Clear Sky Science · en
Advancements in psoriasis classification using custom transfer learning algorithms
Why smarter skin diagnosis matters
Psoriasis is more than a stubborn rash. This long‑lasting skin condition can crack, bleed, itch, and even damage joints, disrupting sleep, work, and social life. Yet doctors still diagnose it mostly by eye, which can be slow and subjective—especially when the disease takes different forms on different parts of the body. This study explores how modern artificial intelligence (AI) can help: by training computer programs to recognize seven distinct types of psoriasis from photographs of the skin, with an accuracy that rivals, and may one day support, expert clinicians.
One disease, many faces
Psoriasis does not look the same on everyone. The researchers focus on seven subtypes: plaque (the classic scaly patches), guttate (small drop‑like spots), nail psoriasis, pustular psoriasis (pimple‑like bumps filled with pus), erythrodermic psoriasis (widespread fiery redness), inverse psoriasis (smooth red patches in skin folds), and psoriatic arthritis, which combines skin changes with painful, swollen joints. Distinguishing among these matters because each type can call for different treatments and signals different risks. However, symptoms can overlap with one another and with other skin diseases, which makes visual diagnosis challenging, especially outside specialist clinics.
Building a rich picture library
To teach computers to tell these subtypes apart, the team first had to assemble suitable data. Existing public skin‑image collections rarely label the exact psoriasis subtype, and some forms are much rarer than others. The authors pulled together 4,005 images from several open medical image repositories, including ISIC, HAM10000, and DermNet. They then grouped each image into one of the seven psoriasis categories. To prevent the computer from over‑learning common types and ignoring rare ones, they used “image augmentation”: creating varied copies of pictures by rotating, zooming, and flipping them. This balancing step made the dataset more even across all seven classes and helped the models learn robust patterns instead of memorizing a few frequent examples.
Teaching machines to read the skin
Rather than starting from scratch, the researchers relied on transfer learning. They took three powerful image‑recognition systems—ResNet50, InceptionResNetV2 (referred to as InceptionV2 here), and InceptionV3—originally trained on millions of everyday photos, and fine‑tuned them on psoriasis images. Before feeding in the pictures, they standardized each one to a fixed size and normalized the pixel values. They then froze most of the internal layers, added new “top” layers tailored to the seven psoriasis types, and trained these additions on their curated dataset. Two popular training procedures, called Adam and RMSprop optimizers, were compared to see which produced more reliable learning.
Which AI learns psoriasis best?
All three AI models could recognize psoriasis types with promising accuracy, but one clearly stood out. The ResNet50 model performed reasonably well, correctly classifying around four out of five test images. InceptionV2 did much better, reaching about 97% accuracy on unseen test data when trained with the RMSprop optimizer. The strongest results came from InceptionV3, again paired with RMSprop: it correctly identified the subtype for about 99% of test images, and its precision and sensitivity (how often its positive predictions and detections were right) were similarly high. Visual explanation tools, which highlight the areas of an image that drive the AI’s decision, showed that the model focused on clinically meaningful regions of the lesions rather than irrelevant background, an encouraging sign for future clinical trust.
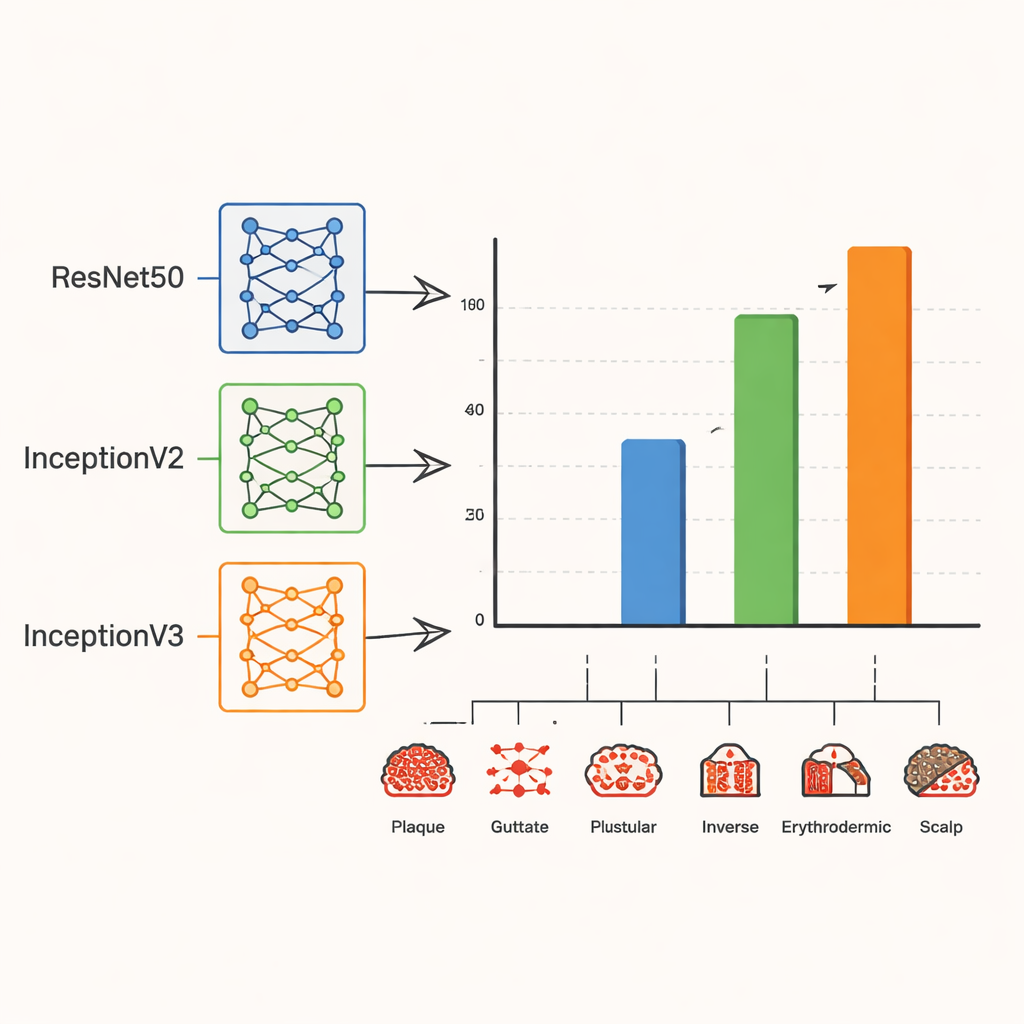
What this could mean for patients
For people living with psoriasis, these advances do not replace a dermatologist, but they could soon provide a powerful second set of eyes. An accurate, automated system able to sort skin photos into detailed subtypes could support telemedicine, help non‑specialist doctors in remote areas, and flag complex or severe cases sooner. The authors stress that their tool still needs testing on real‑world clinical photos and across many skin tones and cameras. Even so, their work shows that carefully trained AI—especially the InceptionV3 model—can reliably distinguish among seven forms of psoriasis, opening the door to faster, more consistent diagnosis and, ultimately, more tailored care.
Citation: Lakshmi, L., Dhana Sree Devi, K., Rao, K. et al. Advancements in psoriasis classification using custom transfer learning algorithms. Sci Rep 16, 7007 (2026). https://doi.org/10.1038/s41598-026-38197-0
Keywords: psoriasis, skin imaging, deep learning, medical AI, disease classification