Clear Sky Science · en
Platelet-rich plasma promotes cellular recovery from nicotine-induced toxicity via autophagy modulation
Why this matters for your gums
If you smoke or use nicotine products, your gums are fighting an invisible battle every day. Nicotine doesn’t just stain teeth or cause bad breath; it quietly weakens the very cells that keep your gums firm and able to heal. This study asked a hopeful question: can platelet‑rich plasma—a blood‑derived product already used to speed healing in surgery and sports medicine—help gum cells recover from nicotine’s damage and better resist long‑term disease?
How smoking quietly harms the mouth
Periodontitis is a chronic gum disease in which the tissues and bone that support teeth slowly break down. Normally, gum cells and the immune system keep harmful bacteria in check and repair everyday wear. Nicotine disrupts this balance in several ways. It makes blood vessels constrict, reducing oxygen and nutrients. It stresses gum cells so they grow poorly, age faster, and die more easily. It also stirs up inflammation and encourages bone‑eating cells that loosen teeth. The authors focused on gingival fibroblasts—key cells that build and remodel gum tissue—to see exactly how nicotine pushes them toward disease.
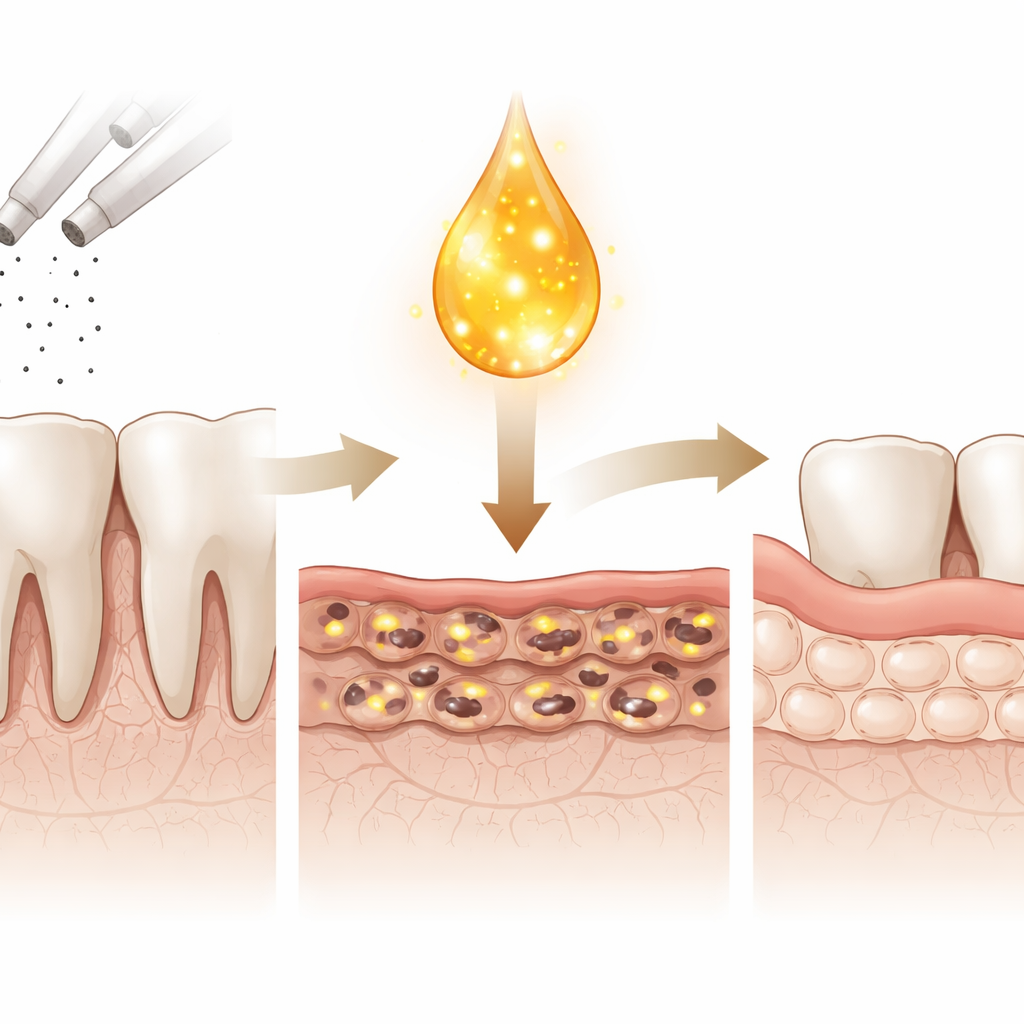
A healing boost taken from blood
Platelet‑rich plasma (PRP) is made by spinning down a small sample of blood to concentrate platelets, which are tiny fragments packed with growth factors and signaling molecules. Dentists already use PRP in some surgeries to encourage faster healing. In this work, researchers treated human gum fibroblasts grown in the lab with realistic doses of nicotine similar to those found in smokers’ blood. High nicotine levels caused the cells to swell with fluid‑filled bubbles, lose energy, stop dividing, and eventually die. When the same damaged cells were then exposed to a modest amount of PRP, many of these harmful changes were reversed: energy levels recovered, more cells survived, and the sheet of cells became denser and healthier‑looking.
Nicotine, cellular “self‑eating,” and how PRP calms it down
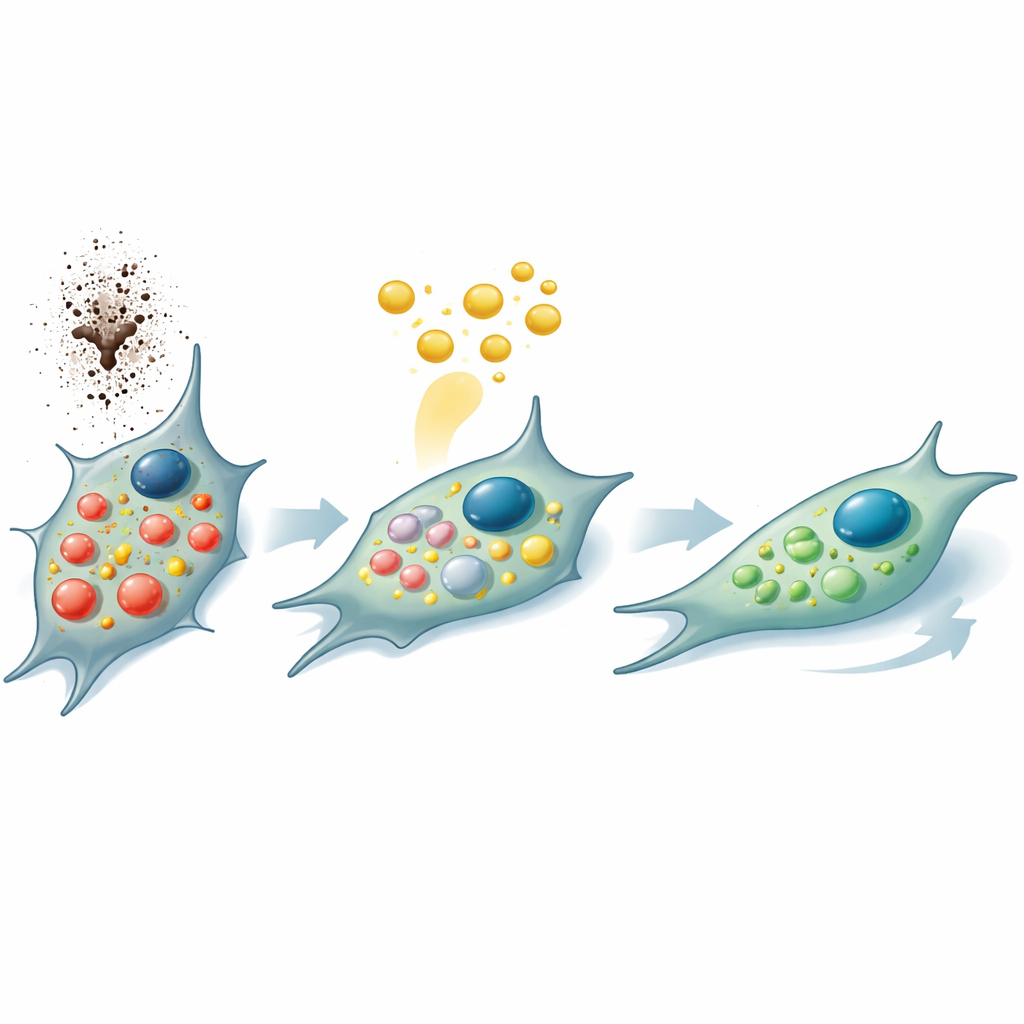
One of nicotine’s key effects is to crank up autophagy, a sort of cellular “self‑cleaning” or “self‑eating” system. In small doses, this process keeps cells healthy by recycling worn‑out parts; when overactivated, it becomes a sign of stress and can tip cells toward damage and premature aging. The team showed that nicotine increased acidic compartments and waste‑processing vesicles inside gum cells, along with a surge in reactive oxygen species—high‑energy molecules that attack cell components. PRP treatment dialed down these stress signals, reduced the number of overactive vesicles, and cut oxidative stress. The researchers also examined worms of the species C. elegans, a classic aging model. Nicotine shortened their lifespan and triggered excessive autophagy, but adding PRP reduced this overactivity and helped the worms live longer under stress.
Signals that link healing, inflammation, and recycling
To understand how PRP reshapes cell behavior, the scientists measured dozens of signaling proteins released by nicotine‑exposed gum cells. With PRP present, several messengers involved in inflammation, blood vessel growth, and tissue remodeling rose in a coordinated pattern. Many of these molecules are known to intersect with the pathways that govern autophagy, suggesting that PRP does more than simply feed cells growth factors—it appears to rebalance the way cells respond to stress, curb overactive self‑eating, and promote a more repair‑oriented state that supports migration and rebuilding of damaged gum tissue.
What this could mean for smokers’ dental care
Overall, the study suggests that PRP can protect and revive gum cells that have been harmed by nicotine, in part by calming excessive autophagy and oxidative stress and by encouraging healthier cell movement and survival. For dentistry, this raises the possibility that adding PRP to certain periodontal treatments might improve healing in patients who still use nicotine. However, the experiments were done in cell cultures and in worms, not in people with long histories of smoking. The authors stress that no blood‑based treatment can substitute for quitting tobacco: stopping nicotine remains the single most powerful step to protect your gums and overall health. PRP should be viewed as a potential helper in repair, not a license to keep smoking.
Citation: Vérièpe-Salerno, J., Cancela, J.A., Vischer, S. et al. Platelet-rich plasma promotes cellular recovery from nicotine-induced toxicity via autophagy modulation. Sci Rep 16, 7979 (2026). https://doi.org/10.1038/s41598-026-38188-1
Keywords: gum disease, nicotine, platelet rich plasma, cellular stress, regenerative dentistry