Clear Sky Science · en
Distinct gut microbiome signatures associated with sedentary behavior improvement following rehabilitation in chronic obstructive pulmonary disease patients with higher functional exercise capacity
Why sitting less matters for lung disease
Chronic obstructive pulmonary disease (COPD) makes breathing hard and often drains people of the energy they need to move. Many patients spend long hours sitting, which is linked to worse health and a shorter life. This study asked a timely question: when people with COPD follow a simple home rehab program, who actually manages to sit less—and could tiny organisms in the gut help explain the difference?
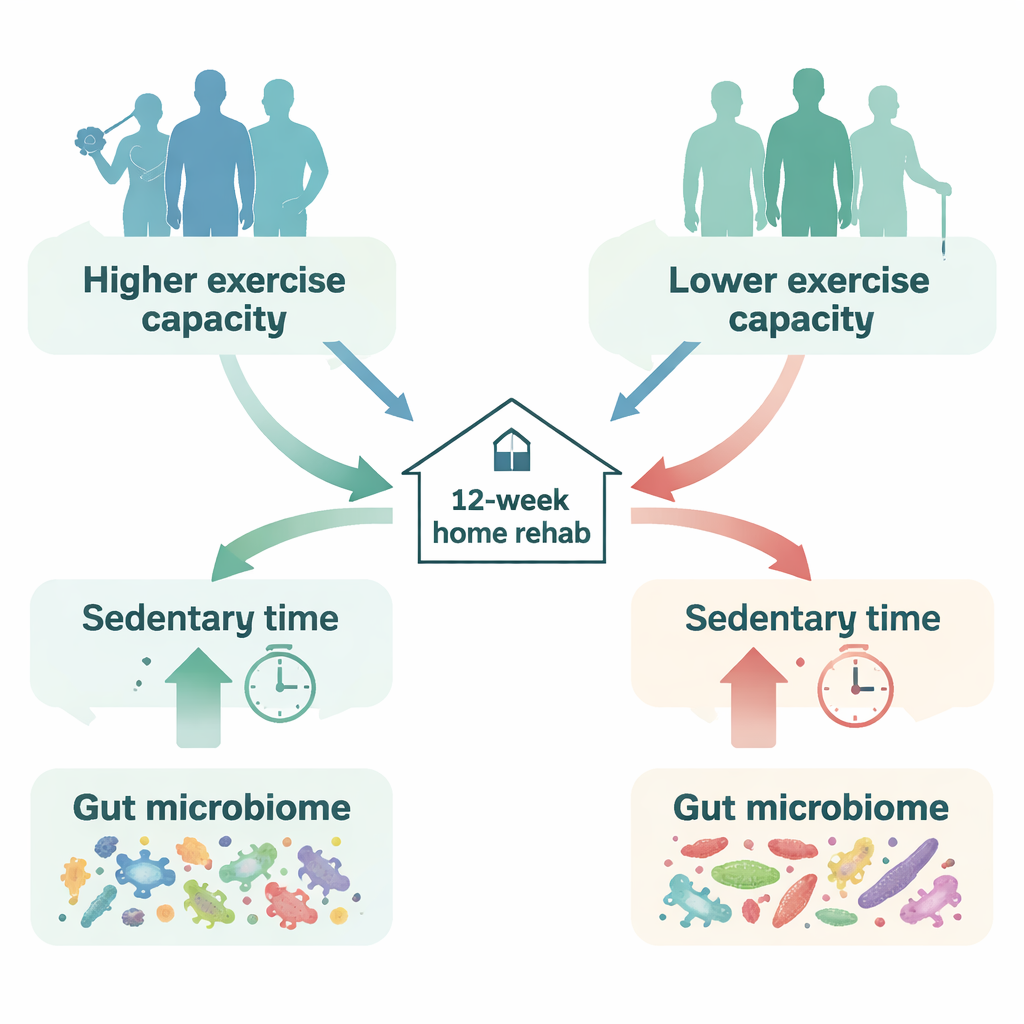
Two groups, same disease, different walking ability
The researchers followed 37 men with stable COPD who were treated at a single hospital in Japan. First, they measured how far each person could walk in six minutes, a common test of everyday exercise capacity. Using the median walking distance of 444 meters, they split the volunteers into two groups: a higher-capacity group that could walk farther and a lower-capacity group that could not. Although both groups had similar body weight and symptom scores, the higher-capacity patients were slightly younger, had smoked less, and had better lung function and stronger lower-body muscles. They also walked more steps per day and spent more time in moderate-to-brisk activity, even though both groups logged similar amounts of sitting time at the start.
A home rehab program that targets daily life
All participants completed a 12-week, home-based rehabilitation program. Instead of frequent hospital visits, they received one detailed instruction session, a printed rehab manual, and a pedometer. They were encouraged to reach a personalized step target based on age, breathlessness, and lung function. Each day, they recorded temperature, symptoms, breathlessness, and step counts in a diary. Their physical activity was tracked with a waist-worn motion sensor for two weeks before and after the program, capturing steps and time spent at different effort levels, from very light “sitting-style” activity to more demanding walking. Stool samples were also collected before and after rehab to analyze gut bacteria using modern DNA sequencing methods.
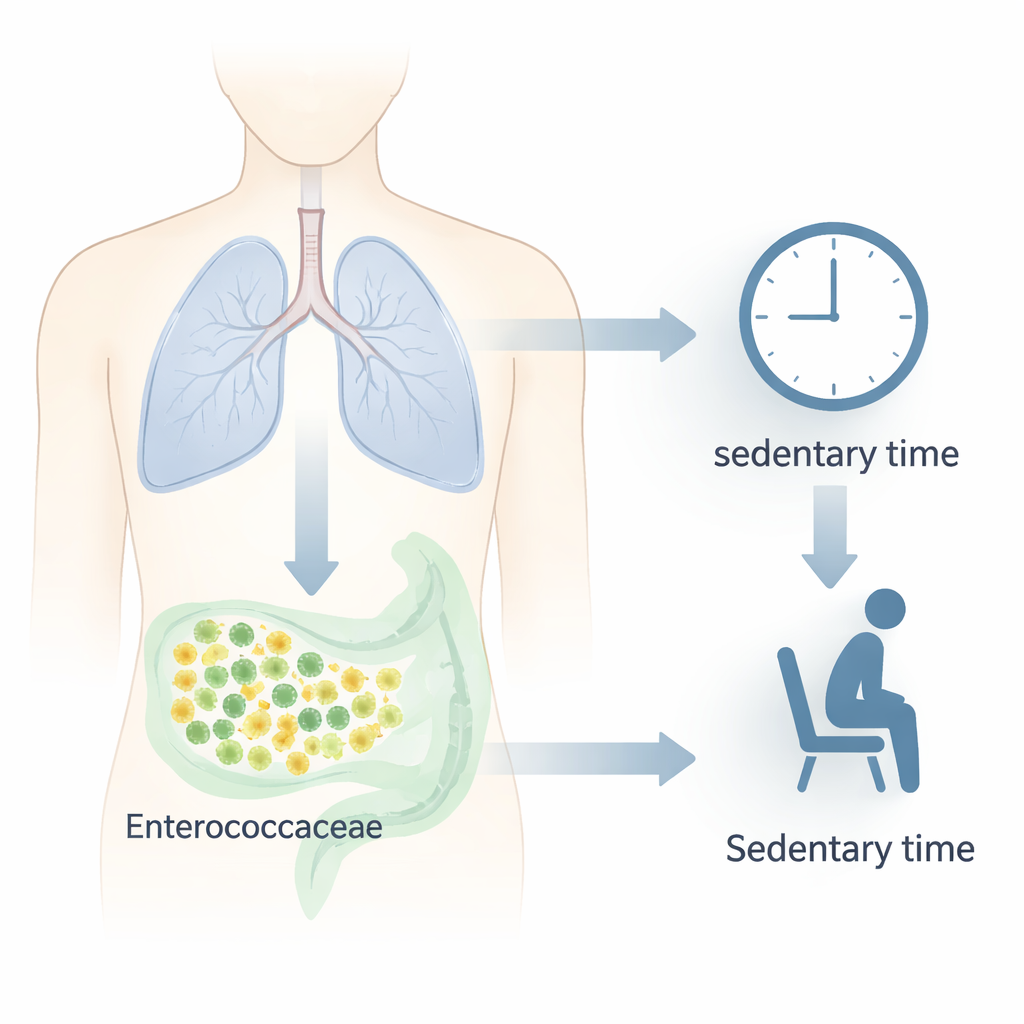
Same rehab, opposite changes in sitting time
Surprisingly, classic measures such as walking distance, muscle mass, and time spent in moderate or vigorous activity did not improve clearly in either group over 12 weeks. The striking change was in sedentary behavior—the time spent in very low-effort activities like sitting or lying down while awake. In the higher-capacity group, sedentary time fell by about 26 minutes per day on average. In the lower-capacity group, it actually rose by about 19 minutes per day. This suggests that people who start out able to walk farther may be more able, or more ready, to translate home rehab advice into small lifestyle changes like standing up or walking a bit more often.
Tiny gut residents that shift with behavior
The team then looked at the “gut microbiome,” the community of bacteria living in the intestines. At baseline, the overall mix of gut bacteria differed between higher- and lower-capacity patients, even though broad diversity measures were similar. Certain helpful groups, such as Faecalibacterium and some relatives within the Firmicutes family, were more common in higher-capacity patients, while others, including Veillonella and related types, were lower. After rehabilitation, both groups showed changes in specific bacterial families and genera, but the patterns were not the same. In the higher-capacity group—the only group whose sedentary time improved—a family of bacteria called Enterococcaceae clearly decreased. This particular change was not seen in the lower-capacity group, hinting that losing these bacteria may be linked to moving a bit more and sitting a bit less.
What this means for people living with COPD
For people with COPD, this study delivers two key messages in plain terms. First, even a modest home-based rehab program may help those who still have relatively good walking ability trim down the amount of time they sit each day, an important goal because long sedentary stretches are tied to higher death risk. Second, the gut seems to be part of the story: people who successfully reduced sitting time also showed a drop in specific gut bacteria that may be harmful. While the study is small and does not prove cause and effect, it points toward a future in which COPD care may combine early rehabilitation with approaches that gently reshape the gut microbiome, such as diet, probiotics, or other targeted treatments, to support more active daily lives.
Citation: Tashiro, H., Kuwahara, Y., Kurihara, Y. et al. Distinct gut microbiome signatures associated with sedentary behavior improvement following rehabilitation in chronic obstructive pulmonary disease patients with higher functional exercise capacity. Sci Rep 16, 7312 (2026). https://doi.org/10.1038/s41598-026-38360-7
Keywords: COPD, sedentary behavior, pulmonary rehabilitation, gut microbiome, exercise capacity