Clear Sky Science · en
Genomic analysis of ST117, 155, 1011, 167, 744, and 17391 in poultry-associated multidrug resistant Escherichia coli isolates from India
Why chicken farms matter to your health
Chicken is one of the world’s favorite meats, and India’s poultry industry is expanding rapidly to keep up with demand. But along with affordable protein comes a quieter problem: some bacteria living in poultry farms are becoming resistant to many of the antibiotics doctors rely on to treat infections in people. This study looks closely at drug-resistant Escherichia coli (E. coli) from poultry farms in southern India to understand how common they are, what makes them dangerous, and how they might spread from barns and bedding into the wider environment and, eventually, into human communities.
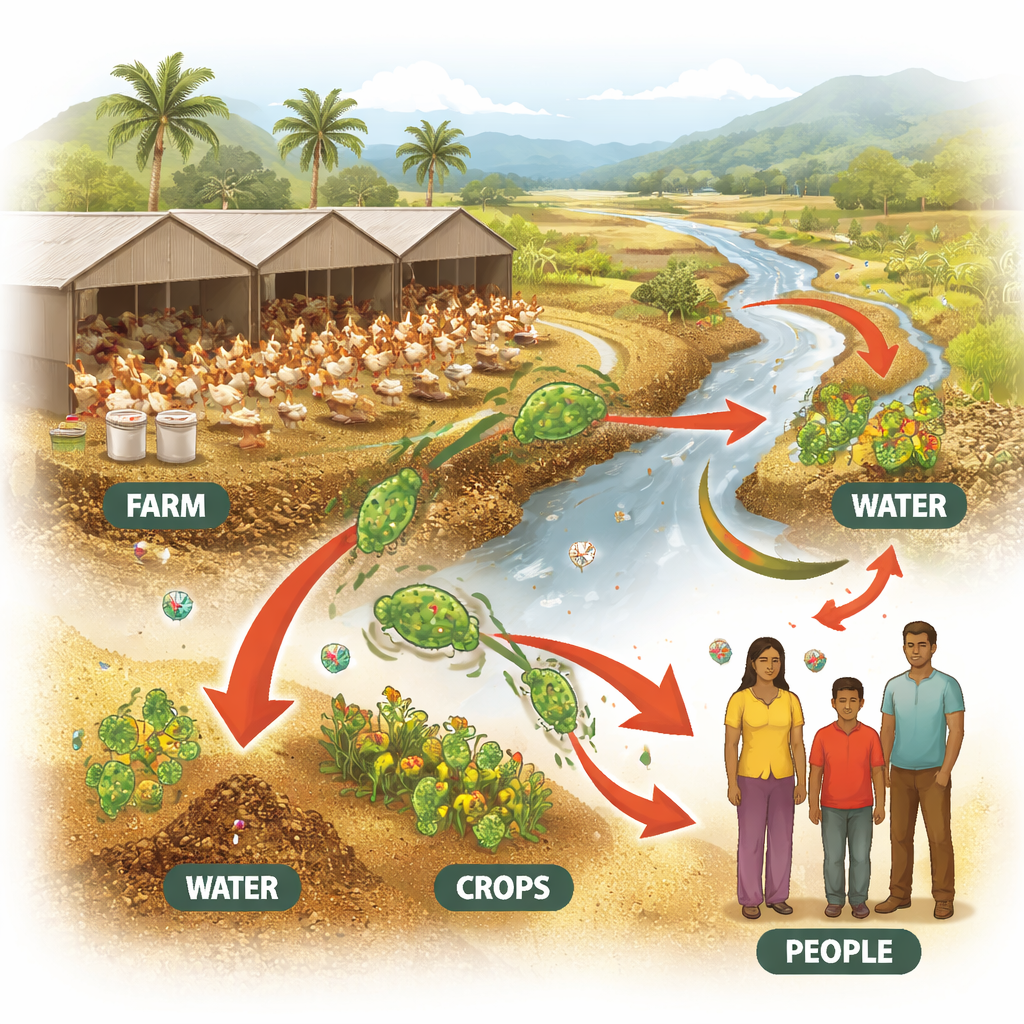
Digging into dirty bedding and farm water
The researchers collected 38 samples of bedding material and drinking water from seven poultry farms in Tamil Nadu. These are places where bird droppings, leftover feed, and spilled water mix—a perfect setting for bacteria to grow and swap genetic material. Lab tests showed that many E. coli from these samples were able to withstand several common antibiotics, including penicillins, cephalosporins, fluoroquinolones, and tetracycline. On average, each strain was resistant to more than half of the drugs tested, a warning sign that antibiotics are being heavily and repeatedly used in these flocks.
Reading the bacteria’s instruction manuals
To understand why these bacteria are so hard to kill, the team chose seven of the most resistant E. coli strains and read their entire DNA sequences—a bit like scanning the full instruction manual for each microbe. They discovered many known resistance genes, including ones that protect against tetracycline, fluoroquinolone, and several other antibiotic families. Some strains carried powerful beta-lactamase genes, such as CTX-M and TEM-1B, which can neutralize a wide group of penicillin-like drugs that doctors often use for serious infections. The bacteria also carried small extra DNA rings called plasmids, which can move between bacteria and help spread resistance traits quickly across a farm.
Global troublemakers in Indian chicken sheds
When the researchers compared these E. coli to strains reported around the world, several of them fell into “pandemic” lineages—genetic families that have been linked to disease in both animals and humans. These included ST117, ST167, and ST744, which have appeared in farm animals, hospital patients, and environmental samples in many countries. Even more concerning, the team identified a brand-new genetic type, ST17391, in the bedding from one farm. This strain carried genes that help it withstand multiple drugs and may also make it better at colonizing animals or people. Finding such high-risk lineages in routine farm samples suggests that poultry operations can act as quiet hubs for bacteria that are already known to cause hard-to-treat infections in hospitals.
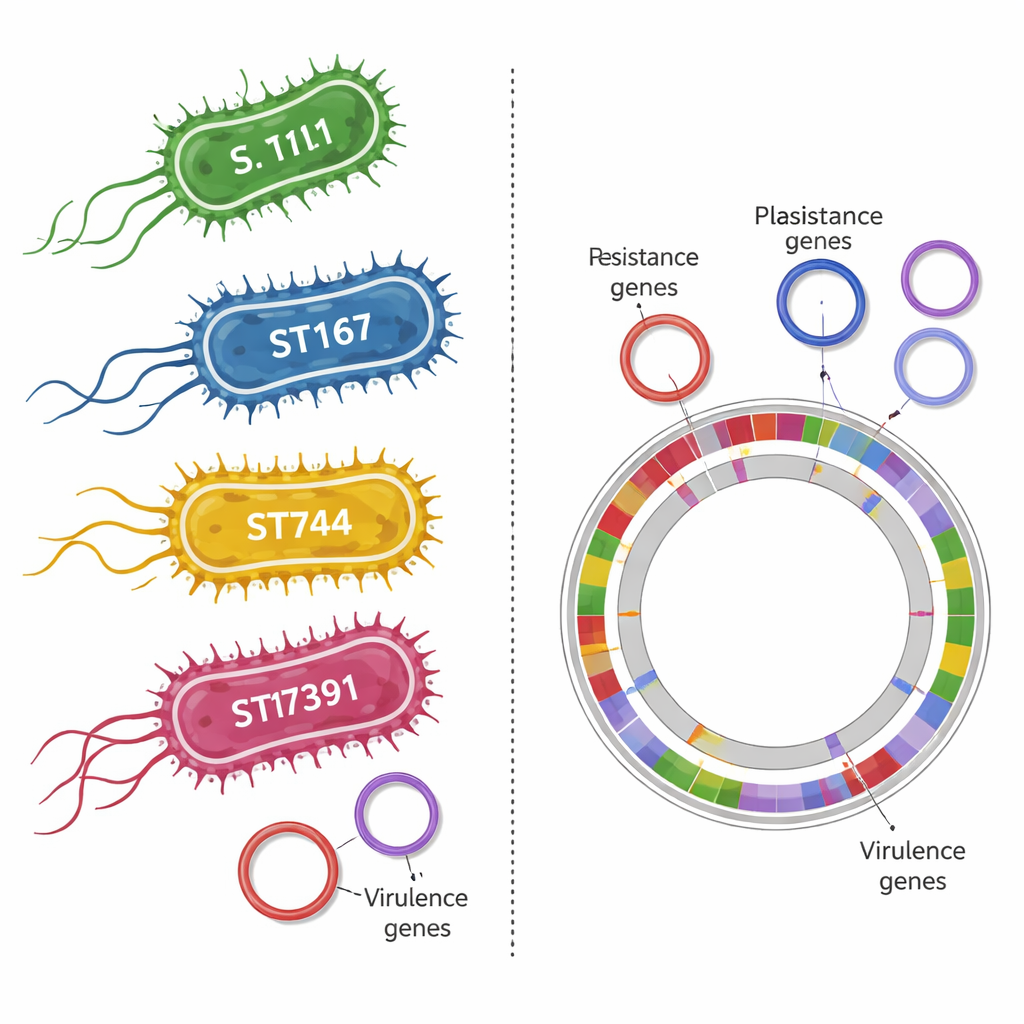
Hidden helpers that make bacteria more harmful
The DNA scans revealed not only resistance genes but also “virulence” genes—traits that help E. coli stick to tissues, steal iron from the host’s body, and survive attacks from the immune system. Many of the strains carried combinations of these factors, indicating they are not just harmless passengers. In one case, the scientists went beyond single strains and sequenced all the DNA in a sample of bedding from a farm with a particularly worrisome E. coli type. This metagenomic snapshot showed a crowded community of microbes carrying genes that resist multiple classes of antibiotics. In effect, the bedding acted as a genetic marketplace where resistance traits are stored and shared among many species.
What this means for farms, food, and families
For non-specialists, the message is clear: how we raise chickens can influence the effectiveness of antibiotics in human medicine. Routine use of these drugs in poultry helps select for E. coli that carry powerful resistance genes and virulence factors, which can leave the farm on contaminated litter, in water runoff, or along the food chain. The study’s authors argue for a “One Health” approach that treats human, animal, and environmental health as deeply linked. They call for better waste handling, stricter rules on antibiotic use in farms, and wider DNA-based surveillance to track dangerous bacterial lineages. These steps, they argue, are essential to keep everyday infections treatable and safeguard antibiotics for future generations.
Citation: P, R., Srijith, L., G, K. et al. Genomic analysis of ST117, 155, 1011, 167, 744, and 17391 in poultry-associated multidrug resistant Escherichia coli isolates from India. Sci Rep 16, 7438 (2026). https://doi.org/10.1038/s41598-026-38232-0
Keywords: antimicrobial resistance, poultry farming, Escherichia coli, One Health, whole genome sequencing