Clear Sky Science · en
Regional variations in serum pepsinogen levels and their influencing factors: a multi-center cross-sectional study
Why this matters for everyday health
Stomach cancer is one of the world’s most common cancers, yet many people never notice early warning signs. This study explores whether a simple blood test, already used to check the stomach’s condition, behaves differently in various parts of China—and how everyday habits like diet and infection with the common stomach bacterium Helicobacter pylori (H. pylori) might change the test’s readings. Understanding these differences could lead to more accurate, less invasive screening tailored to where people live and how they live.
A blood test window into the stomach
The blood test at the center of this research measures substances called pepsinogens, which are made in the stomach and help digest proteins. When the stomach lining becomes damaged or thinned, as it can along the pathway toward stomach cancer, levels of one type (PGI) and the ratio of PGI to another type (PGII) usually drop, while PGII can rise. Doctors have considered using these measurements to pick out people who might benefit most from an endoscopy, the camera test for the stomach. But a key unanswered question has been whether “normal” values are the same everywhere, or whether background differences in diet, infection, and other factors shift the baseline from region to region.
A nationwide checkup across twelve hospitals
To probe this, researchers analyzed data from 2,902 adults who went for routine health checkups at twelve medical centers across Southern, Eastern, Southwest, Northeast, Northern, and Central China between 2016 and 2021. Everyone had blood drawn to measure PGI and PGII, and most also underwent stomach examination with a scope and microscopic review of tissue samples. This allowed the team to group people by how healthy or damaged their stomach lining was—from non-atrophic gastritis (essentially no thinning) through mild and severe atrophy to full-blown cancer. Participants also completed detailed questionnaires on smoking, drinking, and how often they consumed salty foods, fruits, vegetables, and dairy products. H. pylori status was determined using breath, blood, and tissue tests.
What the blood revealed about stomach damage
First, the study confirmed that pepsinogen levels do track the stomach’s structural damage. Compared with people whose stomach lining was not thinned, those with mild or severe thinning and those with stomach cancer had progressively lower PGI levels and lower PGI/PGII ratios, while PGII tended to be higher. Age and H. pylori infection were more common in people with more advanced damage. Interestingly, H. pylori infection peaked in the most severely atrophic group but then fell in the cancer group, suggesting that the bacterium may disappear once the stomach environment becomes too hostile—even though the long-term harm has already been done.
Regional differences shaped by salt, fruit, and infection
The heart of the study focused on people whose stomachs appeared not thinned under the microscope (the “baseline” group). Even in this apparently healthy slice of the population, pepsinogen levels were not uniform across China. Central China’s baseline values differed clearly from most other regions, and Southern and Central China looked more alike than other pairings. When the researchers used statistical models to adjust for multiple influences, they found that older age, being male, having H. pylori infection (or a history of it), eating a high-salt diet, and dietary patterns involving fruits and vegetables were all independently linked with shifts in the PGI/PGII ratio. H. pylori infection was especially powerful: infected individuals had markedly lower ratios than uninfected ones. High salt intake was tied to a higher ratio, while frequent fruit consumption was associated with a lower ratio, and frequent vegetable intake with a higher ratio. These relationships held up when the team looked separately at infected and uninfected people, hinting that diet and infection act through partly distinct pathways on the stomach and its secretions.
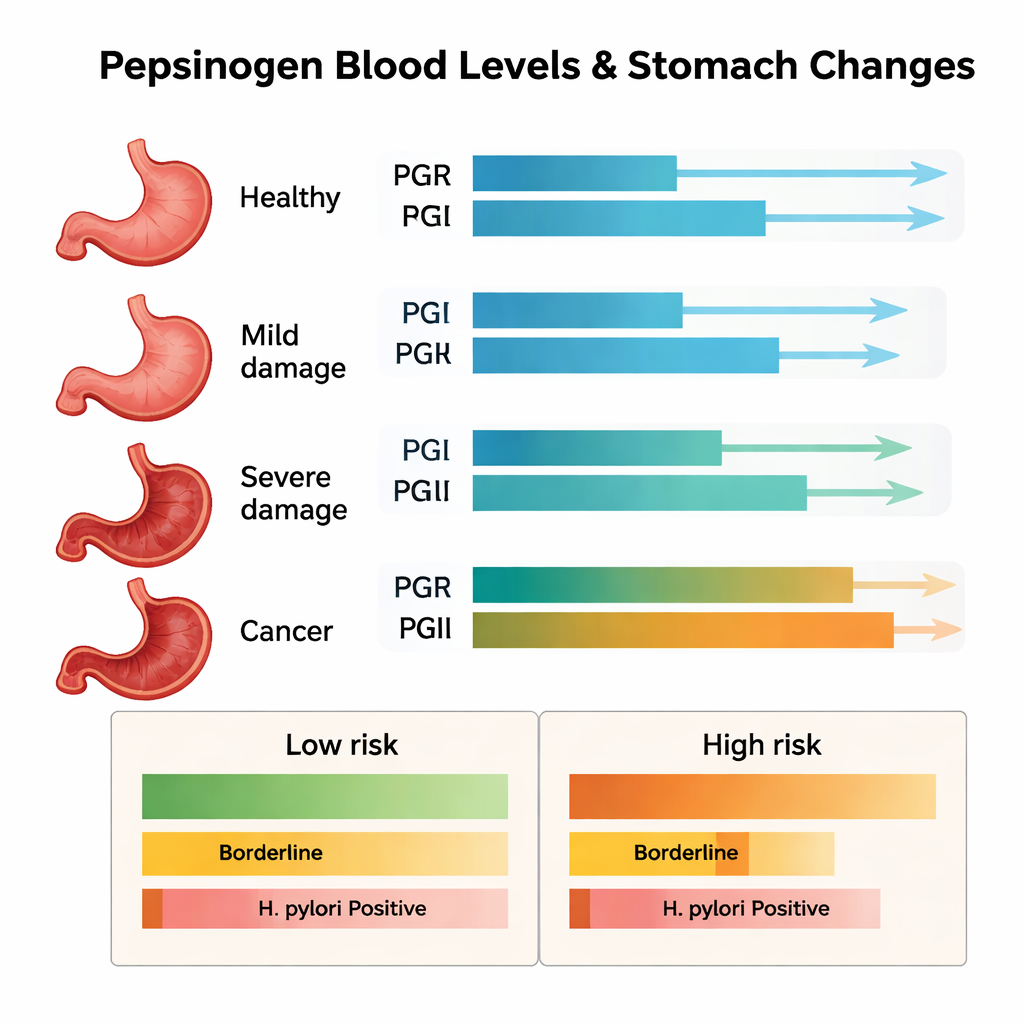
What this means for future screening
From a layperson’s perspective, the key takeaway is that a “normal” blood result is not truly one-size-fits-all. Where a person lives in China, whether they carry H. pylori, how much salt they eat, and how often they consume fruits and vegetables can all nudge stomach-related blood markers up or down, even before serious damage is visible. Because of this, using a single nationwide cutoff to decide who needs an endoscopy could miss people at risk in some regions while over-testing others elsewhere. The authors argue that region-specific and H. pylori–specific thresholds for pepsinogen tests may be needed to more accurately identify those at risk for precancerous stomach changes and gastric cancer, though they stress that future long-term studies must confirm the best cutoffs before such tailored screening can be put into routine practice.
Citation: Jiaojiao, H., Jiaying, Y. & Yuling, T. Regional variations in serum pepsinogen levels and their influencing factors: a multi-center cross-sectional study. Sci Rep 16, 7773 (2026). https://doi.org/10.1038/s41598-026-38326-9
Keywords: gastric cancer screening, pepsinogen blood test, Helicobacter pylori, diet and stomach health, regional differences in China