Clear Sky Science · en
Contribution of family Support, illness perception, and psychological factors to fluid management behaviors in peritoneal dialysis patients
Why water balance matters for kidney patients
For people whose kidneys have failed and who rely on peritoneal dialysis at home, something as simple as drinking a glass of water can become a daily calculation. Taking in too much fluid can strain the heart and blood vessels, while taking in too little can cause low blood pressure and other problems. This study asks a seemingly simple but important question: beyond medical prescriptions, what helps patients actually follow their fluid limits in real life—and how much do family and emotional health matter?
Living with dialysis and daily fluid limits
Peritoneal dialysis is a life-sustaining treatment for end-stage kidney disease, but it also shifts much of the work of care from hospitals to patients and their families. People must monitor how much they drink, watch salt in their food, and look out for signs of swelling or shortness of breath. Past research shows that many patients struggle with these restrictions, and poor fluid control can lead to high blood pressure, heart enlargement, heart failure, and a higher risk of death. The authors of this study wanted to move beyond machines and medicines to understand how family relationships and emotional well-being shape day-to-day fluid management.
Who was studied and what was measured
The researchers surveyed 314 adults on peritoneal dialysis at a large hospital in China. All had been on treatment for at least three months. They completed questionnaires about how often they followed advice on limiting fluids and salt, weighed themselves, and watched for swelling. The team also measured symptoms of anxiety and depression, how threatening or uncontrollable patients felt their illness to be (called their illness perception), and how supportive and functional they felt their family life was. Medical records provided details such as age, cause of kidney failure, time on dialysis, and basic lab tests like hemoglobin and albumin.
Family ties, mindset, and emotions
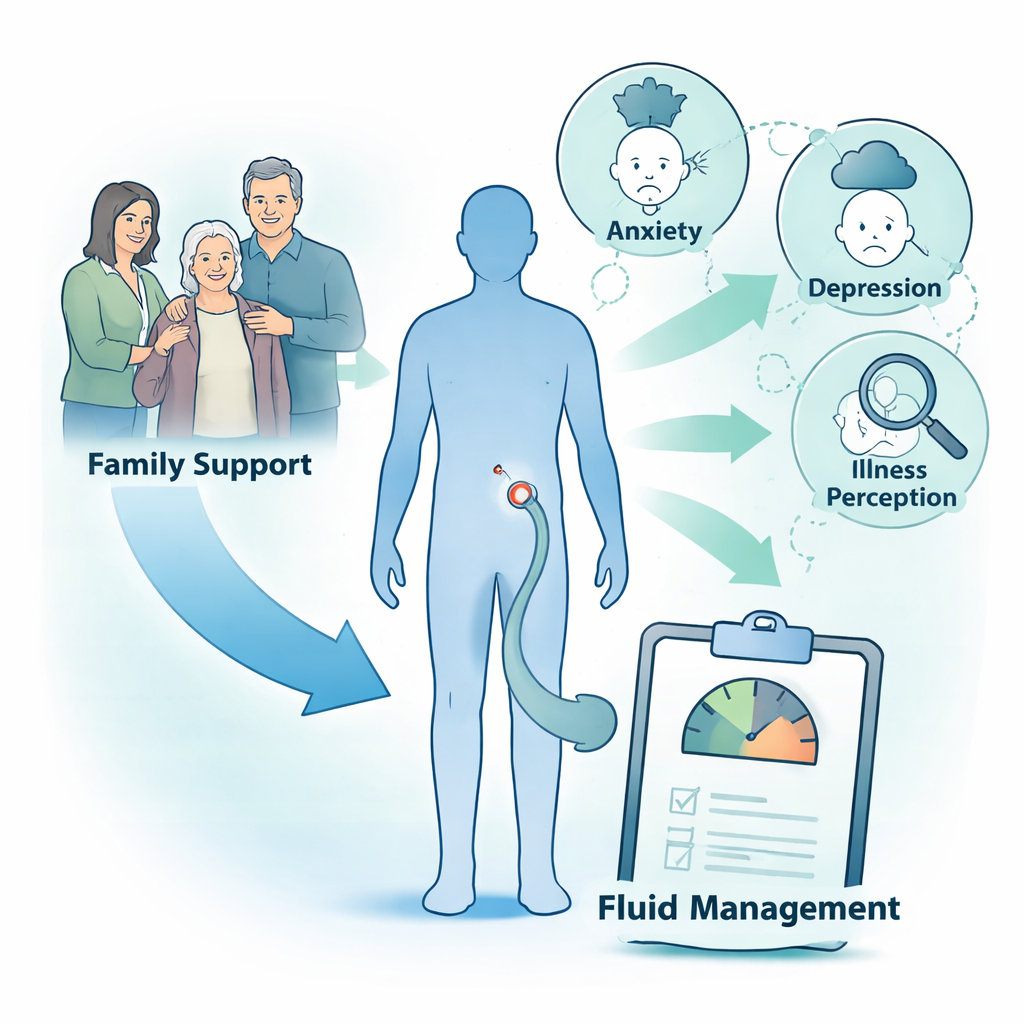
When the researchers analyzed the data, they found that patients who reported stronger family support tended to have better fluid management habits. Good family function was linked with more regular monitoring and closer adherence to fluid and salt limits. Better overall diet management—which includes reading food labels, watching salt, and choosing appropriate protein—also traveled together with stronger fluid control. In contrast, patients who had been on dialysis longer, felt more anxious, or saw their illness as more severe and less controllable were more likely to have difficulty managing their fluid.
How family support works through the mind
To dig deeper, the team used statistical models to see whether emotional health and illness perception help explain how family support translates into better behaviors. They found that part of the benefit of a supportive family runs through lower anxiety and depression and, even more strongly, through a healthier way of thinking about the illness. Patients who felt backed by their families were less distressed and less likely to see their kidney disease as a hopeless threat, and these mental shifts were linked to better fluid management. Illness perception accounted for about one-third of the total connection between family support and fluid control, suggesting that what patients believe and feel about their disease may be as crucial as practical help.
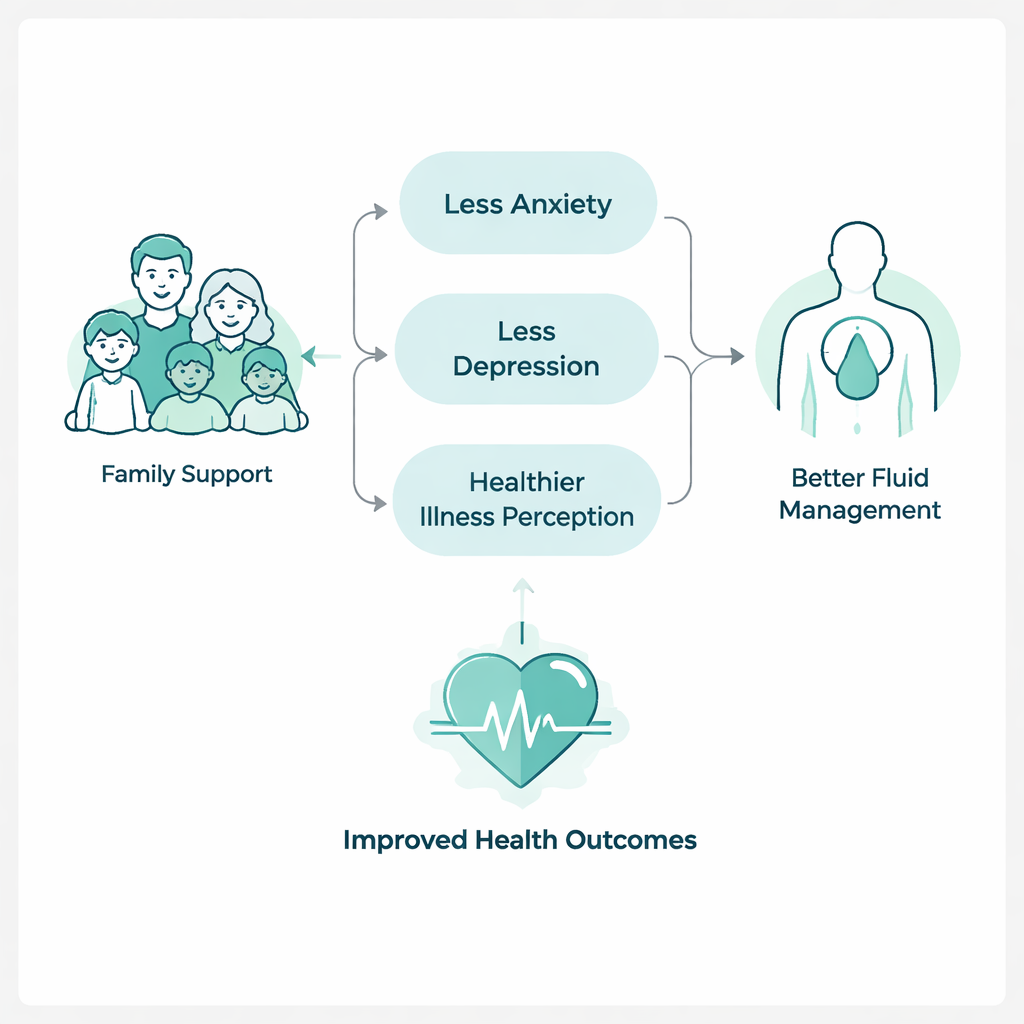
What this means for care
Interestingly, many medical and demographic factors—such as age, sex, and common lab values—were not as strongly tied to fluid management as family and psychological factors were. This supports a “whole-person” view of dialysis care, where nurses and doctors work not only on prescriptions and lab targets but also on strengthening family involvement and addressing anxiety, depression, and discouraging beliefs about illness. The authors caution that their study is cross-sectional, meaning it captures a single snapshot in time, so it cannot prove cause and effect. Still, it highlights promising targets for future programs: counseling that includes family members, education that reshapes how patients think about their disease, and psychological support to ease distress.
Take-home message for patients and families
For people on peritoneal dialysis, staying within fluid limits is not just a matter of willpower or medical orders. This study suggests that feeling supported at home, having a more hopeful and manageable view of kidney disease, and reducing anxiety and depression all make it easier to keep fluid in check. In plain terms, strong families and calmer minds appear to help protect the heart and circulation just as much as careful measuring cups and salt shakers. Future research will test whether programs that build these strengths can improve health and quality of life for dialysis patients around the world.
Citation: Tian, F., Zhang, M., Wang, Y. et al. Contribution of family Support, illness perception, and psychological factors to fluid management behaviors in peritoneal dialysis patients. Sci Rep 16, 7786 (2026). https://doi.org/10.1038/s41598-026-38097-3
Keywords: peritoneal dialysis, fluid restriction, family support, mental health, self-management