Clear Sky Science · en
Subendometrial platelet-rich plasma injection for refractory thin endometrium: a prospective pilot study
Why this fertility study matters
For many people undergoing in vitro fertilization (IVF), one stubborn hurdle is a uterine lining that stays too thin for an embryo to implant and grow. Standard drugs and procedures sometimes fail to fix this problem, leaving couples with repeated disappointments and cancelled treatment cycles. This study explores a promising new option: injecting a patient’s own platelet-rich plasma—concentrated healing components from blood—just beneath the surface of the uterine lining to see whether it can safely thicken the tissue and improve the chances of pregnancy.
A tough problem in IVF treatment
The inner lining of the uterus, called the endometrium, must reach a certain thickness and blood supply to welcome an embryo. When it remains thin despite powerful hormones and surgical repair, doctors call it “refractory” thin endometrium. Women with this condition often have scarring from past procedures, infections, or other damage that leaves the tissue fibrous and poorly supplied with blood. Even with modern fertility techniques, these patients face low implantation rates, frequent cycle cancellations, and a heavy emotional and financial burden.
Using the body’s own repair toolkit
Platelet-rich plasma (PRP) is made by concentrating platelets, the blood components best known for helping clots form. Platelets also release many growth factors that encourage new blood vessels and tissue repair. In orthopedics and skin medicine, PRP has been used to stimulate healing. Fertility specialists have recently begun applying PRP inside the uterus to try to coax the lining to grow. However, simply dripping it into the cavity may not deliver enough of these repair signals to the deep layer where the lining regenerates. This study tested a more targeted approach: injecting PRP directly into the tissue just beneath the lining surface, guided by a tiny camera and ultrasound.
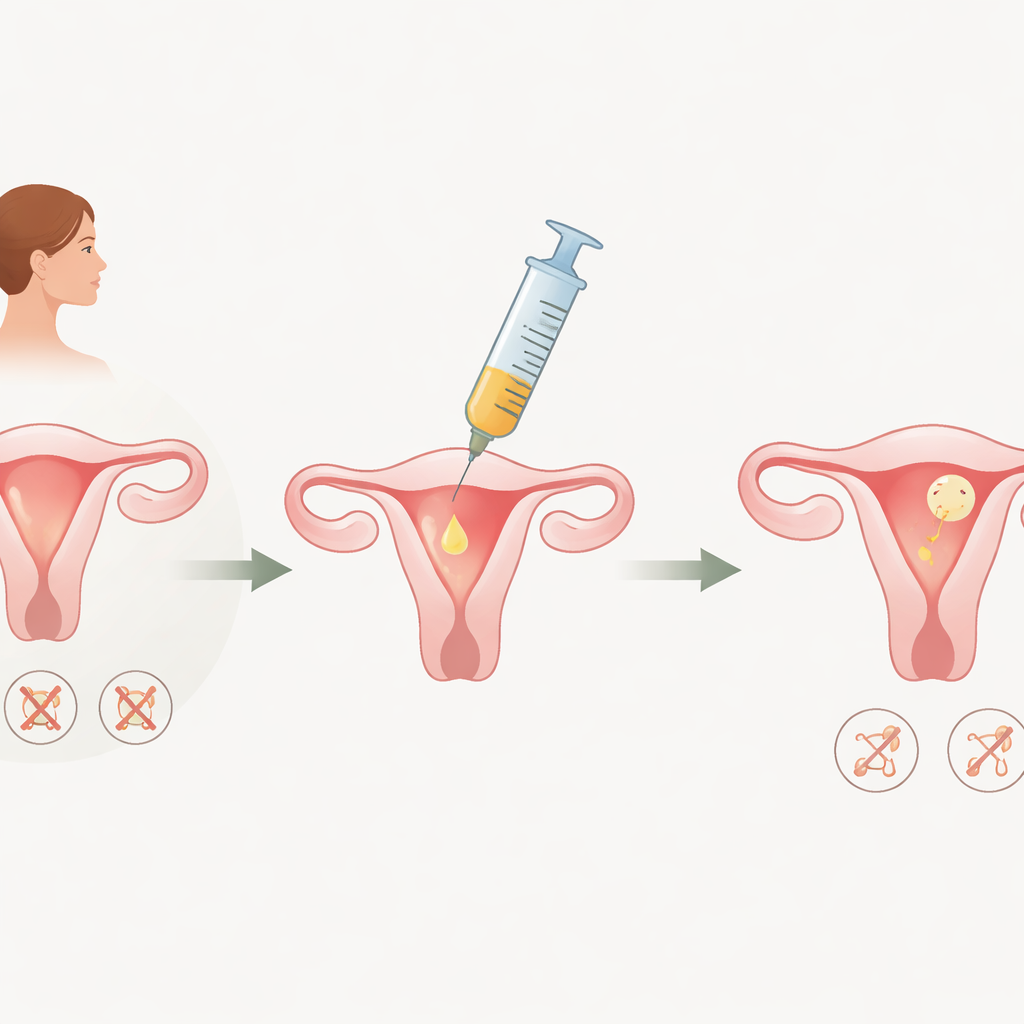
How the pilot trial was done
The researchers enrolled 21 women with long-standing thin uterine linings—less than 7 millimeters thick—who had already failed at least two rounds of standard treatments. Eighteen completed the study and served as their own comparison group, with their results after PRP measured against their past IVF or frozen embryo transfer cycles. Each woman first had her uterine cavity checked with a scope. Then doctors injected about four milliliters of her own PRP into several spots in the uterine wall, including scarred areas when present. In the following cycle, they used their usual frozen-embryo transfer routine, adjusting estrogen and progesterone to support growth of the lining and proceeding to transfer once its thickness and appearance were acceptable.
What changed after PRP injections
Overall, the uterine lining became measurably thicker after the subendometrial PRP treatment, increasing by about 0.9 millimeters on average. Two-thirds of the women finally reached a lining of at least 7 millimeters, a level often associated with better outcomes in IVF. Blood flow signals around the lining improved in most patients who started with poor circulation, and scarring inside the cavity eased in some cases. Importantly, the procedure appeared safe: there were no serious side effects or treatment withdrawals, and the PRP samples were highly enriched in platelets while containing very few white or red blood cells, reducing the chance of inflammation.
Pregnancy results and remaining questions
Among the 18 women who completed the protocol, eight pregnancies occurred, giving a clinical pregnancy rate of 44.4 percent and an implantation rate of 40 percent for transferred embryos. There were two live births and six ongoing pregnancies at the time of reporting. Most pregnancies arose from transfers of embryos that had been grown to the blastocyst stage, which is already known to improve IVF success. Not every woman benefited: those with very severe adhesions and those with poorer ovarian reserve still struggled, and in two cases the lining actually became thinner. The study also suggested that there may be a “sweet spot” for how concentrated the platelets should be, since very high baseline platelet counts were more common in women who did not conceive.
What this could mean for patients
For people facing repeated IVF failures because the uterine lining refuses to respond, this early study offers cautious hope. Direct injection of platelet-rich plasma appeared to safely thicken the lining and was linked to encouraging pregnancy rates in a group for whom standard options had largely been exhausted. At the same time, the research was small, lacked a comparison group, and cannot yet prove that PRP was the decisive factor behind each pregnancy. Larger, controlled trials are now needed to pin down who benefits most, how often injections should be given, and what dose works best. Until then, subendometrial PRP remains an experimental but intriguing tool in the effort to help more embryos find a stable home.
Citation: Zhang, H., Wang, H., Yu, J. et al. Subendometrial platelet-rich plasma injection for refractory thin endometrium: a prospective pilot study. Sci Rep 16, 9240 (2026). https://doi.org/10.1038/s41598-026-38286-0
Keywords: thin endometrium, platelet-rich plasma, IVF, endometrial thickness, fertility treatment