under the receiver operating characteristic curve, a common summary of diagnostic performance, was 0.75, indicating useful but not definitive discrimination. 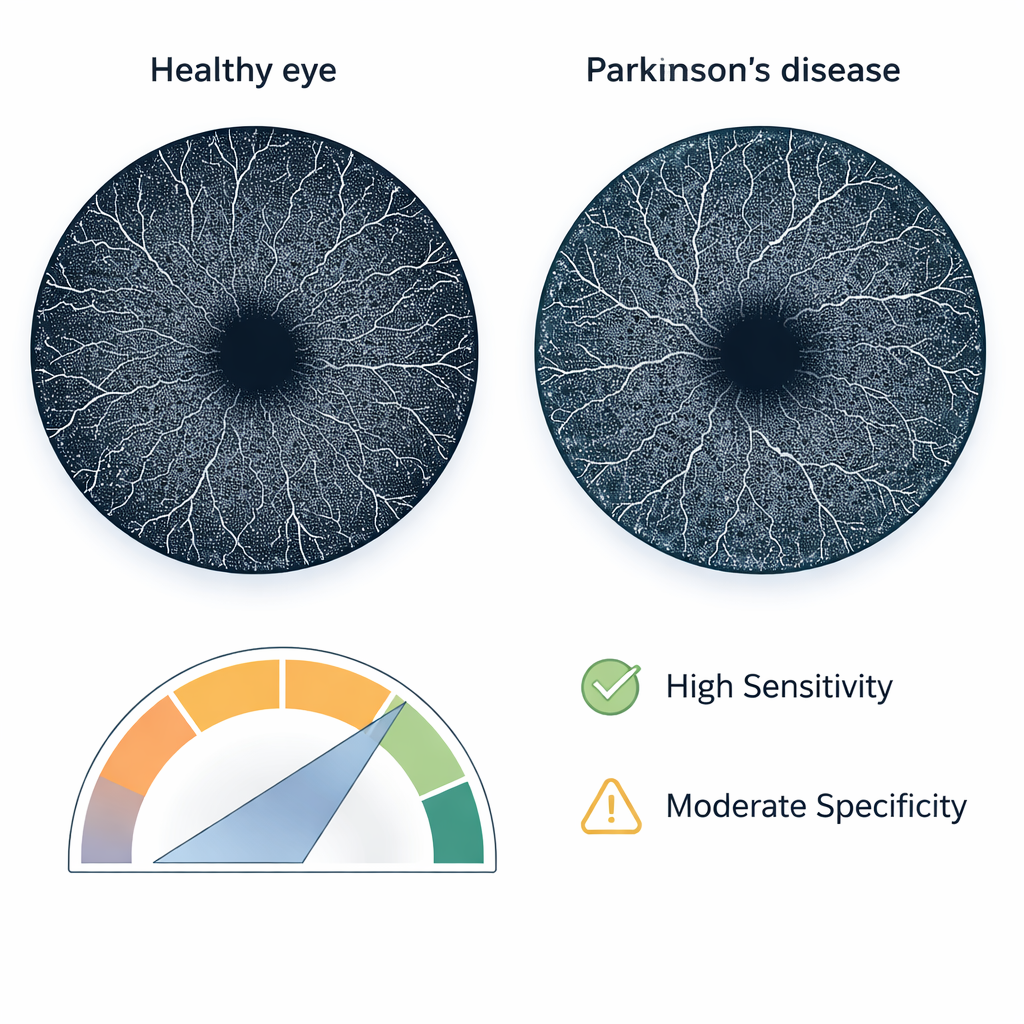
From Algorithm to Clinic
To move beyond theory, the team wrapped their methods into a prototype software tool called Parkinson’s Disease Artificial Intelligence (PDAI). Through a simple graphical interface, clinicians can load OCTA scans, review the automatically traced blood vessels and central foveal zone, see the key numerical features, and obtain an instant prediction of whether a scan resembles those from Parkinson’s patients. Because the system relies on handcrafted, clearly defined measurements rather than an opaque “black box,” the contributors to each decision are easier for clinicians to interpret and potentially relate to underlying biology.
What This Means for Patients
This work does not yet offer a stand-alone test for Parkinson’s, but it shows that a quick, non-invasive eye scan, analyzed with carefully designed machine-learning methods, can pick up disease-related changes with high sensitivity. In practice, such a tool could one day be used as a screening aid—helping eye doctors and neurologists decide who should be monitored more closely or referred for further evaluation long before disabling symptoms appear. Larger, multi-center studies are still needed, but the study suggests that the eyes may indeed provide a practical early warning signal for Parkinson’s disease.
Citation: Hasanshahi, M., Mehdizadeh, A., Mahmoudi, T. et al. An ensemble machine learning classifier for Parkinson’s disease diagnosis using optical coherence tomography angiography. Sci Rep 16, 7297 (2026). https://doi.org/10.1038/s41598-026-38407-9
Keywords: Parkinson’s disease, retinal imaging, OCTA, machine learning, early diagnosis