Clear Sky Science · en
A bilayered microneedle patch loaded with methotrexate and dexamethasone for transdermal treatment of psoriasis
Why a tiny patch could matter for itchy, scaly skin
Psoriasis is more than just dry, flaky skin: it is a chronic immune disease that can cause pain, intense itching, and embarrassment, and it often comes with other health problems such as arthritis and heart disease. Many people need years of treatment, but pills and injections can bring serious side effects, while ordinary creams struggle to get drugs through the tough outer layer of skin. This study explores a new idea: a fingertip-sized patch covered with microscopic, dissolving needles that can quietly push two familiar drugs right into the inflamed skin, aiming for strong relief with fewer whole‑body risks.
A stubborn skin disease that runs deep
Psoriasis develops when the body’s defense system mistakenly attacks healthy skin, driving skin cells to multiply far too quickly. Instead of renewing over weeks, the outer skin layers turn over in just days, building up as thick, red, scaly plaques. Immune cells and chemical “alarm signals” called inflammatory factors flood the area, keeping the reaction going. Doctors already use two powerful medicines to calm this storm: methotrexate, which tamps down overactive immune cells, and dexamethasone, a strong anti‑inflammatory steroid. Taken by mouth or injection, however, these drugs travel through the whole body, can irritate the liver and other organs, and are not ideal for life‑long use. Creams and ointments avoid some of these issues but are largely blocked by the skin’s outer shield, so much of the medicine never reaches the problem zone.
A two-layer needle you can barely feel
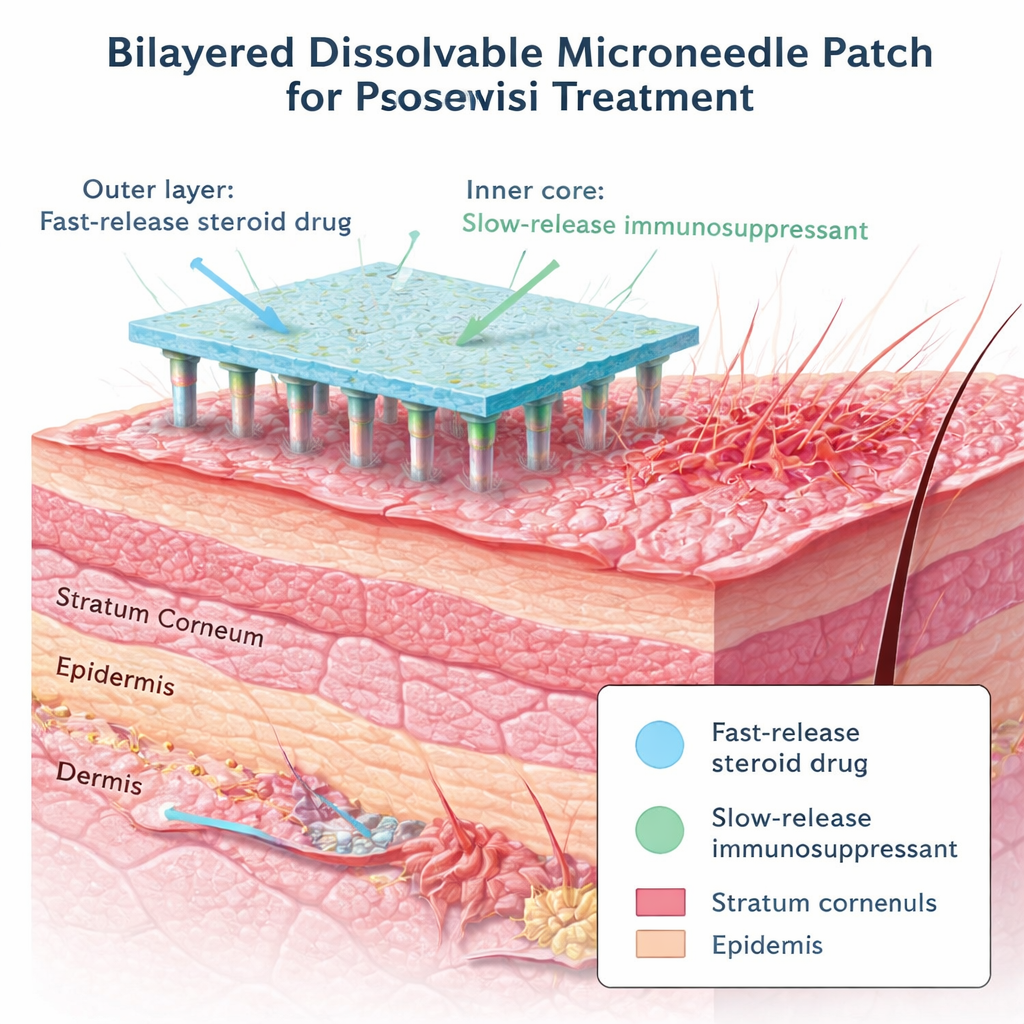
To solve this delivery problem, the researchers created a “bilayer microneedle patch,” a flexible strip carrying a 12 by 12 grid of microscopic, water‑soluble needles. Each needle is shorter than a millimeter and thin enough to slip through the outer skin without the pain of a normal injection. The upper part of each needle is made from a sturdy gelatin and polyvinyl alcohol gel that carries dexamethasone and provides the strength needed to pierce the skin. The deeper core is built from a modified form of hyaluronic acid, a natural substance found in skin, which is chemically linked to methotrexate. Once pressed onto the skin, the needles quickly pierce the hardened outer layer and then dissolve, leaving the drugs embedded directly within the diseased tissue.
Fast relief on the surface, slow control underneath
In laboratory tests and mouse studies, the patch behaved in a carefully staged way. The outer steroid‑loaded layer released dexamethasone quickly, especially in the slightly acidic, cooler conditions typical of psoriatic plaques, providing a rapid anti‑inflammatory effect. The inner methotrexate core released its drug much more slowly over at least two days, acting as a longer‑term “brake” on runaway skin cell growth and immune activity. Tests showed that the microneedles were strong enough to pierce skin without breaking, formed tiny channels that closed within about half an hour, and dissolved completely. Cell cultures exposed to extracts from the patch remained mostly healthy, and blood tests suggested that the materials did not damage red blood cells, indicating good basic safety.
Calmer skin, quieter immune signals
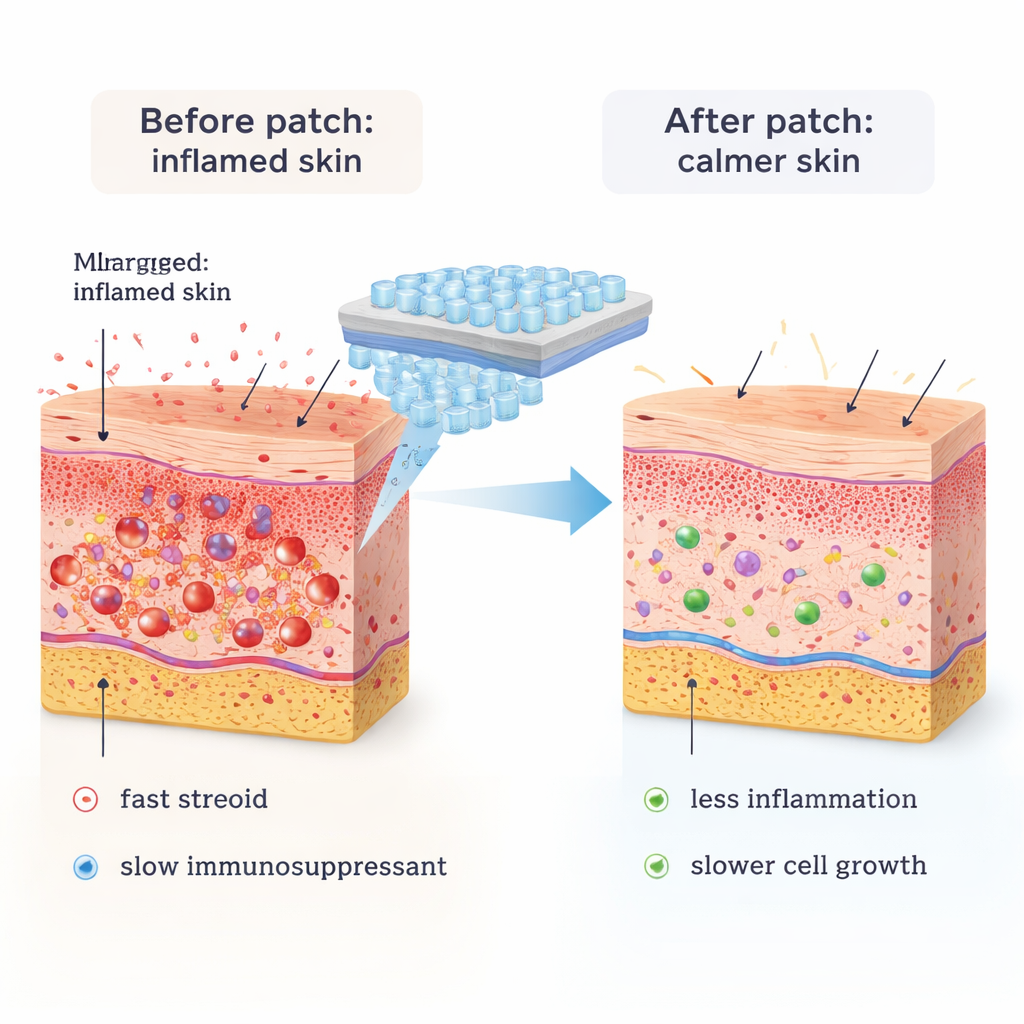
When the team used the patch on mice with chemically induced psoriasis‑like lesions, the animals’ red, thick, scaly skin improved markedly. Compared with untreated mice, or mice given empty patches, those treated with drug‑loaded microneedles showed thinner outer skin, fewer invading immune cells, and smoother surface appearance. Their clinical scores for redness, scaling, and thickness dropped, in some cases matching or surpassing the effect of a standard prescription ointment. Blood tests revealed that key inflammatory signals—such as TNF‑α, IL‑6, IL‑1β, and IL‑17A—fell sharply. In immune cell experiments, the patch’s drug mix nudged inflammatory “fighter” macrophages toward a more calming, tissue‑repairing state. Detailed gene‑activity profiling of treated skin confirmed that pathways linked to inflammation and abnormal skin growth were dialed down, while those involved in tissue repair were more balanced.
What this could mean for people with psoriasis
Put simply, this bilayer microneedle patch is designed to do what pills and creams struggle to accomplish: get the right drugs to the right place, in the right order, with less impact on the rest of the body. The fast‑acting outer layer aims to quickly soothe redness and itching, while the slow‑release inner core works behind the scenes to keep the disease in check. Although this work has so far been done in cells and mice, not people, it points toward a future where some psoriasis patients might manage flares with a nearly painless patch applied at home, instead of repeated systemic treatments. If confirmed in human studies, such patches could offer a more precise, convenient, and potentially safer way to live with a long‑lasting skin disease.
Citation: Wang, T., Li, D., Bi, H. et al. A bilayered microneedle patch loaded with methotrexate and dexamethasone for transdermal treatment of psoriasis. Sci Rep 16, 7604 (2026). https://doi.org/10.1038/s41598-026-38216-0
Keywords: psoriasis, microneedle patch, transdermal drug delivery, methotrexate, dexamethasone