Clear Sky Science · en
Ursodeoxycholic acid alleviates α-Casein-induced cow’s milk protein allergy via the TGR5/NF-κB signaling pathway
Why baby milk allergies matter
For many families, the first signs that something is wrong with a baby’s health are alarming episodes of vomiting, diarrhea, or blood-streaked stools after feeding. One of the most common culprits is cow’s milk protein allergy, in which the infant’s immune system overreacts to proteins in milk. This study explores how a natural substance made from bile, called ursodeoxycholic acid (UDCA), might help calm this kind of allergy by repairing the gut lining and dialing down inflammation.
Milk, microbes and an overactive gut
Cow’s milk protein allergy most often shows up as tummy troubles rather than dramatic swelling or hives. The lower part of the colon becomes inflamed, the protective lining of the gut is damaged, and babies can fail to gain weight properly. In recent years, scientists have learned that the trillions of bacteria in the intestine, and the chemical by-products they make, are closely linked to these problems. In earlier work, the authors found that infants with this allergy had low levels of several “secondary bile acids” made by gut microbes, especially UDCA, hinting that this missing molecule might be important in controlling gut inflammation.
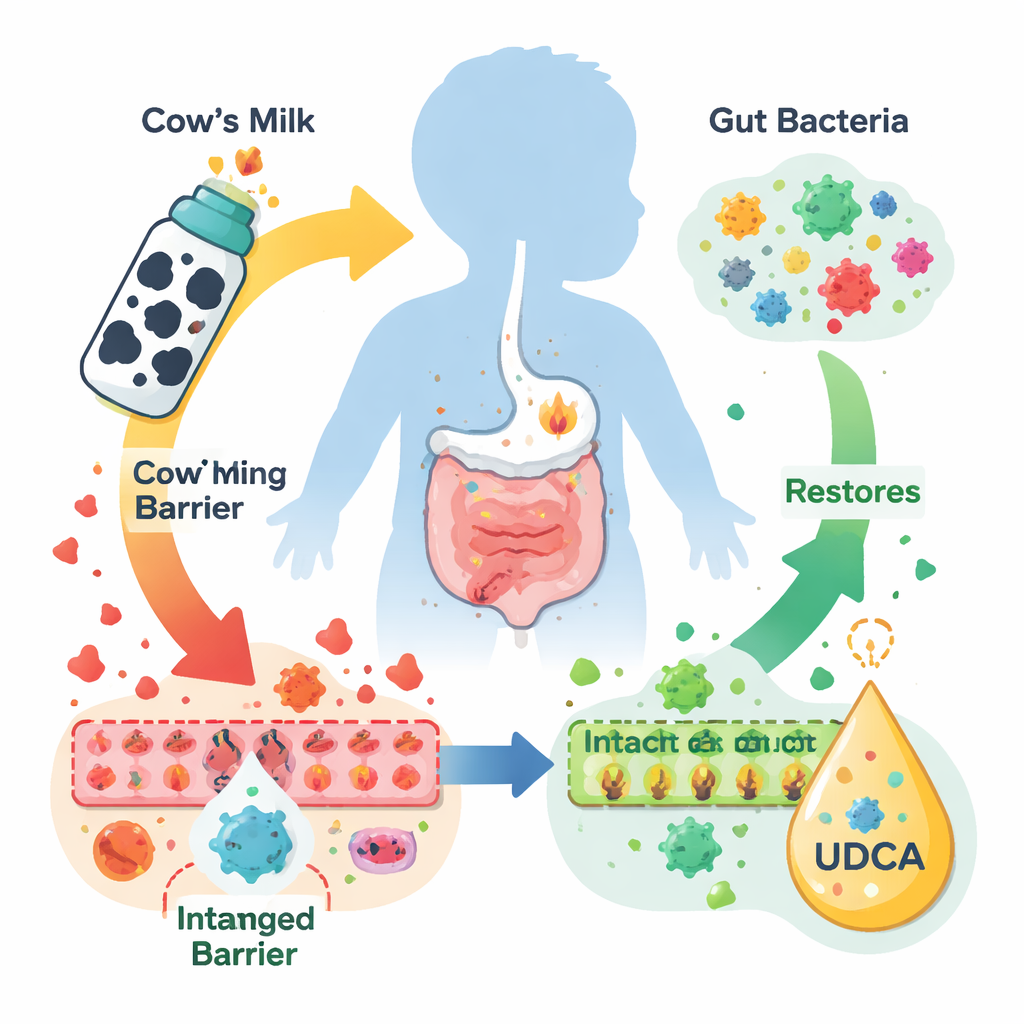
A mouse stand‑in for milk‑allergic babies
To test UDCA’s role, the researchers created a mouse model of cow’s milk protein allergy using α‑casein, one of the main milk proteins that often triggers strong reactions in children. Mice that were repeatedly exposed to α‑casein developed classic allergic signs such as wheezing, intense scratching, and poor weight gain. When the animals were examined under the microscope, their livers showed damage and immune cell invasion, and their colons had ulcers, distorted glands, and a loss of mucus‑producing goblet cells that normally help shield the gut wall. Giving the mice UDCA by mouth, especially at a moderate dose, eased their clinical symptoms, helped them regain weight, and largely restored normal liver and colon structure, including the number of goblet cells and the integrity of the tight junctions that seal neighboring intestinal cells together.
Turning down the immune “fire”
The team then asked how UDCA was changing the immune response. In the colons of allergic mice, genes that encode powerful inflammatory messengers such as IL‑1β and TNF‑α, as well as several chemokines that call more immune cells into the tissue, were strongly switched on. UDCA treatment sharply reduced the activity of these genes and boosted the gene for occludin, a protein central to maintaining a leak‑proof intestinal barrier. Focusing on macrophages—immune cells that both clean up damage and orchestrate inflammation—the researchers showed that UDCA improved their ability to move and “heal” in culture while simultaneously reducing production of inflammatory molecules, nitric oxide, and reactive oxygen species that can injure surrounding tissue.
A molecular brake inside immune cells
At the molecular level, UDCA acted through a receptor called TGR5, found on the surface of macrophages and other cells. In allergic mice, levels of TGR5 in the colon fell, while activity of NF‑κB, a master switch that drives inflammatory gene expression, rose. UDCA reversed this pattern: it increased TGR5, raised levels of the messenger molecule cAMP inside cells, and blocked the movement of the NF‑κB component p65 into the nucleus where it turns on inflammatory genes. When the scientists added a drug that specifically blocks TGR5, UDCA could no longer effectively shut down NF‑κB or reduce cytokine production, showing that this receptor is a key part of its action. Similar effects were seen in macrophage cell lines exposed to α‑casein, strengthening the case that the same pathway operates in gut immune cells.
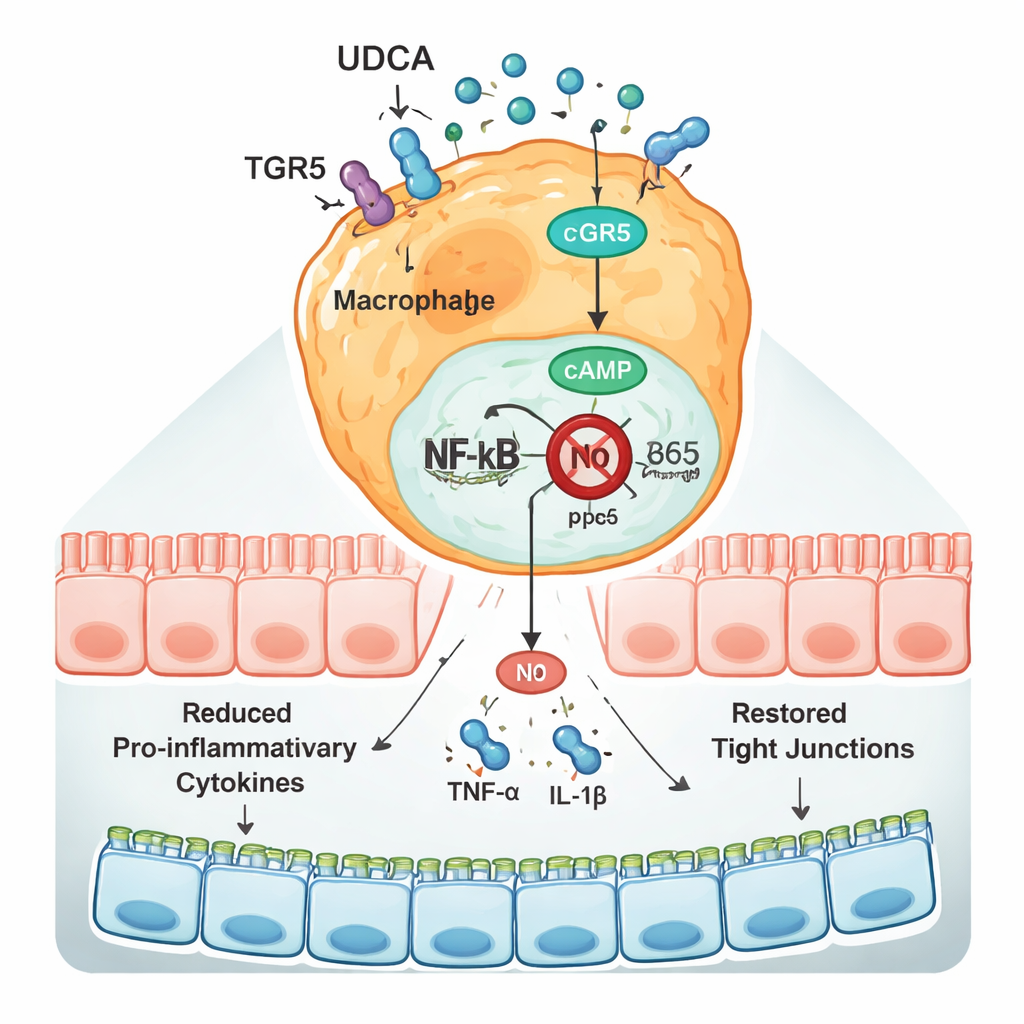
What this could mean for children
Put simply, this work suggests that UDCA, a molecule our own bodies and gut microbes can make, helps “cool” milk‑induced gut allergies by shoring up the intestinal barrier and reprogramming macrophages into a less aggressive, more repair‑oriented state. It does this mainly by activating TGR5 and in turn putting a brake on the NF‑κB system that fuels inflammation. While these findings come from mice and cultured cells, they point to UDCA—or therapies that increase its levels or mimic its effects—as a potential future strategy to ease cow’s milk protein allergy and perhaps other gut‑based allergic diseases. Further studies in humans and careful work on how UDCA interacts with the developing gut microbiome will be essential before such treatments reach the clinic.
Citation: Yu, Z., Wang, Z., Yue, L. et al. Ursodeoxycholic acid alleviates α-Casein-induced cow’s milk protein allergy via the TGR5/NF-κB signaling pathway. Sci Rep 16, 7808 (2026). https://doi.org/10.1038/s41598-026-38293-1
Keywords: cow’s milk protein allergy, ursodeoxycholic acid, gut microbiota, intestinal inflammation, macrophages