Clear Sky Science · en
UCMSC-derived exosomes ameliorate dry eye disease pathogenesis by modulating neutrophils on Th17/Treg balance
Why Dry, Irritated Eyes Are More Than a Nuisance
Millions of people, especially older women and heavy screen users, live with dry, burning, or gritty eyes. We tend to reach for artificial tears, but these offer only brief comfort and do little to tame the underlying inflammation. This study explores a new, cell-free therapy made from tiny particles released by umbilical cord stem cells, asking whether they can not only soothe symptoms but also correct the immune imbalance that drives dry eye disease in the first place.
A Fresh Look at What Drives Dry Eye
Dry eye disease is now recognized as a chronic immune disorder of the eye’s surface, not just a problem of “not enough tears.” In people with dry eye, the balance of immune cells is disturbed: aggressive T helper 17 (Th17) cells that fuel inflammation become more abundant, while regulatory T cells (Tregs), which act as peacekeepers, are reduced. This imbalance, together with faulty tear production, leads to an unstable tear film and damage to the clear surface of the eye. Standard treatments, such as artificial tears, steroids, and immune-suppressing eye drops, can ease symptoms but often bring side effects and do not directly reset this immune imbalance.
Tiny Packages From Stem Cells as Medicine
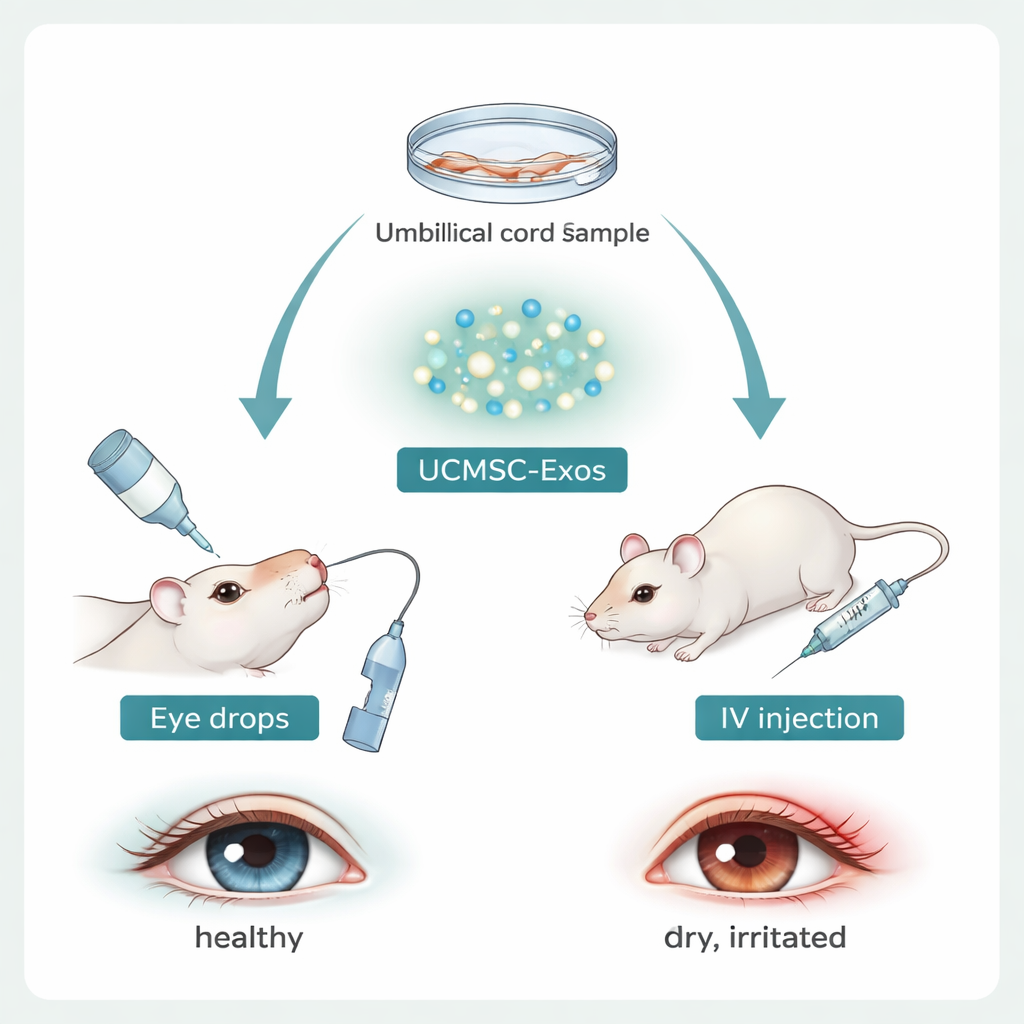
Researchers have been interested in mesenchymal stem cells because they can calm inflammation, but using whole cells raises safety and ethical concerns. The team behind this study focused instead on exosomes—nano-sized bubbles naturally released by umbilical cord mesenchymal stem cells. These exosomes carry proteins and genetic material from their parent cells and can slip through barriers on the eye’s surface. The scientists purified these vesicles in the lab, confirmed their size and characteristic markers, and then tested whether they could help corneal cells “crawl” to seal wounds in a dish. Corneal cells exposed to exosomes closed scratch-like gaps faster, hinting that these particles can directly aid surface repair.
Testing the Therapy in a Mouse Model of Dry Eye
To see how exosomes perform in a living system, the researchers used female mice exposed to a drying environment and a drug that shuts down tear glands, mimicking human dry eye. Both young and older mice developed classic signs: more fluorescent staining on the cornea, indicating surface damage, and lower tear production. At the same time, the outer edge of the cornea showed abnormal numbers of neutrophils—first-responder immune cells—and the nearby lymph nodes displayed more inflammatory Th17 cells and fewer calming Tregs. This pattern confirmed that the model captured the immune chaos seen in patients.
How Exosomes Calm the Immune Storm
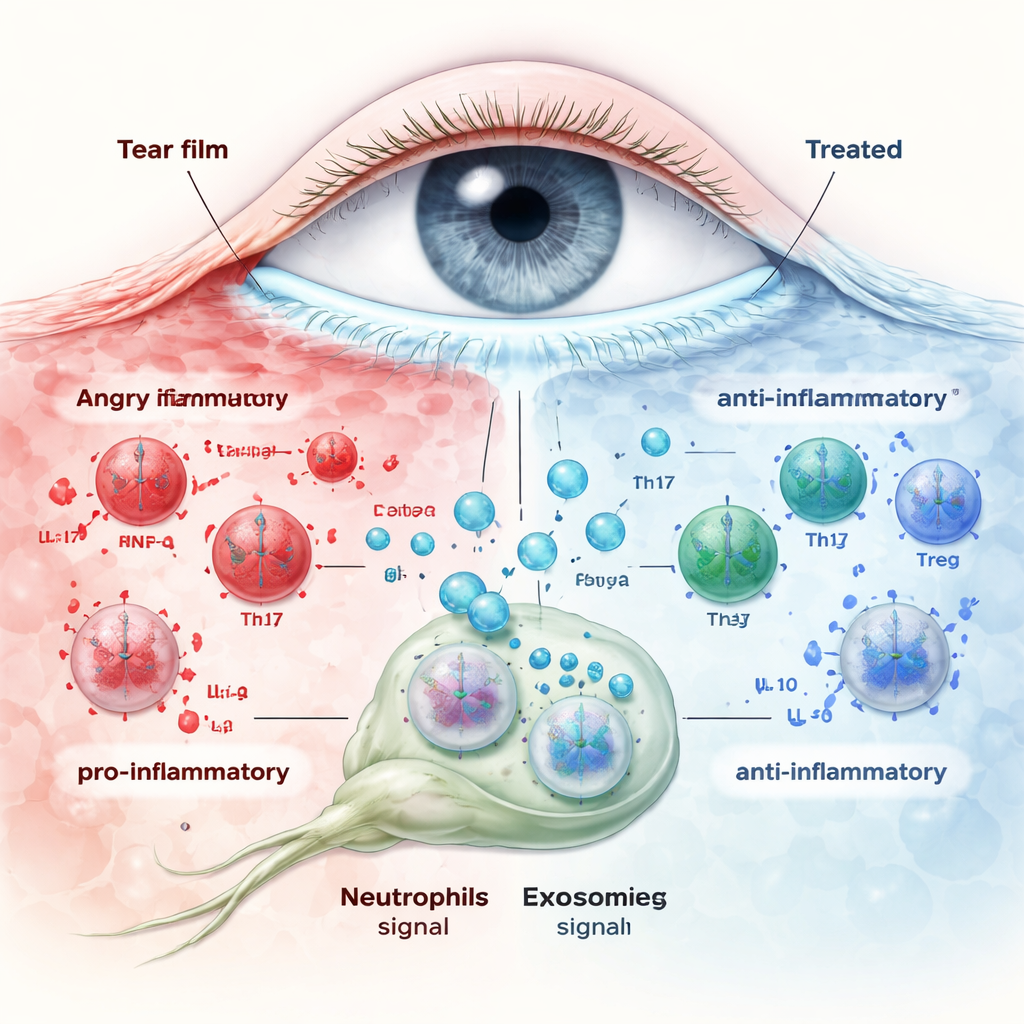
The team then treated dry-eye mice with umbilical cord exosomes either as eye drops or by a single injection into a vein. Both routes improved corneal health and tear output, with stronger effects in younger animals and after systemic injection. Gene activity in the cornea shifted away from alarm signals and toward normal tissue repair. Importantly, exosome treatment restored neutrophil numbers around the cornea and changed what these cells were “saying.” In untreated dry eye, neutrophils pumped out pro-inflammatory messages such as IL‑1β and IL‑17, while dialing down soothing factors like IL‑10, TGF‑β, and Arg‑1. Exosomes reversed this pattern, increasing anti-inflammatory signals and reducing inflammatory ones in both neutrophils from eye-draining lymph nodes and in the cornea itself. As these signals changed, the Th17/Treg balance in lymph nodes moved back toward normal, linking the behavior of innate immune cells (neutrophils) to the resetting of adaptive T cells.
What This Could Mean for Future Treatments
In plain terms, this work suggests that tiny particles from umbilical cord stem cells can both help damaged eye surfaces heal and teach the immune system to calm down. Rather than simply adding moisture, these exosomes appear to coach neutrophils to release more “peacekeeping” molecules and fewer inflammatory ones, which in turn restores the balance between harmful and protective T cells. The benefits were stronger in younger animals and when given through the bloodstream, but even eye drops showed promise. Because exosomes avoid many of the safety issues of live stem cells and can be manufactured in a controlled way, they may one day offer people with dry eye a more targeted, long-lasting therapy that tackles the root cause of their discomfort, not just the dryness they feel.
Citation: Gong, Y., Ding, Y., Yang, J. et al. UCMSC-derived exosomes ameliorate dry eye disease pathogenesis by modulating neutrophils on Th17/Treg balance. Sci Rep 16, 7350 (2026). https://doi.org/10.1038/s41598-026-38010-y
Keywords: dry eye disease, ocular inflammation, exosome therapy, mesenchymal stem cells, immune balance