Clear Sky Science · en
Establishment and application of a duplex RPA-LFS detection system for Candida glabrata and Candida krusei
Why this matters for everyday patients
Hospital infections caused by fungi are quietly on the rise, and two culprits, Candida glabrata and Candida krusei, are especially worrying because many common antifungal drugs barely touch them. Doctors often have just a day or two to choose the right treatment, yet current lab tests can take nearly a week and miss many cases. This study reports a new rapid test that can spot these two hard-to-treat yeasts at the bedside in about half an hour, potentially saving lives and helping preserve the power of existing drugs.
Dangerous yeasts hiding in plain sight
Invasive yeast infections, grouped under the term invasive candidiasis, are now among the most common serious fungal infections in hospitals worldwide, with death rates reaching up to half of affected patients. Candida glabrata and Candida krusei stand out because they are unusually good at dodging standard medications. One often resists widely used azole drugs such as fluconazole by altering its drug targets and pumping drugs out of the cell, while the other comes with built-in resistance from the start. Because they respond differently to backup drugs, simply knowing that a patient has a “Candida infection” is not enough; clinicians urgently need to know which species is present within the first 24 to 48 hours of illness.
Why current tests fall short
Traditional laboratory methods rely on growing the yeast from blood or other body fluids and then testing which drugs stop its growth. This gold-standard approach can take three to seven days and still fails to detect up to half of true infections. Color-based culture plates and advanced DNA methods such as real-time PCR can speed things up, but they require specialized equipment, expert staff and dedicated laboratories. As a result, these tools are hard to deploy in emergency rooms, intensive care units in smaller hospitals or clinics with limited resources, exactly where quick answers are most needed.
A fast strip test built on clever chemistry
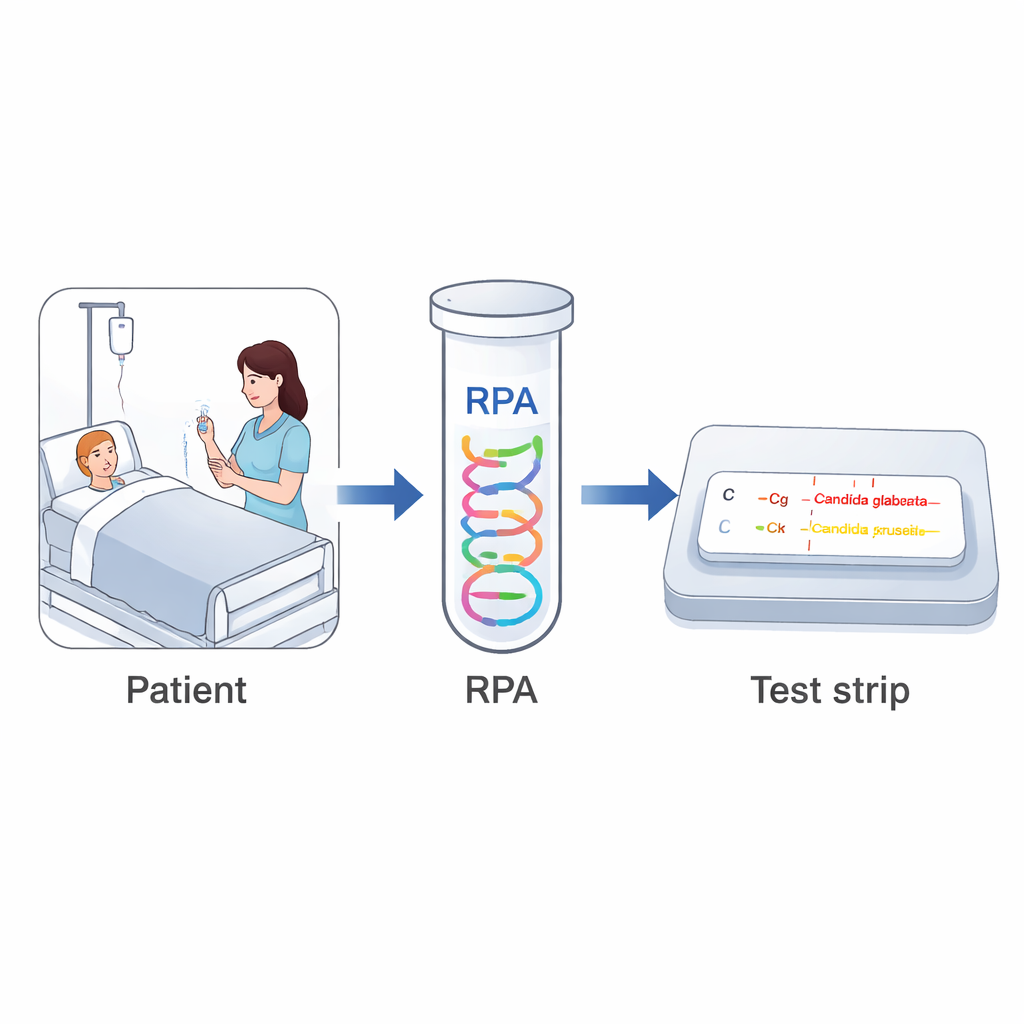
The research team combined two technologies to create a simple, dual-purpose test: recombinase polymerase amplification (RPA) and a lateral flow strip, the same basic format as a home pregnancy test. First, a tiny amount of DNA from a patient sample is placed in a small tube, where it is copied many times at body-like temperatures, without the need for a bulky thermal cycler. Special short DNA pieces, tailored to unique regions of the two yeast species, are tagged so that each species carries its own “color code.” After about 15 minutes of amplification, the liquid is dropped onto a paper-like strip. As it flows along, the tagged DNA is trapped on one of two test lines—one dedicated to C. glabrata, the other to C. krusei—while a separate control line confirms the strip is working. Within minutes, visible colored bands reveal whether none, one or both species are present, all by eye, without any machine. 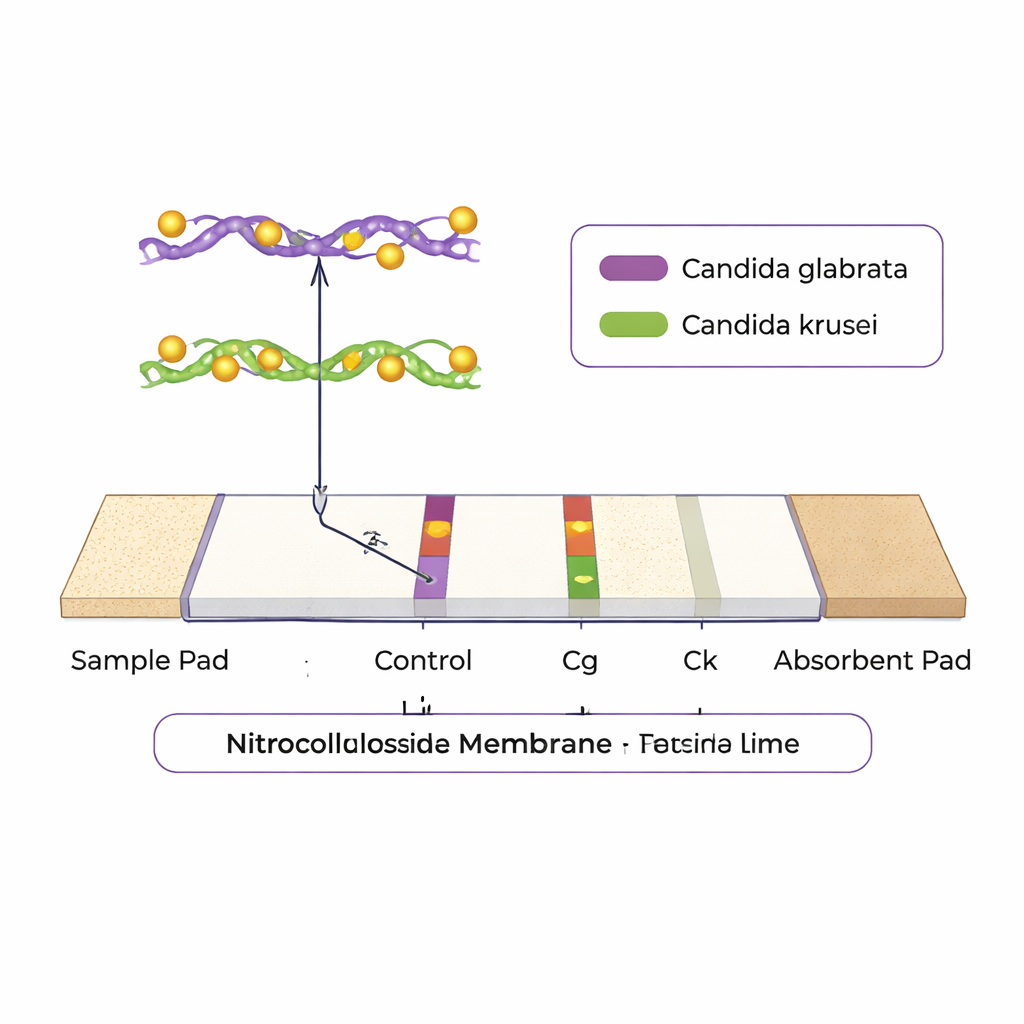
How well the new test performs
To see if this approach could work in the real world, the investigators challenged their system with many different yeast and bacterial strains, and with hundreds of patient samples. The strip reliably detected extremely low amounts of the target yeasts—down to about 10 genetic copies per milliliter for C. glabrata and 100 for C. krusei—levels on par with or better than standard PCR tests. It lit up for every one of the intended strains, including both reference and clinical isolates, while ignoring closely related yeasts and common hospital bacteria, showing no cross-reactions. In 328 real clinical samples, its results agreed perfectly with conventional qPCR: all 107 positive cases were correctly identified and separated by species, and all 221 negative samples remained negative. From sample preparation to visual readout, the entire process took about 30 minutes and needed only a simple heat source.
What this means for care and what comes next
For non-specialists, the core message is that this is essentially a rapid, two-in-one “yes/no and which one” strip test for dangerous, drug-resistant yeasts. It could allow doctors in intensive care units, emergency departments and small clinics to tailor antifungal treatment much earlier, instead of guessing and possibly using drugs that do not work. The same design principles—quick DNA copying at a single temperature plus a simple paper strip with multiple lines—could be expanded to detect more fungal species, including emerging threats such as Candida auris. While further work is needed to adapt the test to whole blood and to automate sample handling, this study shows that accurate, bedside-friendly detection of high-risk yeasts is within reach, bringing precision antifungal therapy closer to everyday clinical practice.
Citation: Wang, L., Lu, Y., Zhang, T. et al. Establishment and application of a duplex RPA-LFS detection system for Candida glabrata and Candida krusei. Sci Rep 16, 7717 (2026). https://doi.org/10.1038/s41598-026-38310-3
Keywords: Candida infection, rapid fungal testing, drug-resistant yeast, point-of-care diagnostics, lateral flow assay