Clear Sky Science · en
Comparison of choroidal hypertransmission and retinal pigment epithelium loss for quantification of geographic atrophy across commonly used SD-OCT devices
Why this matters for people losing sight
Geographic atrophy is an advanced form of age-related macular degeneration, a leading cause of vision loss in older adults. As new drugs to slow this disease finally reach the clinic, doctors urgently need reliable ways to measure whether the damaged areas in the retina are growing or stabilizing. This study asks a deceptively simple question with big consequences: when different eye scanners are used to track the same patient, do they actually agree on how large the damaged area is?
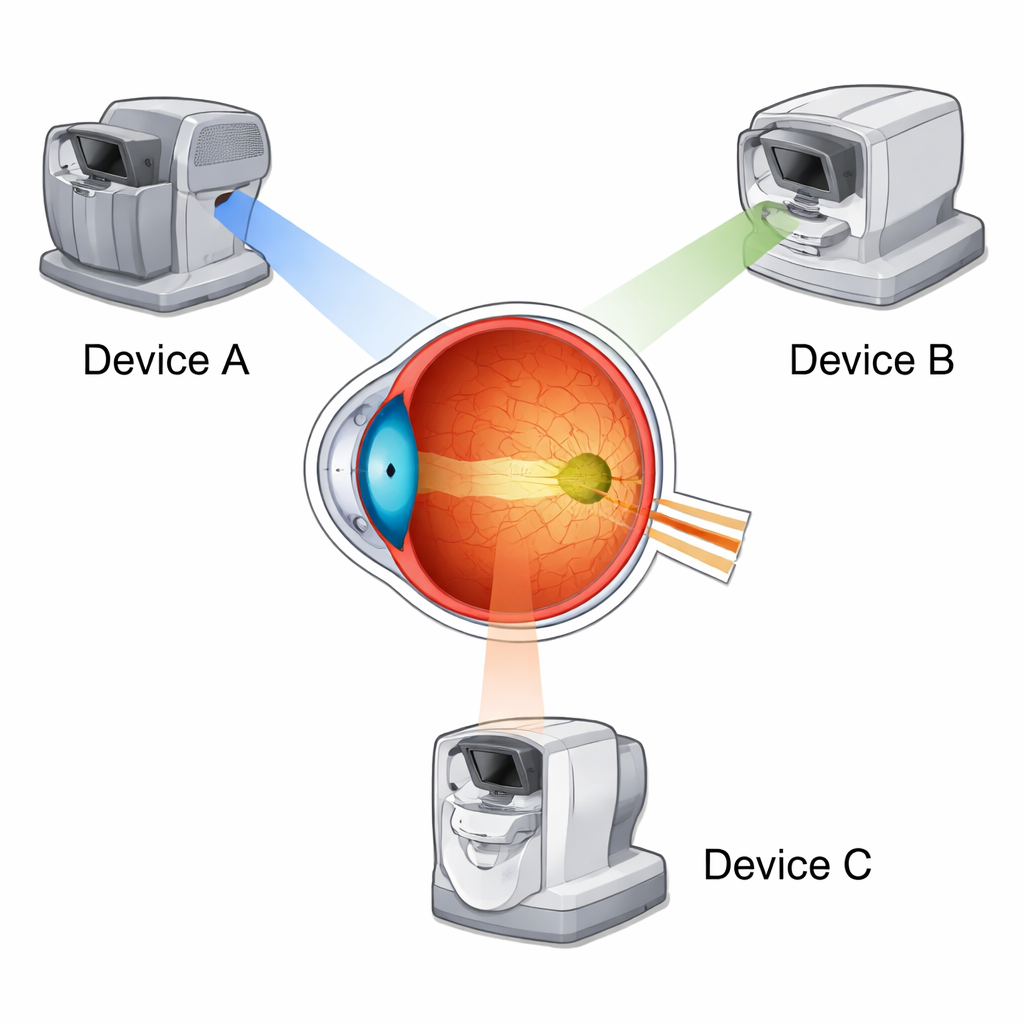
Different cameras looking at the same damaged retina
The researchers focused on three of the most commonly used optical coherence tomography (OCT) machines in eye clinics today. OCT is a noninvasive imaging technique that creates cross-sectional "slices" of the retina, a bit like ultrasound with light. Forty patients with geographic atrophy were imaged on all three devices during a single visit. This allowed the team to compare measurements made from exactly the same eyes, rather than from different patient groups, removing one major source of variation.
Two ways to see the scar: structure versus light leak
Instead of trying to capture every microscopic change, the study zoomed in on two key signatures of damage within the light-sensitive tissue. One is the actual loss of a crucial support layer called the retinal pigment epithelium (RPE), which nourishes the photoreceptors and helps keep vision functioning. The other is a brightening signal called choroidal hypertransmission, which appears when light passes more easily through areas where overlying tissue has thinned or disappeared. Expert readers carefully outlined, by hand, the areas of RPE loss and hypertransmission in over 7,000 OCT slices, then converted these markings into two-dimensional maps of the damaged regions.
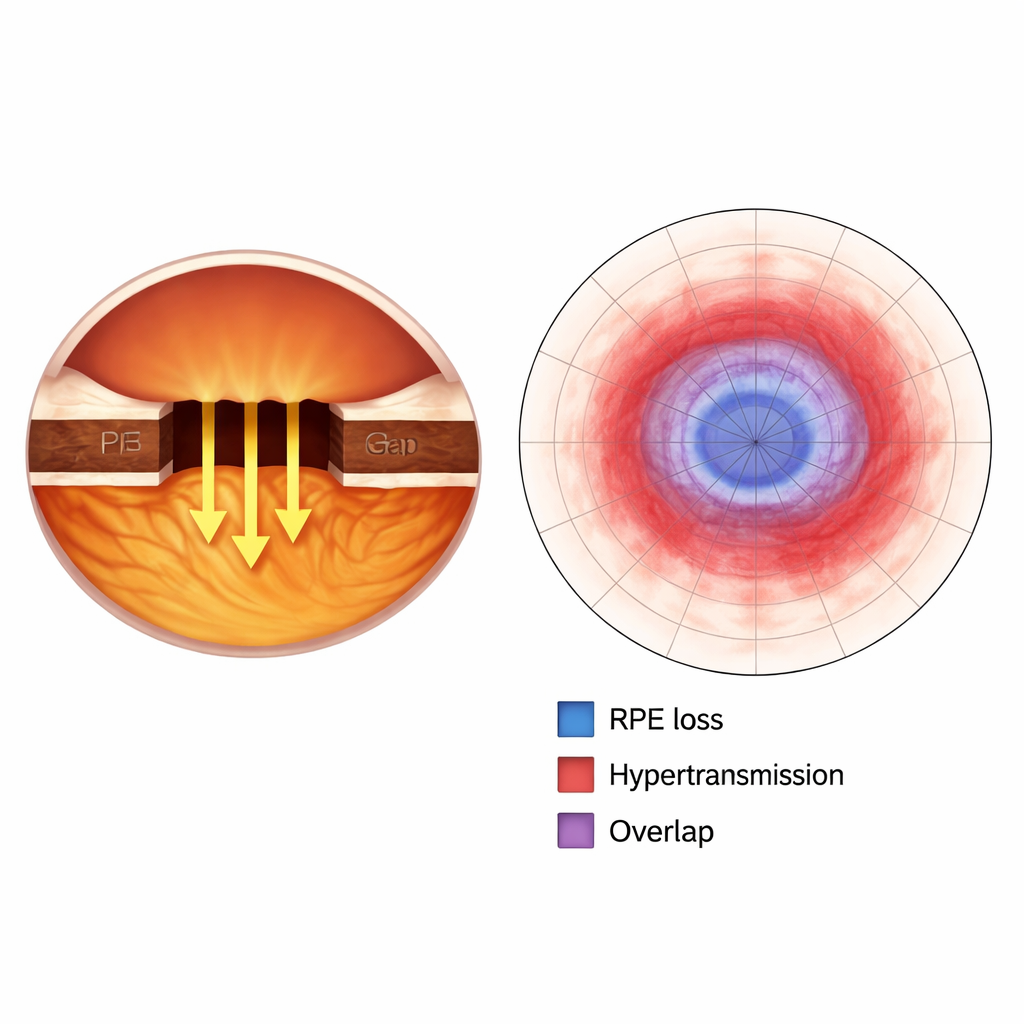
How well did the machines agree?
Overall, the three devices showed good agreement when measuring the size of both RPE loss and hypertransmission, meaning that, in broad terms, they told similar stories about how big the atrophic patches were. However, there were consistent differences. One machine, the Cirrus OCT, tended to report smaller damaged areas than the Heidelberg Spectralis or the Topcon Maestro2. The latter two devices were in much closer alignment with one another. Across all scanners, the regions of increased light transmission were always larger than the zones of outright RPE loss, and the overlap between the two ranged from moderate to good. This suggests that the "light leak" signal often extends beyond the area where the supporting layer has fully disappeared.
Why image quality and device choice still matter
The study also examined how the images themselves differed. The Spectralis device produced sharper images with better contrast and less noise, making delicate retinal layers easier to distinguish. Maestro2 also performed well, while Cirrus sometimes showed more background noise and motion artefacts, likely due to slower scanning. These technical differences help explain why the devices, although broadly consistent, did not match perfectly. Importantly, the variation between machines tended to increase as the damaged area grew larger, meaning that discrepancies are most pronounced in patients with more advanced disease.
What this means for patients and future treatments
For patients, the reassuring message is that the size of geographic atrophy can be measured reasonably reliably on modern OCT devices, especially when attention is paid to how the images are analyzed. The findings highlight RPE loss as a particularly robust marker of real biological damage, closely tied to loss of visual function, while hypertransmission reflects a broader light-based signal that can be influenced by several factors. For doctors, clinical trial designers, and developers of artificial intelligence tools, the key takeaway is caution: switching between different OCT machines can subtly change measured lesion size. To judge whether a treatment is truly slowing disease, studies must account for these device-dependent differences and validate automated algorithms separately for each scanner.
Citation: Eidenberger, A., Birner, K., Frank-Publig, S. et al. Comparison of choroidal hypertransmission and retinal pigment epithelium loss for quantification of geographic atrophy across commonly used SD-OCT devices. Sci Rep 16, 7240 (2026). https://doi.org/10.1038/s41598-026-38182-7
Keywords: geographic atrophy, macular degeneration, optical coherence tomography, retinal imaging, artificial intelligence