Clear Sky Science · en
The effect of inflammatory factors on unstable angina risk, from the gene level
Why heart inflammation genes matter to you
Chest pain from heart disease often seems to strike out of nowhere, even in people who don’t smoke, watch their diet, and keep their blood pressure under control. This study looks under the hood of the immune system to ask a simple question with big consequences: do small inherited differences in our “inflammation genes” help explain why some people’s heart arteries suddenly become unstable, setting the stage for a heart attack?
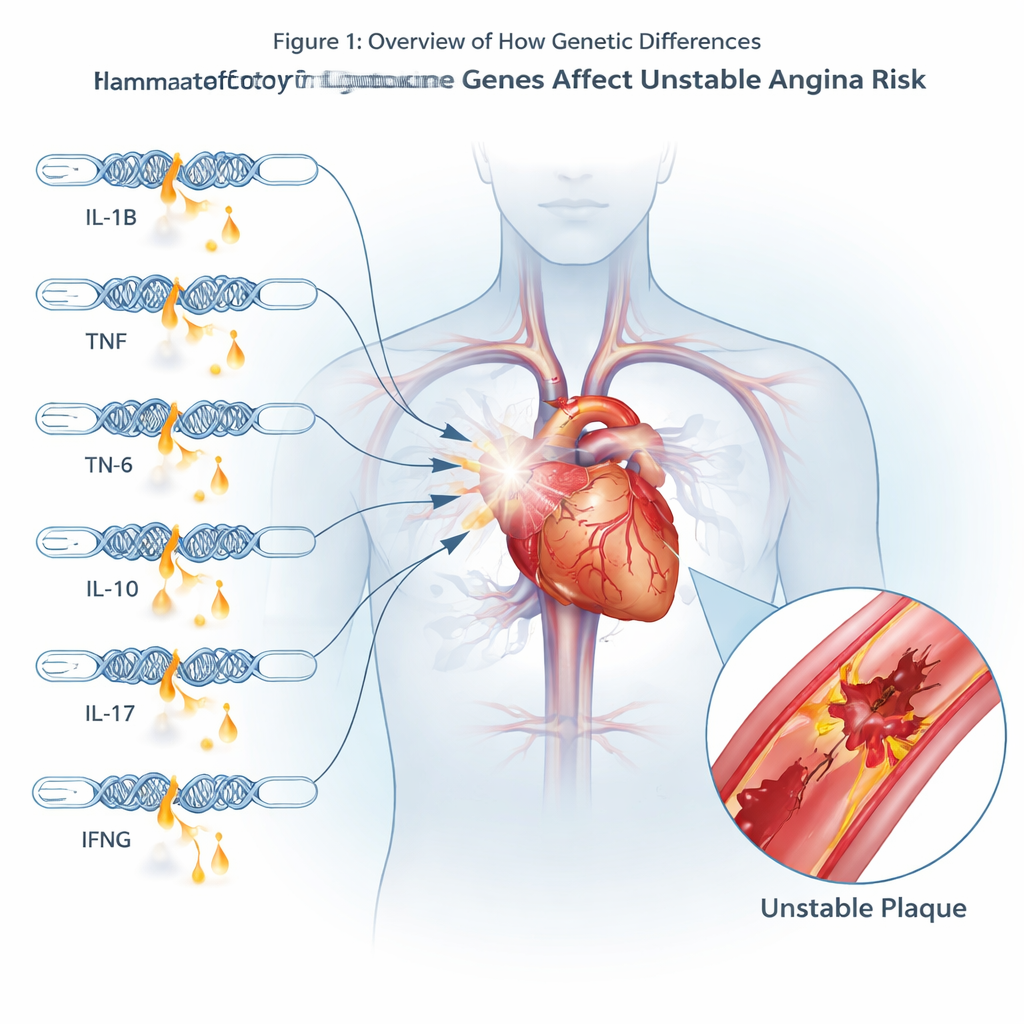
The danger zone between stable and heart attack
Unstable angina is a medical red alert. It happens when fatty buildup in the heart’s arteries suddenly becomes fragile and prone to cracking, allowing a blood clot to form and choke off blood flow. Unlike a classic heart attack, the damage may not yet be permanent, but the risk is high and urgent. Doctors have long known that chronic inflammation in the artery wall fuels the growth and rupture of these plaques, but people differ widely in how strongly their bodies stir up inflammatory signals. This work focuses on whether inherited variations in key inflammation-related genes help tip someone toward this unstable state.
Taking blood and reading the body’s signals
The researchers recruited 160 patients with unstable angina and 280 similar adults without heart disease from a hospital in Southwest China. Everyone underwent careful checks to rule out other illnesses that might confuse the picture, such as infections, autoimmune diseases, or severe kidney and liver problems. From each volunteer, the team drew blood twice in a sense: they measured actual levels of several inflammatory messenger proteins in the serum, and they also analyzed stretches of DNA that control how strongly these messengers are made. The proteins included well-known immune signals like interleukins, tumor necrosis factor, and interferon; the genetic sites were chosen because earlier work suggested they can dial these signals up or down.
Stronger inflammatory signals in people with chest pain
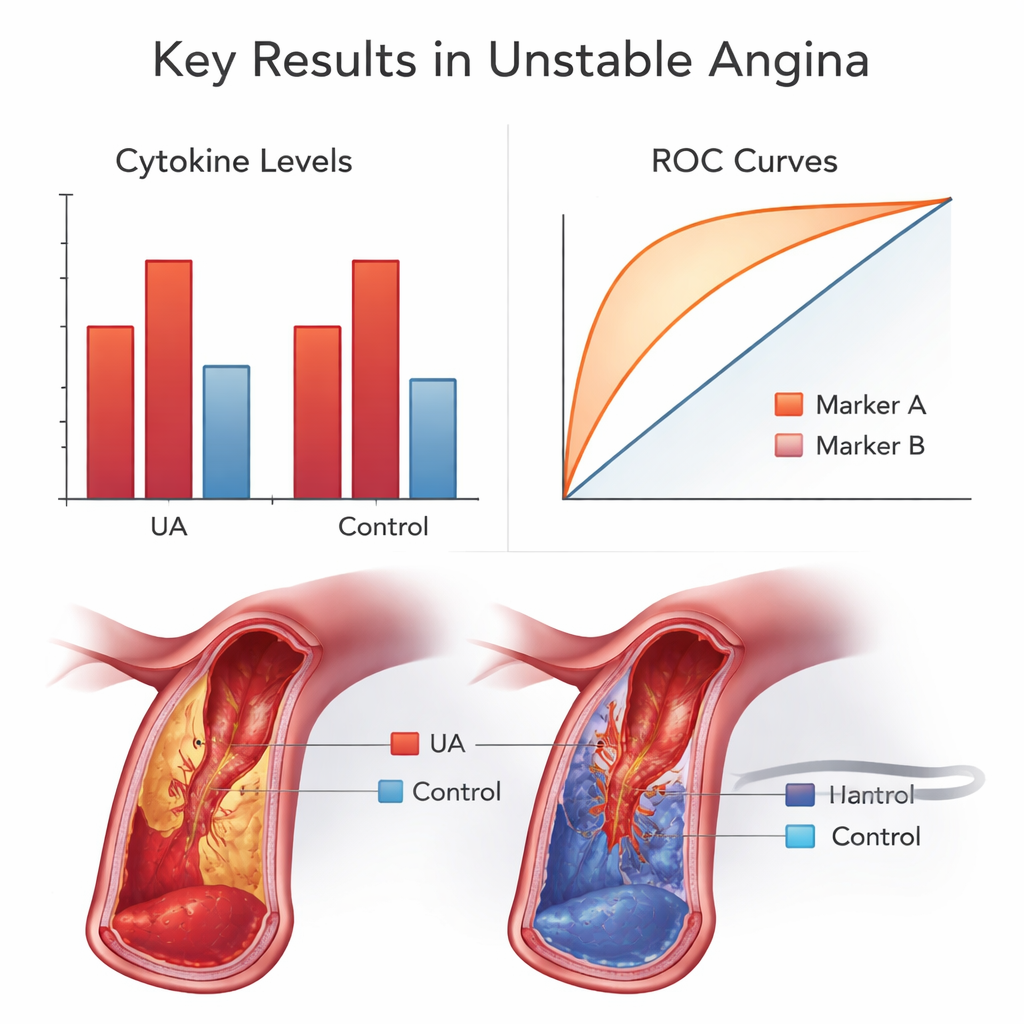
The first clear pattern was in the blood tests. Every inflammatory messenger measured was higher in patients with unstable angina than in the healthy comparison group. Some signals, such as IL-6 and IL-1β, were roughly one-and-a-half to two times higher. One molecule, IL-10, commonly thought of as a soothing, “brake-like” signal, was more than tripled. Rather than contradicting its calming role, this surge likely reflects the body’s attempt to counterbalance an already raging inflammatory fire in the arteries. Together, these findings reinforce the idea that unstable angina is not just a plumbing problem of clogged pipes, but an active inflammatory storm inside the vessel wall.
Inherited switches that turn inflammation up or down
The DNA results showed that certain common genetic variants are strongly linked to who landed in the unstable angina group. People carrying specific versions of the IL-1β and TNF-α genes had several-fold higher odds of unstable angina compared with those who lacked them. By contrast, a particular version of the IL-6 gene appeared to be protective, lowering risk. Variants in IL-10, IL-17, and interferon-γ genes also shifted risk upward. Importantly, these genetic differences were not just abstract markers: carriers of the “risk” versions had higher actual blood levels of the matching inflammatory messengers. In other words, the genetic switches seemed to be stuck more toward the “high” setting, pushing the immune system into a more aggressive mode that can destabilize artery plaques.
Toward more personalized heart risk prediction
When the team tested how well some of these gene variants distinguished patients from healthy people, two of them performed surprisingly well, with accuracy measures that are often sought in diagnostic tools. Still, the authors caution that this is an early step. The study was done in a single region and in a moderate number of volunteers, and it did not test whether using these genetic markers in the clinic would change outcomes. For now, the main takeaway for non-specialists is that heart risk is not only about cholesterol numbers and lifestyle, but also about how your inherited immune wiring handles inflammation. In the future, combining genetic information about these inflammatory switches with traditional risk factors could help doctors identify who is most likely to enter the danger zone of unstable angina and tailor prevention and treatment more precisely.
Citation: Lou, J., Huang, Q., Zhan, R. et al. The effect of inflammatory factors on unstable angina risk, from the gene level. Sci Rep 16, 7152 (2026). https://doi.org/10.1038/s41598-026-37963-4
Keywords: unstable angina, heart inflammation, genetic risk, cytokines, coronary artery disease