Clear Sky Science · en
Human bone marrow derived mesenchymal stem cells do not promote oral cancer cell growth in vitro and metastasis in vivo
Why this matters for cancer patients
When surgeons remove oral cancers, they often must take parts of the jawbone with the tumor. Rebuilding that bone is difficult, and one promising option is to use a person’s own stem cells from their bone marrow to help the bone regrow. But a key worry remains: could these helpful stem cells accidentally feed any hidden cancer cells and make the disease worse? This study directly tackles that concern for oral cancer, asking whether bone marrow stem cells used in reconstruction might actually fuel tumor growth or spread.
Healing cells with a double edge
Bone marrow–derived mesenchymal stem cells are a type of “repair cell” that can turn into bone, cartilage, and fat cells, and also send out chemical signals that calm inflammation and encourage healing. Because of this, they are being explored as living tools to repair large jawbone defects after oral cancer surgery. At the same time, these cells can travel to injured or diseased tissues, including tumors. Earlier work in other cancers has painted a confusing picture: in some settings, these stem cells seem to slow tumors; in others, they appear to help them grow and invade. Before such cells can be widely used to rebuild jaws in people treated for oral cancer, researchers need clear safety data focused on this specific disease.
Putting stem cells and cancer cells in the same dish
The researchers first tested what happens when oral cancer cells are exposed to the cocktail of molecules that stem cells release. They grew human bone marrow stem cells from several donors in the lab, collected the liquid they had been bathing in (called conditioned medium), and added it to two different oral cancer cell lines. They checked whether this changed how fast the cancer cells multiplied, moved, or invaded a three-dimensional gel that mimics tissue. The conditioned medium did not make the cancer cells divide more or burrow deeper into the gel. Surprisingly, in a scratch “wound” test on flat plates, the cancer cells actually crawled more slowly when exposed to stem cell–conditioned liquid, suggesting that the secreted factors from these repair cells may dampen, rather than spur, cancer cell movement in this setting.
Following the path of stem cells inside the body
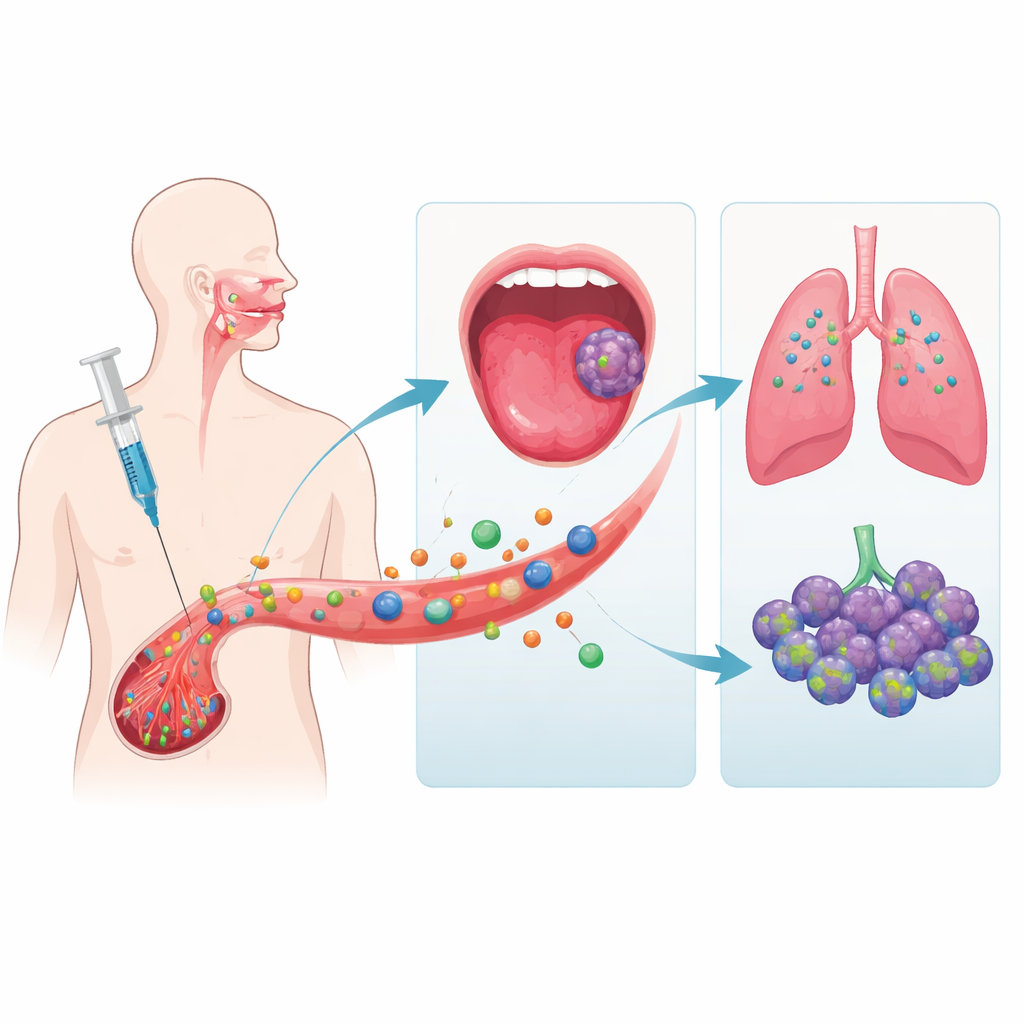
To see what happens inside a living organism, the team turned to mice that had human tongue tumors grafted onto their tongues. They engineered the bone marrow stem cells to glow so that they could be tracked with a sensitive camera. After injecting these cells into the animals’ bloodstream, the researchers watched where the glowing cells went over several weeks and examined tissues under the microscope and by genetic tests. Almost all of the stem cells became trapped in the lungs soon after injection and gradually disappeared over time. Crucially, there was no detectable clustering of stem cells in the tongue tumors or surrounding tissues, and no stem cells were found in other organs such as the liver, spleen, or kidneys.
Did stem cells change tumor growth or spread?
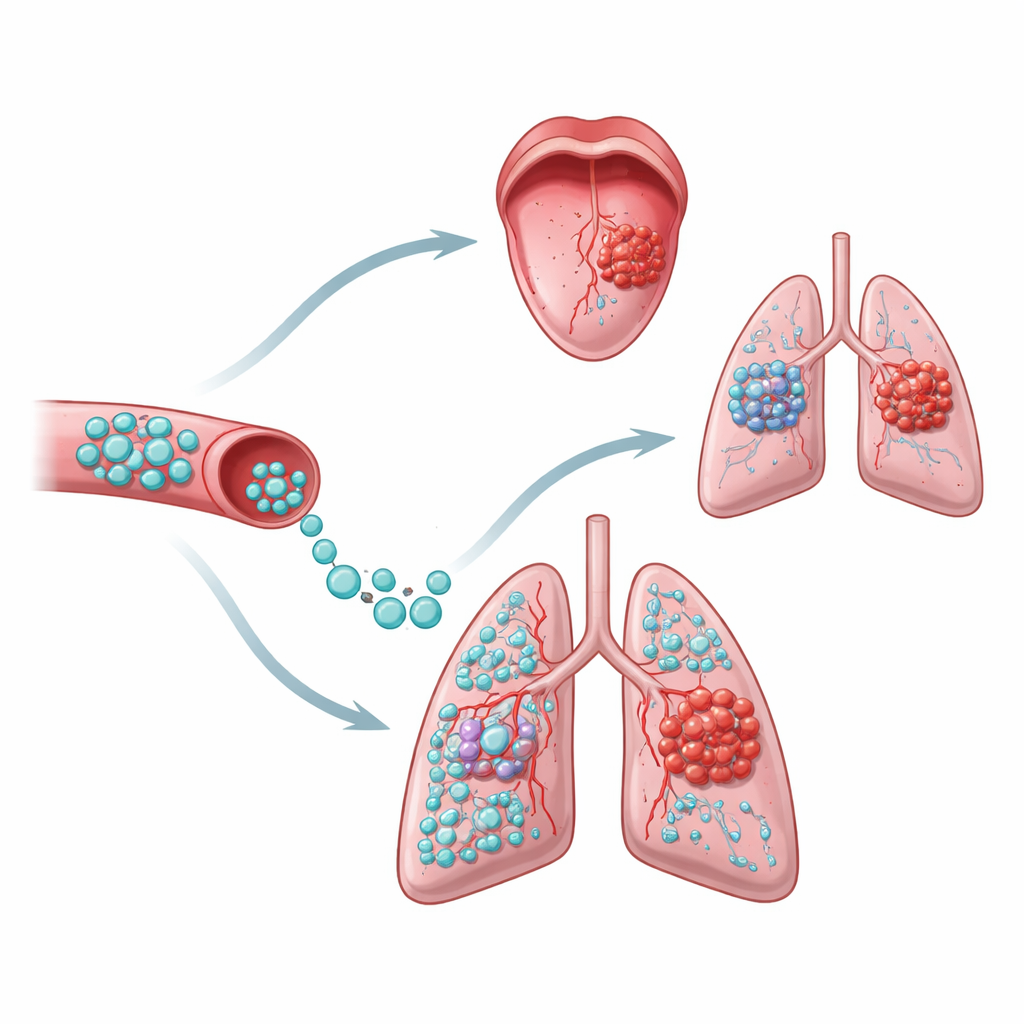
Next, the team asked whether having stem cells circulating in the blood changed how the tongue tumors behaved. They measured tumor size in mice that had tumors alone and in those that also received stem cell injections. Tumor growth over time was nearly identical in both groups, and the animals’ body weights remained similar, arguing against any major harmful effect. Because injected cells often lodge in the lungs, the researchers carefully examined lung tissue for cancer deposits. Both groups of mice developed lung metastases, as expected in this aggressive model, but the presence of stem cells did not increase how many cancer cells were found there. If anything, there was a slight, non-significant trend toward fewer cancer cells in the lungs of stem cell–treated animals.
What this means for future jaw reconstruction
Taken together, the study suggests that, under the tested conditions, bone marrow–derived mesenchymal stem cells do not make oral cancer cells grow faster, invade more deeply, or spread more widely. In laboratory dishes, the liquid they release actually slowed cancer cell movement, and in mice most of the injected cells were short-lived and confined to the lungs without homing to the tongue tumors. While more research is needed to explore different doses, delivery routes, and longer time frames, these findings provide an encouraging safety signal: using a patient’s own bone marrow stem cells to help rebuild jawbone after oral cancer surgery may not, by itself, worsen the cancer.
Citation: Siyam, D., Parajuli, H., El herch, I. et al. Human bone marrow derived mesenchymal stem cells do not promote oral cancer cell growth in vitro and metastasis in vivo. Sci Rep 16, 8072 (2026). https://doi.org/10.1038/s41598-026-38370-5
Keywords: oral cancer, bone marrow stem cells, jaw reconstruction, cancer metastasis, regenerative medicine