Clear Sky Science · en
Effect of simultaneous application of low-level diode laser and leukocyte platelet-rich fibrin on gingival tissue healing: an in vitro investigation
Faster Healing for Sore Gums
Bleeding gums, loose teeth, and painful dental work all have something in common: they depend on how well the soft tissue around our teeth can heal. This study explores whether two modern helpers—a gentle medical laser and a special blood‑derived gel—can work together to speed healing in gum tissue. Understanding this could one day mean quicker recovery, less pain, and better long‑term outcomes after gum disease treatment or oral surgery.
What Keeps Our Gums Healthy
The tissue that supports our teeth, called the periodontium, includes the gums, ligament, root surface, and surrounding bone. When gum disease or injury strikes, the fibers and cells that normally anchor the gums to the teeth are damaged. Healing then relies on fibroblasts—workhorse cells that migrate into the damaged area, divide, and lay down new collagen, the structural protein that acts like scaffolding. At the same time, new blood vessels must grow to feed the repairing tissue, and old or damaged matrix must be remodeled so healthy tissue can take its place.
Two Modern Helpers: A Gel from Your Blood and a Gentle Light
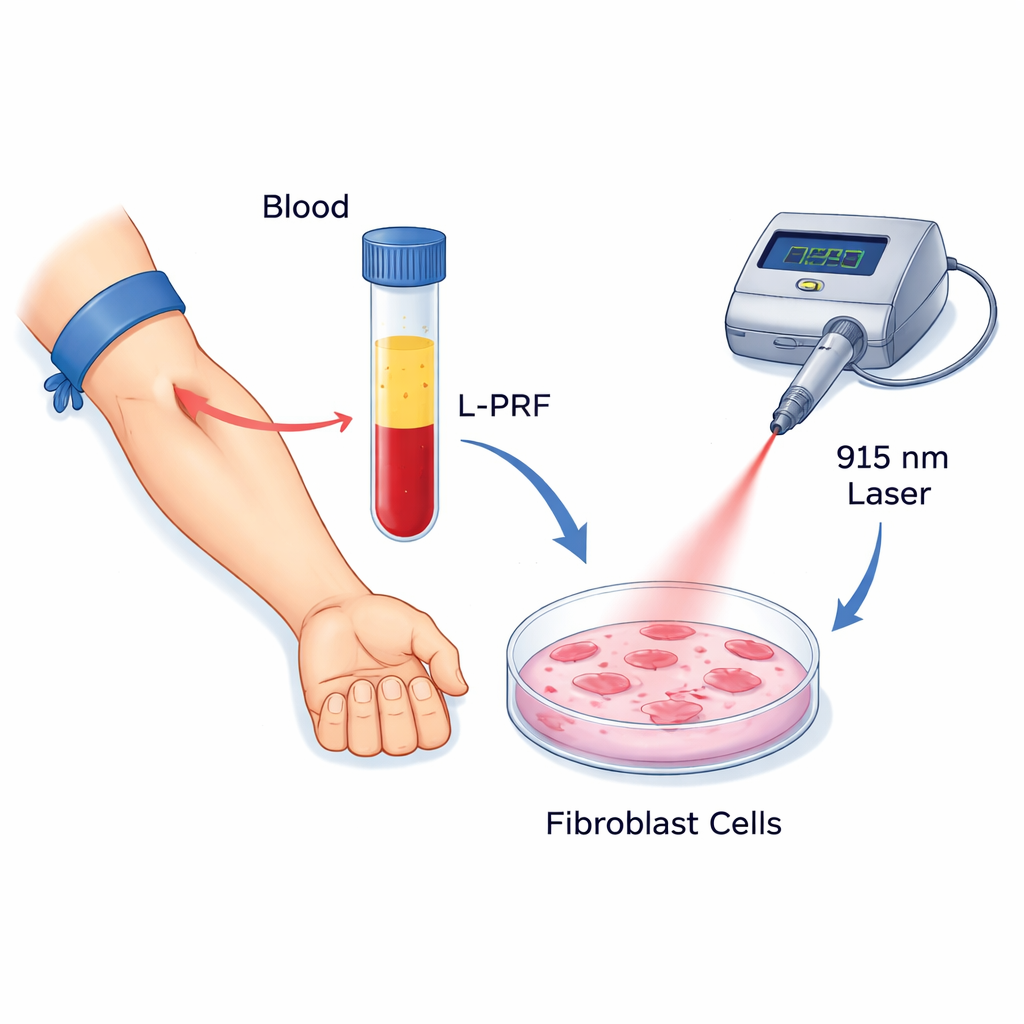
The researchers focused on two promising tools that dentists are already beginning to use. The first is leukocyte platelet‑rich fibrin (L‑PRF), a clot‑like material made from a patient’s own blood by spinning it in a centrifuge. This sticky matrix is rich in platelets, white blood cells, and growth factors that are slowly released over time and are known to encourage cell growth, movement, and tissue repair. The second tool is low‑level laser therapy (LLLT), here delivered by a 915‑nanometer diode laser. Unlike the powerful cutting lasers used in surgery, this low‑energy light aims to gently stimulate cells, reduce inflammation, and boost their activity without heating or damaging tissue.
Putting Gum Cells to the Test
To see how these two therapies behave alone and together, the scientists grew standard human gingival fibroblast cells in the lab. They exposed the cells to different concentrations of L‑PRF and to laser light at several energy doses, and then chose a 25% L‑PRF solution that boosted cell survival without overcrowding the dishes. The fibroblasts were assigned to eight groups: no treatment, L‑PRF alone, three laser settings alone, and the same three laser settings combined with L‑PRF. The team measured how many cells survived and divided, how quickly they migrated across an artificial “scratch” wound, and how strongly they switched on three key healing‑related genes linked to tissue remodeling, collagen formation, and blood vessel support.
What Happened When Light Met Blood‑Derived Gel
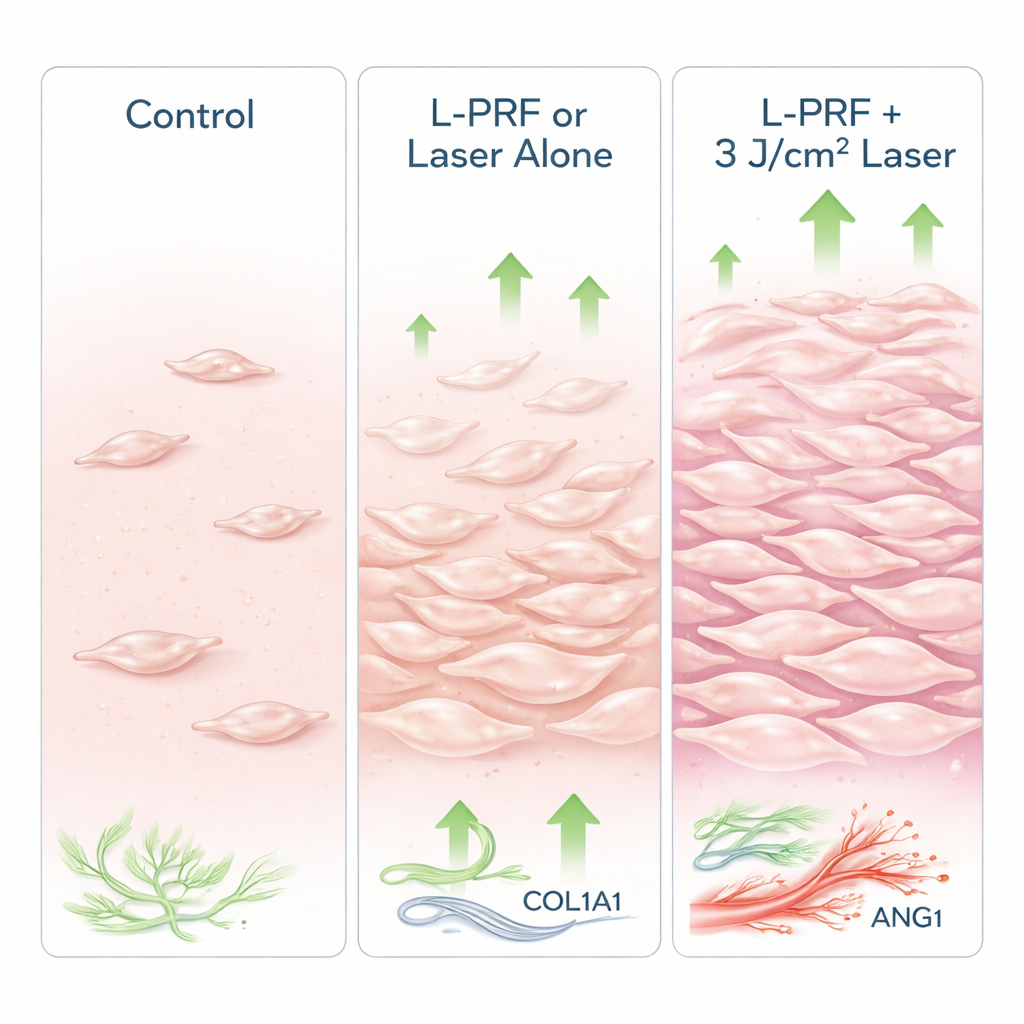
Both L‑PRF and the laser on their own clearly helped the gum cells compared to no treatment: survival, growth, movement, and healing‑related gene activity all increased. When the two were combined, the benefits generally became stronger. The standout condition was L‑PRF used together with the 3 J/cm² laser dose, which produced the highest overall cell viability and proliferation. This combination also triggered the greatest rise in genes related to collagen production and blood vessel stability, suggesting stronger, better‑organized repair tissue. Interestingly, L‑PRF alone drove the largest jump in one remodeling gene involved in breaking down old collagen, which is useful early in healing but potentially harmful if overdone—hinting that the combined treatment may provide a more balanced response.
What This Could Mean for Patients
This work was done in dishes, not in people, so it cannot yet dictate dental practice. Still, the findings support a simple message for lay readers: a patient’s own blood‑derived gel and a carefully dosed soft laser beam may work better together than either one alone in encouraging gum cells to grow and organize new tissue. In particular, the pairing of L‑PRF with a moderate laser dose (3 J/cm²) appeared to give the most favorable mix of cell growth, movement, and supportive healing signals. If future clinical studies confirm these results, dentists may be able to combine these two tools to help gums heal faster and more comfortably after treatments for gum disease or surgical procedures.
Citation: Nazari, H., Hodjat, M., Saberi, S. et al. Effect of simultaneous application of low-level diode laser and leukocyte platelet-rich fibrin on gingival tissue healing: an in vitro investigation. Sci Rep 16, 7036 (2026). https://doi.org/10.1038/s41598-026-38012-w
Keywords: gum healing, low level laser therapy, platelet rich fibrin, periodontal regeneration, gingival fibroblasts