Clear Sky Science · en
Pilot study of psilocybin in patients with post-treatment lyme disease
Why lingering Lyme symptoms matter
For many people, a tick bite and a course of antibiotics mark the end of Lyme disease. But for a sizable minority, the story doesn’t end there. Months or years later, they may still battle exhaustion, brain fog, pain, poor sleep, and low mood—problems that can upend work, relationships, and daily life. This condition, known as post-treatment Lyme disease (PTLD), has no proven treatments, leaving patients and doctors searching for new options. The study described here explores an unconventional candidate: psilocybin, the psychedelic compound found in certain mushrooms, given in a carefully supervised medical setting.
A new idea for an old problem
PTLD affects an estimated 10–20 percent of people treated for Lyme disease and is linked not only to physical complaints but also to high rates of depression, anxiety, and reduced quality of life. At present, there are no widely accepted medical therapies that reliably ease this long-lasting burden. Meanwhile, research on psilocybin has suggested that, under controlled conditions, it can rapidly relieve depression and anxiety and may even influence inflammation in the body. These hints led researchers at Johns Hopkins to ask whether psilocybin-assisted treatment could help people whose lives had been derailed by PTLD.
How the study was done
The researchers ran an open-label pilot trial—meaning everyone knew they were receiving psilocybin rather than a placebo—with 20 adults who had well-documented Lyme disease followed by years of ongoing symptoms. Participants first completed screening visits and three weeks of preparatory meetings with two trained facilitators, who provided education about psilocybin, discussed life history and illness, and helped clarify personal goals. During weeks four and six of the eight-week program, participants received psilocybin capsules in a controlled clinic room, starting with a moderate dose and, for most, a higher dose two weeks later. They wore eyeshades, listened to music, and were supported throughout by the facilitators. Follow-up visits took place over six months, during which the team tracked symptom burden, mood, pain, fatigue, sleep, and quality of life using standard questionnaires.
What happened after treatment
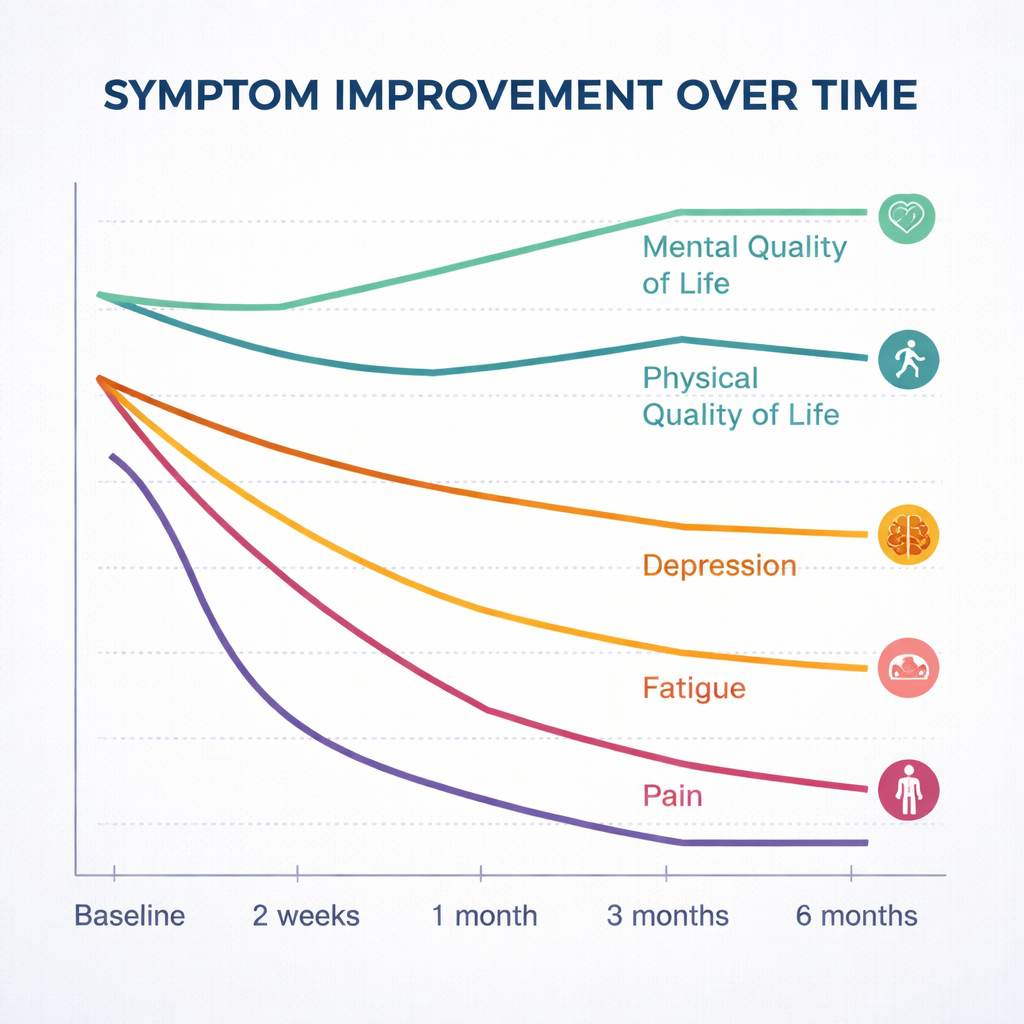
By the first main follow-up, one month after the second psilocybin session, participants reported striking improvements. Overall PTLD symptom burden had fallen by more than 40 percent, and many people described feeling more capable and less overwhelmed by their illness. Scores for mental and physical quality of life both rose by around 13 percent, suggesting gains in everyday functioning as well as emotional well-being. Measures of depression dropped by roughly half, sleep problems eased, and fatigue and pain scores all declined substantially. Importantly, these benefits were not fleeting: on average, improvements in symptoms and quality of life persisted for the full six months of observation.
Safety, side effects, and open questions
Safety was a major concern because psilocybin can temporarily alter perception, blood pressure, and heart rate. In this carefully monitored setting, however, no serious side effects were attributed to the drug. Nearly all participants experienced short-lived increases in blood pressure and many had headaches or fatigue after sessions, but these issues resolved on their own or with simple over-the-counter remedies. One participant developed suicidal thoughts after starting a new antidepressant weeks later, and another was diagnosed with cancer during the study; both events were judged unrelated to psilocybin. Still, the trial had important limitations: it was small, had no comparison group, and relied on self-reported symptoms, so expectations and the intensive supportive care could have amplified perceived benefits.
What this could mean for patients
To a lay reader, the key takeaway is that a small, early-stage study suggests psilocybin-assisted treatment—two carefully guided psychedelic sessions embedded in several weeks of psychological support—may offer meaningful, long-lasting relief for some people struggling with the lingering fallout of Lyme disease. The results do not prove that psilocybin is a cure, nor do they justify unsupervised use, which can be risky and is often illegal. Rather, they point to a promising direction for future, more rigorous trials that include control groups and biological measurements. If confirmed, this approach could open a new path not only for PTLD, but potentially for other chronic, infection-related conditions that currently leave patients with few good options.
Citation: Garcia-Romeu, A., Naudé, G.P., Rebman, A.W. et al. Pilot study of psilocybin in patients with post-treatment lyme disease. Sci Rep 16, 7497 (2026). https://doi.org/10.1038/s41598-026-38091-9
Keywords: Lyme disease, psilocybin, chronic symptoms, psychedelic therapy, quality of life