Clear Sky Science · en
Meta regression of endoscopic sleeve gastroplasty versus intragastric balloon investigating influence of duration and baseline body mass index
Two New Ways to Rethink Weight-Loss Procedures
As obesity rates soar worldwide, many people are searching for options that fall between diet-and-exercise programs and major surgery. Two endoscopic procedures—endoscopic sleeve gastroplasty (ESG) and the intragastric balloon (IGB)—promise meaningful weight loss without cutting into the abdomen. This study pools data from more than 5,000 patients to ask a practical question that matters to patients and doctors alike: which option works better, for how long, and for whom?
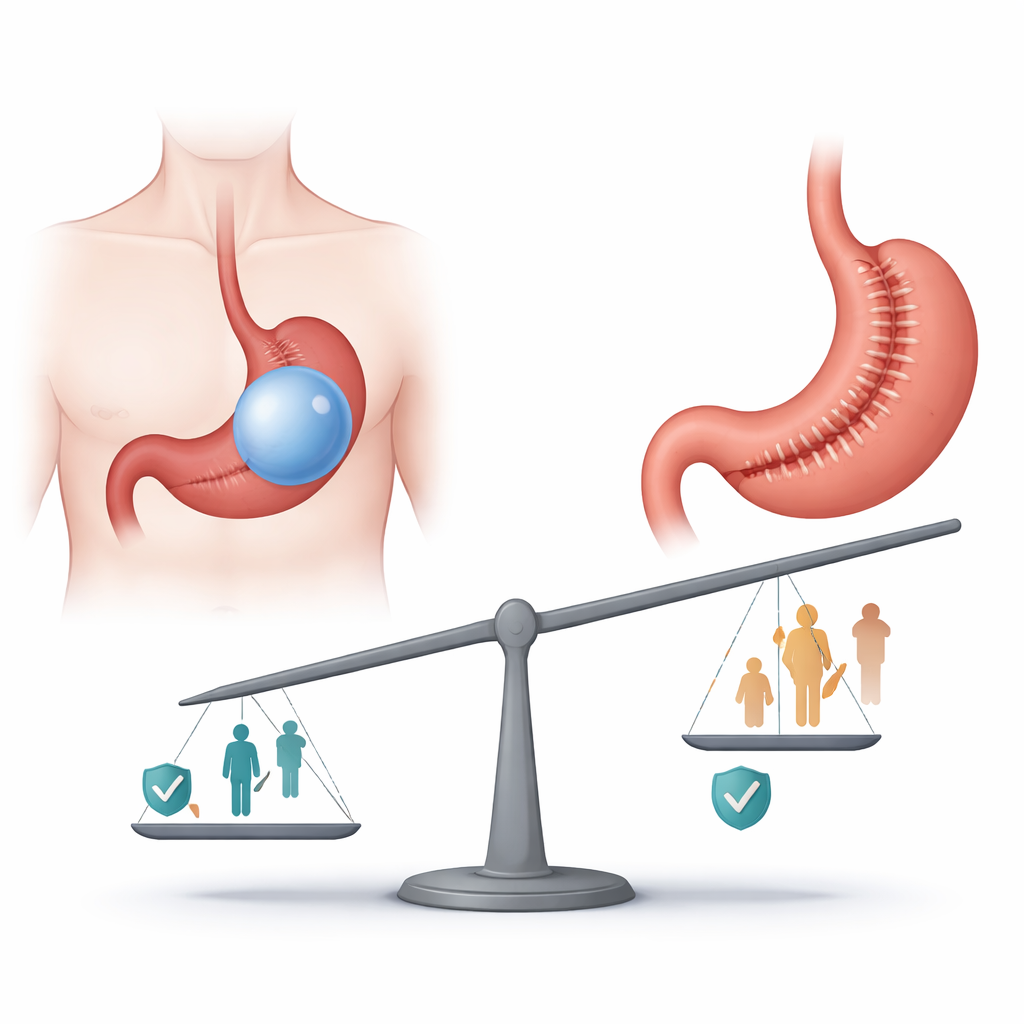
How These Procedures Help People Eat Less
Both ESG and IGB are performed through a flexible tube passed down the throat, avoiding external incisions. The intragastric balloon is a temporary, fluid-filled device placed inside the stomach to take up space and make a person feel full sooner. It is usually removed after about six months, and many patients regain some of the lost weight soon afterward. ESG, by contrast, uses an internal suturing system to fold and tighten the stomach, permanently reducing its volume while keeping the basic anatomy intact. In everyday terms, one method temporarily crowds the stomach, while the other subtly reshapes it.
What the Combined Studies Reveal About Weight Loss
The authors searched multiple medical databases and found six comparative cohort studies, together following 5,330 adults with obesity who received either ESG or an intragastric balloon. They focused on total body weight loss as a percentage of a person’s starting weight and tracked results up to one year. Overall, ESG led to a modest but meaningful extra weight loss of about 2.5 percentage points compared with the balloon. For example, someone starting at 120 kilograms might lose roughly three additional kilograms with ESG versus IGB, on average.
Why Time and Starting Weight Matter
When the researchers looked more closely at timing, an important pattern emerged. In the first few months, the two treatments performed similarly; at three months, the difference between them was not statistically clear. After that point, however, the ESG advantage grew. At six months and again at twelve months, ESG patients maintained noticeably greater weight loss than those who had received a balloon. A separate analysis showed that people who began with higher body mass index (BMI)—that is, more severe obesity—tended to benefit more from ESG than from IGB. In other words, ESG’s edge becomes clearer both as time passes and as starting weight increases.
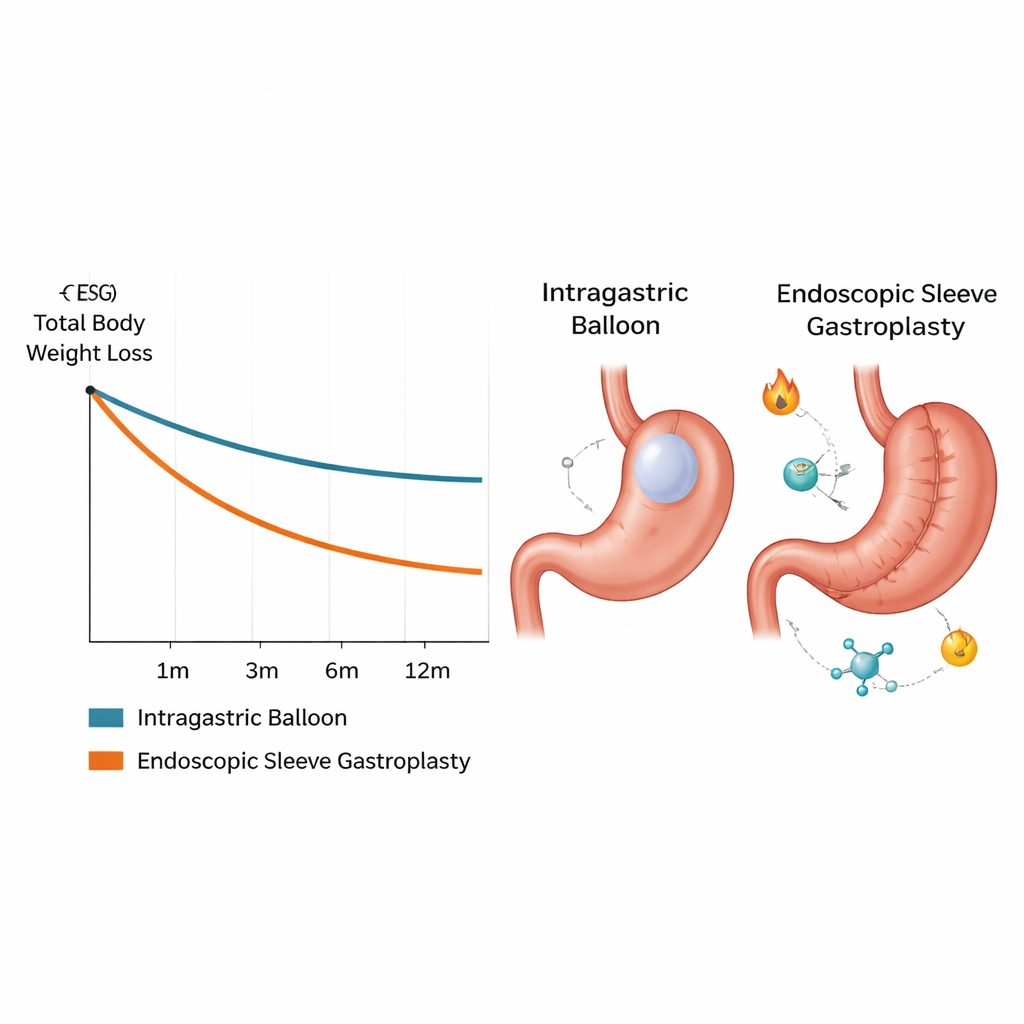
Safety, Side Effects, and Daily Life
Safety is a central concern for anyone considering an endoscopic weight-loss procedure. Across the studies that reported complications, overall risk was similar between ESG and intragastric balloons. However, balloons were more often linked to trouble tolerating the device, including nausea, vomiting, and discomfort that sometimes forced early removal. ESG, while technically more complex to perform and more expensive up front, showed low rates of serious problems and appeared easier for many patients to live with over time. Both approaches worked best when combined with ongoing nutrition and behavioral counseling, underscoring that procedures alone are not a cure.
What This Means for People Living With Obesity
Put simply, this research suggests that ESG may offer more durable weight loss than a gastric balloon, especially for individuals with more severe obesity and for those looking at results beyond the three-month mark. The balloon can still be a useful option for people in lower BMI ranges or those seeking a simpler, short-term tool, but its benefits tend to fade after removal. ESG reshapes the stomach in a way that appears to support longer-lasting changes in eating patterns and metabolism, without adding major safety concerns. Longer studies are still needed, but for many patients who want a non-surgical yet durable approach, ESG may represent the stronger long-term choice.
Citation: Huang, PF., Chen, HW., Huang, TY. et al. Meta regression of endoscopic sleeve gastroplasty versus intragastric balloon investigating influence of duration and baseline body mass index. Sci Rep 16, 7280 (2026). https://doi.org/10.1038/s41598-026-38374-1
Keywords: endoscopic weight loss, endoscopic sleeve gastroplasty, intragastric balloon, obesity treatment, bariatric endoscopy